
Normal Estradiol Levels and Your Hormone Health in 2026
Mar 17, 2026
When we talk about “normal” estradiol levels, one of the biggest misconceptions is that we’re looking for a single, perfect number. The truth is, there isn't one. Estradiol is a dynamic hormone, and its levels are meant to rise and fall in a predictable rhythm throughout your life.
For women in their reproductive years, levels can swing from 30 to 400 pg/mL. After menopause, however, they typically settle below 30 pg/mL. It’s less about a static number and more about a healthy, predictable flow.
What Normal Estradiol Levels Look Like
Think of your hormones, especially estradiol, as a tide. They ebb and flow throughout your menstrual cycle and across your entire lifespan, from puberty through your post-menopause years. What’s considered a "normal" estradiol level for a 25-year-old who is about to ovulate is completely different from what’s normal for a 55-year-old who is post-menopausal.
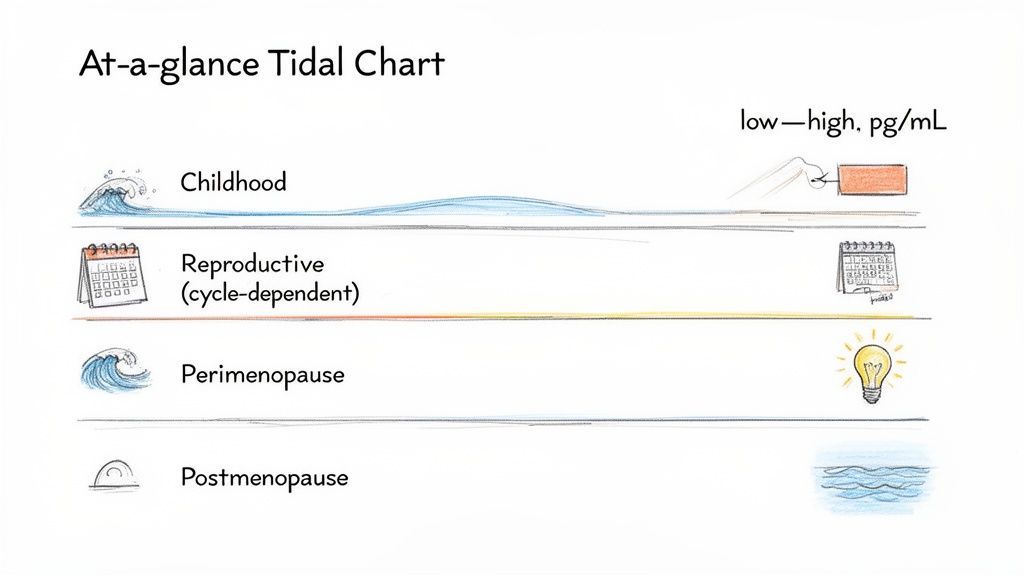
This constant fluctuation isn't a sign of a problem—it’s actually a sign of a healthy, functioning reproductive system. Instead of focusing on one number, it’s much more helpful to think in terms of reference ranges that are specific to your age and where you are in your monthly cycle.
Quick Guide to Typical Estradiol Levels (pg/mL)
To help you get a clearer picture of what this looks like, the following table provides a snapshot of typical estradiol ranges across different life stages. These are measured in picograms per milliliter (pg/mL). Remember, labs can have slightly different ranges, so this is meant to be a helpful guide, not a diagnosis.
Life Stage or Cycle Phase | Typical Estradiol Range (pg/mL) |
|---|---|
Follicular Phase (Start of Cycle) | 20 - 150 pg/mL |
Ovulation (Mid-Cycle Peak) | 150 - 750 pg/mL |
Luteal Phase (After Ovulation) | 30 - 450 pg/mL |
Perimenopause (Fluctuating) | Varies Greatly (Can be <30 or >400) |
Post-menopause (Consistently Low) | 0 - 30 pg/mL |
As you can see, the numbers vary dramatically. Perimenopause is particularly noteworthy for its wild swings, as the body’s hormone production becomes more erratic before declining to the low, stable levels of post-menopause.
The key takeaway here is that context is everything. An estradiol level of 40 pg/mL could be perfectly normal during your period or after menopause, but it would be considered low right before ovulation. This is why timing your hormone tests correctly is absolutely critical for getting an accurate reading.
Understanding these rhythms helps you make sense of your lab results and your body. It shifts the goal from chasing a "perfect" number to appreciating your body’s unique hormonal dance. This knowledge is especially empowering as you navigate perimenopause, when fluctuations can feel chaotic. Knowing what to expect allows you to have more productive conversations with your doctor and better understand the changes you're experiencing.
Understanding Estradiol's Role in Your Body
If you think of your hormones as an orchestra, then estradiol is the conductor. While most people know it as a "female sex hormone," its job goes way beyond reproduction, influencing just about every system in your body. It's the strongest and most active form of estrogen you produce during your reproductive years, and keeping it in balance is fundamental to how you feel day in and day out.
This powerhouse hormone is made mostly in your ovaries, with your adrenal glands and even fat cells pitching in a little. Production isn’t a flat line; it rises and falls in a predictable rhythm that drives your menstrual cycle and shifts dramatically throughout your life.
The Conductor of Your Physical Wellbeing
Estradiol’s to-do list is surprisingly long, with tasks that impact everything from your bones to your brain. It’s a true multitasker working behind the scenes to keep you feeling healthy and strong.
First and foremost, estradiol runs your menstrual cycle and supports fertility. It’s the hormone responsible for building up your uterine lining each month in preparation for a potential pregnancy, and it also sends the signal to your brain that it's time to ovulate. But that's just the beginning.
Here are a few of its other critical jobs:
Bone Health: Estradiol is a key regulator of bone remodeling—the natural process of replacing old bone with new. It essentially puts the brakes on bone breakdown, which is why maintaining normal estradiol levels is so vital for preventing osteoporosis later in life.
Heart Health: It does a lot for your cardiovascular system, like helping to manage cholesterol levels and keeping blood vessels flexible. This protective effect is a big reason why heart disease risk in women climbs after menopause when estradiol drops.
Skin and Hair: Ever notice your skin looks plumper and more glowy at certain times of the month? You can thank estradiol. It boosts collagen production, elasticity, and hydration in your skin and also plays a role in the health and thickness of your hair.
Think of estradiol as a crucial nutrient for your cells. When your levels are where they should be, your body's systems just work better. When they're off, you feel it everywhere—from your energy to the ache in your joints.
How Estradiol Shapes Your Mood and Mind
It's not just your body that estradiol directs; it has a massive impact on your brain and mental health, too. It helps manage key neurotransmitters like serotonin (the "feel-good" chemical) and dopamine (tied to pleasure and motivation).
This brain-hormone link is why shifts in estradiol can directly mess with your mood, memory, and focus. When your levels are balanced, you’re more likely to feel sharp, optimistic, and able to roll with the punches.
But when those levels start to dip or swing wildly, like they do in perimenopause, it can trigger symptoms that feel purely psychological but are actually rooted in your hormones:
Brain Fog: That frustrating feeling of being unable to concentrate or grasp for the right word.
Mood Swings: Suddenly feeling irritable, weepy, or anxious for no apparent reason.
Sleep Disruption: Estradiol has a hand in regulating your sleep-wake cycle. When it's low, you might find it harder to fall asleep or stay asleep, often thanks to night sweats.
Making this connection is so empowering. It's validation that you're not "just imagining things" or "being emotional"—you're having a real physiological response to a hormonal shift. Seeing estradiol as the conductor for both your physical and mental wellness is the first step in understanding why finding your normal estradiol levels is so important for feeling like yourself again.
Your Estradiol Levels Throughout the Menstrual Cycle
When we talk about normal estradiol levels, it's a mistake to think of a single, static number. A much better way to picture it is as a rhythmic hormonal wave that rises and falls throughout your menstrual cycle. This constant ebb and flow isn't just normal—it's the very engine that drives your reproductive system.
Understanding this monthly dance is key, as it highlights why the timing of any hormone test is so critical. An estradiol reading from day 3 of your cycle will look wildly different from one taken on day 14, yet both can be perfectly healthy for that specific point in time.
The Follicular Phase: The Slow Build
The first part of your cycle, which kicks off on day one of your period, is known as the follicular phase. Right at the beginning, while you're menstruating, your estradiol levels are at their lowest. Think of it as the tide being all the way out.
But as the days go by, your ovaries get to work preparing a new batch of follicles, each housing an egg. These growing follicles start to produce estradiol, causing your levels to climb steadily. This slow, deliberate rise is like the tide gradually rolling back in, setting the stage for the cycle’s main event.
Ovulation: The Powerful Crest
Around the middle of your cycle, that hormonal wave is about to hit its peak. In the 24-48 hours leading up to ovulation, one dominant follicle goes into overdrive, dramatically increasing its estradiol output. This creates a massive surge that signals your brain to release luteinizing hormone (LH).
That LH surge is the final trigger, causing the follicle to rupture and release its mature egg. This is ovulation. Right before this happens, your estradiol is at its absolute highest point of the entire month. The wave has crested in a powerful peak that's essential for fertility.
This diagram shows how estradiol, produced in the ovaries, is a major player throughout your entire body and mind.
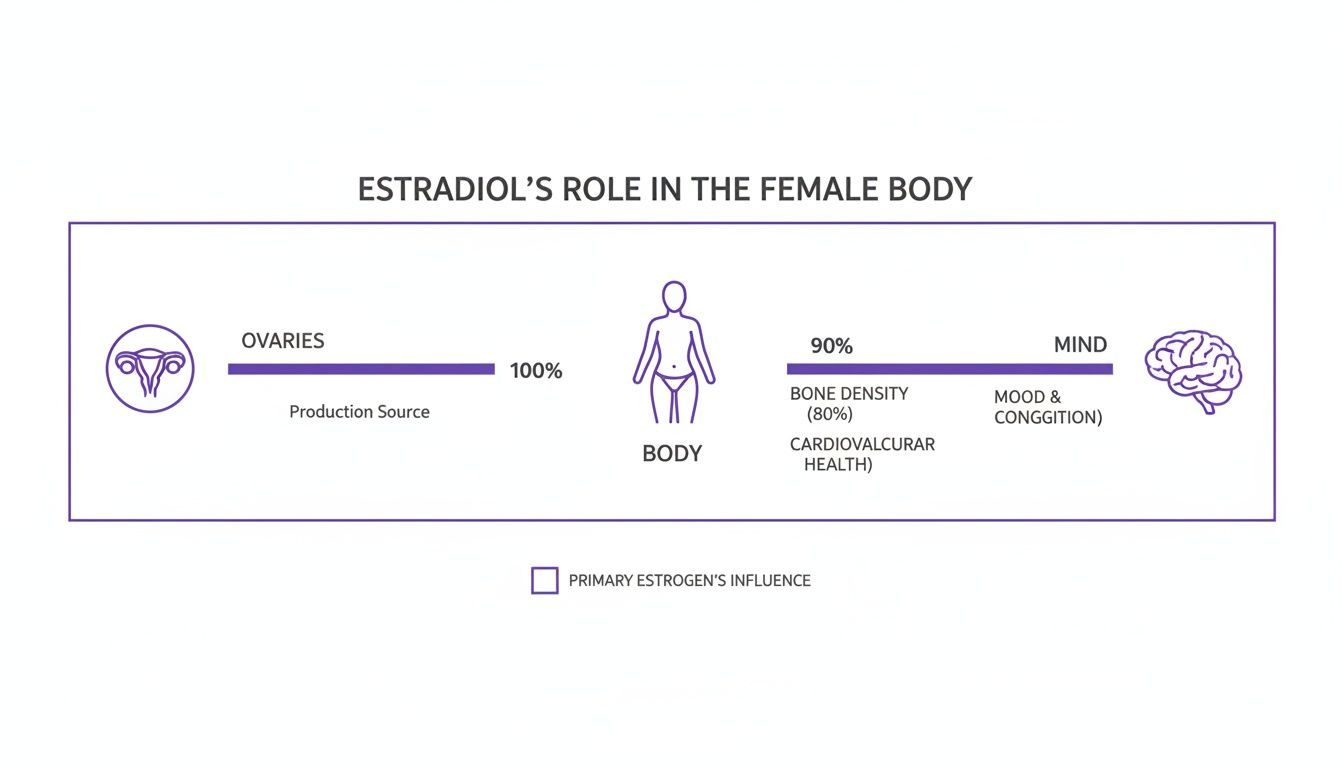
As you can see, estradiol's job isn't confined to your ovaries. It's a master coordinator, influencing everything from your mood and energy to your bone health, all in sync with your cycle.
The Luteal Phase: The Gradual Retreat
Once ovulation is over, the wave begins to recede. The follicle that released the egg transforms into a temporary structure called the corpus luteum. Its new job is to produce hormones, mainly a lot of progesterone but also a moderate amount of estradiol.
During this luteal phase, estradiol levels dip from their pre-ovulation high but stay elevated compared to the start of your cycle. If you don't become pregnant, the corpus luteum starts to break down toward the end of the phase. This makes both estradiol and progesterone levels plummet, which tells your body to shed its uterine lining and start a new period. The tide goes back out, and the whole process begins again.
The cyclical nature of estradiol production is why a single blood test may not capture the full picture. Understanding where you are in your cycle provides the crucial context needed to interpret your results correctly.
These dramatic fluctuations are the hallmark of a healthy, functioning reproductive cycle. For instance, normal estradiol levels can swing from under 50 pg/mL during your period all the way up to 400 pg/mL or more just before you ovulate. This huge variation is precisely why timing is everything when assessing your hormone health. As you can see from in-depth estradiol analysis on news-medical.net, knowing this pattern helps you have a much more meaningful conversation with your doctor about what your lab results truly mean for you.
How Perimenopause and Menopause Change Your Estradiol Levels
If your reproductive years were a fairly predictable hormonal rhythm, think of perimenopause as the time when the band starts playing off-beat. This transitional stage, which can last for years, is marked by hormonal chaos as your ovaries gradually wind down estrogen production. Getting a handle on this shift is the first step to making sense of the new and often confusing symptoms you might be experiencing.
I often use the analogy of a lightbulb that’s been shining brightly for decades. During perimenopause, that lightbulb doesn't just switch off. It flickers. One month, your estradiol might surge higher than it did in your 20s, causing symptoms like heavy periods and breast tenderness. The next, it could plummet, bringing on hot flashes, brain fog, and night sweats.
This erratic up-and-down swing is the defining characteristic of perimenopause. It’s exactly why you can feel on top of the world one week and completely depleted the next. Your body is still trying to ovulate, but the process is becoming less efficient, leading to these wild hormonal spikes and drops.
The Flicker of Perimenopause
During this time, the idea of a “normal” estradiol level becomes almost useless. A single blood test might show a result anywhere from below 30 pg/mL to over 400 pg/mL. That’s why I tell my clients that one lab result is just a snapshot of a moving target—it rarely captures the full story of what your body is going through.
This is where tracking your symptoms becomes so incredibly powerful. While a lab report might show a number that seems fine on paper, the pattern of your symptoms tells the real, day-to-day story.
The unpredictable nature of perimenopause validates your experience. The mood swings, sleep issues, and brain fog aren't "in your head"—they are direct physiological responses to the hormonal rollercoaster your body is riding.
As estradiol fluctuates, many women also notice changes in their metabolism and where they store fat. It becomes more important than ever to understand how to lose perimenopause belly fat by adapting your lifestyle to your body's new hormonal reality. For a more detailed look at this journey, our guide on the stages of perimenopause can offer more clarity.
The New Normal of Post-Menopause
Eventually, the flickering stops. Menopause is officially confirmed once you’ve gone 12 consecutive months without a period. At this point, you’re considered post-menopausal, and the hormonal chaos finally gives way to a new, steady state. Your ovaries have mostly stopped producing estradiol, and your levels settle into a new, consistently low baseline.
So, what are normal estradiol levels after menopause?
Typical Post-Menopausal Range: Most women’s levels will settle somewhere below 30 pg/mL, and often even under 10 pg/mL.
This new hormonal environment is stable, but it’s a world away from what your body was used to for decades. The loss of estradiol’s widespread protective effects is what solidifies many of the symptoms that first started flickering on and off during perimenopause.
Common experiences tied to low post-menopausal estradiol include:
Persistent Hot Flashes and Night Sweats: Without enough estradiol to help regulate the body's internal thermostat, these can continue for years.
Vaginal Dryness and Atrophy: Estradiol is vital for maintaining the health, lubrication, and elasticity of vaginal tissues.
Accelerated Bone Loss: The risk of osteoporosis climbs because estradiol plays a key role in slowing down bone breakdown.
Changes in Mood and Cognitive Function: Lingering brain fog or shifts in mood are common as the brain adjusts to a low-estrogen state.
While this might sound intimidating, the post-menopausal phase brings stability. The unpredictable ride is over. This new baseline allows you and your healthcare provider to create a clear, long-term strategy for managing symptoms and protecting your health. Understanding this entire journey—from predictable waves, to a chaotic flicker, and finally to a new, quiet shore—is what empowers you to navigate these changes with confidence.
Recognizing High and Low Estradiol Symptoms
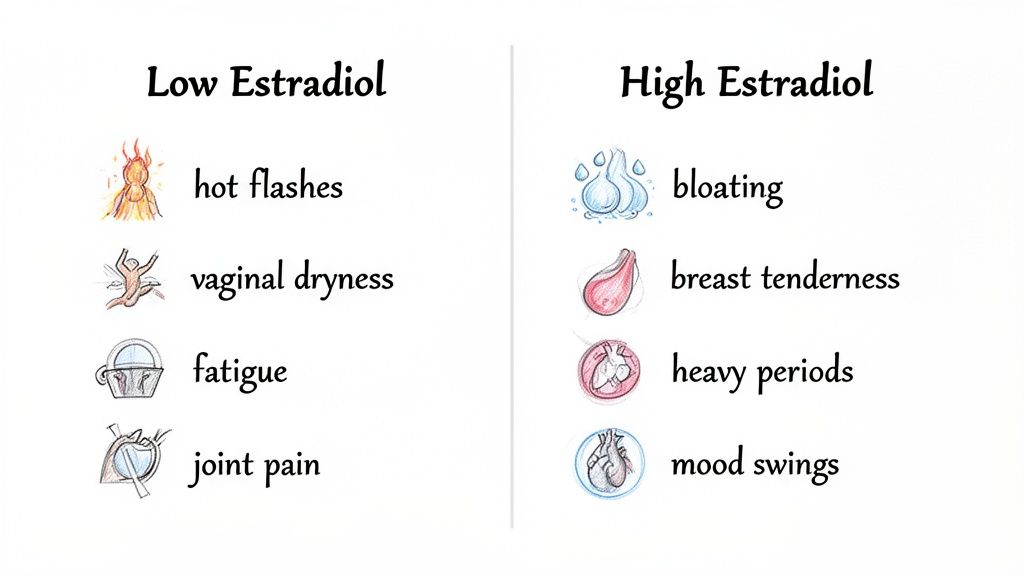
One of the most important things to understand about hormonal health is that your lab results are only half the story. A number on a report might tell you your estradiol is technically high or low, but it doesn't capture how you actually feel. Learning to connect those numbers to your body's own signals is key.
Think of it this way: your lab report is the map, but your symptoms are the real-time weather. You need both to truly understand where you are. When you start to recognize the classic signs of high and low estradiol, you can connect the dots between hormonal shifts and your daily experience—especially during the rollercoaster ride of perimenopause.
This isn't about diagnosing yourself. It's about becoming an expert in your own body and learning the language to talk about it. When you can walk into your doctor's office and clearly describe your symptoms, you're better equipped to have a productive conversation and figure out what "normal" really means for you.
Symptoms of Low Estradiol
When estradiol levels fall, it can feel like someone slowly turned down a dimmer switch on your body’s energy and vitality. This is the hormonal pattern we associate with menopause, but it can also happen at other points in your cycle or for different health reasons. The symptoms are often a direct result of losing estradiol's protective and supportive effects.
Common signs of low estradiol often include:
Hot Flashes and Night Sweats: This is the hallmark symptom of menopause. Estradiol helps manage your body's internal thermostat, and when it drops, the system goes haywire.
Vaginal Dryness and Discomfort: Estradiol keeps the tissues in the vagina plump, moist, and elastic. Without it, they can become thin and dry, leading to discomfort.
Fatigue and Low Energy: Estradiol plays a big role in your overall vitality. A significant dip can leave you feeling completely drained.
Joint Pain and Aches: This hormone has natural anti-inflammatory properties. As levels decline, you might find yourself feeling more achy and stiff.
Sleep Disturbances: Many women struggle with insomnia or wake up frequently, often drenched from night sweats.
Brain Fog or Trouble Concentrating: Because estradiol supports healthy brain function, low levels can leave you feeling mentally fuzzy and unfocused.
Many of these are also classic perimenopause symptoms. You can see the full picture by exploring the 34 symptoms of perimenopause and how they link back to your hormones.
Symptoms of High Estradiol
On the flip side, high estradiol can feel like your body is stuck in overdrive. This condition, sometimes called estrogen dominance, is incredibly common during the chaotic hormonal swings of perimenopause, when levels can spike to new highs before crashing. It can also be influenced by things like excess body fat, which actually produces its own estrogen.
Think of high estradiol as having too much of a good thing. While essential, an excess can overwhelm your system and create its own set of challenging symptoms.
Common signs of high estradiol may include:
Bloating and Water Retention: A classic sign is feeling puffy and swollen, especially around your abdomen.
Breast Tenderness or Swelling: Your breasts might feel sore, heavy, or even lumpy before your period.
Heavy or Irregular Periods: High estradiol can cause the uterine lining to build up excessively, which leads to much heavier bleeding.
Mood Swings, Irritability, and Anxiety: Just like low levels, high levels can throw off the delicate balance of your brain's mood-regulating chemicals.
Weight Gain: This is particularly true for weight that seems to stubbornly collect around the hips, thighs, and belly.
Looking at these two lists, you might start to see a pattern in your own body's behavior. Recognizing these symptoms is the first step toward understanding the hormonal story unfolding within you.
How to Navigate Testing and Your Hormone Health
Knowing your symptoms is one thing, but figuring out what to do next is how you truly start to feel in control again. If you've been feeling "off" and suspect your estradiol levels are on a rollercoaster—especially during perimenopause—it’s the perfect time to talk with your healthcare provider.
Think of it this way: a single blood test is just a snapshot in time. With hormones that fluctuate daily, that one picture can be misleading. What really matters is seeing the whole movie. The best way to do that is by tracking your own experiences over time.
Preparing for Your Doctor's Visit
Before you even step into the clinic, start keeping a simple log of your symptoms. This isn't just a list of complaints; it's crucial data that tells a story a single lab number never could. It helps your doctor see the bigger picture, especially when a test result falls into a vague "normal" range.
When you meet with your provider, be ready to discuss a few key things:
Your Symptom Patterns: Get specific. Don't just say you have hot flashes; explain that they wake you up at 3 a.m. every night. Mention if brain fog hits you hardest after lunch. This context is gold.
The Timing of Your Test: If you still get a period, ask when you should have your blood drawn. An estradiol test on day 3 of your cycle reveals something very different from one taken on day 14.
A Complete Hormone Panel: Estradiol doesn't work in a vacuum. Ask about testing other hormones like FSH (Follicle-Stimulating Hormone), which provides much-needed context for what's happening during perimenopause. You can learn more about which tests are useful in our guide on how to test for menopause.
Never forget that your symptoms are real, valid data. When you pair your lived experience with lab results, you get a far more accurate health profile that leads to truly effective decisions.
Building Your Action Plan
Once you and your provider have a better handle on your hormonal patterns, you can work together on a plan. This might start with lifestyle shifts, changes to your diet, or other targeted interventions. It's also a good time to become aware of all the options available, including treatments like Biote Hormone Therapy.
This is where you can connect the dots. Tools like the Lila app can help you see how your daily habits—from what you eat to how you sleep—directly impact your mood and energy. By tracking your symptoms and your lifestyle in one place, you're empowered to discover what truly works for your body.
Your Top Estradiol Questions, Answered
As you get to know your hormones, it's only natural to have a lot of questions. Even when you have a good handle on what normal estradiol levels are, you’ll likely wonder about the nitty-gritty of testing, symptoms, and what it all means for you. Let's tackle some of the most common questions we see.
Can I Test My Estradiol Levels at Home?
You absolutely can. There are plenty of at-home hormone tests out there that use a bit of saliva or a finger-prick blood sample. They’re certainly convenient for getting a quick snapshot of your hormonal landscape, but just be aware that their accuracy can be a bit variable. Following the kit instructions to the letter is key.
No matter what the home test says, the most crucial step is always to review the results with your doctor or a qualified healthcare provider. They are the only ones who can truly interpret what your numbers mean in the context of your health and, if needed, order a formal lab-drawn blood test to confirm things.
Why Did My Doctor Say My Estradiol Is "Normal" When I Feel Awful?
We hear this all the time, and it’s one of the most frustrating things to experience, especially if you're in perimenopause. The truth is, the "normal" ranges on lab reports are incredibly wide and don't necessarily reflect the optimal level for your individual body. Your result can fall squarely within that "normal" window but still be far too low for you to feel good.
What's more, estradiol is a moving target. Your levels can swing wildly from one day to the next. It’s entirely possible that you just happened to have your blood drawn on a "good day" when your levels were temporarily higher. This is exactly why a single test can be so misleading, and why tracking your symptoms over time gives a much more honest picture of what's really going on.
Do Birth Control Pills Mess With Estradiol Test Results?
Yes, they have a huge impact. The whole point of most hormonal birth control pills is to deliver synthetic hormones that suppress your body's own hormone production—including your natural estradiol.
If you get your estradiol tested while you're on the pill, the results will almost certainly come back as very low. This number doesn't reflect your body's true hormonal state; it just shows that the medication is doing its job. To get a real baseline of your natural normal estradiol levels, you’d need to have a conversation with your doctor about safely stopping the pill for a period of time before you test.
Ready to move beyond confusing symptoms and get clear, personalized guidance? Lila uses AI to analyze your daily check-ins and create a custom action plan to help you manage hot flashes, improve sleep, and stabilize your mood. Start your journey toward feeling like yourself again at getlila.com.
You should not have to do it all on your own









