Your Guide to Calming Perimenopause Stomach Problems
Struggling with perimenopause stomach problems? Understand the causes of hormonal bloating and pain, and discover practical strategies for lasting gut relief.

If you're suddenly at war with your own stomach—battling bloating, gas, and pain that seems to come out of nowhere—you are not imagining things. These perimenopause stomach problems are very real, and they're directly tied to the massive hormonal shifts happening inside your body. It's not a vague feeling; it's biology.
Why Does My Stomach Feel So Awful During Perimenopause?
If your digestive system suddenly feels like it's gone completely haywire, you're in the right place. The uncomfortable truth is that the hormonal chaos of perimenopause often makes its grand entrance right in your gut. So many women are caught off guard by this, chalking up the new symptoms to a sudden food intolerance or just a normal part of getting older.
But there’s a much more specific reason for your discomfort. Think of your digestive system as a finely tuned orchestra that has played in harmony for decades. Now, during perimenopause, the main conductors—your hormones estrogen and progesterone—start sending erratic and unpredictable cues, throwing the entire performance into disarray.
The Hormone-Gut Connection
These hormonal fluctuations are the primary culprits behind most new digestive woes in midlife. Here’s a quick breakdown of what’s really going on:
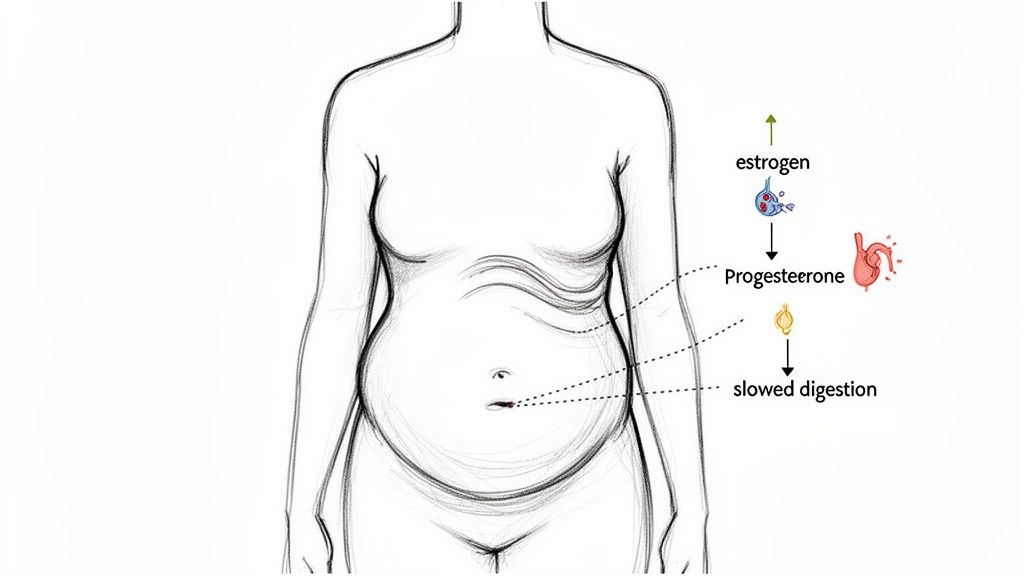
Estrogen's Role: This key hormone does more than you think. It helps regulate fluid balance and even manages cortisol (the stress hormone). As estrogen levels become unpredictable and decline, your body can start retaining more water and digestion can slow down.
Progesterone's Impact: Progesterone is known for its calming effect on smooth muscles, including the ones that line your intestines. When progesterone levels drop, it can slow the movement of food through your digestive tract, creating a "traffic jam" effect.
This combination is a perfect storm for digestive trouble. When food moves too slowly, it sits in your gut longer, where it ferments and produces excess gas. This leads directly to that all-too-familiar feeling of bloating, pressure, and general discomfort.
It's worth repeating: your experience is far from unusual. For many women, the digestive system is one of the very first places they notice the effects of perimenopause—sometimes even before classic symptoms like hot flashes show up.
You Are Definitely Not Alone
If it feels like your stomach is constantly giving you grief, you're in good company. The number of perimenopausal women dealing with gastrointestinal symptoms is incredibly high.
One major study revealed that nearly 94% of women in this stage report digestive health issues. Of those women, a staggering 77% experience bloating, 54% deal with constipation, and 50% suffer from stomach pain. Yet, despite how common these problems are, they often go unaddressed.
Common Perimenopause Stomach Problems and Their Hormonal Links
To help you connect the dots, this table breaks down the most common gut symptoms women report during perimenopause and links them back to the likely hormonal drivers.
Symptom | Primary Hormonal Driver(s) | Common Experience |
|---|---|---|
Bloating & Gas | Fluctuating Estrogen & Progesterone | A feeling of fullness, pressure, or a visibly distended belly, often worsening as the day goes on. Caused by slowed digestion and water retention. |
Constipation | Low Progesterone | Difficulty passing stools or infrequent bowel movements. Progesterone's decline slows intestinal muscle contractions. |
Diarrhea | Fluctuating Estrogen & Cortisol | Sudden, urgent, and loose bowel movements. Can be linked to estrogen's impact on the stress hormone cortisol, which can speed up gut motility. |
Stomach Pain & Cramping | Prostaglandins, Estrogen | Aching, sharp, or cramp-like pains in the abdomen. Hormonal changes can increase sensitivity and inflammation in the gut. |
Acid Reflux / Heartburn | Low Estrogen | A burning sensation in the chest. Estrogen helps regulate stomach acid and the muscle that keeps acid down; fluctuations can weaken it. |
Seeing your symptoms listed here can be a relief. It confirms that what you're experiencing is a recognized part of the perimenopausal transition, not just random discomfort.
From Discomfort to Empowerment
Recognizing that your gut issues are a valid part of the perimenopause journey is the first step toward feeling better. It means what you're feeling isn't "all in your head"—it's a direct result of biology. These digestive troubles are just a few of the many changes you might experience; you can learn more by exploring the 34 symptoms of perimenopause in our comprehensive guide.
This knowledge shifts the narrative from confusion and frustration to clear, focused action. Once you understand the root causes, you can start exploring targeted strategies that work with your body instead of against it.
The Four Main Drivers of Your Digestive Discomfort
To get a real handle on stomach problems during perimenopause, we have to look under the hood. While hormones are the main culprits, they kick off a cascade of events that can throw your entire digestive system into chaos. Let's walk through the four key factors behind your discomfort, using some simple analogies to picture what’s really going on.
1. Hormonal Fluctuations: The Unpredictable Conductors
Think of your digestive system as a finely tuned orchestra. For years, the conductors—estrogen and progesterone—have kept a steady, predictable rhythm. But during perimenopause, they start missing cues and changing the tempo erratically.
Estrogen’s role: Estrogen is like the stage crew, responsible for maintaining the integrity of the concert hall itself—your gut lining. It also helps manage fluid balance. As estrogen levels bounce around, the gut lining can become weaker and more sensitive. At the same time, your body might start retaining water, which is where that frustrating, puffy bloating comes from.
Progesterone’s role: Progesterone has always been the metronome, setting a calm, consistent pace for digestion. It has a natural relaxing effect on the smooth muscles in your intestines. When progesterone levels drop, this relaxation can go overboard, creating a major digestive traffic jam. Food starts moving much more slowly, leading to constipation, trapped gas, and that uncomfortably full feeling.
2. The Microbiome Shift: An Unbalanced Internal Garden
Your gut is home to trillions of microorganisms, a complex community we call the gut microbiome. The best way to picture it is as a garden, where helpful bacteria (the "flowers") and less-helpful microbes (the "weeds") live together. In a healthy gut, the flowers are thriving, helping you digest food and keeping the weeds in check.
The hormonal swings of perimenopause, particularly the drop in estrogen, really disrupt this delicate balance. Estrogen is known to support the diversity of your good gut bacteria. When it plummets, it's like a drought hits your garden. The flowers wither, giving the opportunistic "weeds"—unhelpful bacteria and yeasts—a chance to take over.
These overgrown weeds are notorious for fermenting undigested food, producing significant amounts of gas. This is often the direct cause of the embarrassing and uncomfortable gas and severe bloating that seem to appear from nowhere during perimenopause.
3. The Gut-Brain Connection: Panic Signals From Headquarters
There's a constant, two-way communication line between your brain and your gut, often called the gut-brain axis. It's like a direct hotline between headquarters (your brain) and the factory floor (your gut). When things are calm upstairs, operations run smoothly down below.
The problem is, perimenopause often brings a surge in stress and anxiety. This causes your body to pump out more of the stress hormone, cortisol, which then sends "panic signals" down the hotline to your gut. Your digestive system responds to this perceived emergency by either speeding up (hello, diarrhea) or grinding to a halt (leading to constipation and cramping). This also ramps up your gut’s sensitivity—a phenomenon known as visceral hypersensitivity—meaning you suddenly feel pain from normal digestive rumbles you never used to notice.
It's a frustrating feedback loop:
Stress and anxiety trigger gut symptoms.
Painful gut symptoms cause even more stress.
The cycle repeats, getting worse each time.
4. Lifestyle Accelerants: Adding Fuel to the Fire
Finally, certain changes in our daily habits during this phase can pour gasoline on the fire. These aren't the root cause of your gut issues, but they can definitely make everything feel much worse.
Dietary Shifts: When you're dealing with mood swings or fatigue, it’s natural to crave comfort foods, often those high in sugar or simple carbs. Unfortunately, these are the very foods that feed the "weedy" bacteria in your gut, worsening gas and bloating.
Reduced Physical Activity: Let's be honest, when you feel bloated and tired, a workout is often the last thing on your mind. But less movement slows down your gut motility even further, directly contributing to constipation.
Poor Sleep: Perimenopause is famous for wrecking sleep. That lack of quality rest sends your cortisol levels soaring, which, as we just saw, shoots those panic signals straight to your gut.
These four drivers don't work in isolation; they team up to create a perfect storm of digestive distress. But understanding how they interact is the first, most powerful step toward taking back control and feeling like yourself again.
Is It Perimenopause or Another Gut Condition?
▶ PlayWhen your stomach starts acting up out of the blue, it’s completely normal to wonder: is this just perimenopause, or is something else going on? The truth is, the symptoms of perimenopause-related gut issues can look a lot like other common gastrointestinal (GI) conditions, making it tricky to tell them apart.
That nagging bloat, unpredictable gas, and seesawing bowel habits? They’re classic signs of both hormonal shifts and conditions like Irritable Bowel Syndrome (IBS). Similarly, the burning sensation rising in your chest could be hormone-driven reflux or a more chronic case of Gastroesophageal Reflux Disease (GERD).
My goal here isn't for you to self-diagnose, but to give you the knowledge to have a more informed, productive conversation with your doctor. Understanding the overlaps is the first step.
Common Symptom Overlaps
Many women in their 40s and 50s find themselves dealing with digestive drama that perfectly mirrors the symptoms of well-known GI disorders. Let’s break down the most common areas of confusion.
Irritable Bowel Syndrome (IBS): This condition is defined by a frustrating mix of abdominal pain, cramping, bloating, gas, diarrhea, and constipation. Sound familiar? The hormonal rollercoaster of perimenopause can either kickstart these symptoms or make existing ones much worse. It often leaves women wondering if they’ve suddenly developed IBS.
Gastroesophageal Reflux Disease (GERD): As estrogen levels drop, the muscle that acts as a gate between your esophagus and stomach (the lower esophageal sphincter) can become a bit lazy. This allows stomach acid to splash back up, causing heartburn. If you're popping antacids more than twice a week, it might be more than just a fleeting hormonal symptom and could be GERD.
New Food Intolerances: Suddenly struggling with foods you’ve enjoyed your whole life? Slower digestion and shifts in your gut microbiome during perimenopause can make it harder for your body to process things like dairy (lactose) or gluten. This can lead to gas and bloating that feels exactly like a newly developed food intolerance.
This diagram shows how hormones, the gut microbiome, and even stress can team up to create a perfect storm for digestive trouble during perimenopause.
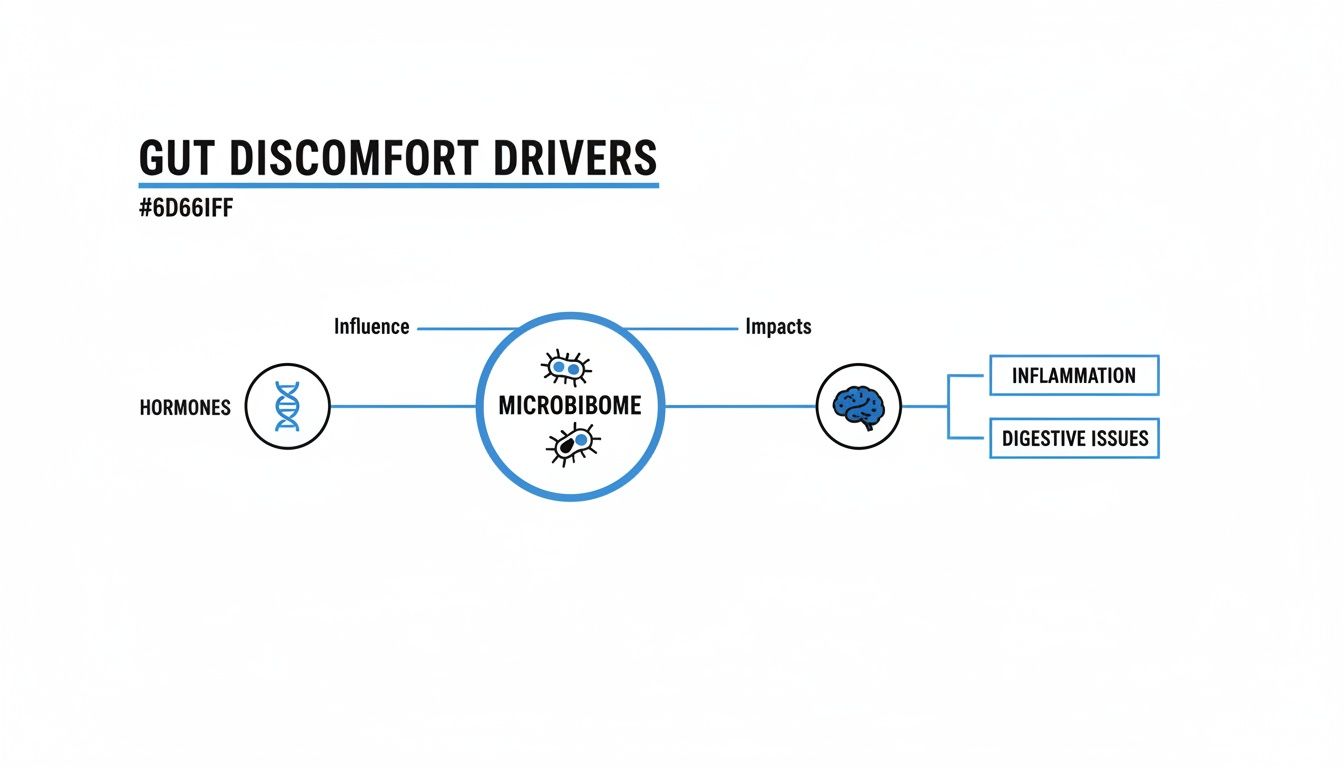
As you can see, fluctuating hormones are often the root cause, setting off a chain reaction that affects your gut bacteria and your stress response. If you're experiencing nausea specifically, our guide on can menopause cause nausea offers a more focused look.
Symptom Checker: Perimenopause vs. Other GI Conditions
Trying to figure out what's "normal" for perimenopause versus what might be a sign of something else can be confusing. This table is designed to help you spot some key differences, not for diagnosis, but to help you better understand your body's signals.
Symptom | Typical in Perimenopause | May Indicate Another Condition (e.g., IBS, GERD, SIBO) | When to See a Doctor |
|---|---|---|---|
Bloating/Gas | Often cyclical; may worsen before your period. Comes and goes. | Persistent, severe, or accompanied by significant pain or distention. | If it's new, severe, and doesn't improve with simple lifestyle changes. |
Heartburn | Occasional episodes, especially after certain foods or when lying down. | Occurs more than twice a week; wakes you up at night; difficult to manage. | For frequent symptoms, as chronic reflux can damage the esophagus. |
Bowel Changes | Fluctuates between mild constipation and looser stools, often tied to your cycle. | Chronic diarrhea or constipation lasting weeks; extreme urgency. | If changes are sudden, severe, or accompanied by other red flags. |
Abdominal Pain | Mild, crampy discomfort that is usually manageable. | Severe, sharp, or localized pain that doesn't go away. | Any severe or persistent abdominal pain warrants a visit. |
Nausea | Mild, intermittent waves of queasiness, sometimes in the morning. | Persistent nausea or vomiting that interferes with eating or daily life. | If you are vomiting frequently or experiencing unexplained weight loss. |
Remember, this is just a guide. Your experience is unique, and the best person to help you connect the dots is your healthcare provider.
When to See a Doctor
While a bit of gut turmoil is a common companion during the perimenopause transition, some symptoms should always be taken seriously. Think of them as "red flags" that signal the need for a professional evaluation.
Your body is giving you important signals. While mild, intermittent bloating is common, persistent, severe, or worsening symptoms are your cue to seek professional medical advice.
It's time to schedule a visit with your doctor if you experience any of the following:
Unexplained Weight Loss: Losing weight without changing your diet or exercise routine.
Blood in Your Stool: This is never normal and needs immediate investigation.
Severe or Worsening Abdominal Pain: Pain that is intense, doesn't go away, or gets progressively worse.
Difficulty Swallowing: A sensation of food getting stuck can indicate an issue with your esophagus.
Persistent Nausea or Vomiting: Occasional nausea is one thing, but frequent vomiting is a definite red flag.
The link between this life stage and gut issues is becoming clearer with research. Studies show menopausal women are 2.9 times more likely to have GERD symptoms, with 42% of perimenopausal women reporting distress in their upper GI tract.
If you're trying to figure out if your symptoms are driven by hormonal shifts, options like at home hormone testing can offer valuable clues. These tests can help clarify if hormonal fluctuations are a major factor in your discomfort, giving you and your doctor a better starting point.
Your Action Plan for a Calmer Gut

Understanding the "why" behind your perimenopause stomach problems is a great first step. But turning that knowledge into action is where you'll find real relief. Think of this as your practical roadmap to feeling better, built on three core pillars: diet, lifestyle, and smart support.
If your gut has been acting up, you are far from alone. Research shows that about 55% of menopausal women deal with digestive issues every day or week. An equal percentage say these problems seriously mess with their quality of life. The good news? A whopping 89% of women are already taking control with dietary changes and stress management, which tells us that we’re motivated to find solutions that work. You can read more about it in this report on menopause and gut health.
This proactive mindset is exactly what we need. Let’s build a plan to calm your gut that you can actually stick with.
Pillar 1: Your Dietary Strategy
What you eat is probably the most powerful tool you have for managing digestive issues. But this isn't about harsh restrictions. It’s about making strategic additions and smart swaps to support your gut through this transition.
Go Slow with Fiber: Fiber is fantastic for keeping you regular, but adding too much too quickly can backfire, causing even more bloating and gas. Think evolution, not revolution. Gently increase your intake of soluble fiber from foods like oats, apples, and carrots, which helps soften stool and make it easier to pass.
Embrace Gut-Friendly Foods: Think of it as tending to your internal garden. You want to nurture the good stuff with probiotics and prebiotics. Probiotic-rich foods like plain yogurt, kefir, and kimchi introduce beneficial bacteria. Then, feed those good bugs with prebiotic foods like garlic, onions, and bananas.
Pinpoint Your Personal Triggers: It’s a strange reality of perimenopause: you might suddenly start reacting to foods you’ve eaten your whole life. Dairy, gluten, and even high-sugar foods are common culprits. Instead of cutting everything out at once, start paying close attention to how you feel after meals to identify your unique triggers. A structured approach, like our 5-day perimenopause diet plan to boost well-being, can be a great starting point.
Pillar 2: Lifestyle and Stress Management
During perimenopause, the connection between your brain and your gut becomes extra sensitive. This means managing stress is no longer just a nice-to-have—it's a core strategy for digestive health. When you calm your mind, you send a powerful "all clear" signal straight to your gut.
Practice Mindful Eating: It sounds simple, but it works. Slow down. Chew your food thoroughly. This easy habit reduces the amount of air you swallow (a common cause of bloating) and gives your digestive enzymes a head start, easing the overall burden on your system.
Incorporate Gentle Movement: You don't need to run a marathon. A daily 20-30 minute walk, some gentle yoga, or stretching can work wonders. This type of movement helps stimulate gut motility, which can relieve constipation and help move trapped gas along.
Use Simple Breathing Exercises: The next time you feel a cramp or bloating coming on, try box breathing. Inhale for a count of four, hold your breath for four, exhale for four, and hold again for four. This technique helps calm your nervous system and can quickly dial down stress-induced gut spasms.
Key Insight: Your action plan isn't just about what you eat; it's about how you live. Combining gentle nutrition with stress-reducing lifestyle habits creates a powerful synergy that addresses both the physical and emotional drivers of perimenopause stomach problems.
Pillar 3: Smart Supplementation and Support
While diet and lifestyle changes are your foundation, a few targeted supplements might offer that extra layer of support. The key here is to approach this step wisely and with professional guidance.
Since hormonal shifts are at the root of so many perimenopausal digestive woes, a crucial part of any long-term plan is to balance hormones naturally.
Here are a few options worth discussing with your doctor:
Magnesium: This essential mineral can have a gentle laxative effect by drawing water into the intestines, making it particularly helpful for constipation during perimenopause. Magnesium glycinate is often a well-tolerated form that's less likely to cause digestive upset.
Peppermint Oil Capsules: For cramping and bloating, enteric-coated peppermint oil can be a lifesaver. The coating ensures the oil is released in the intestines, not the stomach, where it can relax the gut muscles and provide relief.
Probiotics: A high-quality probiotic supplement can help repopulate your gut with beneficial bacteria, which may help reduce gas and bloating.
Always consult with your doctor or a qualified healthcare provider before starting any new supplement. They can help you choose the right option and dosage for your specific situation and make sure it won’t interfere with any medications you're taking. This three-pillar approach gives you a structured, manageable way to take back control and find lasting relief.
How Tracking Can Uncover Your Personal Triggers
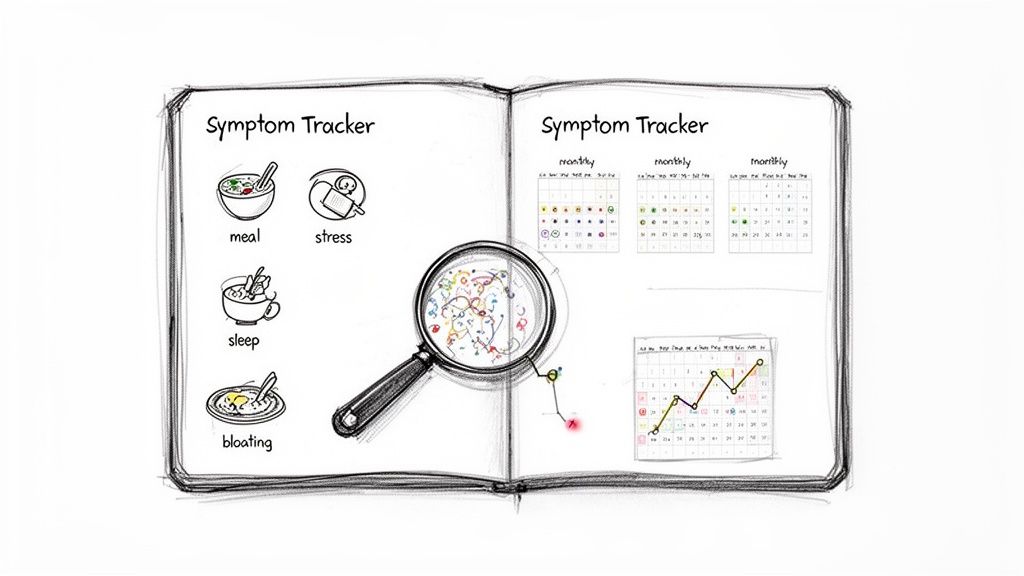
Because perimenopause unfolds differently for everyone, managing symptoms can feel like a frustrating game of trial and error. What works wonders for one person might do absolutely nothing for you. This is especially true for perimenopause stomach problems, where your specific triggers are completely unique. The key is to stop guessing and start gathering your own data.
By becoming a detective for your own body, you can shift from feeling powerless to feeling in control. Consistently tracking key variables—what you eat, how stressed you feel, your sleep quality, and your digestive symptoms—helps you connect the dots. You might assume your evening bloat is from dinner, but what if it’s actually tied to the stress of your morning commute plus your afternoon coffee?
These kinds of connections are nearly impossible to spot without a record. While a simple notebook can work, a dedicated app makes the process much simpler, helping you log information in seconds and spot trends over time.
From Data Points to Clear Patterns
The whole point of tracking is to build personalized evidence. After just a few weeks, the information you've gathered starts to tell a clear story about your body. You're no longer dealing with "random" bloating; you're seeing how specific inputs lead to specific outcomes.
This process helps you identify things like:
Trigger Foods: You might discover that bloating is consistently worse on days you eat dairy or gluten.
Stress Impact: Perhaps you’ll see a clear link between high-stress workdays and painful cramps in the evening.
Hormonal Cycles: Tracking alongside your menstrual cycle might show that your stomach issues flare up in the days before your period.
The Sleep Connection: A night of poor sleep often means higher cortisol, which you might see reflected in more indigestion the next day.
By logging your daily inputs and outputs, you create a personalized roadmap. This data is what transforms you from a passive sufferer into an active participant in your own wellness, armed with the knowledge to make targeted changes.
Making Tracking Work for You
The real power of this approach is its precision. Instead of overhauling your entire diet and lifestyle at once, you can make small, informed adjustments based on your own data. For instance, if you confirm that caffeine is a major trigger for your heartburn, you can try switching to herbal tea and see if your symptoms improve.
Tracking takes the guesswork out of feeling better. When you consistently check in, you create a feedback loop that highlights correlations you might have missed. This is what makes the process so effective—it helps you move from guessing what's wrong to knowing exactly what works for your body.
Common Questions About Perimenopause and Digestion
When you're dealing with perimenopause stomach problems, it's natural to have a lot of questions. Getting clear, expert-backed answers can bring a huge sense of relief and give you a path forward. Let's tackle some of the most common things women ask about their digestion during this time.
Can Hormone Replacement Therapy Improve My Gut Issues?
For many women, yes, it absolutely can. Since the root cause of so many of these new gut issues is plunging and chaotic estrogen, stabilizing your hormones with Hormone Replacement Therapy (HRT) can make a world of difference. Restoring estrogen helps get your gut motility back on track, tames water retention, and supports a healthier gut microbiome, which often means much less bloating, constipation, and reflux.
That said, HRT isn't a magic bullet for everyone. Its effectiveness can vary based on the specific type and dose, and it isn’t the right choice for every woman. This is a conversation you absolutely must have with your doctor to weigh the pros and cons and see if it's a safe and appropriate option for you.
How Long Do These Digestive Problems Typically Last?
This is the million-dollar question, and unfortunately, the answer is deeply personal. Perimenopause itself can last anywhere from a few years to over a decade. Most women find their digestive symptoms come and go, often mirroring the wild unpredictability of their hormones.
The good news? These perimenopause stomach problems don't have to be your new normal forever. Once you transition into postmenopause and your hormones settle into their new, lower baseline, many of the most frustrating symptoms tend to calm down. Even better, by making targeted changes to your diet and lifestyle now, you can find significant relief long before perimenopause is over.
Is It Normal for New Food Sensitivities to Appear?
Yes, it's surprisingly common to suddenly have trouble with foods you've eaten your whole life without a second thought. As estrogen levels drop, it can slow down your entire digestive tract and change the makeup of your gut bacteria. This can make it much harder for your body to break down things like lactose (in dairy) or even gluten (in wheat), leading to gas, bloating, and discomfort you've never had before.
You’re not imagining it. Foods that were once your go-to favorites can suddenly feel like your gut's worst enemy during perimenopause. This is a direct result of hormonal shifts messing with how well your gut can process them.
Why Does Bloating Seem Worse Around My Period Now?
If you feel like you inflate like a balloon in the days before you bleed, you're experiencing a classic perimenopause pattern. Even in a regular menstrual cycle, pre-period hormonal shifts cause some water retention and bloating. But in perimenopause, those hormonal swings can be far more dramatic and extreme, super-sizing all those premenstrual symptoms—including that awful, painful bloating.
Trying to figure all this out can feel like a lonely, full-time job. But you don't have to go it alone. Lila is an AI-powered app built to help you connect the dots between your unique symptoms, including all these digestive issues. By tracking what you eat, your stress levels, and how you feel, you can finally pinpoint your personal triggers and get a clear action plan for relief. Take the first step toward a happier gut and start your journey with Lila today.
Get Lila, your personal coach for perimenopause.
Built for women in their 40s. 24/7 coaching, in your pocket.


