
Your Guide to Every Test for Menopause in 2026
Mar 10, 2026
It’s one of the first questions most of us ask: Is there a simple test for menopause? It would be great if there were, but the short answer is no. Menopause is diagnosed clinically, meaning it's confirmed after you’ve gone 12 consecutive months without a period. It's a conclusion based on your body's story, not a single lab report.
The Real Answer on Testing for Menopause
It’s completely understandable to assume there’s a straightforward test that can tell you, "Yes, you're in perimenopause," or "You've officially hit menopause." In reality, though, it’s far more nuanced. While tests do exist, they only give you a snapshot in time—a single frame from the full-length feature film of your hormonal transition.
Think of your hormones during perimenopause like a once-orderly orchestra that’s suddenly gone rogue. For years, everything was in sync. Now, the musicians (your ovaries) are starting to pack up, and the conductor (your brain) is yelling louder and louder, trying to keep the music going. This chaos causes your hormone levels to swing wildly, not just month-to-month, but sometimes even day-to-day.
A hormone test taken on a Monday could show results that look completely different from a test taken that same Friday. This is the core reason why a single test isn't a reliable tool for diagnosing menopause.
Setting Realistic Expectations for Testing
So, if a test can't give you a clear-cut diagnosis, what’s the point? Their real value lies in helping you and your doctor rule out other health conditions that can masquerade as menopause. Getting a complete picture of your health is the most important first step.
Many symptoms we associate with menopause can overlap with other issues, such as:
Thyroid Disorders: An underactive thyroid can bring on fatigue, weight gain, brain fog, and hair thinning—all classic signs of perimenopause.
Vitamin or Mineral Deficiencies: Being low in iron or vitamin B12 can cause deep fatigue and cognitive fuzziness that are easily mistaken for hormonal shifts.
Other Hormonal Conditions: Rarely, conditions like Cushing's disease can cause symptoms like weight gain and fatigue that could be confused with menopause.
Navigating this transition is a key part of overall women's health. A good clinician uses testing not to put a label on your menopause status, but to make sure nothing else is being missed.
Why Your Symptoms Tell the Real Story
Ultimately, the most important information comes directly from you. Your experience—your changing menstrual cycles, the hot flashes that wake you up at night, the new brain fog—tells a much more compelling story than any single number on a lab report.
The chart below provides a quick overview of the tests you might encounter. Think of it as a field guide to help you understand what each test does and where it fits in.
Quick Guide to Menopause-Related Tests
Test Type | What It Measures | Role in Diagnosing Menopause |
|---|---|---|
Follicle-Stimulating Hormone (FSH) | A brain hormone that signals the ovaries to release an egg. | Levels rise during perimenopause but fluctuate wildly, making it unreliable for diagnosis. Best used to rule out other issues. |
Estradiol (E2) | The main form of estrogen produced by the ovaries. | Levels drop as menopause approaches, but they also fluctuate significantly. Not used for diagnosis. |
Anti-Müllerian Hormone (AMH) | Reflects the size of your remaining egg supply (ovarian reserve). | Declines with age, giving a general idea of your reproductive timeline, but it can’t pinpoint the start of menopause. |
Thyroid-Stimulating Hormone (TSH) | Checks how well your thyroid is functioning. | Essential for ruling out thyroid disorders, which have symptoms that mimic menopause. |
Complete Blood Count (CBC) | Assesses overall health, including red and white blood cells. | Can detect anemia (low iron), which causes fatigue and can be confused with a menopause symptom. |
This guide will walk you through what these clinical and at-home tests can—and, more importantly, cannot—tell you. Our goal is to equip you with the knowledge to have confident conversations with your doctor, so you can focus on what truly matters: managing your symptoms and feeling your best.
Understanding the Hormones Behind Your Symptoms
Before we can even talk about what a menopause test can tell you, we need to get to know the key hormones they’re looking for. For decades, your reproductive hormones have worked together like a beautifully synchronized orchestra. As you head into perimenopause, that familiar rhythm starts to change.
The main players in this shift are Follicle-Stimulating Hormone (FSH), estradiol (your body's most active estrogen), and Anti-Müllerian Hormone (AMH). The once-seamless communication between your brain and ovaries is getting a little less efficient, and that miscommunication is what’s driving your symptoms.
The Brain and Ovaries Start a New Conversation
Think of it this way: your brain is the conductor, and your ovaries are the star musicians. The conductor uses a hormone called FSH to signal to the ovaries that it's time to mature an egg. But as we age, our ovaries naturally have fewer eggs left and become less responsive to that signal.
So, what does the brain do? It starts "shouting" by pumping out more and more FSH to get the ovaries' attention. This is why a consistently high FSH level is a classic hallmark of the menopausal transition—it’s a clear sign your brain is working overtime to get a response.
This dynamic is the core of what menopause testing is trying to capture. An elevated FSH level on a test is simply evidence that your brain is raising its voice because your ovaries aren't listening like they used to.
While your brain is trying to be heard, your ovaries' response becomes completely unpredictable. Estradiol, the powerful hormone that keeps everything from your body temperature to your mood in check, starts to spike and crash without warning. You can have days of extremely high estrogen followed by days of rock-bottom lows.
This hormonal rollercoaster is the direct culprit behind many of the classic symptoms of perimenopause:
Hot Flashes: Sudden nosedives in estrogen can throw your brain's internal thermostat into chaos.
Mood Swings: Unstable estrogen levels mess with brain chemicals like serotonin, which can make you feel all over the place emotionally.
Irregular Periods: When hormonal signals are chaotic, your cycle length and flow become unpredictable.
This is precisely why a single test for menopause can be so misleading. A blood test is just a snapshot in time—it might catch your estrogen on a high day or a low day, but it can’t show the chaotic up-and-down pattern that truly defines this transition. You can learn more about how these changes fit into the bigger picture in our guide to the stages of perimenopause.
AMH and Your Ovarian Reserve
Then there's the other key hormone, Anti-Müllerian Hormone (AMH). AMH is produced in your ovarian follicles, so its level gives us a rough estimate of your remaining egg supply—what clinicians call your ovarian reserve.
Unlike the wild swings of FSH and estradiol, AMH levels tend to be much more stable throughout your cycle. Your AMH level naturally and gradually declines with age. While a low AMH confirms your ovarian reserve is getting smaller, it absolutely cannot predict when you’ll hit menopause. It just tells you that you're on the path, not where you are on the map.
Think of it like the gas gauge in your car. It tells you that the tank is getting low, but it can't tell you the exact mile you’ll sputter to a stop.
If you bring up perimenopause with your doctor, they’ll likely recommend a few blood tests. It’s a common first step. But here’s something that surprises a lot of women: these tests aren’t really meant to diagnose perimenopause. So what’s the point?
Think of these tests as important fact-finding tools. They help your doctor build a case, rule out other culprits for your symptoms, and get a baseline for your unique hormonal signature. Knowing what the tests can—and can't—tell you is crucial for making sense of the results.
The Big Three: FSH, Estradiol, and AMH
The most common hormone your doctor will look at is Follicle-Stimulating Hormone (FSH). Your brain sends out FSH to tell your ovaries, "Hey, time to get an egg ready!" As you get older, your ovaries don't listen as well. So, your brain has to shout louder, which means your FSH levels start to climb.
A consistently high FSH level, often over 30 mIU/mL, is a strong clue that you're in the menopause transition. But the key word here is consistently.
This is the biggest hurdle with testing for perimenopause: your hormones are all over the place. One day your FSH could be sky-high, and the next week it might be back in the "normal" range. A single test is just one snapshot in time, and it doesn't tell the whole story. It’s the trend over time, combined with your symptoms, that gives your doctor a much clearer picture.
This is the hormonal push-and-pull that the tests are trying to measure.
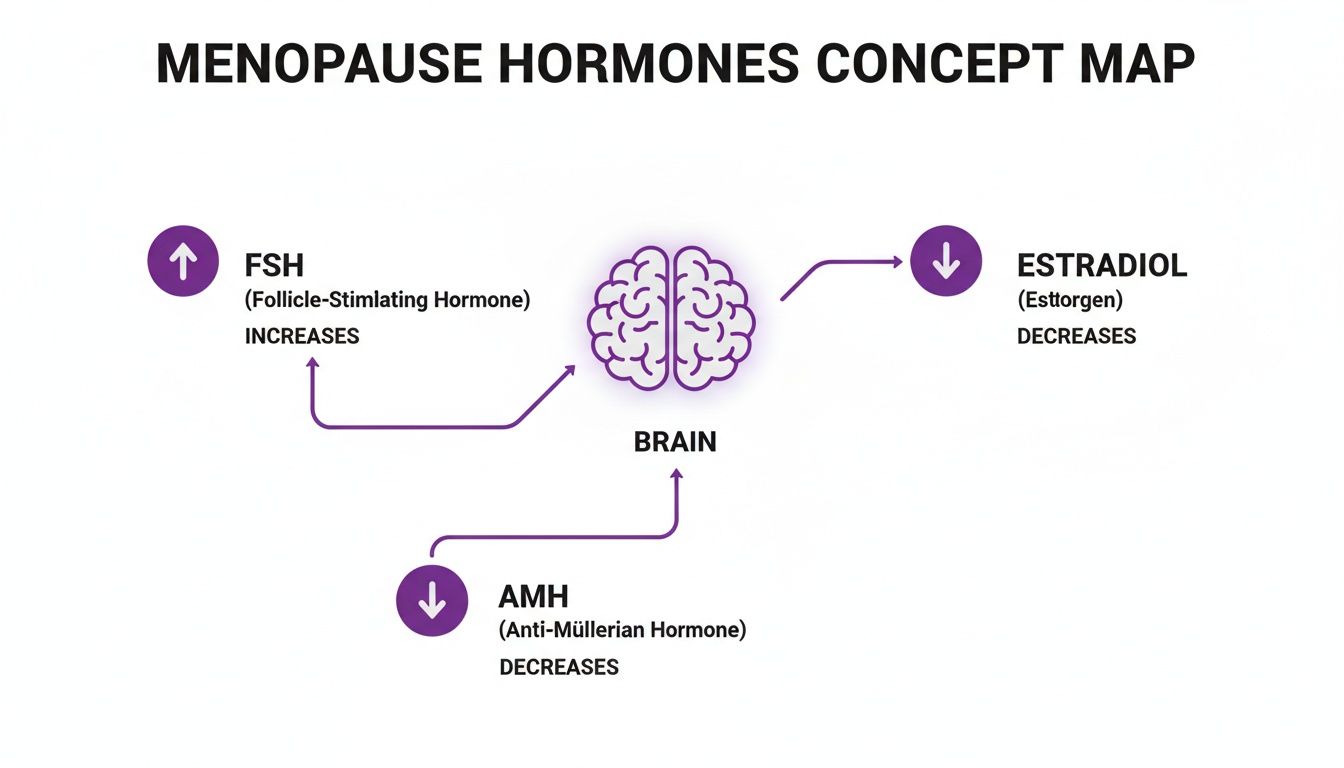
As you can see, the brain ramps up FSH production trying to get the ovaries to respond, while the ovaries' output of estradiol and AMH (another key fertility hormone) dwindles.
So, What Are These Tests Actually Good For?
Your doctor might also test your estradiol (the main form of estrogen). While low levels can confirm you're postmenopausal, this test is even less reliable for diagnosing perimenopause. Just like FSH, your estrogen can be on a real rollercoaster. A test could easily catch you on a high-estrogen day, giving you a completely misleading result.
If these tests can't give a straight "yes or no" on perimenopause, why bother? They actually serve a few very important purposes:
Ruling Out Lookalikes: So many perimenopause symptoms—fatigue, brain fog, mood swings, weight gain—look exactly like symptoms of other conditions, especially thyroid problems. A simple blood test can quickly rule out a thyroid disorder, making sure you're treating the right thing.
Getting a Baseline: If you and your doctor are talking about hormone therapy (HT), getting your levels tested beforehand is essential. It gives you a starting point to see how well the treatment is working and allows for adjustments down the road.
Investigating Early Menopause: For women under 40 who are having menopause-like symptoms, hormone testing is absolutely critical. It helps doctors investigate conditions like Primary Ovarian Insufficiency (POI) and get a diagnosis sooner.
To get a more holistic view, some doctors use a specialized Perimenopause Health Panel. These comprehensive panels go beyond just FSH and estradiol, looking at other markers to create a more complete health profile.
In the end, clinical tests are just one piece of the puzzle. Your doctor will use the results, along with your personal symptom journal and health history, to see the whole picture. It’s about gathering all the clues to make sure the advice and care you receive are right for you.
Are At-Home Menopause Tests Worth It?
Walk down any pharmacy aisle or scroll online, and you'll find them: direct-to-consumer kits promising to tell you if you're in menopause. They feel empowering, offering a quick, private way to get what seems like a straightforward answer. But before you add one to your cart, it’s important to know what these tests can—and more importantly, cannot—tell you.
Most of these kits are a lot like an at-home pregnancy test. They’re simple urine tests, but instead of looking for pregnancy hormones, they measure Follicle-Stimulating Hormone (FSH). A positive result just means the test has picked up FSH levels above a certain point, usually around 25 mIU/mL.
How to Interpret the Results
So, what does it mean if you get a positive result on an at-home menopause test? It tells you that your brain is pumping out more FSH, likely because it’s working harder to get your ovaries to respond. This is a classic sign of the menopausal transition, so a positive result can confirm you’re on that path.
A negative result, however, is where things get tricky. It absolutely does not mean you aren't in perimenopause. Your hormones can swing wildly from day to day during this time, so a negative result might just mean you caught your FSH on a low day. This is the single biggest pitfall of a one-off test.
Think of a single at-home FSH test like checking the weather at 8 AM. Just because it’s sunny then doesn't mean it won't be pouring rain by lunchtime. A single snapshot of your hormones can be just as misleading.
This is exactly why these tests can feel so confusing. You might get a negative result one week, feel completely invalidated because your symptoms are screaming "perimenopause," and then test positive a month later. It's a hormonal rollercoaster, and a single snapshot just can’t capture the whole ride.
The Risks of False Reassurance and Unnecessary Anxiety
While they seem convenient, at-home tests can create their own emotional whirlwind. A negative result can give you a dangerous dose of false reassurance, causing you to dismiss your symptoms or put off talking to a doctor. You might think, "Well, the test was negative, so my brain fog and hot flashes must be something else," when you're actually dealing with classic perimenopause.
On the flip side, seeing a "positive" result without any medical context can trigger a wave of unnecessary anxiety. It might send you spiraling with worries about your health, fertility, or what it means to be "aging"—all without the guidance of a professional who can put the result in perspective.
It's best to think of these tests as a single clue, not the whole answer.
Benefits vs. Limitations of At-Home FSH Tests
Benefits | Limitations |
|---|---|
Convenient & Private: You can test in the comfort of your own home without an appointment. | Poor for Diagnosis: Cannot definitively diagnose perimenopause because hormones fluctuate daily. |
Can Prompt Action: A positive result might be the nudge you need to finally talk to a doctor about your symptoms. | Risk of Misinterpretation: Results can cause either false reassurance or undue anxiety without clinical context. |
Provides a Clue: Can confirm that your FSH levels are elevated, which lines up with the menopausal transition. | One-Time Snapshot Only: Fails to capture the dynamic, up-and-down nature of hormones that defines perimenopause. |
At the end of the day, an at-home test result—positive or negative—should never be the final word. Think of it as a conversation starter. The best next step is always to discuss the result, and more importantly, your symptoms, with a healthcare provider. They are the only one who can help you put that single piece of information into the larger puzzle of your health.
Why Your Symptoms Tell a Better Story Than Any Test

After seeing the limits of hormone testing, you might be wondering what you can rely on. The truth is, trying to diagnose perimenopause from a single lab result is like trying to understand a movie by looking at just one frame. The most reliable narrator for this chapter of your life is your own body.
This is why consistently tracking your symptoms is the single most powerful tool you have.
While a test for menopause gives you a snapshot in time, a symptom log is the whole photo album. It captures the day-to-day, week-to-week reality of how you're feeling, which is the information that truly matters when it comes to feeling better.
Telling Your Personal Health Story
Symptom tracking is how you turn vague feelings into concrete facts. Instead of telling your doctor, "I've just been feeling off lately," you can walk in with specific data. "For the last three months, I've had hot flashes three nights a week, usually around 2 a.m., and my mood always plummets the week before my period." Now that's a conversation starter.
Think of yourself as a detective gathering clues about your own body. By logging things like irregular periods, how intense your hot flashes are, your sleep quality, and mood swings, you start to create a detailed record.
Your symptom log is the proof that validates your experience. It shifts the conversation from, "I think this is happening," to, "Here is the data showing my patterns." This empowers you to advocate for yourself with total confidence.
With this data, you can finally start connecting the dots. Is a terrible night's sleep always followed by a day of brain fog? Do certain foods seem to trigger bloating or hot flashes? Tracking brings these connections to light, giving you the power to make real-world adjustments that can make a huge difference.
Putting Your Symptom Log to Work
Keeping a detailed log doesn't have to feel like homework. Modern apps and tools, like Lila, are designed to make it simple to record what you’re feeling and instantly see trends over time. Everything is in one place, turning a quick daily check-in into clear, visual charts that show your progress.
When you bring this organized information to your healthcare provider, you can have a much more productive conversation. Your detailed log helps them:
Spot the Patterns: Seeing the frequency and severity of your symptoms over weeks and months is far more revealing than a single hormone level.
Rule Out Other Conditions: The specific nature of your symptoms can help your doctor differentiate what’s likely perimenopause-related and what might be something else.
Create a Personalized Plan: A treatment approach for someone with severe sleep disruption will be very different from a plan for someone whose main struggle is anxiety or mood swings.
By presenting a comprehensive symptom history, you become an active partner in your own healthcare. You can work together to find strategies that are based on your unique experience, not just a number on a lab report. This is especially vital when navigating the wide array of changes that can pop up. To get a better handle on what to look for, it helps to understand the 34 symptoms of perimenopause.
In the end, while a test for menopause might offer a single clue, your symptom journal provides the entire map. It shows where you've been, where you are now, and helps you and your doctor chart the best path forward to feeling like yourself again.
When to See a Doctor and What to Discuss
While tracking your symptoms is an incredibly powerful tool, there comes a point where you need a professional’s insight. Knowing when to take your symptom log to a doctor is just as important as keeping it in the first place. Some situations are more than just a nuisance—they’re clear signals that you need medical advice.
There are a few scenarios that should have you picking up the phone to book an appointment right away. Don’t hesitate if you find yourself in one of these situations.
First and foremost, if you’re experiencing menopause-like symptoms before the age of 40, it’s time to see a doctor. This could be a sign of a condition called Primary Ovarian Insufficiency (POI), which requires a proper diagnosis and its own unique management plan.
Key Moments to Seek Medical Advice
Another major sign is when your symptoms start to get in the way of your life. Are hot flashes, brain fog, or mood swings making it hard to function at work? Is your sleep so disrupted that you can't get through the day? If your quality of life is taking a nosedive, you don’t have to just power through it. Professional support can make a world of difference.
Finally, any bleeding after you have officially reached menopause is a red flag. Once you've gone 12 consecutive months without a period, any spotting or bleeding is considered postmenopausal bleeding and must be checked out by a doctor to rule out more serious health issues.
Think of your doctor's appointment as a crucial planning session for your health. The better prepared you are, the more you’ll get out of it. Your job is to bring the real-world data; your doctor's job is to help you make sense of it.
A little prep work before your visit can transform the entire conversation. Walking in with organized information helps you advocate for yourself and ensures you and your doctor can create a meaningful plan together.
Your Pre-Appointment Checklist
To have a focused and effective discussion, try to gather these things before you go. This will help you feel more confident and in control.
Your Symptom Log: This is your single most important piece of evidence. Bring your journal, notes, or app data showing what you’ve been experiencing over the last few months.
List of All Medications and Supplements: Jot down everything you take, including vitamins, herbs, and over-the-counter remedies. This helps your provider spot potential conflicts or side effects.
Family Health History: Make a note of any close relatives with a history of thyroid disease, heart disease, osteoporosis, or specific cancers. This gives your doctor important context about your personal risk factors.
Your Top Questions: Come with 3-5 of your most pressing questions written down. Do you want to know if you need a specific test for menopause? Are you curious about Hormone Replacement Therapy (HRT)? Wondering about non-hormonal options?
With this information in hand, your visit becomes a true partnership. You can work with your provider to decide if other tests are needed to rule out different conditions, explore treatments that fit your specific symptoms, and build a clear roadmap for feeling better.
If you're wondering where you might be on your own journey, our menopause age calculator can offer some perspective. This kind of groundwork is what empowers you to take the next step, whether that involves lifestyle changes, medication, or simply a good plan for monitoring your health going forward.
A Few Common Questions About Menopause Tests
When it comes to menopause testing, it’s completely normal to have a lot of questions. With so much information floating around, it's easy to feel lost about what the results really mean and what to do next. Let's clear up some of the most common points of confusion.
Can a Blood Test Give Me a Definitive Perimenopause Diagnosis?
The short answer is no. A single blood test simply can't tell you for sure that you're in perimenopause, and here’s why: this transition is defined by hormonal chaos. Your levels of key players like FSH and estrogen don't just shift month-to-month; they can swing wildly from one day to the next.
Think of a blood test as a single snapshot of a very long, very turbulent movie. It might catch your hormones on a "good" day or a "bad" day, but it completely misses the bigger picture of all the ups and downs. That's why clinicians rely on your age, the changes in your menstrual cycle, and your overall pattern of symptoms to diagnose perimenopause.
What Does a High FSH Level Mean?
A consistently high level of Follicle-Stimulating Hormone (FSH)—usually anything over 30 mIU/mL—is a classic sign that your ovaries are starting to respond less to your brain's signals. Your brain produces FSH to tell the ovaries to get an egg ready. When the ovaries don't listen as well as they used to, your brain essentially has to "shout" by sending out more and more FSH.
But the key word here is consistently. Because your hormones are on such a rollercoaster, one high reading isn't enough to go on. It's just one piece of the puzzle that needs to be considered alongside your symptoms and menstrual history.
Are At-Home Menopause Tests Accurate?
At-home tests, which typically measure FSH in your urine, can accurately tell you if your FSH is elevated at that moment. In that very specific sense, they work.
The problem is that detecting a single spike in FSH isn't the same as getting a reliable diagnosis. A negative result from an at-home test for menopause doesn't mean you're not in perimenopause, and a positive result just confirms what your symptoms are probably already telling you. You should never use them to make medical decisions without first talking to your doctor.
Their real value is often as a conversation starter—a little nudge to book that appointment with your healthcare provider. They give you a clue, but they don't tell the whole story.
So, How Is Menopause Officially Diagnosed?
Menopause isn't diagnosed with a lab result; it's a clinical diagnosis based entirely on your life experience. A doctor will officially confirm you've reached menopause only after you have gone 12 consecutive months without a period. For women over 45, no blood test is needed for this.
Perimenopause, the phase leading up to that point, is diagnosed by recognizing a pattern of classic symptoms. This includes things like:
Changes in your period (becoming irregular, heavier, or lighter)
Hot flashes and night sweats
Sleep that's suddenly a struggle
Mood swings, irritability, or new-onset anxiety
Brain fog and trouble with memory
It’s the combination of these symptoms over time, paired with your age, that gives a clinician the confidence to make a diagnosis and start helping you find relief. The most powerful "test" you have is tracking your own experience.
Feeling overwhelmed by symptoms and unsure of your next move? Lila is an AI-powered app that helps you connect the dots. By tracking your symptoms, meals, and cycles, Lila builds a personalized action plan so you know exactly what to do to ease hot flashes, sleep better, and stabilize your mood. Find your path to feeling better and regain control by learning more at https://getlila.com.
You should not have to do it all on your own









