
Your Guide to Perimenopause Muscle Pain Causes and Relief
Mar 12, 2026
If you’ve started waking up with a stiff back, feeling a new ache in your shoulders, or just find yourself sore for no good reason, you’re not imagining it. Perimenopause muscle pain is a genuine and common symptom, and it can be incredibly confusing when it seems to pop up out of the blue.
It's a frustrating experience, especially when you feel like you haven't done anything to deserve the sudden discomfort. But you're definitely not alone in this.
The Sudden Ache: Understanding Perimenopause Muscle Pain
That unfamiliar ache in your hips, the morning stiffness that takes a while to shake off, or the soreness you feel after a simple walk isn't just a random sign of aging. More often than not, it's a direct result of the hormonal rollercoaster that defines the perimenopausal years.
In fact, this is an incredibly widespread experience. Some studies show that over 70% of women report experiencing new or worsening symptoms in their bones, joints, and muscles during this transition. These new sensations can be disruptive and even a little scary, leaving you to wonder what’s going on with your body.
Why Your Muscles Suddenly Hurt
At the heart of perimenopause muscle pain is one key player: estrogen. The dramatic fluctuations and eventual decline of this hormone are the primary drivers behind why you feel so sore. Estrogen does a lot more than just manage your menstrual cycle; it's deeply involved in your entire musculoskeletal system.
Here’s a breakdown of what’s happening:
It keeps inflammation in check. Estrogen is one of your body’s natural anti-inflammatory agents. As your levels become erratic and drop, low-grade, body-wide inflammation can increase, leading directly to aches and stiffness.
It helps maintain muscle. This hormone is crucial for building and repairing muscle tissue. Without a steady supply, muscles can lose some of their strength and become more susceptible to soreness and injury.
It influences collagen production. Collagen is the essential protein that provides structure to your tendons, ligaments, and skin. Lower estrogen means less collagen, which can make these connective tissues less flexible and more prone to pain.
Think of estrogen as your body's on-call maintenance crew for your muscles and joints. During your reproductive years, the crew is fully staffed, constantly handling repairs and keeping inflammation at bay. In perimenopause, the crew starts showing up erratically and with fewer workers, leaving your muscles more vulnerable to daily wear and tear.
To get a complete picture of how your body changes during this time, our guide on Women's Health Through Every Life Stage offers a broader look at what to expect.
Understanding these connections is the first step toward feeling better. A simple tool like the Lila app can be a huge help here, allowing you to track your symptoms and see how they line up with your cycle, diet, or activity levels. When you start to see your own patterns emerge, you can build a targeted plan for relief.
How Hormone Fluctuations Trigger Muscle and Joint Pain
If you've ever felt like your body’s hormones are a finely tuned orchestra, then perimenopause is when the conductor abruptly leaves the stage. The music gets chaotic, and for many of us, this shows up as widespread muscle pain and joint stiffness. Figuring out the science behind this new discomfort is the first step toward feeling more in control.
So, what's really going on here? It all comes down to the star of the show: estrogen. The unpredictable swings and eventual drop in this key hormone are the main drivers behind the aches and pains of perimenopause. Estrogen does so much more than manage your cycle; it's also the unsung hero of your entire musculoskeletal system.
This concept map shows a clear line from those hormonal shifts to the physical pain you might be feeling, and how you can start to manage it.
As you can see, the hormonal transition is the root cause of the physical symptoms. The good news is that this means we can use targeted strategies to address them.
The Estrogen Effect on Muscles and Joints
Think of estrogen as your body's natural anti-inflammatory and tissue repair manager. When levels are stable, it works quietly in the background, keeping everything running smoothly. But during perimenopause, its influence wanes, leaving your muscles and joints more vulnerable.
Let's break down exactly what happens when estrogen levels start to drop:
Inflammation Rises: Estrogen has potent anti-inflammatory properties. As levels fall, your body's baseline level of inflammation can creep up. This can lead to that generalized achiness, soreness, and morning stiffness that just seems to take forever to shake off.
Collagen Production Slows: This hormone is crucial for producing collagen, the protein that acts like the "scaffolding" for your muscles, tendons, and ligaments. With less estrogen, you produce less collagen, making these tissues stiffer, less flexible, and more susceptible to strain or pain.
Muscle Repair is Impaired: Estrogen also plays a direct role in helping your muscles recover and rebuild after use. When it's in short supply, your muscles don't bounce back as quickly. This explains why a workout you used to handle easily might now leave you sore for days.
"When someone enters the menopause transition, estradiol is no longer the primary estrogen. Estrone, a weaker form of estrogen, replaces estradiol, and this weaker version cannot preserve the musculoskeletal system as effectively, leading to loss of muscle mass, decreased bone density and cartilage."
This isn't just a minor annoyance; it's a significant biological event. A massive study of over 93,000 women found that while about 40% report muscle or joint pain before the transition, that figure jumps to 57% during perimenopause. That's a 1.35-fold increased risk, making this a critical window for new or worsening aches. For a deeper look at the data, you can explore the full study about perimenopause and musculoskeletal health.
Cortisol: The Stress and Pain Amplifier
Of course, hormones don't operate in a vacuum. The stress from classic perimenopause symptoms—think hot flashes, mood swings, and especially poor sleep—can trigger a surge in cortisol, your body's main stress hormone.
High cortisol then kicks off a vicious cycle that makes muscle pain even worse. It keeps your body stuck in a low-grade "fight or flight" mode, which means your muscles are constantly tense. This chronic tension is a direct cause of a lot of the neck pain, shoulder knots, and lower back stiffness that women report.
On top of that, elevated cortisol can actually make your brain more sensitive to pain signals. An ache that you might have barely noticed before can suddenly feel intense and all-consuming. Understanding this connection helps explain why the pain can feel so random and overwhelming, and turns it into a problem with a solution.
Hidden Factors That Amplify Perimenopause Pain
If you're dealing with new aches and pains during perimenopause, it's easy to blame your hormones—and you're not wrong. But they're rarely the whole story. Several other factors can sneak in and crank up the volume on your discomfort, turning a manageable ache into something that feels truly overwhelming.
Think of it this way: if dropping estrogen levels create the initial spark for pain, these other issues are the dry kindling that helps that fire spread.
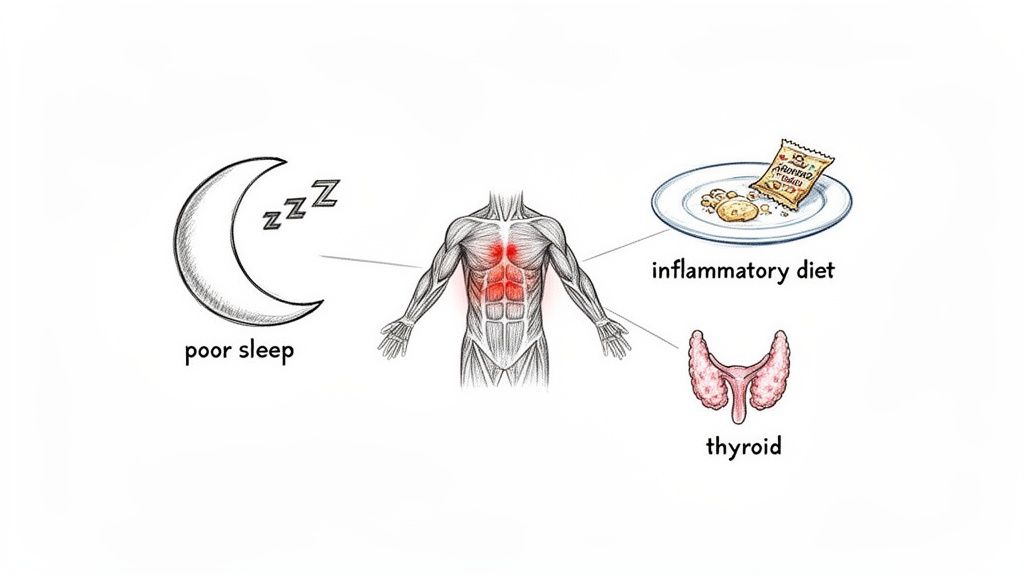
This is why getting relief isn't just about one thing. It’s about understanding how all these pieces fit together for you. By noticing your personal pain patterns, you can shift from just reacting to aches to proactively getting ahead of them. This is where tracking your lifestyle can be a game-changer—it helps you connect the dots between how you feel and what’s actually going on in your daily life.
The Sleep-Pain Connection
It’s a cruel irony of perimenopause: just when your body needs rest the most, sleep often goes completely off the rails. Between night sweats, anxiety, and the general hormonal rollercoaster, getting a solid night's sleep can feel impossible. But this does more than just make you groggy; it directly sabotages your body's ability to heal.
Deep sleep is when your body gets down to business with repairs. It releases growth hormone, which is critical for mending the microscopic tears our muscles get from just moving through the day. When sleep is constantly interrupted, that vital repair cycle never gets a chance to finish.
Imagine your body has a road crew that only works the night shift. If they’re constantly interrupted by traffic (like hot flashes or a racing mind), they can't properly fill in the day's potholes. You wake up feeling like you’ve been driving on a bumpy road all night—stiff, sore, and anything but refreshed.
This lack of overnight maintenance is a huge reason why so many women wake up with intense morning stiffness. Your muscles simply didn't get the repair they needed, making those first few movements of the day feel incredibly painful.
How Your Diet Can Fuel Inflammation
What you eat can either help calm inflammation or pour gasoline on the fire. We know that certain foods, especially those packed with sugar and highly processed ingredients, can promote low-grade inflammation all over the body.
When your system is already more prone to inflammation because of lower estrogen, a diet heavy in these culprits can make perimenopause muscle pain so much worse.
Common Inflammatory Triggers to Watch For:
Sugary Foods and Drinks: Think sodas, candy, and pastries. They can spike your blood sugar, which is a known trigger for an inflammatory response.
Refined Carbohydrates: Things like white bread, pasta, and crackers break down into sugar almost immediately, having a very similar effect.
Processed Meats and Fried Foods: These often contain compounds called advanced glycation end products (AGEs), which are powerfully inflammatory.
Start paying attention to how you feel an hour or two after you eat. You might be surprised to find that your aches and pains flare up after certain meals. This is an often-overlooked but powerful way to start taking back control.
The Thyroid's Under-the-Radar Role
Another key piece of the puzzle is your thyroid. This small gland in your neck is the master control center for your metabolism, producing hormones that dictate everything from your energy levels to your body temperature. Unfortunately, the hormonal chaos of perimenopause can throw your thyroid out of whack, sometimes leading to an underactive thyroid (hypothyroidism).
An underactive thyroid can cause its own set of muscle-related symptoms, including:
Persistent muscle aches, stiffness, and tenderness
A feeling of weakness in the muscles
Cramps and deep fatigue
Because these symptoms look so much like standard perimenopause muscle pain, thyroid problems are frequently missed. It's a critical angle to investigate, especially if your muscle pain comes with other clues like profound exhaustion, unexplained weight gain, or constantly feeling cold. While many aches are linked to sex hormones, it's also wise to explore the relationship between menopause and joint pain to see the full picture.
The reality is that this kind of pain is incredibly common. While some studies suggest around 71% of women experience it, other tools reveal even higher numbers. For example, a meta-analysis using the Menopause-Specific Quality of Life Questionnaire (MENQOL) found that a staggering 80% of women reported musculoskeletal pain. The data also showed that perimenopausal women have a 1.63 times higher chance of having these symptoms compared to premenopausal women. You can read the detailed analysis of perimenopause pain prevalence to see the full breakdown.
Your Action Plan for Easing Perimenopause Muscle Pain
Alright, understanding the why behind your muscle pain is a huge first step. But now it’s time to put that knowledge into action. Building your personal action plan isn’t about a massive, overwhelming overhaul. It’s about making small, consistent changes that add up to real relief.
This is your framework for fighting inflammation, supporting your muscles, and finally getting back to feeling like yourself.
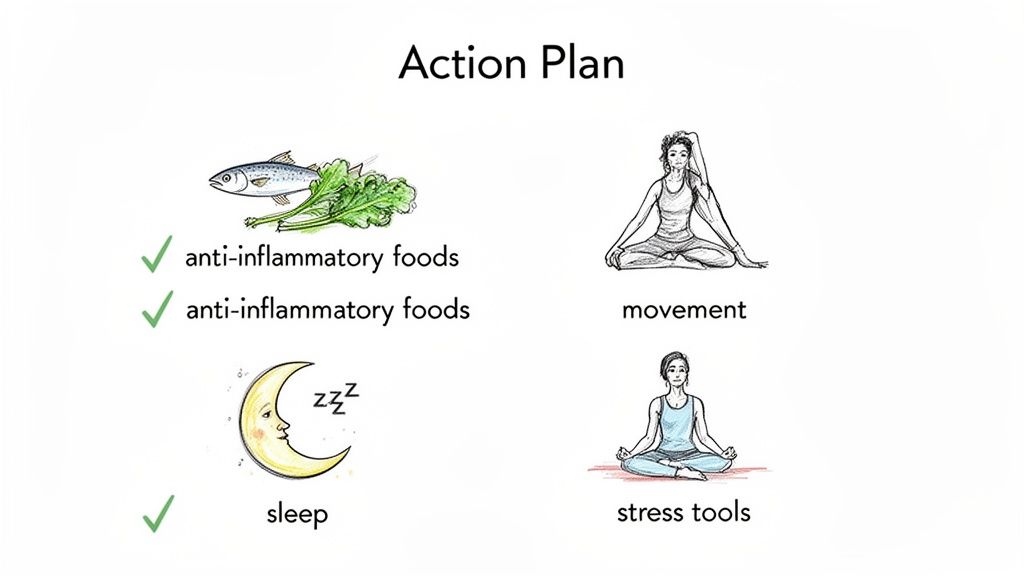
Think of the following not as a rigid set of rules, but as a menu of options. The goal is to experiment and find the right combination that feels good for your body. Just remember, consistency will always beat intensity.
Start With What's on Your Plate
Your diet can either fuel the fire of inflammation or help put it out. Adopting an anti-inflammatory eating style is one of the most powerful things you can do to manage the aches and pains of perimenopause. This isn't about deprivation; it's about loading up on delicious, nutrient-rich whole foods.
Foods to Add In:
Oily Fish: Think salmon, mackerel, and sardines. They’re packed with omega-3 fatty acids, which are potent anti-inflammatory agents that can help soothe stiff, sore joints.
Leafy Greens: Spinach, kale, and chard are bursting with antioxidants that combat cellular stress and calm inflammation.
Berries: Blueberries, strawberries, and raspberries are full of compounds called anthocyanins, which have a proven anti-inflammatory effect.
Nuts and Seeds: Walnuts and flaxseeds are fantastic plant-based sources of those crucial omega-3s.
Foods to Reduce:
Sugar and Refined Carbs: Things like white bread, pastries, and sodas can trigger blood sugar spikes that kickstart an inflammatory response.
Processed Foods: These often hide unhealthy fats and additives that contribute to systemic inflammation throughout your body.
By simply shifting your plate toward more of these whole foods, you’re giving your body the tools it needs to calm down from the inside out. For a broader look at managing discomfort, you can explore other effective muscle pain relief strategies that cover both immediate and long-term approaches.
Reintroduce Gentle, Strategic Movement
When every muscle aches, the thought of exercise can be cringe-worthy. I get it. But the right kind of movement is absolutely critical for preventing stiffness and holding onto the precious muscle mass that supports your joints. The trick is to be gentle and smart about it.
A well-rounded routine is your best friend here. Forget high-impact activities that can jolt your joints and focus instead on movements that build both strength and flexibility.
Your Weekly Movement Blueprint:
Light Strength Training (2-3 times per week): This is non-negotiable for women in this phase of life. Keeping your muscle mass not only boosts your metabolism but also provides vital support for your entire skeletal structure. You can start with simple bodyweight exercises, resistance bands, or light dumbbells.
Low-Impact Cardio (3-5 times per week): Activities like swimming, cycling, or even a brisk walk get your blood flowing, delivering oxygen and nutrients to tired muscles without adding stress to your joints.
Daily Flexibility and Mobility: Make time for yoga, Pilates, or just a few simple stretches every day. This helps ease stiffness, improves your range of motion, and has the added benefit of calming your nervous system. A particularly nasty issue that can pop up is frozen shoulder; you can learn how to manage the unique symptoms of frozen shoulder during menopause in our detailed guide.
Think of strength training as building a supportive scaffold around your joints. The stronger your muscles are, the less strain your joints have to bear, which can dramatically reduce aches and pains.
Prioritize Sleep and Manage Stress
Bad sleep and high stress are a brutal combination that creates a vicious cycle, making pain feel so much worse. It’s during deep sleep that your body gets to work on critical muscle repair. When that sleep is constantly interrupted by night sweats or anxiety, the repair cycle gets cut short, leaving you feeling stiff and sore when you wake up.
Likewise, chronic stress keeps your body flooded with cortisol, which tightens muscles and makes your brain more sensitive to pain signals. So, tackling your sleep and stress head-on is a direct strategy for pain relief.
Simple Steps for Better Rest:
Stick to a Sleep Schedule: Try to go to bed and wake up around the same time every day, even on weekends. This helps regulate your body’s internal clock, or circadian rhythm.
Wind Down for an Hour: An hour before bed, power down your screens. Instead, do something calming like reading a book, taking a warm bath with Epsom salts, or listening to quiet music.
Practice a Little Mindfulness: Just 5-10 minutes of mindfulness or meditation a day can help lower cortisol, release muscle tension, and make the pain you feel seem less overwhelming.
By weaving these strategies into your daily life, you create a powerful, multi-pronged approach to managing perimenopause muscle pain. Using a tool like the Lila app can help you track your efforts and see exactly how these changes connect to your symptoms, empowering you to fine-tune your plan for the best possible relief.
Knowing When to Talk to Your Doctor About Muscle Pain
While a certain amount of general achiness is almost a rite of passage during perimenopause, it's so important to learn how to tell the difference between "normal" and a sign that something else is going on. Your body has its own way of sending signals, and we need to listen.
Think of it like the check engine light in your car. Sometimes it’s just a minor alert, but other times it’s a flashing red light telling you to pull over immediately. Learning to spot those "red light" symptoms is the key to getting the right help and ruling out more serious issues.
Red Flags That Need a Medical Opinion
It can be tempting to write off every new ache as "just perimenopause," but you should never ignore pain that feels severe, new, or just plain different. Be on high alert if your muscle pain shows up with any of the following signs.
These symptoms might point to something beyond hormonal shifts, like inflammatory arthritis, a thyroid problem, or another condition that needs a proper diagnosis and its own specific treatment plan.
Don't ignore these warning signs:
Severe or Highly Localized Pain: If the pain is intense and you can point to one specific spot—like a single knee, hip, or wrist—and it just won't quit, it's time to get it checked out.
Pain with Swelling, Redness, or Heat: These are the classic signs of inflammation. This could be a signal of an infection or an autoimmune condition, such as rheumatoid arthritis.
Noticeable Muscle Weakness: This isn't just feeling a bit tired. This is a sudden inability to do things you normally do, like struggling to get up from a chair, climb stairs, or lift a bag of groceries you used to handle easily.
Pain That Wrecks Your Sleep: We all know night sweats can disrupt sleep, but that's different. If the pain itself is so bad that it consistently wakes you from a sound sleep, that's a major red flag.
Getting a clear diagnosis from a doctor is crucial. It’s the only way to know for sure if you’re dealing with hormonally-driven muscle pain, something like osteoarthritis, or another condition altogether. This ensures you get the most effective treatment for what’s really going on.
Preparing for Your Doctor's Appointment
Once you decide to make an appointment, a little prep work can make a world of difference. Walking in and saying "I just ache all over" makes it incredibly difficult for your doctor to figure out the next steps. The more specific you can be, the better.
Try keeping a simple log in a notebook for a week or two beforehand. Jotting down a few details each day creates a clear record that can help your provider spot patterns they might otherwise miss.
Your Pre-Appointment Checklist:
Pinpoint the Pain: Where, exactly, does it hurt? Is it on one side or both? Is it deep in the muscle, or does it feel closer to the joint? For instance, describing specific menopause hip pain gives your doctor a much clearer picture.
Describe the Sensation: Find the right words. Is the pain sharp, dull, burning, stabbing, or a deep ache?
Note the Timing: When does the pain flare up? Is it worst first thing in the morning? Does it get worse after you've been active, or is it a constant bother all day long?
List What Helps or Hurts: What have you tried? Does resting it help? Does a hot bath provide some relief? Does a long walk make it much worse?
Mention Other Symptoms: Make sure to bring up anything else that’s been going on, even if it seems totally unrelated. This includes things like fatigue, mood swings, sleep issues, or even changes in your digestion.
When you come to your appointment with this kind of clear information, you and your doctor can work together as a team to get to the bottom of your pain and find the best path forward.
Turning Your Daily Data Into Real Relief with Lila
Trying to figure out what's behind your muscle pain can feel like being a detective with no clues. You know something is off, but connecting the dots between your lifestyle and your symptoms is a frustrating guessing game. This is where a little bit of tracking can make all the difference, moving you from feeling overwhelmed to feeling back in control.
The Lila app is designed to be your partner in this process, turning your own health information into a clear path forward. As you log details about your symptoms, sleep, what you eat, and your stress levels, you’re building a picture that is completely unique to you. This isn’t just about collecting data for data’s sake; it’s about revealing the hidden patterns that dictate how you feel from one day to the next.
Finding Your Personal Pain Triggers
After a little while, you might start to see things click into place. Maybe your muscle aches always flare up after a rough night’s sleep, or during a week when work stress is through the roof. For others, the connection might be dietary—perhaps you’ll notice that eating certain foods, like dairy or a lot of sugar, leads to more stiffness the next morning.
Lila does the heavy lifting for you by analyzing all the information you share. It looks for these connections in your daily check-ins and offers up personalized insights based on how your body is actually responding.
Think of it like having a personal health analyst who can spot the subtle cause-and-effect links you might have missed on your own. Instead of getting generic advice, you get specific guidance built from your own lived experience.
This changes everything. Managing your symptoms is no longer a shot in the dark. With the right information, you can finally see what’s making your perimenopause muscle pain better or worse.
A Real-World Example From a Lila Member
Take Jane, a 46-year-old who was dealing with a persistent, nagging pain in her hip. It was waking her up at night and making her daily walks miserable. She was frustrated and had pretty much resigned herself to living with it. When she started using Lila, she began logging her symptoms, how long she slept, and her daily stress levels.
Within just a few weeks, a clear pattern emerged:
Her hip pain was always worse on mornings after she’d gotten fewer than six hours of sleep.
The pain also spiked on days right after a high-stress deadline at work.
With this new understanding, Jane used the app’s 24/7 coaching feature to ask for practical advice. Her Lila coach suggested she start a simple "wind-down" routine an hour before bed—no phone, just reading and some gentle stretches. She also began using a 5-minute guided breathing exercise from the app during her afternoon work breaks to manage stress.
The difference was incredible. By making sleep a priority and actively managing her stress, Jane’s hip pain eased dramatically. She was finally sleeping through the night and enjoying her walks again. Her story is a perfect example of how tracking with a tool like Lila can lead directly to real, lasting relief.
Frequently Asked Questions About Perimenopause Muscle Pain
It's completely normal to have a long list of questions when you're navigating the twists and turns of perimenopause. When muscle pain enters the picture, getting straightforward answers is the first step toward feeling like yourself again.
Can Hormone Replacement Therapy Help With Muscle Pain?
I get this question a lot, and the short answer is: for many women, yes. Think of it this way: HRT can help address the root of the problem by restoring your estrogen levels. This, in turn, helps dial down body-wide inflammation and slow the breakdown of collagen, which are two of the biggest culprits behind achy muscles and stiff joints during this transition.
That said, HRT isn't a magic bullet for everyone. It's so important to have an open, thorough conversation with your doctor. They'll walk you through your personal health history to figure out if it's a safe and effective option for you.
What Are the Best Exercises for Perimenopause Muscle Aches?
The goal here is to move in a way that supports your body, not pushes it past its limits. A gentle, well-rounded routine is your best friend.
Low-Impact Cardio: Think swimming, cycling, or going for a brisk walk. These activities are fantastic for getting your blood flowing and delivering oxygen to sore muscles without putting extra stress on your joints.
Strength Training: Don't be afraid of weights! Using dumbbells, resistance bands, or even just your own body weight 2-3 times per week is crucial. Building and maintaining muscle gives your skeleton a strong, natural support system.
Flexibility and Mobility: Making time for daily stretching, yoga, or Pilates can make a huge difference. It's a powerful way to ease that dreaded morning stiffness, improve your range of motion, and even help calm your nervous system.
The most important rule? Listen to your body. Feeling some muscle fatigue after a workout is normal, but sharp or sudden pain is a stop sign. Learning to adapt your movement isn't giving up—it's getting smarter.
Is This Pain Perimenopause or Something Else Like Fibromyalgia?
This is a tricky one because the symptoms can definitely overlap, which is why a proper medical diagnosis is non-negotiable. Typically, perimenopause muscle pain feels like a widespread achiness or stiffness, often worse in the morning or after a busy day.
Fibromyalgia usually involves more than just pain. It's characterized by chronic, widespread pain along with specific tender points on the body. It also commonly comes with debilitating fatigue and cognitive issues that many call "fibro fog."
This is where tracking your symptoms is invaluable. Keeping a simple log of your pain levels, what makes it better or worse, and other lifestyle factors gives your doctor the detailed clues they need to distinguish between conditions and get you the right diagnosis.
Ready to turn your health data into real relief? Lila provides a personalized action plan based on your unique symptoms. Find out how you can start feeling better with Lila today.
You should not have to do it all on your own










