Gas and Menopause Your Guide to Beating Bloat
Struggling with gas and menopause? Learn the hormonal link behind bloating and discover actionable diet, lifestyle, and tracking strategies for lasting relief.

If you've noticed a sudden uptick in gas and bloating as you navigate menopause, you’re not imagining it—and you're certainly not alone. There's a very real biological reason for this uncomfortable shift, and it all comes back to your hormones.
Think of estrogen and progesterone as the behind-the-scenes managers of your digestive tract. For years, they've kept things running smoothly and predictably. But as their levels start to fluctuate and decline during perimenopause and menopause, that well-oiled system can become sluggish and a lot less predictable.
Why Gas and Bloating Are Common in Menopause
Among the many surprising symptoms that can crop up during the menopausal transition, a significant increase in gas and bloating is one of the most frequently reported. The hormonal upheaval your body is going through doesn't just impact your reproductive cycle; it sends ripple effects throughout your entire system, with your gut being one of the most sensitive areas.
The Hormonal Slowdown Effect
The main culprit behind the surge in gas and menopause symptoms is the drop in estrogen. Estrogen does more than you might think, including helping to regulate gut motility—the coordinated muscle contractions that push food along your digestive tract.
Imagine your digestive system is a busy highway. When estrogen is at its usual level, traffic flows efficiently. But as estrogen levels fall, it’s like suddenly closing off a few lanes. Everything slows down, creating a digestive traffic jam.
This slowdown has a direct and gassy consequence. Food ends up sitting in your intestines for longer than it should, giving gut bacteria extra time to ferment it. While fermentation is a normal part of digestion, a prolonged process produces a lot more gas. The result is that uncomfortable, trapped feeling of bloating and a noticeable increase in flatulence.
To put it simply, key hormonal changes during menopause can throw your digestive system for a loop. Here's a quick summary of how it all connects.
How Hormones Impact Your Digestion
Hormonal Change | Impact on Your Gut | Resulting Symptom |
|---|---|---|
Declining Estrogen | Slows gut motility (the speed of digestion). | Food ferments longer, creating excess gas and bloating. |
Hormonal Fluctuations | Disrupts the balance of your gut microbiome. | An overgrowth of gas-producing bacteria and lower microbial diversity. |
Declining Progesterone | Can contribute to fluid retention in the body. | Worsens the sensation of abdominal fullness and distension. |
Understanding these direct links is often the first step toward feeling validated and taking control of your symptoms.
Changes to Your Gut Microbiome
The hormonal roller coaster does more than just slow things down; it can actually change the environment inside your gut. Your gut microbiome is a complex community of trillions of bacteria, and hormones play a key role in keeping this delicate ecosystem in balance. During menopause, that balance can be thrown off.
This internal shift can trigger a few specific problems:
An Overgrowth of Gassy Bacteria: Certain types of gut bacteria are naturally more inclined to produce gas. Hormonal changes can create conditions that allow these particular strains to thrive and multiply.
Less Microbial Diversity: A healthy gut is home to a wide and diverse range of bacteria. Menopause can sometimes lead to a less diverse microbiome, a state often linked to digestive problems like bloating and increased sensitivity.
New Food Sensitivities: You might suddenly find that foods you’ve eaten your whole life without a problem now trigger immediate discomfort. This isn’t a true allergy but a new sensitivity, likely brought on by your digestive system's altered state.
Finally, falling estrogen and progesterone levels can also encourage your body to hold onto more water. This fluid retention can compound the feeling of abdominal fullness, making bloating feel even more pronounced. Getting to the root of this "why" is the foundation for finding strategies that genuinely work.
If you've ever found yourself wondering, "Why am I suddenly so gassy and bloated?" you're not alone. To get to the bottom of menopause gas, we have to talk about hormones—specifically, the connection between estrogen and your gut.
Your entire digestive system is equipped with estrogen receptors. Think of them as tiny docking stations. When you have plenty of estrogen, these stations get the signals they need to keep everything running smoothly. But as estrogen levels drop during perimenopause and menopause, those signals become weaker and less frequent, throwing a wrench in your digestive works.
This hormonal shift also has a sneaky side effect: it can cause your cortisol levels to spike. Cortisol is your body's main stress hormone, and when it’s high, it directly makes digestive problems worse. It’s a vicious cycle—hormonal changes create digestive distress, which causes stress, which in turn makes your gut feel even more out of whack.
Why Digestion Slows to a Crawl
One of the biggest culprits behind menopause gas is a slowdown in gut motility. This is just a technical term for the muscle contractions that push food along your digestive tract. When estrogen was plentiful, this process was like a well-oiled assembly line, moving things along at a steady pace.
Now, with less estrogen, that assembly line has slowed way down. Food sits in your intestines for much longer than it should, giving your gut bacteria extra time to ferment it. The result? A whole lot of extra gas.
This diagram helps visualize how the dominoes fall, starting with that initial drop in estrogen.
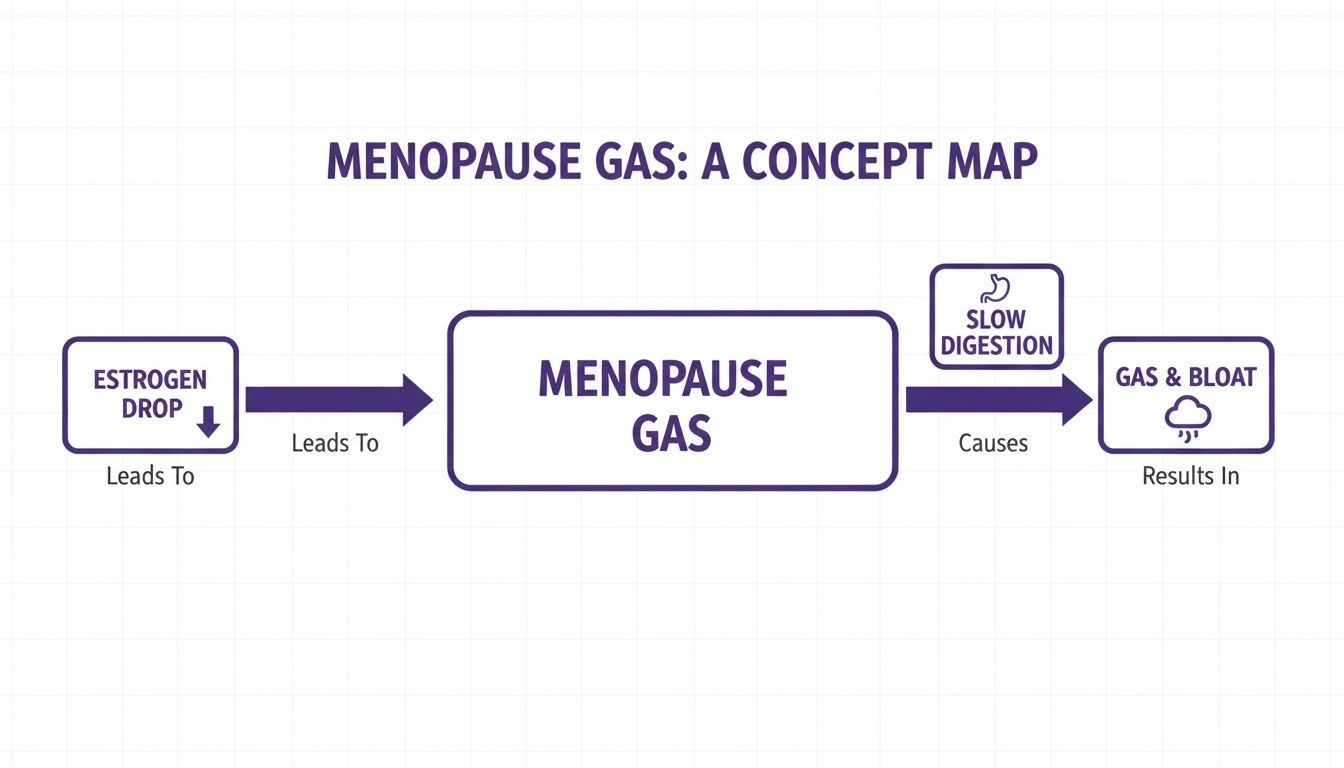
But your hormones aren't working in isolation. This is where the gut-brain axis—the constant two-way highway of communication between your gut and your brain—comes into play. The anxiety, mood swings, and poor sleep that often accompany menopause send stress signals straight down to your gut. These signals can slow digestion even more and make you physically more sensitive to the gas and bloating you’re already experiencing.
You end up stuck in a frustrating feedback loop. Hormonal dips cause gut problems, which then mess with your mood and sleep, which then makes the digestive issues even worse. Figuring out how to step out of that cycle is the key to feeling better.
This Is a Global Health Conversation
If it feels like you're the only one dealing with this, I can assure you, you are not. This is a massive, global issue. As our population ages, the number of women navigating menopause is growing every year.
In fact, the World Health Organization reported that by 2021, women over 50 made up 26% of all females worldwide. And with the average 60-year-old woman expected to live another 21 years, the long-term impact of symptoms like intestinal gas becomes a major quality-of-life issue.
For some women, exploring natural supplements for managing hormonal changes during menopause can offer support alongside other lifestyle changes. The first step is simply understanding what’s happening in your body. When you know the why behind your symptoms, you can stop feeling confused and start taking targeted, effective action.
Identifying Common Bloating Triggers
Okay, so we’ve established that hormonal shifts are a major player in that frustrating gas and bloating. But the story doesn't end there. Now, it’s time to connect those internal changes to what’s happening in your daily life. Think of this as getting to know your body on a deeper level—finding the specific, everyday things that might be making your symptoms flare up.
It can feel overwhelming, but breaking it down makes it much more manageable. When you start paying close attention to what you eat, how you move, and even your stress levels, you’ll begin to spot patterns you never noticed before. This is where you take back control.
Dietary Culprits to Watch For
More often than not, the most obvious place to start looking for answers is your plate. As digestion slows down during menopause, foods that you’ve eaten for years without a problem can suddenly cause a lot of discomfort. The trick is to become mindful of how your body is reacting.
Some of the most common dietary triggers include:
Carbonated Drinks: That fizz you love in seltzer or soda? It's literally just gas. Swallowing all those bubbles can lead to almost instant bloating as they get trapped in your digestive tract.
Artificial Sweeteners: Sugar alcohols like sorbitol and xylitol—often found in "sugar-free" gums, candies, and snacks—are notoriously difficult for our gut to break down. For many, this leads to significant gas and cramping.
High-FODMAP Foods: This is a big category of fermentable carbs that gut bacteria absolutely love. While super healthy, things like beans, lentils, onions, garlic, cabbage, and even some fruits like apples can produce a ton of gas in a sensitive system. Learning more about which foods support you during menopause can help you choose options that work with your body, not against it.
Lifestyle Factors and Medication Side Effects
What happens outside the kitchen plays a massive role, too. Stress is a well-known gut disruptor; it floods your body with cortisol, which can slam the brakes on healthy digestion. Simply eating too fast or while you’re distracted means you're swallowing extra air and not chewing thoroughly, giving your gut even more work to do.
Consider this: When you're stressed or rushed, your body enters "fight-or-flight" mode. Digestion is not a priority in this state. Taking a few deep breaths before a meal can switch you back to "rest-and-digest" mode, making a significant difference.
Even a lack of gentle movement can be a trigger. A simple walk after a meal does wonders for stimulating your gut and helping trapped gas move along. And finally, don’t forget to check your medicine cabinet. Certain supplements (especially iron) and some prescription drugs can list digestive upset as a common side effect. Just becoming aware of these connections is a huge first step toward feeling better.
Your Action Plan for Managing Menopause Gas
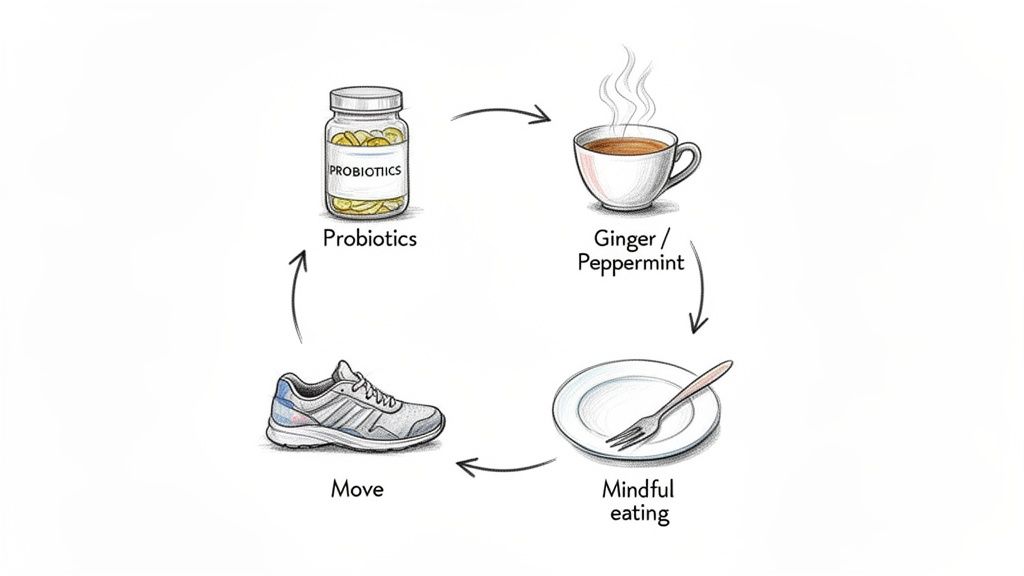
Knowing why you’re suddenly so gassy during menopause is one thing, but knowing what to do about it is everything. Let's move from understanding the problem to taking real, practical steps. This simple plan is based on evidence and gives you actions you can start today to find some relief.
Think of this less as a strict set of rules and more as a series of mindful upgrades to your daily life. It’s amazing how small, consistent tweaks can make a world of difference to your digestive comfort.
Smart Dietary Adjustments
Rather than immediately cutting things out and feeling deprived, let’s focus on what you can add to your diet. Bringing in more gut-friendly foods and drinks can help calm your system down and counteract the sluggishness that hormonal shifts often cause.
Here are a few powerful additions to consider:
Probiotic-Rich Foods: Start incorporating things like yogurt, kefir, and kimchi. These foods are packed with beneficial bacteria that help restore balance to your gut microbiome, which can get thrown out of whack during this time.
Soothing Teas: A warm cup of ginger or peppermint tea after a meal can be a game-changer. Both are well-known for helping relax the intestinal muscles, allowing trapped gas to find its way out.
Gentle Soluble Fiber: Fiber is your friend, but adding too much, too fast, can definitely backfire. The key is to gradually increase soluble fiber from sources like oats, psyllium husk, and carrots. This type of fiber forms a gel-like substance in your gut, which helps soften stool and keep you regular without creating a ton of extra gas.
As you build your plan, researching the right probiotic for menopause can offer targeted support, not just for your gut but for your overall well-being during this transition.
Mindful Eating Habits
Sometimes, how you eat is just as important as what you eat. When we rush through meals, we’re not just swallowing our food—we’re swallowing air, which puts extra pressure on our digestive system.
When you eat in a stressed or hurried state, your body diverts energy away from digestion. Creating a calm environment for meals signals to your gut that it's safe to "rest and digest," improving function and reducing discomfort.
Try putting these simple habits into practice:
Chew Thoroughly: Digestion truly begins in the mouth. When you take the time to chew your food completely, you’re mechanically breaking it down and mixing it with enzymes, giving your stomach a much-needed head start.
Eat in a Relaxed State: This one is huge. Step away from your desk, turn off the news, and just take a few deep breaths before your first bite. This simple pause can make a significant difference in how your body processes your meal.
Gentle Movement and Exercise
You don’t have to run a marathon to get digestive relief. In fact, gentle movement is one of the best tools you have for easing the discomfort of menopause-related gas.
A simple 10-15 minute walk after eating helps stimulate your gut, physically encouraging any trapped gas to move along and out of your system. Other regular, low-impact activities like yoga or swimming are fantastic, too. They not only support digestive regularity but also help manage stress—another major trigger for gut issues. For more ideas, check out our guide to natural remedies for bloating.
By weaving these small but meaningful changes into your routine, you create a powerful wellness cycle that supports better digestion and offers lasting relief.
How Smart Tracking Can Pinpoint Your Triggers
Trying to figure out what’s causing your gas and bloating during perimenopause can feel like a frustrating guessing game. One day, you blame the lentils you had for dinner. The next, you eat the same thing and feel perfectly fine. It's confusing, and honestly, this kind of guesswork rarely leads to real, lasting relief.
Think of it this way: if your car engine was making a strange noise, you wouldn't just guess what's wrong. You'd want a diagnostic tool to see the root cause. A smart tracking app works the same way for your body, helping you move beyond generic advice to find what’s really going on with you.
From Guesswork to Clear Answers
This is where dedicated tools like the Lila app can make a world of difference. By taking a few moments to log key details about your day, you start building a personal health story. Behind the scenes, the app’s intelligence can analyze this data to find connections your brain would almost certainly miss.
The process is simple but incredibly effective:
Log Your Day: Quickly record what you ate, how you slept, your mood, and how severe your symptoms are.
Find Hidden Connections: The system then gets to work connecting the dots. It might discover your bloating always flares up two days after a poor night's sleep, or that a certain breakfast food leads to afternoon gas.
Get Personalized Insights: Instead of just having a vague hunch, you get clear, data-backed feedback on your unique triggers.
This allows you to see all your health data in one place, making it easier to connect the dots between your daily habits and how you feel.
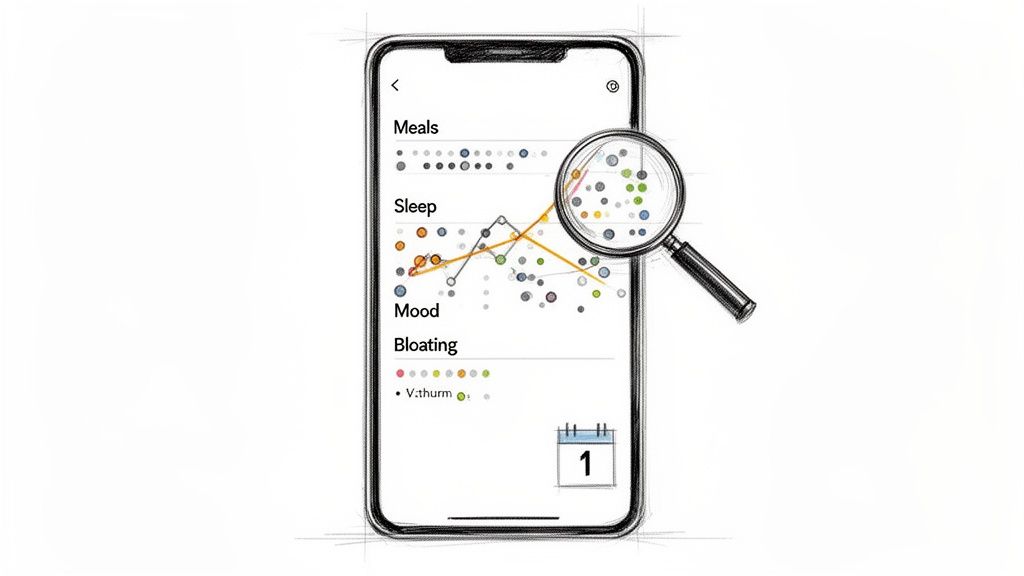
Suddenly, those abstract feelings and frustrating symptoms become concrete data points you can actually work with.
Turning Insights Into Action
This data-driven approach is vital because digestive issues are so often misunderstood during this life stage. A 2026 global study highlighted that while most women know about hot flashes, symptoms like gas and menopause-related bloating are frequently dismissed, leading to a major gap in care. Tracking brings these symptoms into the light, making them impossible to ignore.
When you log everything in one place, you shift from feeling overwhelmed by your symptoms to feeling empowered by information. You get a personalized plan to tackle your specific issues, not just a generic list of "don'ts."
This is particularly powerful for a complex symptom like bloating. Using a dedicated menopause symptom tracker app can help you discover that your trigger isn’t just one food. It might be a combination of stress, a specific ingredient, and a lack of movement on a particular day.
With over 35,000 users already seeing improvements, this method provides a clear path to feeling better, helping you take back control of your body—often in just a few weeks.
When You Should Talk to Your Doctor
▶ PlayWhile most of the gas and bloating you experience during menopause can be handled with lifestyle adjustments, it's absolutely essential to know when your symptoms need a professional eye. Taking charge of your own health is fantastic, but a doctor is the only one who can rule out other underlying conditions and give you some much-needed clarity.
Think of it like an odd noise your car starts making. Most of the time it’s nothing serious, but you know there are certain sounds that mean it’s time to see a mechanic. The same logic applies to your body.
Recognizing Red Flag Symptoms
It's time to book an appointment with your doctor if your gas or bloating comes with any of the following "red flag" symptoms:
Severe or Persistent Pain: A little discomfort is one thing, but sharp, unrelenting, or truly severe abdominal pain is not normal.
Unintentional Weight Loss: If the pounds are coming off without you changing your diet or exercise routine, it’s a signal that needs to be investigated.
Blood in Your Stool: This is a sign that should always be checked out by a healthcare professional right away.
Sudden, Lasting Changes: A brand-new and persistent shift in your bathroom habits, like sudden-onset diarrhea or constipation that just won't go away.
Going to your appointment armed with data can make a world of difference. When you can show your doctor clear patterns from a tracking app like Lila—pinpointing exactly when bloating happens after you eat certain foods, for example—you can have a much more focused and productive conversation.
Your doctor can figure out if your symptoms are truly tied to menopause or if something else might be going on. They can also talk to you about medical options, like Hormone Replacement Therapy (HRT), which sometimes helps digestive issues by getting the hormones that influence your gut back on a more even keel.
Frequently Asked Questions
It's completely normal to have questions when your body starts changing in ways you don't expect. Let's tackle some of the most common ones we hear about the connection between menopause, gas, and bloating.
Will Menopause Give Me Food Intolerances?
It's a common worry, but here's the good news: menopause doesn't usually cause true food allergies. What it can do, however, is make you much more sensitive to foods that never gave you trouble before.
Think of it this way: declining estrogen often slows down your entire digestive tract. When food moves more slowly through your gut, it has more time to sit and ferment, creating extra gas. That's why a food you've eaten your whole life might suddenly leave you feeling bloated. The best way to pinpoint these new triggers is to become a bit of a detective, tracking your meals and how you feel afterward.
Can Hormone Replacement Therapy Help with Gas and Bloating?
For some women, it absolutely can. Since the root cause of a sluggish gut during menopause is often low estrogen, bringing those hormone levels back into balance with Hormone Replacement Therapy (HRT) can help get things moving again. When your digestion speeds up, there's less opportunity for that symptom-causing fermentation to happen.
This is a perfect example of why it’s so important to talk to your clinician about all your symptoms, not just the "big" ones like hot flashes. Your digestive discomfort is a key piece of the puzzle, and it can help them see if HRT might be a good fit for you.
How Long Does Menopausal Bloating Last?
This is the million-dollar question, and the honest answer is: it’s different for everyone. Many women find their digestive issues are at their worst during perimenopause, when hormones are on a rollercoaster.
Once you’re in post-menopause and your hormones settle into their new, lower baseline, these symptoms often calm down. But you don’t have to simply wait and suffer through it. Making thoughtful changes to your diet and lifestyle can bring significant relief from gas and bloating, no matter where you are in your menopause journey.
Ready to stop guessing and get real answers about what’s causing your symptoms? Lila uses AI to analyze your daily habits, helping you connect the dots and create a personalized action plan for relief. Start your journey with Lila today.
Get Lila, your personal coach for perimenopause.
Built for women in their 40s. 24/7 coaching, in your pocket.


