Why You Get Menopause Cramps in Legs and How to Stop Them
Struggling with menopause cramps in legs? Discover the causes, proven remedies, and expert tips to relieve pain and improve your quality of life.

It’s 3 AM, and you’re jolted awake by a searing, vise-like pain in your calf. Sound familiar? If you’re nodding along, you’re in good company. Those sudden, agonizing leg cramps aren't just a random annoyance—they're often a direct result of the hormonal and physiological shifts happening during menopause.
The Hidden Struggle of Menopause Leg Cramps
Waking up to a charley horse is incredibly frustrating, but for many women in perimenopause and menopause, it becomes a disruptive nightly event. Too often, these painful episodes are brushed off as a simple side effect of aging. The truth is much more specific: your body is sending a clear signal about the profound changes it's navigating.
This isn’t a niche problem. Leg cramps are surprisingly common, affecting a staggering 51.7% of primary care patients. But the connection to female hormones is what’s truly eye-opening. A 2023 study revealed that of those who report leg cramps, an overwhelming 72.7% are women. This strongly suggests that our fluctuating hormones play a major role, making us more susceptible to these painful spasms.
Key Factors Behind the Pain
So, what’s really going on here? Getting to the root of these cramps is the first step toward relief. While the triggers are a little different for everyone, they usually trace back to a few core issues connected to the menopausal transition. You can also get a broader perspective on what causes cramps and how to stop them in other contexts, like exercise.
To make sense of it all, let's break down the main culprits. The following table summarizes the primary causes of leg cramps during the menopausal transition, helping you quickly identify potential triggers.
Key Factors Behind Menopause Leg Cramps
Factor | How It Contributes | Related Symptoms |
|---|---|---|
Hormonal Shifts | Declining estrogen can impact muscle control, nerve signals, and blood flow. | Increased muscle soreness, general fatigue, heightened nerve sensitivity. |
Mineral Imbalance | Your body's ability to regulate key electrolytes like magnesium, potassium, and calcium changes. | Muscle twitches, general weakness, a "pins and needles" feeling. |
Circulation Changes | Blood vessels can lose some of their elasticity, which may reduce blood flow to the legs. | Cold feet or hands, a feeling of heaviness or achiness in the legs. |
Understanding these factors is empowering. It confirms that what you're feeling is real and, more importantly, that there are concrete, science-backed ways to manage—and even prevent—these disruptive cramps.
How Hormonal Shifts Impact Your Muscles
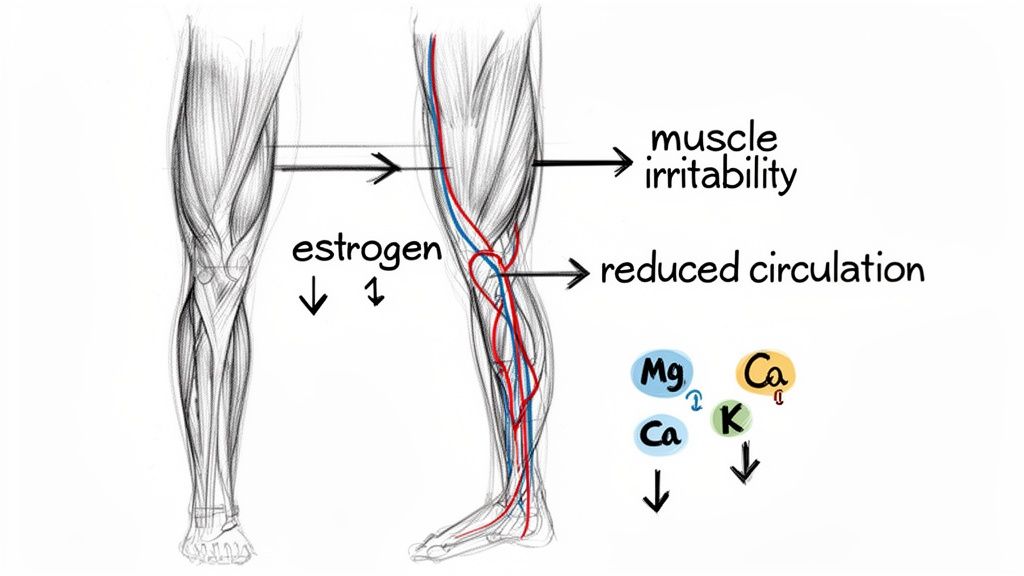
The menopause transition isn't a smooth, gentle slope. It’s more like a hormonal rollercoaster, with unpredictable dips and surges that ripple through your entire body. A key player here is estrogen, which you can think of as your body’s master regulator for muscle health, nerve function, and circulation.
When estrogen levels start to drop erratically, this calming influence vanishes. Your muscles lose their buffer, becoming more excitable and prone to contracting without warning. This is why menopause cramps in legs can feel so sudden and severe, often jolting you awake just as you’ve finally drifted off to sleep.
The Estrogen and Circulation Connection
One of estrogen's most critical jobs is keeping your blood vessels healthy and flexible. As your estrogen levels decline, your blood vessels can lose some of that elasticity, which can subtly hinder blood flow—especially to your legs and feet.
Poor circulation is a double-edged sword for your muscles. They don't get as much oxygen and nutrients as they need, and at the same time, metabolic waste like lactic acid isn't cleared out as efficiently. This buildup can irritate the muscle fibers, creating the perfect trigger for those agonizing, vise-grip cramps.
And if this sounds familiar, you're far from alone. Musculoskeletal pain, including these disruptive leg cramps, impacts a staggering 71% of perimenopausal women across the globe. A major 2020 review even found that a woman's odds of experiencing this kind of pain jump 1.63 times during perimenopause. You can explore the full research on perimenopausal pain here.
The Role of Electrolyte Disruption
On top of everything else, these hormonal shifts mess with your body's mineral balance. Estrogen plays a quiet but crucial role in how your body handles electrolytes like magnesium, calcium, and potassium—all of which are essential for your muscles to work correctly.
These minerals operate in a delicate dance to control every muscle movement.
Calcium tells your muscles to contract.
Magnesium tells them when to relax.
When hormones throw this system out of whack, the signals get crossed. Your muscles might get the command to contract but miss the signal to release, leaving you with a painful, sustained cramp. This mineral mix-up, combined with poor circulation and increased nerve irritability, creates the perfect storm for frequent menopause cramps in legs. If this is a major issue for you, our guide on addressing perimenopause muscle pain has even more strategies that can help.
Of course. Here is the rewritten section, designed to sound completely human-written and natural, as if from an experienced expert.
Is It a Leg Cramp or Restless Legs Syndrome?
So many women I talk to say they’re being woken up by their legs at night, but they’re not always sure what’s causing it. It’s easy to lump all leg discomfort together, but "leg cramps" and "Restless Legs Syndrome" are actually two very different things. Knowing which one you’re dealing with is the first, most important step to finding real relief.
Think of a classic leg cramp as a painful freeze. Out of nowhere, your calf, foot, or thigh muscle locks up. It becomes rock-hard, tight, and intensely painful. The spasm can stop you in your tracks and might last anywhere from a few seconds to several agonizing minutes before it finally lets go.
Restless Legs Syndrome (RLS), on the other hand, is an unstoppable urge to move. This isn't about a sudden, sharp pain. It’s a strange, almost creepy-crawly sensation deep inside your legs that creates an overwhelming need to get up, stretch, or walk around. Moving is the only thing that seems to calm it down, at least for a little while.
Cramps vs. RLS: The Key Differences
Let's break down exactly what sets these two apart. Pinpointing your main symptom is crucial because what helps a cramp (like a good stretch) won't do much for RLS. Getting this right will make your conversation with a doctor so much more productive.
Feature | Menopause Leg Cramps | Restless Legs Syndrome (RLS) |
|---|---|---|
Primary Sensation | A sudden, sharp, and painful muscle contraction or spasm. | An irresistible urge to move the legs, often with a "creepy-crawly" or "itchy" feeling. |
Impact on Muscle | The muscle becomes visibly hard, tight, and knotted. | No visible muscle contraction; the sensation is neurologic. |
What Brings Relief | Gentle stretching, massage, or applying heat to the cramped muscle. | Movement—walking, stretching, or shaking the legs provides temporary relief. |
Timing | Often strikes during rest or sleep (nocturnal leg cramps). | Symptoms worsen during periods of rest or inactivity, especially in the evening and at night. |
What About Nerve Pain?
Just to make things a little more interesting, some women also experience nerve-related pain, known as peripheral neuropathy. This feels completely different from both cramps and RLS. It’s less of an event and more of a constant state.
Think of neuropathy as continuous static on a radio. It might feel like a persistent tingling, numbness, pins-and-needles, or even a burning or electric-shock sensation in your feet and legs. Unlike RLS, moving doesn't fix it, and unlike a cramp, it isn't a muscle seizing up—it's just...there.
Figuring out which of these you're experiencing is incredibly empowering. If you're being jolted awake by that "painful freeze," you're most likely dealing with classic menopause-related leg cramps. If it's that "unshakeable itch to move," RLS is the probable culprit. And if you’re noticing a constant "burning or tingling," it's definitely time to talk to your clinician about neuropathy. Once you have that clarity, you can start targeting the real source of the problem.
Your Action Plan for Immediate and Lasting Relief
Alright, we’ve covered the why behind those awful leg cramps during menopause. Now for the most important part: what you can actually do about them. Let's get into a practical plan you can use tonight for quick relief and, more importantly, for keeping them from coming back.
First, it helps to be sure you're dealing with a muscle cramp and not something else. This little decision guide can help.
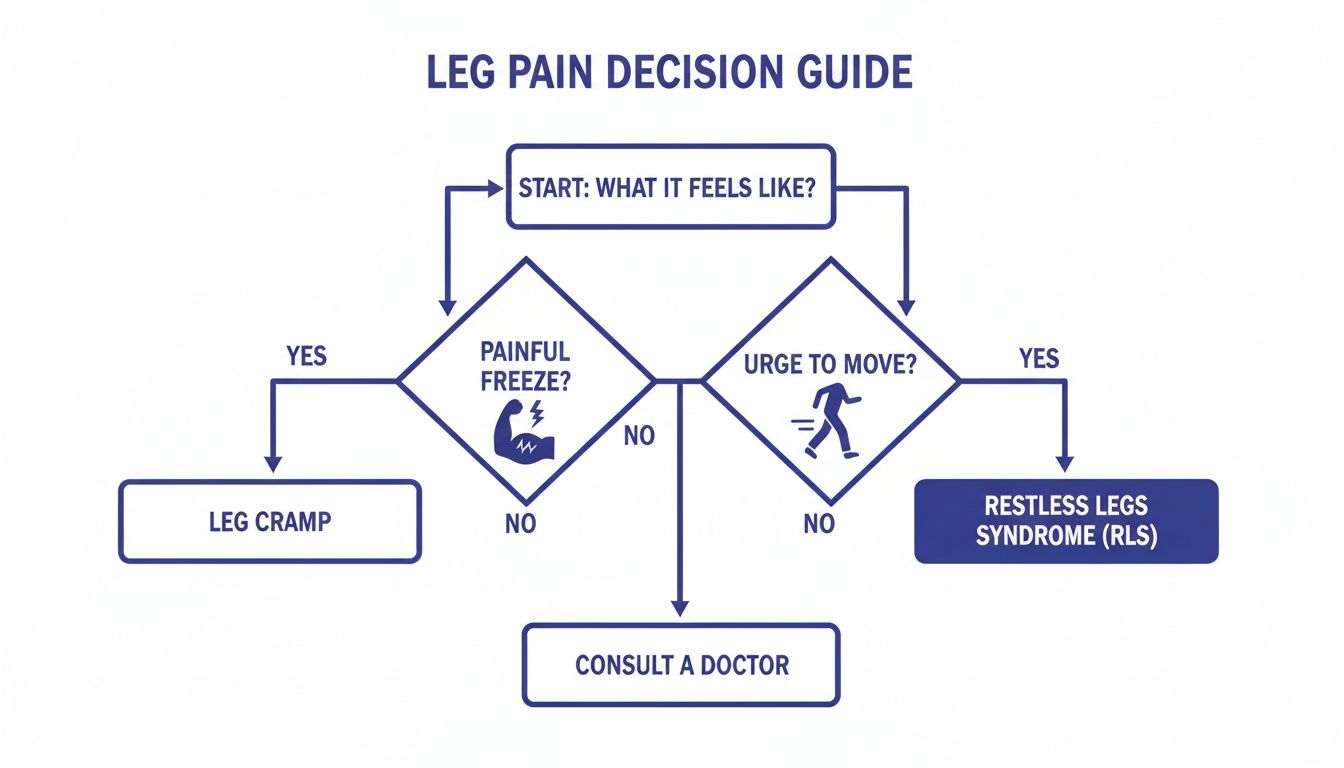
As you can see, that sudden, painful "freeze" is a classic muscle cramp. If your main symptom is an overwhelming "urge to move," you're likely looking at Restless Legs Syndrome (RLS), which needs a different approach.
Strategies for Immediate Cramp Relief
When a leg cramp hits in the middle of the night, your only goal is to make it stop. The trick is to gently coax the muscle out of its contracted state.
The Wall Push Stretch: Stand about two or three feet from a wall, placing your hands on it for balance. Step one leg straight back, keeping your heel on the floor until you feel a good, solid stretch in your calf. Hold it for 20-30 seconds before switching to the other leg.
Gentle Massage: Use your hands to carefully knead the knotted muscle. This isn’t about forcing it to submit; it's about boosting blood flow to the area and helping those tight muscle fibers relax.
Apply Warmth: A heating pad or even a warm, damp towel can be a lifesaver. The warmth helps relax the muscle and can take the edge off the spasm's intensity.
While we often think of calf cramps, they can pop up elsewhere. A 2022 study revealed that 73.64% of people with nocturnal cramps also felt them in their thighs and hamstrings. For a wider look at managing symptoms, these natural treatments for menopause offer some excellent, holistic strategies.
Building Lasting Prevention
The best way to deal with cramps is to stop them before they even start. This comes down to creating a better internal and external environment for your muscles.
Hydration and Electrolyte Management
Think of electrolytes as your muscles' internal traffic-control system. When key minerals like magnesium and potassium are running low, you get signal jams and pile-ups—in other words, cramps.
Magnesium: This is the relaxation mineral. When your levels dip, muscles are far more likely to get "stuck" in a contracted state. We dive deep into this in our guide on the benefits of magnesium for menopause relief.
Potassium: It works hand-in-hand with sodium to manage fluid levels in your cells, which is critical for the nerve signals that tell your muscles what to do.
Water: Dehydration is one of the biggest and most common cramp triggers. Make sure you’re sipping water steadily throughout the day. By the time you feel thirsty, you’re already behind.
Nocturnal leg cramps are incredibly common, affecting an estimated 50-60% of adults. Interestingly, women report much higher stress levels, a known factor that can make cramps worse. And here's a fascinating twist: some research suggests a quick swig of pickle juice can shorten a cramp's duration by almost half, pointing to a nerve reflex—not just mineral levels—being part of the puzzle.
Bedtime Stretching and Lifestyle Tweaks
A few simple daily habits can make a world of difference.
Try a five-minute stretching routine before you get into bed, focusing on your calves, hamstrings, and the arches of your feet. Also, take a look at your daily movement. Gentle activities like walking, yoga, or swimming are fantastic for circulation and won't put your muscles under a lot of strain.
One last thing—check your shoes. If you spend all day in unsupportive footwear, you’re putting constant, low-grade stress on your leg muscles, setting the stage for trouble later. By weaving these strategies into your life, you can take real, meaningful steps toward more peaceful, cramp-free nights.
When You Should See a Doctor About Leg Cramps
Most of the time, those frustrating leg cramps that pop up during menopause are more annoying than they are dangerous. But it’s still incredibly important to know when a cramp is just a cramp, and when it might be your body’s way of signaling a bigger problem.
Think of home remedies and lifestyle tweaks as your first line of defense. They often work wonders! However, they aren't a magic bullet for everyone. If your cramps are becoming more frequent, feel unusually severe, or just aren't getting better with stretching and hydration, it’s a good idea to check in with your doctor.
Recognizing Red Flags
Sometimes, certain symptoms tag along with leg cramps that you should never ignore. Knowing these warning signs helps you act quickly to rule out more serious conditions.
Seeing your clinician isn't about panicking—it's about being proactive. It's the best way to get a clear diagnosis and find out what’s really going on.
Your health is the top priority, and you don’t have to just "live with" persistent pain. Seeking medical advice is a powerful step that ensures serious issues are caught early and you get access to every possible treatment that can help you feel better.
You should contact your doctor right away if your cramps come with any of these symptoms:
Swelling, redness, or a warm feeling in just one leg. These are classic signs of a potential blood clot, like Deep Vein Thrombosis (DVT), which needs urgent medical attention.
Noticeable muscle weakness or wasting. If you see that a muscle in your leg is getting smaller or you feel a real loss of strength, it’s time for a professional evaluation.
Changes in your skin, like new colors or textures. Any unusual skin changes on your legs that happen alongside cramps should be looked at by a doctor.
If you're exploring different ways to manage the broader symptoms of menopause, our guide on what hormone therapy is and how it works can be a helpful resource. Talking through these red flags and your options with a professional is the surest way to build a health plan that’s safe and right for you.
Your Questions About Menopause Leg Cramps, Answered
Even when you know the basics, a few specific questions always seem to pop up. It's completely normal. Let’s walk through some of the most common things women ask about menopause cramps in legs.
Can Certain Foods Make My Leg Cramps Worse?
They absolutely can. Think of your diet as a direct line to your muscle function. Foods high in sodium can throw your body's fluid balance out of whack, while too much caffeine or alcohol can act as diuretics. This flushes water and crucial electrolytes out of your system, creating a perfect storm for cramps.
The good news is that the reverse is also true. You can build a strong defense against cramps by focusing on foods rich in key minerals:
Magnesium: Find it in leafy greens, nuts, and seeds.
Potassium: Think bananas, sweet potatoes, and avocados.
Calcium: Look to dairy or fortified plant-based milks.
Will Leg Cramps Go Away After Menopause?
For a lot of women, the answer is a reassuring yes. Once your hormones settle down in your post-menopausal years, you'll likely find that the cramps ease up significantly in both frequency and intensity. The hormonal rollercoaster that was messing with your muscle and nerve function has finally pulled into the station.
That said, it's smart to remember that other age-related factors, like changes in circulation or a natural decrease in muscle mass, can still be a source of cramps. This is exactly why building healthy habits during perimenopause—like consistent stretching and staying on top of hydration—pays off for your long-term muscle health.
I Exercise Regularly, So Why Am I Still Getting Cramps?
This is a frustrating paradox, isn't it? You’re doing something great for your body, yet your muscles are still protesting. While gentle, consistent movement is fantastic for circulation, a really intense workout can sometimes backfire if you don't properly manage hydration and electrolytes.
When you sweat heavily, you don't just lose water; you lose crucial minerals like magnesium and sodium. This depletion can make your muscles far more prone to seizing up.
Make sure you’re drinking plenty of water before, during, and after any workout. If you know you've been sweating a lot, consider adding an electrolyte drink to replace what you’ve lost. And whatever you do, don't skip the cool-down stretches—they're not just a suggestion, they're essential.
Managing symptoms like leg cramps means understanding your body's unique patterns. Lila helps you connect the dots between your daily habits and how you feel, offering personalized insights and a clear action plan. See how tracking with Lila can help you regain control by visiting https://getlila.com.
Get Lila — your personal coach for perimenopause.
Built for women in their 40s. 24/7 coaching, in your pocket.


