Perimenopause Spotting Between Periods: Causes, When to Worry
Experiencing perimenopause spotting between periods? Understand causes, when to worry, and manage symptoms with our complete guide for 2026.

Spotting between periods is an incredibly common, though often unsettling, part of the perimenopause journey. While it can be alarming to see unexpected bleeding, it’s most often a normal sign that your body is transitioning—not a sign of trouble.
Why Am I Spotting Between Periods During Perimenopause
If you’ve started noticing light bleeding outside of your regular cycle, you are far from alone. The experience can be confusing and worrying, but getting a handle on the "why" can bring some much-needed peace of mind. Let’s break down what’s really going on inside your body.
The Hormonal Rollercoaster
For years, your key reproductive hormones, estrogen and progesterone, have worked together like a skilled orchestra, conducting your monthly cycle with a predictable rhythm. Perimenopause is when the orchestra starts playing out of tune.
Estrogen: This is the hormone that builds up your uterine lining (the endometrium). During perimenopause, its levels can suddenly spike and then crash without warning.
Progesterone: This hormone’s job is to stabilize that lining after ovulation. But as ovulation becomes more erratic, progesterone levels also become unreliable.
This hormonal chaos creates an unstable uterine lining. Instead of shedding all at once during a period, it can shed small amounts at random times. The result is what we call perimenopause spotting between periods. It’s not a true period, but more like minor, unscheduled housekeeping.
"The primary cause for spotting in perimenopause is the changing hormonal environment. As estrogen and progesterone levels fluctuate unpredictably, the uterine lining doesn't build up and shed as neatly as it once did, leading to irregular bleeding."
Just How Common Is This, Really?
Seeing blood between cycles can feel isolating, but spotting is the norm, not the exception. Research shows that a staggering 66.8% of women have at least three instances of six or more days of spotting during the perimenopause transition.
That number jumps even higher, to 75.2%, in the late transition phase. This really highlights how widespread this symptom truly is. For a broader look at what to expect, this guide on navigating perimenopause is a fantastic resource.
Even though it’s common, it's still smart to know the difference between typical spotting and bleeding patterns that warrant a call to your clinician.
To help you distinguish between the two, we've created a quick-reference table.
Quick Guide to Perimenopause Spotting
This simple guide can help you figure out if what you're seeing is typical for this transition or if it’s time to seek medical advice.
Bleeding Pattern | What It Typically Means | Recommended Action |
|---|---|---|
Light, brown or pink spotting | Old or minimal blood from an unstable uterine lining. Very common. | Track the frequency and timing in an app like Lila to identify your personal patterns. |
Spotting that is brief and inconsistent | A classic sign of fluctuating hormones and unpredictable ovulation. | Continue monitoring. If it doesn't disrupt your life, it's often considered normal. |
Heavy bleeding or post-sex bleeding | This could signal issues like fibroids, polyps, or significant vaginal dryness. | Schedule an appointment with your healthcare provider to investigate the cause. |
Ultimately, tracking your symptoms is the best way to understand your unique pattern and feel more in control.
The Hormonal Fluctuations Behind Irregular Spotting
So, why the sudden, unexpected spotting? The answer lies in the hormonal shifts that have directed your menstrual cycle for decades. For years, your two primary hormones—estrogen and progesterone—have worked together in a predictable rhythm. Perimenopause is simply the phase where this long-running partnership starts to become less reliable.
It helps to think of your uterine lining (the endometrium) as a garden that’s tended to each month. In this garden, your hormones are the gardeners.
Estrogen is the builder: It’s responsible for creating a thick, nutrient-rich layer of tissue in your uterus. Think of it as laying down fertile soil.
Progesterone is the sustainer: It arrives after ovulation to keep that uterine lining stable and healthy, ready for a potential pregnancy. It’s like a consistent watering schedule that keeps the soil intact.
For most of your life, this teamwork ensures your lining builds up and then sheds on a predictable schedule, which you know as your period. But during perimenopause, the gardeners start missing their shifts.
The Unpredictable Garden
As your body makes its way toward menopause, ovulation becomes less consistent. Some months it happens, other months it doesn't. This is the key change that throws your hormone levels—and your entire cycle—off-kilter.
Estrogen can spike and then crash without warning, causing the uterine lining to build up in uneven patches. At the same time, without regular ovulation, progesterone levels often stay low. This means the lining doesn't get the stability it needs to hold together.
Imagine your garden being over-fertilized one week (an estrogen surge) and then completely neglected the next (no progesterone). The soil becomes unstable, and small sections start to crumble and break away at random.
This crumbling is precisely what’s happening inside your uterus. Little bits of that unstable lining shed at unpredictable times, leading to the light, often brownish or pinkish, spotting you see between periods. It’s not a full-blown period, just a direct result of this hormonal chaos. If you're wondering where your own hormones might stand, you can learn more about normal estradiol levels and how they fluctuate.
How Spotting Patterns Evolve
Perimenopause isn’t one single event; it's a gradual transition with different stages. Your spotting patterns will likely change as you move through it, and knowing what to expect can make the whole process feel a lot less mysterious.
Early Perimenopause: In the beginning, you might just notice your cycles getting a bit shorter or longer. Spotting could show up a few days before your period is due or hang around for a bit after it ends. It's often sporadic and might not even happen every month.
Late Perimenopause: As you get closer to your final period, the hormonal swings become more dramatic. This is often when you'll see:
More anovulatory cycles: These are months where you don't ovulate, which means no progesterone is produced to stabilize your uterine lining.
Longer gaps between periods: It’s common to go 60 days or more between bleeds.
Increased spotting: With a chronically unstable lining, random spotting can become much more frequent.
While it can be frustrating, this phase is a clear indicator that your body is nearing the end of its reproductive chapter. By understanding that these hormonal shifts are the root cause, you can see perimenopausal spotting for what it is—a normal, predictable part of a natural process. Tracking these symptoms in an app like Lila can give you a clear record of your unique patterns, which is invaluable information to share with your clinician.
Other Common Causes of Perimenopause Spotting
While your hormones are the main culprits behind that frustrating, unpredictable spotting, they're not always working alone. Think of your cycle as an intricate orchestra. When the lead violinists (estrogen and progesterone) start playing off-key, it's noticeable. But sometimes, a few other instruments are slightly out of tune too, adding to the racket.
Several other very common—and usually harmless—conditions can cause unexpected bleeding during perimenopause. Knowing what they are can help you make sense of what's happening and have a much clearer conversation with your doctor.
Vaginal Dryness and Atrophy
One of the first things many women notice is that falling estrogen doesn't just mess with their periods; it affects other tissues, too. Your vaginal tissues are very sensitive to estrogen.
When estrogen levels dip, the walls of the vagina can become thinner, less flexible, and much drier. We call this vaginal atrophy, or more formally, genitourinary syndrome of menopause (GSM).
A helpful way to picture this is to think of a plump, juicy grape versus a raisin. Healthy, estrogen-rich vaginal tissue is like the skin of the grape—resilient and moist. But as estrogen declines, that tissue can become more like a raisin: thinner, drier, and more delicate.
Because the tissue is so fragile, even a little friction from sex, a pelvic exam, or sometimes just vigorous exercise can cause tiny tears and a bit of spotting. It’s nothing to be alarmed about, but it’s a very real effect of your changing hormones.
Uterine Fibroids and Polyps
It’s also worth looking at the physical structure of the uterus itself. Often, perimenopause is when benign growths that you never even knew you had decide to make themselves known.
Uterine Fibroids: These are non-cancerous growths that develop from the muscle wall of the uterus. They are incredibly common, affecting up to 80% of women by the time they reach 50. Many women have them with zero symptoms, but the wild hormonal swings of perimenopause can trigger them to bleed irregularly.
Uterine Polyps: These are different from fibroids. They are small, soft overgrowths of the uterine lining (the endometrium). While polyps are also almost always benign, they can definitely cause spotting between periods or after sex simply because they disrupt the otherwise smooth surface of the uterine lining.
Think of these growths as little bumps in the road for your uterine lining. They can cause small areas to shed unpredictably. While they aren't typically dangerous, they are a frequent reason for the kind of bleeding that should get checked out.
The Role of Ovulation Spotting
Even though your cycles are becoming erratic, ovulation doesn’t just stop overnight. In the early stages of perimenopause, your body is still trying to release an egg each month, even if its timing is all over the place.
This process of releasing an egg can sometimes cause a tiny bit of bleeding on its own, known as ovulation spotting. It’s usually triggered by the sharp dip in estrogen that happens right as the follicle bursts. This might be something you've experienced before, but it can feel more random and confusing now that you can't predict when, or if, you're ovulating.
For most women in perimenopause, occasional light spotting without other symptoms is just part of the deal. Things like vaginal dryness, irritation after sex, or even ovulation spotting are often the simple explanation. The real challenge is knowing when the spotting is just "normal for perimenopause" versus a sign that you need to see your doctor. You can find more helpful context on spotting on The Virginia Center for Women's website.
Getting a handle on these other potential causes gives you a much fuller picture. If you start tracking when your spotting happens—is it only after sex? Or does it seem to be in the middle of a cycle?—you’ll collect valuable clues. A detailed record, which is easy to keep using an app like Lila, can be a game-changer when you and your doctor are trying to connect the dots.
Even though spotting between periods is a common sidekick to perimenopause, it’s not something you should ever completely ignore. The hormonal chaos of this transition means some irregular bleeding is par for the course, but that doesn't mean we brush it all off.
Think of spotting as a "check engine" light for your body. Most of the time, it's just a minor hiccup—the hormonal equivalent of a loose gas cap. But you always get the light checked, right? Just in case. Learning to recognize which signs are minor and which are more urgent is the key to trading worry for confidence.
Certain bleeding patterns are your body’s way of saying, "Hey, let's get this checked out." This guide will help you know when it's time to call your doctor.
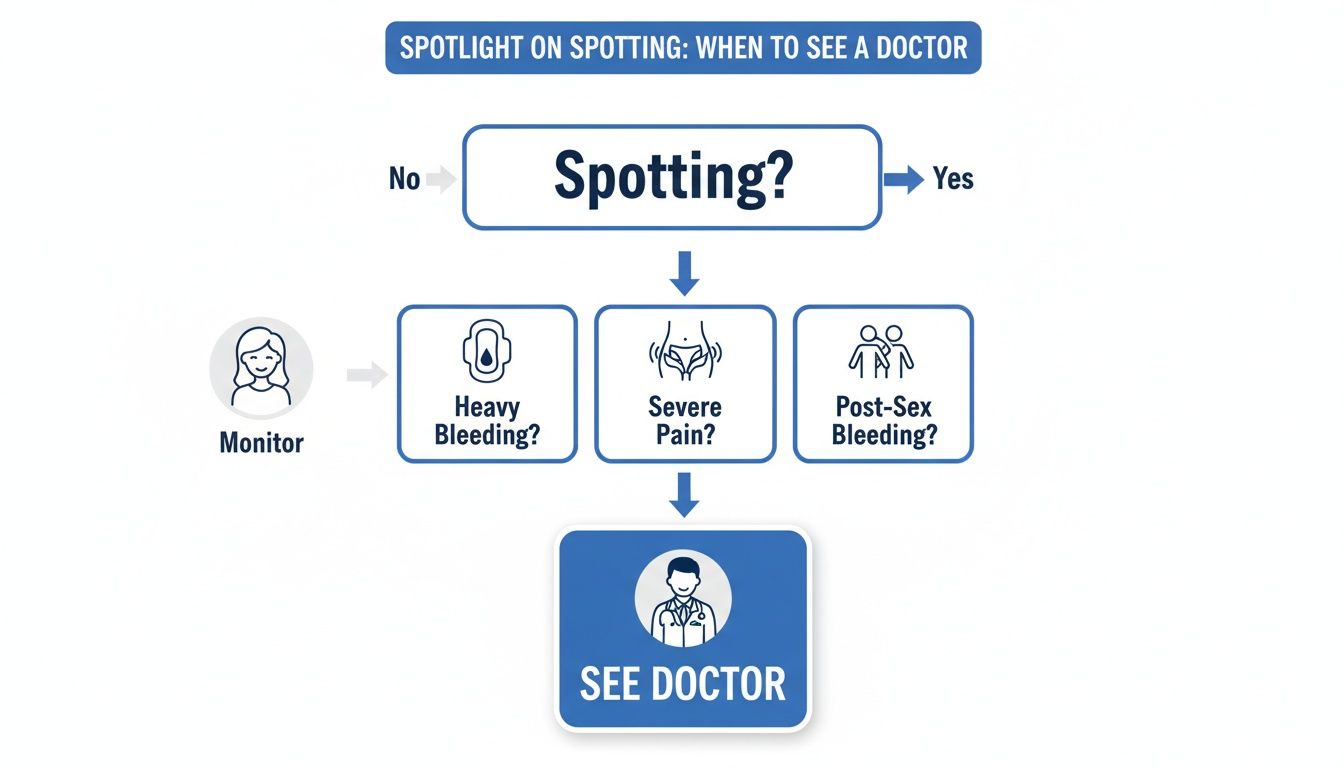
As you can see, while occasional spotting is one thing, other symptoms like a super heavy flow, pain, or bleeding after sex are clear signals that you need a professional opinion.
Spotting That Needs a Closer Look
So, what exactly should raise a red flag? It’s not just about noticing some blood; it’s about the pattern, the amount, and what else is happening in your body at the same time. If any of the following sound familiar, it's time to book that appointment.
You're bleeding through pads or tampons every hour. Let's be clear: this isn't spotting. Typical perimenopausal spotting is light, often just a few drops you notice when you wipe. If you’re soaking a pad or tampon every hour for several hours, this is considered heavy uterine bleeding and needs to be evaluated by a doctor right away.
You're bleeding after sex. Spotting or bleeding that consistently shows up after you've been intimate is a definite red flag. Sometimes, the cause is simple, like the vaginal dryness and thinning tissue that can come with hormonal changes. However, it can also point to issues with your cervix, or things like uterine polyps or fibroids. It's impossible to know without getting it checked.
You're feeling pain. Normal hormonal spotting shouldn't hurt. If your spotting comes with new or worsening pelvic pain, cramping that feels different from your usual period, or a heavy, dragging pressure in your lower abdomen, please don't just "power through." Pain is your body's most direct way of asking for help.
The One Red Flag You Can Never Ignore
There is one rule in this journey that is absolute, with no exceptions. You must see a doctor if you have any bleeding at all after you've officially reached menopause.
Menopause isn't a gradual slide; it has a clear definition: going 12 consecutive months without a single period.
After you've crossed that one-year, period-free finish line, any bleeding that follows is called postmenopausal bleeding. Even the tiniest pink or brown spot on the toilet paper requires an immediate call to your doctor. While the cause is often something benign, it must be investigated to rule out endometrial cancer. Your health is the number one priority.
Keeping a clear record of your symptoms in an app like Lila can make a world of difference. When you can show your doctor a detailed log of your bleeding patterns, flow, and any other symptoms, you transform a vague conversation into a productive one, helping you get the answers and peace of mind you deserve.
How to Track Your Symptoms for a Clearer Picture
When you're in the thick of perimenopause, trying to remember when you spotted last month—let alone the color or flow—is a tall order. Your cycles can become so unpredictable that relying on memory just doesn't cut it. This is where getting serious about tracking becomes your secret weapon.
Think of it as being a detective for your own body. Instead of feeling lost and just reacting to whatever happens next, you're gathering clues. A simple notebook or a dedicated app turns confusing experiences into a clear, factual record, helping you spot patterns you would have otherwise missed entirely.

This visual log helps you establish what your "new normal" looks like during this transition, giving you something tangible to work with.
What to Log for Maximum Clarity
To really understand what's going on, you'll want to jot down more than just your period's start and end dates. The real insights are found in the details. Try to make a daily habit of noting the following:
Bleeding Dates: Mark every single day you see blood, no matter how insignificant it seems. Was it a full period or just a hint of spotting?
Flow Intensity: Create your own simple scale. For instance: spotting (only when wiping), light (panty liner is enough), medium (needs a regular pad/tampon), or heavy (requiring frequent changes).
Blood Color: The color can tell a story. Is it bright red, pink, or dark brown? Brown blood is older, while bright red is fresh. Noting the color can help you and your doctor differentiate between types of bleeding.
Associated Symptoms: Your cycle is so much more than bleeding. Are you also experiencing cramps, bloating, mood shifts, headaches, or pelvic pain? Connecting these physical and emotional feelings to your bleeding patterns is crucial.
By consistently logging these details, you shift from being a passive passenger on the perimenopause rollercoaster to being an informed navigator. You start to see connections—for instance, maybe your spotting only happens after a stressful week or is consistently brown and light.
This information isn't just for you. It’s the single most valuable thing you can bring to a conversation with your clinician.
Transforming Your Doctor's Visit
Think about the difference between these two appointments. In the first, you tell your doctor, "I think I've been spotting a lot, and my periods are just weird." It's a valid concern, but it’s vague and relies entirely on memory.
Now, picture this instead. You walk in, open your notes, and say, "For the past four months, I've had brown spotting for 3-5 days right in the middle of my cycle. It's usually light, but I noticed last month it came right after a really stressful week and I had mild cramps with it. You can see the whole pattern right here in my chart."
The second approach changes everything. A detailed log moves the conversation from guesswork to a focused, data-driven consultation. Your doctor can immediately see the frequency, duration, and character of the bleeding, which helps them ask better questions and arrive at a diagnosis more efficiently.
You become an active partner in your own health. Armed with your own data, you can advocate for yourself with confidence and clarity, ensuring your concerns are fully heard. If you're looking for a tool to help, our guide to the best cycle tracking apps is a great place to start.
What to Expect at Your Doctor's Appointment
▶ PlayDeciding to finally see a doctor about spotting is a big step, but it’s easy to feel a little anxious about the appointment itself. Knowing what’s coming can make the whole process feel much less intimidating. Think of this visit as a fact-finding mission—you and your clinician are simply partners trying to figure out the story your body is telling.
The visit will always start with a conversation. This is where all that symptom tracking you’ve been doing really shines. Be prepared to talk about what you've noticed: how often the spotting happens, what color it is, how heavy it is, and if you're experiencing anything else, like pain or bleeding after sex. Your doctor will also want to know about your personal and family medical history.
The Initial Examination
After you talk, your doctor will likely want to do a physical exam, which includes a pelvic exam. Let’s be honest, they’re not anyone’s favorite thing, but it’s a quick and incredibly important step.
During the exam, your clinician can look for any obvious reasons for the bleeding. They’ll check your vagina and cervix for things like polyps, thinning tissues (vaginal atrophy), or other visible issues. If you’re due for one, they might do a Pap smear at the same time. This initial look gives them crucial clues and helps them figure out what, if anything, to do next.
Common Diagnostic Tools and Tests
If the physical exam doesn't give a clear-cut answer, your doctor might recommend a few other tests. These are all standard procedures designed to get a better look at what’s going on with your hormones and inside your uterus.
Here are some common next steps:
Transvaginal Ultrasound: This is an imaging test that uses a small probe (about the size of a tampon) inside the vagina to get a crystal-clear picture of your reproductive organs. It’s the best way to see things like fibroids or polyps and to measure the thickness of your uterine lining, called the endometrium.
Blood Tests: A simple blood draw can tell you a lot. It can check your hormone levels (like FSH and estrogen) to see where you are in the perimenopause transition, look at your thyroid function, and check for anemia if the bleeding has been particularly heavy.
Endometrial Biopsy: Don't let the word "biopsy" scare you. If your ultrasound shows a thicker uterine lining or if you have other risk factors, your doctor might suggest this. A tiny sample of tissue is taken from the lining of your uterus and sent to a lab to make sure the cells are healthy.
Knowing what these procedures are ahead of time can take the fear out of the appointment. Each test is just a tool to help you and your doctor get the answers you deserve for your own peace of mind.
Walking into your appointment prepared can make all the difference. For a more detailed breakdown of the tests involved, you can read our guide on how to test for menopause.
Your Perimenopause Spotting Questions, Answered
When you start seeing spotting between periods, the questions can start piling up. It’s a confusing time, and it's easy to wonder what's normal and what's not. Let's walk through some of the most common questions and concerns that come up during this transition.
Does Stress Really Make Perimenopause Spotting Worse?
It’s a connection many women notice, and they’re right. When you’re under a lot of stress, your body pumps out more of the hormone cortisol. This isn't just a mental state; it has a very real, physical impact.
Think of your cycle as a delicate hormonal orchestra. During perimenopause, the musicians (estrogen and progesterone) are already a bit out of sync. High cortisol levels act like a loud, disruptive noise that throws off their timing even more. This disruption can easily lead to more frequent or heavier spotting.
Making time for things that genuinely lower your stress—whether that's a walk in nature, mindfulness exercises, or simply carving out quiet time for yourself—is one of the most powerful, non-medical things you can do to support your body.
What's the Difference Between Brown and Red Spotting?
The main difference between seeing brown or red spotting is simply how old the blood is. It’s a clue about how quickly the blood left your body after being shed.
Bright Red Spotting: This is fresh blood. It means the bleeding is happening now, and the blood is exiting your body quickly without having time to oxidize.
Brown Spotting: This is older blood. It has been sitting in the uterus or vagina for a while and has reacted with oxygen, which causes it to turn brown. It’s a sign of a slower flow.
It’s completely normal to see both, sometimes even on the same day. While the color provides a little bit of information, it’s not usually a red flag on its own. What your clinician will really want to know about is the amount, frequency, and timing of any bleeding.
A consistent log of your symptoms—noting patterns rather than just color—is what gives you and your doctor the clearest picture of what’s happening with your health.
How Long Is Perimenopause Spotting Supposed to Last?
This is the million-dollar question, and unfortunately, there’s no single answer. The perimenopause journey is incredibly individual. The entire transition itself can last anywhere from 4 to 10 years.
Some women experience occasional spotting for just a year or two, while for others, it can be an on-and-off companion throughout the entire phase. Spotting often becomes more frequent and unpredictable in the late stage of perimenopause, which is typically the final one to three years before your periods stop for good.
Since there's no universal timeline, the best approach is to get to know your personal pattern. Tracking your unique experience is the only way to understand what's normal for your body and have truly productive conversations with your healthcare provider.
Instead of guessing, you can turn your daily symptoms into clear, actionable insights. Lila helps create a personalized plan based on how you feel each day, making it easier to spot patterns and feel more in control. Start your journey by downloading the app at getlila.com.
Get Lila, your personal coach for perimenopause.
Built for women in their 40s. 24/7 coaching, in your pocket.


