Cold: cold flashes perimenopause - Quick Guide to Relief 2026
Explore the causes of cold flashes perimenopause and practical steps to ease symptoms today in 2026.

Ever get that sudden, bone-deep chill in a perfectly warm room and wonder what on earth is going on? If you're in perimenopause, it could very well be a cold flash. It’s a very real, surprisingly common symptom, though it doesn't get nearly as much airtime as its fiery counterpart, the hot flash.
These episodes are your body’s direct response to the hormonal rollercoaster of perimenopause, which can throw your internal temperature controls completely out of whack.
Your Body's Thermostat Gone Wild
Imagine your body has an internal thermostat, managed by a part of your brain called the hypothalamus. It’s usually brilliant at keeping you at the perfect temperature. But during perimenopause, your estrogen levels start fluctuating wildly, and this sends scrambled messages to your brain's command center.
This hormonal static can fool your hypothalamus into thinking you're overheating when you're perfectly comfortable. In response to this false alarm, it hits the emergency "cool down" button. Your body kicks into high gear to shed heat, and that’s what you feel as a cold flash—a sudden, intense chill that can bring on shivering and clammy skin. It's basically a physiological overcorrection for a problem that was never there to begin with.
You're Not Imagining It (And You're Not Alone)
While hot flashes tend to steal the spotlight, you are far from alone if you're experiencing these icy spells. Research shows that roughly 20-30% of women get cold flashes during the menopausal transition. They just don't get talked about as much as hot flashes, which affect up to 80% of women.
Just knowing the "why" behind these chills can be a huge relief. They aren’t just a weird quirk; they're a direct result of the profound biological shifts happening inside you. Cold flashes are just one piece of the puzzle. To see how they fit into the bigger picture, take a look at our complete guide on the 34 symptoms of perimenopause.
The core issue is a communication breakdown. Fluctuating hormones feed bad data to your brain's thermostat, causing it to launch a cooling defense (a cold flash) against a heat threat that doesn't actually exist.
Cold Flashes vs Hot Flashes
So, is that chill a standalone cold flash or just the aftermath of a hot flash? They can definitely be related—sometimes a drenching hot flash is followed by a sudden chill as your body overcompensates. But a true cold flash is a distinct event that happens all on its own, without any preceding heat.
Learning to tell them apart is the first step in understanding your body's unique patterns during this transition. Let's break down the key differences.
Cold Flashes vs Hot Flashes A Quick Comparison
This table offers a quick side-by-side look to help you pinpoint what you're experiencing.
Symptom Feature | Cold Flashes | Hot Flashes |
|---|---|---|
How it Starts | A sudden, intense feeling of being cold or chilled. | A sudden, intense wave of heat, often in the face and chest. |
Physical Sensations | Shivering, goosebumps, and clammy skin. | Profuse sweating, flushed skin, and a rapid heartbeat. |
Your Reaction | You'll want to grab a blanket or put on a sweater. | You'll want to strip off layers and find a fan. |
Duration | Typically brief, lasting from a few seconds to a few minutes. | Also brief, usually lasting from 30 seconds to a few minutes. |
By recognizing these symptoms for what they are—your body's slightly confused reaction to hormonal changes—you can dial down the anxiety and start figuring out how to manage them.
The Hormonal Rollercoaster Causing Your Chills
To get to the bottom of why you’re suddenly grabbing a sweater in a perfectly warm room, we have to talk about your brain’s command center: the hypothalamus. Think of it as your body's own internal thermostat, a highly sensitive system that spends decades making tiny, precise adjustments to keep your core temperature right where it should be.
Then, perimenopause enters the scene. The main hormone that helps keep this thermostat calibrated, estrogen, starts bouncing all over the place. These unpredictable highs and lows send jumbled signals to your hypothalamus, essentially scrambling its data feed. It’s like the temperature gauge in your car suddenly screaming "overheat!" when the engine is running just fine. This faulty information is the real culprit behind perimenopausal cold flashes.
How Your Brain Triggers a Chill
When your estrogen levels take a sudden nosedive, your hypothalamus can misread this as a sign that your body is getting too hot. It doesn't matter what the room temperature is—your brain perceives a problem and launches an emergency cool-down sequence.
This is the cold flash. It’s a full-body response designed to get rid of heat as fast as possible.
Shivering: Your muscles start to contract and relax in quick succession. It feels completely backward when you're already cold, but it's your body's attempt to generate its own warmth to fight the perceived chill.
Goosebumps: This is a classic evolutionary reflex. The tiny muscles at the base of your body hair tighten up, an ancient instinct meant to trap a layer of insulating air against your skin.
Pale or Clammy Skin: To keep your vital organs warm, your body constricts the blood vessels near your skin's surface. This pulls blood away from your extremities and toward your core, leaving your skin looking pale and feeling cool.
This whole chain of events is an overreaction based on hormonal mixed signals. Your brain is trying to fix a problem that doesn’t actually exist, leaving you shivering for a few minutes until the system finally recalibrates.
This simple diagram shows how it all connects, from the hormonal shift to that all-too-familiar feeling of being chilled.
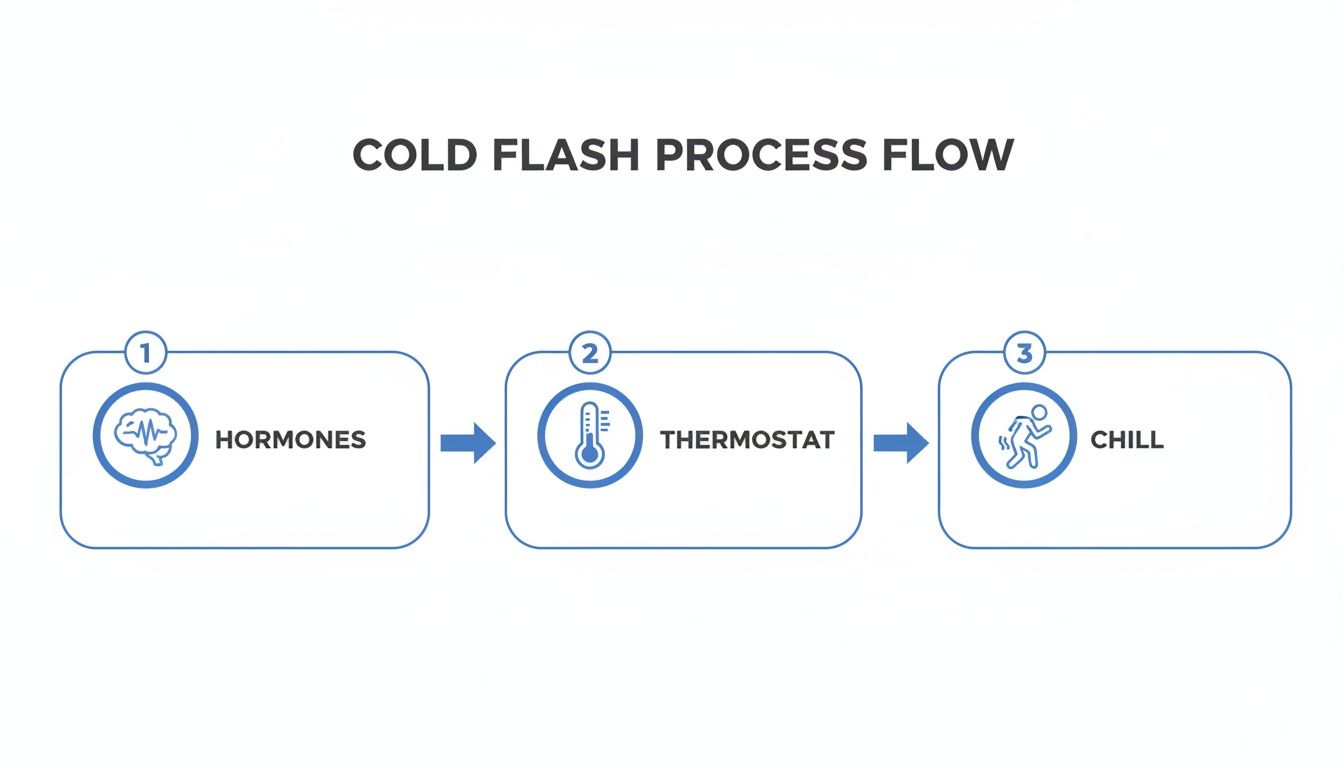
As you can see, it's a direct line from fluctuating hormones to a confused thermostat and, finally, a physical chilling response.
The Hot Flash Rebound Effect
There’s another way cold flashes can show up: right on the heels of a hot flash. When your body is hit with that sudden wave of intense heat and starts pouring sweat, it’s going all-out to cool you down. But sometimes, it works a little too well.
Once the heat passes and all that sweat starts to evaporate, your skin temperature can plummet. This sudden drop can trigger a secondary reaction—a cold flash. It’s a frustrating hormonal whiplash, sending you from burning up one minute to shivering uncontrollably the next.
A cold flash can be a standalone event sparked by an estrogen dip, or it can be the "rebound" effect after a hot flash, where your body's cooling mechanism simply overshoots the mark.
Since these symptoms are so closely tied to your hormones, looking into solutions like hormone balance supplements for women can be a helpful next step. The key is understanding what’s happening in your body. Once you recognize the root cause—this fascinating, if frustrating, neurological mix-up—you’re in a much better position to manage the sudden chills of perimenopause.
Identifying Your Unique Triggers and Patterns
While hormonal shifts are the main reason for cold flashes perimenopause, they're rarely the whole story. Think of it this way: fluctuating hormones make your internal thermostat incredibly sensitive. Then, your daily habits and environment come along and poke at that sensitive thermostat, triggering a sudden chill.
The best way to get a handle on these episodes is to become a bit of a detective. By paying close attention to what’s happening in your day before a cold flash hits, you can start to connect the dots and see what your personal patterns are. This is how you shift from simply reacting to the shivers to proactively managing them.
This isn’t about blaming yourself for that cup of coffee. It’s about empowerment. Once you realize a stressful work meeting or a sugary snack is a consistent trigger, you gain the power to make small, specific changes that can bring huge relief.
Common Lifestyle Culprits
Certain habits are notorious for messing with your body’s delicate balance, making them frequent offenders when it comes to cold flashes. Figuring out why they have this effect is the first step in taming them.
Caffeine: That morning coffee or afternoon tea gives your central nervous system a jolt. This can easily interfere with your hypothalamus's temperature-regulating job, making it more likely to fire off those faulty "cool down now!" signals.
Alcohol: A glass of wine might make you feel warm at first, but alcohol can really throw off your blood sugar and mess with your brain's temperature controls, especially as it wears off. This is a classic trigger for both hot and cold flashes, often waking you up in the middle of the night.
Poor Sleep: Not getting enough quality sleep puts your whole body on edge and can make every hormonal symptom feel ten times worse. When you're running on fumes, your hypothalamus is already over-stressed and much more likely to misread temperature cues.
These are just a few of the usual suspects. Your personal triggers could be completely different, which is exactly why getting to know your own body is so crucial.
The Sugar and Stress Connection
Outside of hormones, two of the biggest players in the cold flash game are unstable blood sugar and chronic stress. They both set off physiological chain reactions that can either mimic or magnify the effects of your estrogen fluctuations, sending your internal thermostat into chaos.
A diet heavy in refined sugars and simple carbs sends your blood sugar on a wild ride. When it comes crashing down after a spike, your body can release stress hormones like adrenaline, which can directly set off a cold flash. It’s a metabolic rollercoaster that just adds another layer of confusion for your already-sensitive hypothalamus.
Key Insight: A sudden blood sugar crash can feel almost identical to a hormonal shift inside your body. This metabolic stress is often enough to fool your brain into launching an unnecessary cool-down response, leaving you with a case of the shivers.
In the same way, chronic stress keeps your body stuck in "fight or flight" mode. The constant drip of cortisol and adrenaline disrupts just about every system you have, including temperature regulation. A tense conversation, feeling overwhelmed by your to-do list, or a family argument can be all it takes to trigger a cold flash.
Why Tracking Is Your Secret Weapon
The only real way to figure out your unique set of triggers is to track them. This is where tools like the Lila app can be a game-changer, giving you an easy way to log your symptoms right alongside your meals, daily activities, and stress levels.
After just a week or two of tracking, you’ll be able to look back and see clear patterns emerging. Maybe your cold flashes almost always pop up after a bad night's sleep or on days you indulge in a sugary dessert.
This is especially important when you consider the link between metabolic health and menopausal symptoms. Insights published in 2026 show a connection between higher insulin levels at age 47 and an earlier start to, and longer duration of, these chills and other vasomotor symptoms. These symptoms hit 75% of transitioning women and can stick around for up to 10 years. You can read more about these findings on vasomotor symptoms and metabolic health.
By carefully tracking these connections, you can create a personalized roadmap to feeling better. This data-driven approach lets you make informed choices, focusing your energy on the lifestyle tweaks that will actually make the biggest difference for you.
7 Practical Ways to Manage and Reduce Cold Flashes
Knowing what triggers your cold flashes is one thing, but having a real-world toolkit to manage them is where the power lies. The good news is you don’t need a massive overhaul. A handful of smart lifestyle shifts, mindful food choices, and simple calming techniques can make a world of difference in how often—and how intensely—those sudden chills hit.
Think of these strategies less like a strict set of rules and more like a series of experiments. Every woman's body is different, so what works wonders for a friend might not be the perfect fit for you. The goal is to find your unique combination of tools that helps stabilize your internal thermostat and keeps you feeling comfortable and in control.
H3: Smart Lifestyle Adjustments
Small, consistent tweaks to your daily rhythm can have a surprisingly big impact on how your body handles those wild temperature swings. These habits are your foundation for feeling better.
Dress in Layers: This is probably the single most effective tactic you can use. Wearing layers—like a tank top, a light long-sleeve shirt, and a cardigan or zip-up—gives you immediate control over your comfort. When a chill sets in, you can add a layer. Feeling a little warm? Just peel one off. It’s that simple.
Stay Active: You don't have to run a marathon. Regular, moderate exercise is fantastic for regulating hormones and improving circulation. Things like brisk walking, swimming, or cycling help stabilize your nervous system, which makes it less likely to overreact to those hormonal dips.
Prioritize Sleep: A well-rested body is a resilient body. When you're exhausted, stress hormones can run rampant, and they're a known trigger for vasomotor symptoms like cold flashes. Aim for a consistent sleep schedule and create a cool, dark, and quiet bedroom. If cold flashes are waking you up, consider investing in the best comforter for cold sleepers to help keep your temperature steady all night long.
H3: What to Eat for Better Hormonal Balance
What you put on your plate has a direct line to your hormonal health and blood sugar—two massive players in the cold flash game. A nutrient-dense diet gives your body the building blocks it needs to navigate this transition more smoothly.
A balanced meal with lean protein, healthy fats, and complex carbs from whole foods helps prevent the sharp blood sugar spikes and crashes that can send your internal thermostat into a frenzy.
Think of it this way: Food is information for your body. By choosing foods that promote stability, you’re sending calming signals to your brain's thermostat, which means fewer false alarms that lead to those bone-deep chills.
Consider adding more phytoestrogens to your meals. These are plant-based compounds that can gently mimic estrogen, potentially helping to cushion the blow of your own fluctuating hormone levels.
Flaxseeds: Add a spoonful of ground flax to your smoothie, oatmeal, or yogurt.
Soy: Stick to whole soy foods like edamame, tofu, and tempeh.
Legumes: Lentils, chickpeas, and beans are all fantastic choices.
At the same time, it can be a game-changer to dial back on common triggers like caffeine, alcohol, and super spicy foods. These can directly poke the bear—your central nervous system—and mess with your body's ability to keep its temperature on an even keel.
H3: Mind-Body Techniques to Calm Your System
Stress is a huge trigger for cold flashes, which makes calming your nervous system an incredibly powerful tool. These practices help shift your body out of "fight-or-flight" mode and into a more relaxed "rest-and-digest" state, making your internal thermostat far less twitchy.
Box Breathing: This is a simple but profound technique you can do anywhere, anytime you feel a chill starting to creep in.
Inhale slowly through your nose for a count of four.
Gently hold your breath for a count of four.
Exhale slowly through your mouth for a count of four.
Hold again for a count of four.
Repeat this cycle for just one or two minutes.
This rhythmic pattern directly soothes the part of your nervous system that’s in charge of temperature control. Other amazing practices include yoga, meditation, or even just spending a few quiet minutes in nature. Find what helps you feel centered.
Many of these tips pull double duty. For example, creating a cool bedroom isn't just for cold flashes; it’s also one of the best natural remedies for menopause night sweats, helping you tackle both ends of the temperature spectrum.
Here’s a quick summary to help you build your personalized plan for managing cold flashes.
Your Cold Flash Management Toolkit
Strategy Category | Actionable Tip | Why It Helps |
|---|---|---|
Lifestyle Habits | Dress in layers of natural, breathable fabrics. | Gives you immediate control to add or remove clothing as your body temperature fluctuates. |
Diet & Nutrition | Incorporate phytoestrogens like flaxseeds and soy. | Plant-based compounds can help buffer the effects of declining estrogen levels. |
Mind-Body Practices | Practice box breathing or meditation daily. | Calms the central nervous system, reducing the stress response that can trigger flashes. |
Exercise | Engage in 30 minutes of moderate activity most days. | Improves circulation and helps regulate hormones and neurotransmitters. |
Sleep Hygiene | Keep your bedroom cool, dark, and quiet. | Prevents overheating and reduces sleep disruptions that can worsen symptoms. |
Trigger Management | Limit caffeine, alcohol, and spicy foods. | These substances can directly stimulate the nervous system and disrupt temperature regulation. |
Remember, consistency is more important than perfection. Pick one or two of these strategies to start with this week and see how you feel. You've got this.
When to Talk to Your Doctor About Your Symptoms
▶ PlayWhile lifestyle adjustments can be a powerful first step in managing cold flashes, they aren’t always enough. It’s important to recognize when your self-care efforts need the backing of professional medical advice.
If your cold flashes are genuinely getting in the way of your day-to-day life, it’s time to book an appointment. Think of your self-care as the foundation of a house. If you're seeing cracks in that foundation—like your sleep is a mess or you're constantly anxious about the next chill—it’s a signal to bring in an expert.
Identifying Your Red Flags
Knowing when to make that call can feel a bit uncertain, but some signs are clear indicators that it's the right move. If your symptoms fall into any of these categories, it's worth having a conversation with your healthcare provider.
You should consider seeking medical advice if:
Your life is disrupted. When cold flashes consistently wreck your sleep, make it impossible to concentrate at work, or have you canceling plans, they’ve moved beyond being a simple nuisance.
They come with other symptoms. Chills that show up alongside heart palpitations, strange dizzy spells, or overwhelming anxiety should always be checked out to rule out other issues.
Self-care isn't cutting it. You've been diligently layering your clothes, managing stress, and tweaking your diet for a few months, but you've seen little to no improvement.
You just feel worried. Never underestimate your gut feeling. If the symptoms feel wrong or just too much to handle, that’s more than enough reason to get a professional opinion.
Your experience is valid. If symptoms are interfering with your ability to live your life comfortably and confidently, you deserve medical support and a clear path forward.
How to Prepare for Your Appointment
Walking into your doctor's office with clear, organized information can make all the difference. The more details you can provide, the better your doctor can help you. This is where a little bit of tracking pays off big time.
Before your appointment, try to jot down the following for a week or two:
Frequency and Timing: How often do the chills happen? Do they strike mostly at night, or perhaps during stressful meetings?
Intensity and Duration: On a scale of 1-10, how bad are they? And how long do they usually stick around?
Associated Symptoms: Note anything else you feel at the same time, like shivering, clammy skin, or a racing heart.
Potential Triggers: What were you eating, drinking, or doing right before a cold flash hit?
Bringing this log with you helps your doctor spot patterns that might otherwise be missed. It changes the conversation from a vague "I feel chilly sometimes" to a specific "I'm experiencing intense, five-minute chills about an hour after my morning coffee."
Depending on what you're experiencing, your provider might discuss different options, including Menopause Hormone Therapy (MHT), which can be very effective for managing vasomotor symptoms like cold flashes. If you're looking into other routes, supplements can also play a supportive role. To learn more before your visit, check out our guide on using magnesium for menopause relief. The more you know, the more confident you'll feel in making the right choice for your health.
Common Questions About Perimenopause Cold Flashes
When your body starts throwing new symptoms your way during perimenopause, it's completely normal to have a ton of questions. Getting a handle on what you're feeling is the first step toward managing it. Let's tackle some of the most common questions women have about cold flashes.
My goal here is to clear up the confusion so you can feel more confident and in control.
Can I Have Cold Flashes Without Hot Flashes?
Yes, you absolutely can. It’s a common myth that a cold flash is always the B-side to a hot flash. While it's true that a sudden chill can follow a hot flash as your body tries to cool down, plenty of women experience cold flashes perimenopause all on their own.
Think of it this way: the same hormonal static that messes with your internal thermostat can trigger a "cool down!" signal without ever sending the "heat up!" one first. This is exactly why getting to know your own specific patterns is so helpful.
How Long Will These Cold Flashes Last?
An individual cold flash is usually over pretty quickly—we're talking a few seconds to maybe a couple of minutes. The bigger question, of course, is how long you'll have to deal with them in general, and that answer varies a lot from woman to woman.
For some, it's a short-lived phase that passes in a few months. For others, cold flashes can come and go for several years, much like hot flashes, which can sometimes stick around for up to a decade. The good news is that consistent lifestyle strategies can make a real difference in how often they pop up.
A cold flash itself is short-lived, but the phase of experiencing them can span years. The key is that their intensity and frequency are not set in stone and can be improved with proactive management.
Are Nighttime Chills a Sign of a Bigger Problem?
Nighttime chills are a classic perimenopause symptom. They're caused by the same hormonal roller coaster, which can feel even more dramatic at night when your body's core temperature is naturally supposed to dip for sleep. The result? Seriously disrupted rest.
By themselves, these chills aren't usually a red flag. However, if they come with a fever, sweats that soak through your clothes, or other symptoms that just feel off, it’s always smart to check in with your doctor to make sure nothing else is going on.
Can Stress Alone Trigger a Cold Flash?
You bet it can. Stress is a huge trigger. When you're under pressure, your body pumps out hormones like cortisol and adrenaline. These directly affect your nervous system and can throw your brain's temperature-regulating center completely out of whack.
This stress response can easily set off a cold flash, even if your estrogen isn't taking a nosedive at that very moment. It’s a perfect example of why stress-management practices—like simple deep breathing exercises or mindfulness—are so incredibly effective for managing cold flashes perimenopause.
Ready to take the guesswork out of managing your symptoms? The Lila app combines AI-powered insights with your unique data to create a personalized action plan. Start feeling better and regain control of your perimenopause journey today.
Get Lila, your personal coach for perimenopause.
Built for women in their 40s. 24/7 coaching, in your pocket.


