
Perimenopause Sore Breasts Explained
May 13, 2026
You get dressed in the morning, pull on your bra, and pause. Your breasts feel heavy, tender, oddly bruised, or sore in a way they didn't used to. Maybe it's both breasts. Maybe it seems to come out of nowhere. Maybe it shows up one month, disappears, then comes back again harder the next time. That unpredictability is often what rattles people most.
If you're in your 40s or 50s, this can be a very real part of perimenopause. Breast pain, also called mastalgia, affects up to 70% of women at some point, and during perimenopause specifically, almost 40% report breast tenderness according to Bonafide's overview of menopause and breast pain. That same source notes it's more common in early perimenopause and often eases as you move closer to menopause.
That matters, because many women immediately go to the scariest possibility. Breast soreness can feel alarming. But in perimenopause, it's often your body's changing hormone patterns showing up in breast tissue before you fully realize what's happening overall.
That Familiar Ache Why Are Your Breasts Suddenly Sore
A lot of women tell me some version of the same story. Their periods have gotten less predictable. Sleep is a little off. Mood feels different. Then breast tenderness starts acting strangely too. What used to be a mild pre-period symptom now feels stronger, arrives earlier, or shows up at random times.
That's one reason perimenopause sore breasts can feel so confusing. It doesn't always follow the old PMS pattern you were used to. Instead of a neat monthly rhythm, the soreness may come in waves.
What this soreness often feels like
For many women, the feeling is more of an ache than a sharp pain. Your breasts may feel:
Heavy or full even when your period isn't due
Tender to touch when getting dressed or rolling over in bed
Swollen or tight in your bra
Sensitive around the outer breast or armpit area
Sometimes it's mild and annoying. Sometimes it's distracting enough that you think about it all day.
Breast pain during this stage is often benign and linked to hormonal ups and downs, not something dangerous on its own.
The important thing to know is that this symptom fits into a bigger perimenopause picture. The timing may be messy because the hormones driving it are messy too. Once you understand that, the soreness starts to feel less random and more explainable.
Why this symptom catches women off guard
Breasts are hormonally responsive tissue. They notice shifts in estrogen and progesterone quickly. So when those hormones stop following a predictable pattern, your breasts often react before you can make sense of the rest of the changes.
That doesn't mean you should ignore breast pain. It means you can approach it calmly. First, understand the hormonal reason. Then learn what “normal for perimenopause” usually looks like, what deserves a medical check, and what practical relief steps are worth trying.
The Hormonal Rollercoaster and Your Breasts
One week your bra feels normal. The next, your breasts feel swollen, tender, or oddly heavy by the end of the day. That shift can feel random, but there is usually a reason.

Estrogen surges can make breast tissue feel full and sore
Perimenopause works more like a faulty thermostat than a slow fade. Instead of settling into a steady setting, estrogen can spike, dip, and spike again. Breast tissue is very sensitive to those changes.
When estrogen rises, the milk ducts and surrounding tissue can hold more fluid and become more stimulated. That can leave your breasts feeling fuller, denser, or more tender than usual. The Cleveland Clinic's overview of breast pain notes that hormonal shifts are a common reason for this kind of soreness.
Progesterone becomes less reliable
In earlier years, progesterone often arrived after ovulation in a fairly predictable pattern. During perimenopause, ovulation may not happen every cycle, or it may happen later than expected. So progesterone is not always there in the same steady way.
That matters because estrogen and progesterone usually work as a pair. When estrogen is more active and progesterone is less consistent, the balance shifts. For some women, that shift shows up as breast tenderness before they even notice other cycle changes.
If you are also seeing sleep changes, mood shifts, or cycle changes, this guide to low estrogen symptoms during perimenopause can help connect the bigger picture.
Tissue sensitivity can make the same hormone shift feel very different
Hormones set the stage, but your breast tissue decides how loudly it reacts. Two women can have a similar month hormonally and feel very different levels of pain.
One reason is inflammation and nerve sensitivity. If the tissue is already more reactive, even a normal amount of swelling can feel sore. Stress, poor sleep, and day-to-day habits can add to that sensitivity, which helps explain why symptoms can flare in one cycle and settle in the next.
Why the pain seems to come out of nowhere
Perimenopause often breaks the old pattern of “symptom, period, relief.” Your cycle may shorten, stretch out, or skip. Breast soreness can follow that same irregular rhythm.
Your own data becomes useful at this stage. If you track breast pain alongside bleeding patterns, sleep, stress, caffeine, workouts, and other symptoms in an app like Lila, you may start to spot your pattern. Maybe soreness peaks after a skipped ovulation month. Maybe it flares during high-stress weeks or when sleep drops off. That kind of tracking gives you something more useful than generic advice. It helps you choose what to change first.
Many women get better results when they pair symptom tracking with supportive habits and, if they want a broader wellness framework, natural hormone balancing strategies that focus on sleep, stress, and daily routines.
Practical rule: Random timing can still fit a hormonal pattern. The pattern just may be visible only after you track it for a few weeks.
Is This Breast Pain Normal for Perimenopause
The most common question behind this symptom is simple. “How do I know if this is typical hormonal soreness or something I need checked?”
That's the right question to ask. Reassurance matters, but clarity matters more.
What typical perimenopause breast pain often looks like
Hormonal breast pain is often diffuse. That means it feels spread out rather than fixed to one tiny point. It may affect both breasts, though sometimes one side feels more noticeable than the other. The sensation is often aching, sore, full, or heavy.
It also tends to fluctuate. Some days are better. Some are worse. You might notice it around cycle changes, during stressful stretches, or during months when your other perimenopause symptoms flare too.
What deserves a medical evaluation
Some patterns are not the kind to watch casually at home. New-onset tenderness after menopause is rare, with incidence listed as under 10%, and it warrants evaluation according to OnStella's menopause breast tenderness guide. The same source says localized pain accompanied by a lump has a 2% to 7% link to cancer.
That doesn't mean every painful lump is cancer. It means that combination deserves proper medical attention.
Here is a simple side-by-side comparison:
Pattern | More typical of hormonal soreness | Needs prompt medical review |
|---|---|---|
Location | Broad, diffuse, hard to pinpoint | One specific spot that stays the same |
Timing | Comes and goes | Persistent or new after menopause |
Feel | Achy, heavy, tender | Focal pain with other breast changes |
Other findings | No major visible changes | Lump, skin change, or unusual nipple symptoms |
Red flags to act on
Call your clinician if you notice any of the following:
A distinct lump with pain especially if it feels new
Pain in one fixed spot that doesn't settle down
Skin changes such as dimpling, puckering, or redness
New breast tenderness after menopause rather than during the transition
If something feels different from your usual pattern, it's worth getting checked. Reassurance from an exam is never wasted.
For women who are facing testing, appointments, or the emotional fog that can come with uncertainty, this piece on the start of a cancer journey may feel grounding and practical.
How to Find Relief from Perimenopause Breast Pain
You wake up, roll onto your side, and your breasts feel heavy, bruised, or strangely full. By afternoon they may calm down, then flare again after a workout, a stressful day, or a bad night of sleep. That pattern can feel random, but relief usually starts once you treat it like a mix of hormone sensitivity and physical irritation.
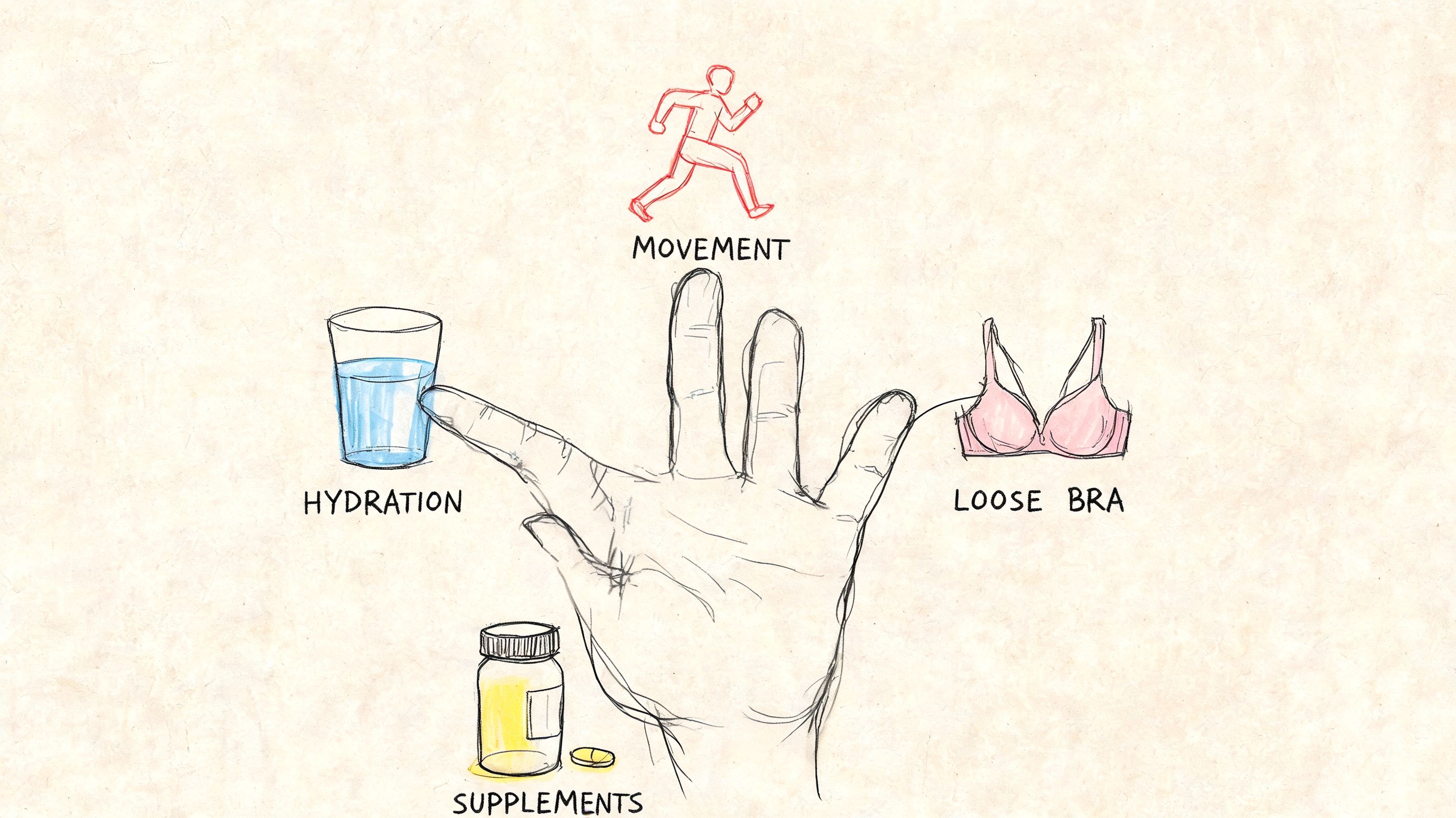
A helpful way to approach breast pain is to work in layers. First reduce friction and pressure. Then look at the habits that may be turning the volume up on pain. If that is not enough, use short-term symptom relief and talk with a clinician about next steps.
According to Cleveland Clinic's guidance on breast pain and menopause, options can include reducing caffeine, lowering stress, trying certain supplements, using over-the-counter pain relievers, and discussing prescription treatment if symptoms are severe.
Start by reducing movement and pressure
Tender breast tissue reacts a bit like a sore ankle. If it keeps getting jostled, compressed, or rubbed, it stays irritated longer.
A few simple changes can make a noticeable difference:
Wear a supportive bra that fits well, especially on days when your breasts feel heavy or swollen
Use a soft sleep bra or supportive crop top if turning in bed makes the pain worse
Skip underwire if it presses into a tender area
Add more support for exercise, since bouncing and friction can amplify soreness even when hormones started the problem
This step is easy to overlook because the symptom feels internal. But external support matters.
Lower the factors that can amplify pain
Hormone shifts may light the match. Stress, poor sleep, and stimulants can keep the fire going.
Some women notice that breast pain is worse during high-caffeine weeks, after several short nights, or when their body feels tense and wired. That does not mean those factors caused the soreness. It means your nervous system and hormone system may be making the same symptom feel stronger.
Try a short, structured experiment:
Cut back on caffeine for two weeks
Prioritize steadier sleep when you can
Use simple stress relief, such as walking, stretching, slower evenings, or brief breathing exercises
Wear softer clothing on flare days to avoid extra pressure and rubbing
The key is to test one or two changes long enough to see whether they help your pattern.
Use symptom relief tools thoughtfully
If support and habit changes are not enough, short-term relief can help you function while you sort out the pattern.
Category | Examples | Best For |
|---|---|---|
Supportive care | Better bra fit, softer sleep support, reducing friction | Daily tenderness and movement-related discomfort |
Lifestyle changes | Caffeine reduction, stress management, gentler routines | Flares that seem tied to sleep, stress, or habits |
Supplements | Evening primrose oil, chasteberry | Women discussing non-prescription options with a clinician |
OTC pain relief | Ibuprofen, naproxen, acetaminophen | Short-term relief when soreness interferes with daily life |
Medical treatment | Prescription options discussed with a doctor | Severe, persistent, or disruptive pain |
A quick visual walk-through can help if you want ideas you can put into practice at home:
Before trying supplements, check with your clinician or pharmacist. “Natural” products can still interact with medications or be the wrong fit for your health history.
Bring your own pattern into the plan
Generic advice only goes so far. Two women can both have sore breasts in perimenopause and need different solutions. One may flare after ovulation-like symptoms. Another may notice the worst pain after poor sleep and intense workouts. Your body's pattern matters more than a general tip list.
That is why tracking can make relief more specific. If you log breast tenderness alongside bleeding changes, sleep, stress, exercise, headaches, and caffeine, you can start to see what shows up together. Tools such as Lila can help you spot those connections, much like using apps to track migraine symptoms helps people identify triggers that memory often misses.
When it is time to talk with a clinician
If breast pain is disrupting sleep, exercise, work, or intimacy, bring it up. A clinician can review whether medications, hormone shifts, cysts, or another breast condition could be contributing, and help you choose treatment based on your symptoms and history.
If hormone treatment becomes part of that conversation, this guide to what hormone therapy for menopause is can make the terminology easier to understand before your appointment.
Relief often comes from a combination of better support, fewer pain triggers, and clearer tracking of what your own body is doing.
Why Tracking Your Symptoms Is a Game Changer
Generic advice has limits. “Cut caffeine.” “Reduce stress.” “Try a better bra.” Good suggestions, yes. But they're much more useful when you know whether they change your pattern.
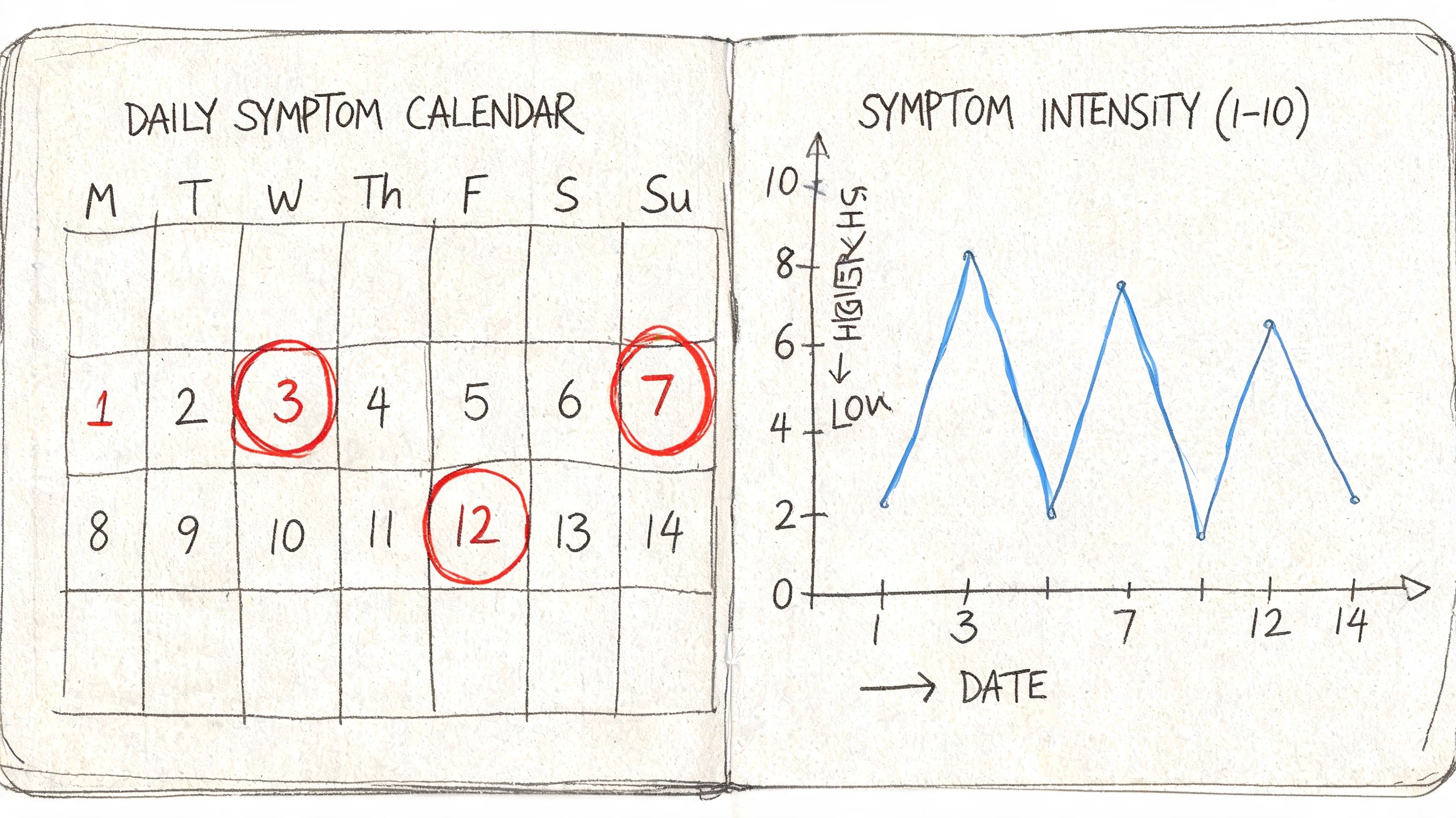
Up to 70% of women experience this pain, but its effect on quality of life is often understated. Tracking can help quantify pain severity and correlate it with other symptoms like sleep disruption and mood changes, as noted in MyAlloy's article on breast pain during perimenopause and menopause.
What tracking reveals that memory misses
Many individuals remember the worst day instead of the entire pattern. That makes sense, but it can distort what's really happening.
Tracking helps you answer questions like:
Does the soreness show up before bleeding starts, or on random days?
Does poor sleep make the next day's tenderness worse?
Do stressful workweeks line up with more intense pain?
Did reducing caffeine help, or did nothing change?
Those answers matter because perimenopause symptoms tend to cluster. Breast tenderness may not be a standalone issue. It may travel with sleep trouble, irritability, bloating, or cycle shifts.
What to track
Keep it simple enough that you'll do it. You don't need a complicated spreadsheet.
A useful symptom log might include:
Pain intensity using your own simple scale
Location such as both breasts, outer breast, nipple area, or one specific spot
Cycle notes if you're still bleeding
Sleep quality
Stress level
Caffeine intake
Exercise and bra support
Other symptoms like mood shifts, bloating, or headaches
This is the same logic people use in other symptom-based conditions. For example, the value of using apps to track migraine symptoms comes from spotting patterns you can't reliably hold in your head. Breast pain in perimenopause benefits from that same personalized approach.
Better data leads to better doctor visits
Symptom tracking also makes appointments more productive. Instead of saying, “My breasts hurt sometimes,” you can say, “It's happening mostly on these days, it's worse after poor sleep, and it improved when I changed this one habit.”
That gives your clinician something concrete to work with. It also helps you notice whether the bigger perimenopause picture is coming into focus. If you're unsure where you are in the transition, this guide on whether you can test for perimenopause can help frame that conversation.
Your own data won't replace medical care. But it can turn a vague complaint into a pattern you can actually act on.
Taking Control of Your Perimenopause Journey
Breast soreness during perimenopause can be unsettling, especially when it appears suddenly or starts behaving differently from the breast tenderness you remember from earlier years. But once you understand the hormonal “why,” the symptom often becomes less mysterious and less frightening.
What helps most is a steady, practical mindset. Know the common hormonal pattern. Know the red flags that deserve prompt evaluation. Then work through relief in a sensible order. Better support, lower irritation, symptom relief when needed, and medical input when the pain is persistent or interfering with daily life.
Just as important, stop relying on memory alone. Perimenopause is uneven by nature. Tracking helps you spot whether your soreness follows sleep changes, cycle shifts, stress, caffeine, or no clear pattern at all. That kind of information makes self-care more precise and medical care more useful.
You don't have to grit your teeth and tolerate this symptom without context. Perimenopause sore breasts are common, real, and manageable. The more clearly you can see your own patterns, the easier it becomes to choose what to try, what to ignore, and when to ask for help.
If you want a simpler way to connect the dots between breast soreness, sleep, mood, stress, and cycle changes, Lila can help you track what your body is doing day to day and turn that information into a more personalized plan. Instead of guessing, you can start seeing patterns and making decisions based on your own data.
You should not have to do it all on your own









