Why Am I Having Hot Flashes? A Guide to Causes and Relief
Wondering 'why am I having hot flashes?' Explore common causes from perimenopause to stress, learn the signs, and discover effective relief strategies.

That sudden, overwhelming feeling of heat can be really jarring, making you stop in your tracks and wonder, "What on earth was that?" While the first thing that comes to mind is often the hormonal shifts of perimenopause, and for good reason, it's not the only possible cause. Hormones are the usual suspect, but medications, lifestyle habits, and even other health conditions can be behind these intense episodes.
Unpacking the Sudden Wave of Heat
A hot flash isn't just a feeling of being a little warm. It’s more like someone cranked up an internal furnace without any warning. One second you're perfectly comfortable, the next a wave of intense heat is creeping up your chest, neck, and face. You might look flushed, feel your heart beating faster, and break out in a sweat—only to be left with a shivery chill once it passes.
If this sounds familiar, you're in good company. Hot flashes are one of the most common signs of the menopause transition, impacting a staggering 75% of women across the globe. Just in the United States, roughly 6,000 women enter menopause every single day, and the vast majority will have to navigate this disruptive symptom. For many, it's far more than a simple nuisance; studies confirm that hot flashes can seriously get in the way of work, social activities, and your overall quality of life. You can learn more about the widespread impact of menopausal symptoms from recent research.
The Brains Behind the Blaze
So, what's actually going on inside your body to cause this? It all comes down to a tiny, powerful region in your brain called the hypothalamus. Think of it as your body's command center for temperature regulation, constantly making tiny adjustments to keep everything stable and balanced.
As you head into perimenopause, your estrogen levels start to fluctuate wildly and eventually decline. This hormonal chaos sends mixed signals to your hypothalamus, making it hyper-sensitive to even the slightest changes in your core body temperature.
Your hypothalamus gets a false signal that you're overheating. It immediately kicks into emergency cool-down mode: your blood vessels widen to release heat (causing the flush), and your sweat glands start working overtime.
It's a massive overreaction to a very minor stimulus. Imagine your home thermostat was malfunctioning, blasting the AC on high every time the temperature went up by a single degree. That’s essentially what your brain is doing.
More Than Just a Feeling
Getting a handle on this biological process is the first step toward finding some real relief. While the sensation is physical, the trigger is a complex dance between your hormones and your brain. Knowing what’s happening can help replace confusion with clarity. The most common triggers usually fall into one of these categories:
Hormonal Changes: This is by far the most common reason, especially for women over 40.
Lifestyle Factors: Things like stress, what you eat (spicy foods, caffeine), and alcohol can all be potent triggers for a hot flash.
Medical Conditions: Though less frequent, thyroid problems or certain medications can produce very similar symptoms.
By digging into these potential causes, you can start to pinpoint what your personal triggers are and begin putting together a plan to manage them.
1. Perimenopause and Menopause: The Primary Cause
If you’re over 40 and suddenly find yourself asking, “why am I having hot flashes?” the most likely answer is perimenopause. This is the multi-year runway leading up to menopause, and it’s all about one thing: hormonal flux.
Imagine your hormone levels have been like a calm, steady river for most of your adult life. During perimenopause, that river turns into unpredictable rapids.
This hormonal rollercoaster directly messes with your body's internal thermostat, a part of your brain called the hypothalamus. As estrogen levels bounce around, your hypothalamus gets confused, thinking your body is overheating when it isn't. It then triggers an emergency cool-down—the hot flash.
Understanding this makes a world of difference. It means those sudden, intense waves of heat aren't random. They're a direct, and completely normal, biological response to a predictable (if chaotic) process your body is navigating.
This handy decision tree shows how most paths lead back to the hormonal shifts of perimenopause and menopause.
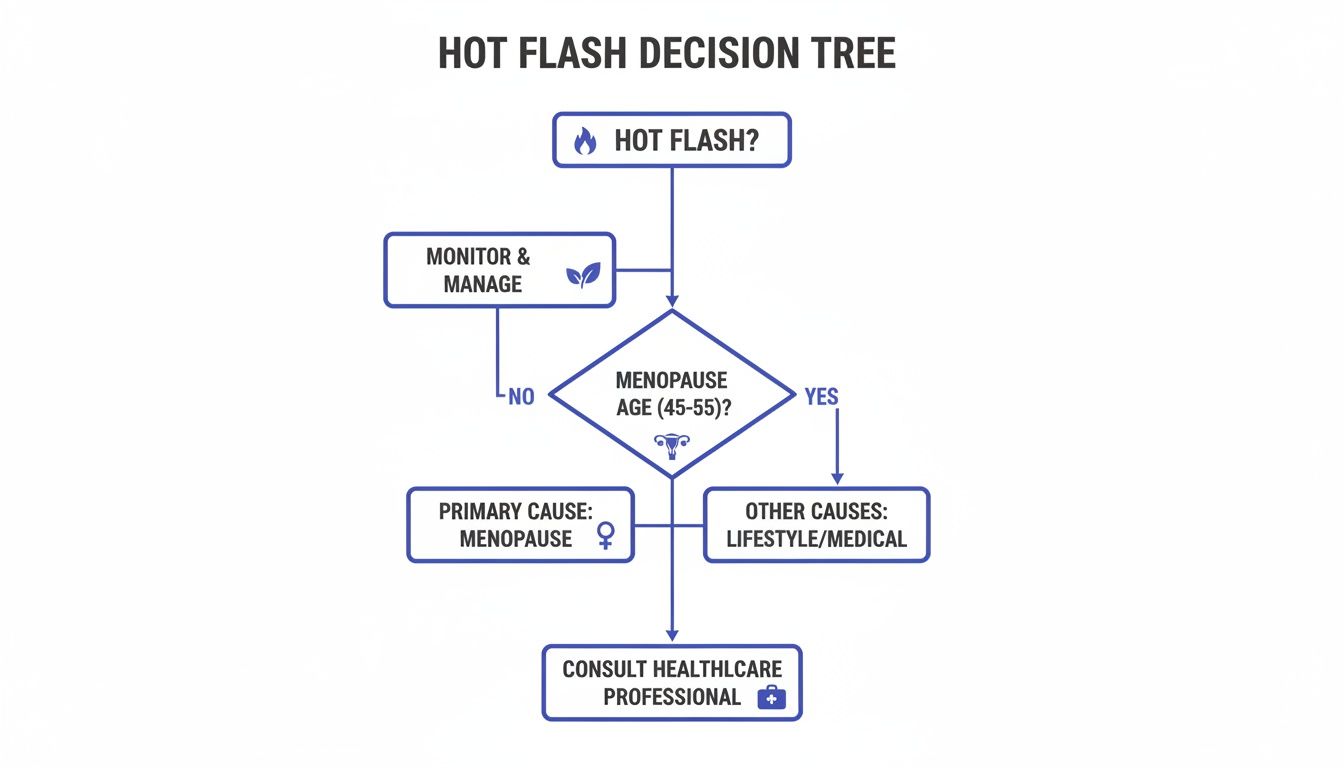
As you can see, while other factors can play a role, the main driver for most women is this natural life transition.
The Symphony of Symptoms
Hot flashes rarely show up alone. They're usually the headliner in a whole cluster of changes that signal perimenopause is underway. When you start noticing these other signs, it helps connect the dots.
This happens because estrogen does more than just regulate your temperature; it has a hand in everything from your mood and memory to your sleep cycle. As its levels become erratic, so does the stability of all those systems.
You might start noticing these classic signs right alongside the heat:
Night Sweats: These are just hot flashes that crash the party while you're sleeping. They can drench your sheets and wreck your rest, leaving you drained the next day.
Irregular Periods: Your once-predictable cycle might go haywire. Periods can become shorter, longer, heavier, or lighter—it's one of the earliest and most reliable clues.
Sleep Problems: Even if you're not having night sweats, you may find it harder to fall asleep or stay asleep.
Mood Swings: Feeling more irritable, anxious, or just plain down? Shifting hormones can have a real impact on your brain chemistry and emotional state.
Brain Fog: Many women describe feeling less sharp, having trouble with focus, or struggling to find the right word.
Think of your body as an orchestra and estrogen as the conductor. When the conductor starts giving erratic signals, the different sections—sleep, mood, temperature—fall out of sync. The result is a chaotic, dissonant experience.
If this sounds familiar, you are far from alone. Around the world, over a billion women are going through some stage of this transition. By 2030, nearly 500 million women will be between the ages of 45-55. And in the U.S. alone, a staggering 85% of postmenopausal women have dealt with symptoms, with hot flashes being one of the top reasons they seek medical advice.
Perimenopause vs Other Causes: A Symptom Checker
It's easy to assume every hot flash is hormonal, but it’s smart to consider the bigger picture. This table helps you spot the difference between hot flashes caused by perimenopause and those from other potential issues by comparing the company they keep.
Symptom | Common in Perimenopause/Menopause | Potential Other Cause (Thyroid, Anxiety, etc.) |
|---|---|---|
Irregular Periods | Yes, this is a hallmark sign. | Unlikely, unless another condition is also present. |
Night Sweats | Very common. | Can be caused by infections, some cancers, or medications. |
Unexplained Weight Changes | Gradual weight gain, especially around the middle, is common. | Sudden weight loss or gain could signal a thyroid issue. |
Heart Palpitations | Can occur with hot flashes. | Can also be a primary symptom of anxiety or hyperthyroidism. |
Sleep Disruption | Extremely common, often tied to night sweats. | Also common with anxiety, but the pattern may differ. |
Mood Swings | Yes, often linked to the menstrual cycle. | Persistent anxiety or depression may have other root causes. |
Brain Fog | Frequent complaint during this transition. | Can be a symptom of thyroid dysfunction or chronic stress. |
Vaginal Dryness | A classic sign of declining estrogen. | Not typically associated with other causes of hot flashes. |
While this table is a helpful guide, it’s not a diagnostic tool. If your symptoms feel out of step with the typical perimenopause pattern or are severe, it's always best to get a professional opinion.
From Chaos to Clarity
By seeing these symptoms as an interconnected web, you can start to find patterns in the chaos. You might realize your hot flashes are worse the week before your period, or that a night of bad sleep makes you feel extra moody the next day. This is where tracking your symptoms becomes a game-changer.
Tools like the Lila app help you map these experiences, turning frustrating moments into useful data. Documenting when your hot flashes hit, how long they last, and what other symptoms pop up at the same time gives you a powerful tool. It not only confirms you're on a normal path but gives you clear, valuable insights to discuss with your doctor.
To get a handle on all the potential changes, our comprehensive guide to the 34 menopause symptoms is a great place to start. And if you’re curious about non-medical approaches, there are many effective natural remedies for perimenopause symptoms worth exploring.
When It’s Not Menopause: Other Medical Causes
While hormonal changes are the number one reason for hot flashes in women over 40, they certainly aren't the only cause. If you're wondering, "why am I having hot flashes?" but aren't noticing other classic signs of perimenopause, it’s smart to look at other medical possibilities.
Think of a hot flash as your body’s check-engine light. Most of the time, it's signaling the normal, expected transition of perimenopause. But every so often, it's flagging a completely different issue that needs a look under the hood.
When Your Thyroid Is the Culprit
One of the most frequent non-menopausal culprits behind hot flashes is an overactive thyroid, a condition called hyperthyroidism. Your thyroid gland is basically the thermostat for your metabolism, controlling how your body burns energy. When it starts pumping out too much thyroid hormone, it sends your metabolism into overdrive.
This metabolic surge generates a ton of internal heat. Your body is essentially running hot all the time, making you feel warm and sweaty far more often than you should. The hot flashes from hyperthyroidism can feel almost identical to menopausal ones, but they usually bring a few other distinct clues with them.
Unexplained Weight Loss: You might find yourself losing weight even though your appetite is the same or even bigger than usual.
Rapid or Irregular Heartbeat: A constantly racing heart, or palpitations, are classic signs that your thyroid is working too hard.
Increased Anxiety or Nervousness: Feeling jittery, irritable, or like you just can't relax is another key indicator.
Hand Tremors: You might notice a fine, subtle shaking in your hands.
If you’re having hot flashes alongside a pounding heart, it’s a connection worth exploring. You can learn more about how to stop hormonal heart palpitations in our detailed guide, as the sensations can sometimes overlap.
Medications That Can Turn Up the Heat
It might surprise you, but certain prescription medications can mess with your body's internal thermostat and trigger hot flashes as a side effect. This isn't an allergic reaction; it's a direct impact on the part of your brain that manages heat—the hypothalamus.
Some of the most common drug categories that list hot flashes on the label include:
Antidepressants: Especially selective serotonin reuptake inhibitors (SSRIs), which can influence brain chemistry that controls body temperature.
Blood Pressure Medications: Certain types can affect how your blood vessels expand and contract, leading to flushing.
Osteoporosis Drugs: Medications like raloxifene are known for causing hot flashes.
Cancer Treatments: Some chemotherapies and hormone therapies, such as tamoxifen for breast cancer, are very well-known triggers.
If your hot flashes started right around the time you began a new medication, that's a clue worth bringing up with your doctor. Just remember to never stop taking a prescribed medication on your own.
Other Potential Medical Triggers
Beyond your thyroid and medications, a few other health conditions can produce symptoms that mimic menopausal hot flashes. They're less common, but it's important to rule them out, especially if your symptoms feel severe or come with other worrying signs.
A hot flash is your body’s fire alarm. Most of the time, it’s just hormonal smoke from the perimenopause transition. But occasionally, it’s warning you of a different kind of fire that needs to be checked out.
These other potential causes include:
Infections: Some infections, like tuberculosis or HIV, can cause night sweats and feverish feelings that are easily mistaken for hot flashes. The key difference here is that infections usually bring an actual fever along for the ride.
Anxiety and Panic Attacks: That sudden flood of adrenaline during a panic attack can absolutely cause flushing, sweating, and an intense wave of heat. These episodes, however, are typically tied to feelings of intense fear, not just a random event.
Neurological Conditions: This is rare, but damage to the hypothalamus from things like surgery or tumors can disrupt the body's temperature regulation.
If your hot flashes are paired with a persistent fever, significant weight loss, or other unusual symptoms, getting a medical check-up is the single most important step you can take. Your doctor can help you dig into the root cause and make sure you get the right care.
How Your Lifestyle Can Fuel the Fire
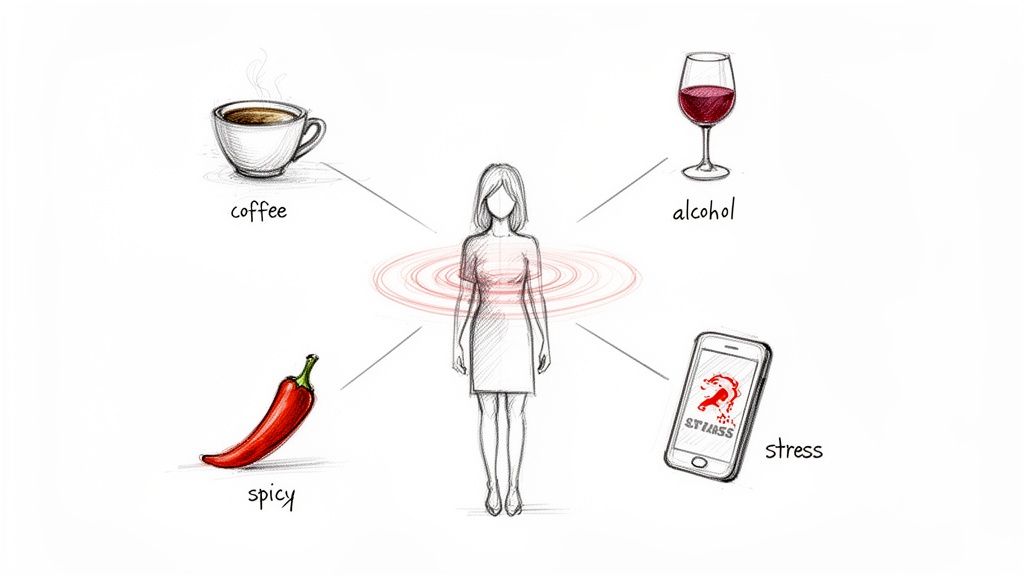
Beyond the big-picture medical causes, what you do every day can feel like throwing kindling on the fire of a hot flash. While your diet or stress levels aren't causing the underlying hormonal chaos, they can absolutely provoke the symptoms that come with it.
Think of your nervous system as being on a hair-trigger during the menopause transition. Certain foods, drinks, or even a tense meeting can nudge it over the edge, setting off that faulty internal thermostat. It’s a bit like having an overly sensitive smoke alarm—sometimes, just making toast is enough to get it screaming.
But this is actually good news. It means you have more control than you might think. By figuring out what your personal triggers are, you can make small, targeted changes that bring real relief without having to completely upend your life.
Common Dietary Triggers
What you eat and drink can have a surprisingly powerful effect on how often—and how intensely—you feel that heat rise. Many of our favorite things can either widen blood vessels or stimulate the central nervous system, which are both invitations for a hot flash to crash the party.
Keep an eye on these common culprits:
Caffeine: That essential morning coffee or afternoon pick-me-up gives you a jolt by revving up your nervous system. For a body that's already on high alert, this stimulation can easily be the final push into a hot flash.
Alcohol: A glass of wine might seem like a great way to unwind, but alcohol is a vasodilator. That means it widens your blood vessels, bringing more blood to the surface of your skin and creating a feeling of warmth that can quickly escalate.
Spicy Foods: The active compound in chili peppers, capsaicin, literally tricks your brain into thinking your body is overheating. Your body, ever helpful, then kicks its cooling mechanisms into gear—hello, flushing and sweating.
Sugary Foods: A sugar-heavy snack can send your blood sugar on a rollercoaster ride, spiking and then crashing. This instability puts a strain on your system and can easily act as another trigger.
Finding your dietary triggers isn't about deprivation. It’s about detective work. When you track what you consume and how you feel, you start to see patterns and learn your personal limits, empowering you to make choices that work for you.
The Powerful Link Between Stress and Heat
Ever feel your face flush when you're anxious or under a tight deadline? That's not in your head. Stress is one of the most potent non-hormonal triggers for hot flashes. This can create a vicious cycle: stress causes a hot flash, which then makes you feel even more stressed out.
When you’re stressed, your body goes into "fight or flight" mode, releasing hormones like adrenaline and cortisol. This biological alarm system is designed for survival, but it has some very physical side effects.
This response directly paves the way for a hot flash in a few key ways:
Increased Heart Rate: Your heart pounds faster to get blood to your muscles.
Blood Vessel Dilation: Your blood vessels expand to improve circulation, which you feel as a wave of heat.
Metabolic Spike: Your body starts burning energy more quickly, generating more internal warmth.
For a nervous system already made sensitive by hormone fluctuations, this adrenaline rush is often all it takes to trip the wire on your brain’s malfunctioning cooling response. Learning to manage your stress—whether it’s through a few deep breaths, a quick walk, or mindfulness—can be just as effective as avoiding trigger foods. It calms everything down, making your body far less likely to overreact and hit the panic button.
How to Manage Hot Flashes and Get Your Life Back
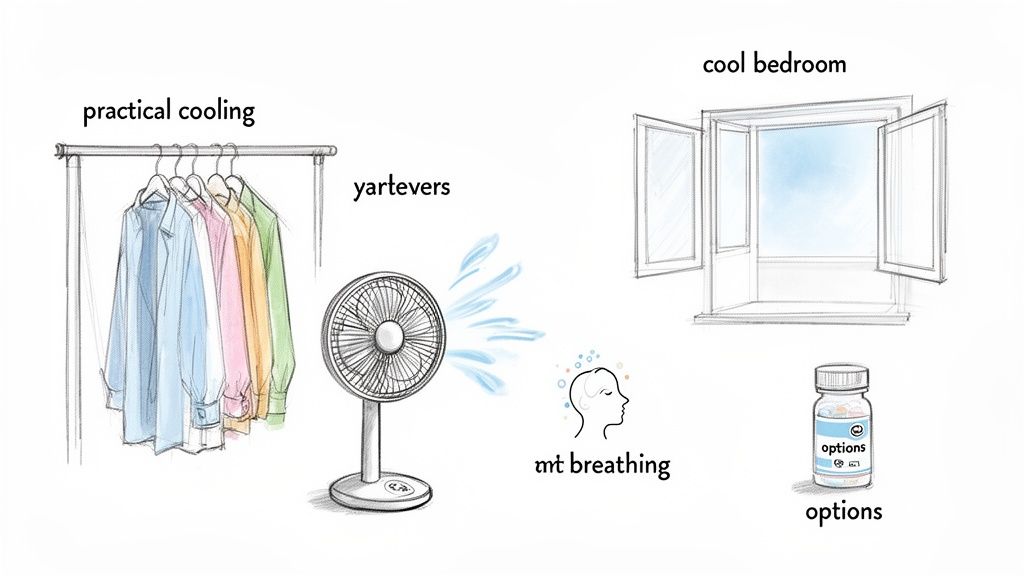
Knowing what’s causing your hot flashes is one thing, but figuring out what to do about them is what really matters. Thankfully, you have a powerful toolkit at your disposal, blending medical treatments with practical, everyday lifestyle changes to help you cool the burn and feel more like yourself again.
Some of these strategies are FDA-approved therapies that tackle the hormonal root of the problem, while others are simple habits you can start building today. The most effective approach is almost always a personal one, tailored to your specific symptoms and health needs.
Evidence-Based Medical Treatments
When hot flashes are more than just an annoyance and start getting in the way of your life, it might be time to consider medical options. This is a conversation to have with your doctor, who can help you weigh the pros and cons based on your unique health history.
The gold standard for treating menopausal hot flashes is Hormone Therapy (HT), sometimes called hormone replacement therapy (HRT). It works by topping up the estrogen your body isn't making anymore, which helps stabilize that haywire internal thermostat.
It might feel like you’re the only one, but these hormonal shifts are incredibly common. 17.1% of perimenopausal women deal with moderate to severe symptoms, and that number climbs to 28.5% in postmenopausal women under 55. For those who are good candidates, hormone therapy can be a game-changer, cutting these episodes by as much as 80%. It’s not for everyone, though, especially if you have a history of certain cancers, blood clots, or heart issues.
If HT isn't a good fit, don't worry—there are excellent non-hormonal options, too:
Low-Dose Antidepressants: Certain SSRIs and SNRIs can help by influencing the brain chemicals that regulate body temperature, effectively turning down the heat.
Gabapentin: Originally a seizure medication, it has proven quite effective at cooling hot flashes for many women.
Fezolinetant: This is a newer non-hormonal drug that targets a specific pathway in the brain responsible for temperature control.
The best first step is always talking to your doctor. They can walk you through all the options—from pills and patches to creams—to find the right fit for your body and your life.
Smart Lifestyle and Self-Care Habits
Medical treatments are powerful, but don't underestimate the impact of small, consistent changes to your daily routine. These practical strategies put you in the driver's seat, helping you manage triggers and feel more prepared when a hot flash hits.
Think of it as creating a personal cooling system. The goal is to keep from overheating in the first place and to have a plan for when you feel that familiar wave of heat.
Dress and Sleep for Comfort
Your environment is your first line of defense, especially at night when hot flashes can completely sabotage your sleep.
Layer Up: Dress in light, breathable fabrics like cotton or linen. Layers are your best friend—you can easily peel one off when you feel yourself getting warm. Steer clear of tight, synthetic clothes that trap heat.
Cool Your Sleep Space: A cool bedroom is non-negotiable. Use a fan, open a window, or turn on the A/C. A lower room temperature can make a huge difference in how often and how intensely night sweats strike.
Rethink Your Bedding: If you're waking up drenched, your sheets could be part of the problem. It’s worth looking into the best sheets for hot sleepers to create a cooler, more comfortable bed.
Mindful Eating and Drinking
What you put into your body can directly affect your internal thermostat. Pinpointing your dietary triggers is a huge step toward relief.
Watch for Triggers: Pay attention to how you feel after consuming common culprits like caffeine, alcohol, and spicy foods. Many women find that cutting back makes a noticeable difference.
Hydrate, Hydrate, Hydrate: Sip cool water all day long. When you're well-hydrated, your body is simply better at regulating its own temperature.
Embrace Plant-Based Foods: Some research suggests that diets rich in plant estrogens, like those found in soy, may help ease symptoms. For more ideas, check out our guide on 9 foods that fight hot flashes.
Calm Your Nervous System
Stress is a massive trigger for hot flashes, so anything you can do to soothe your nervous system is a win.
Breathe Through It: When you feel a hot flash coming on, try to take slow, deep breaths. Inhale through your nose, exhale through your mouth. This simple practice can help short-circuit the "fight or flight" response that makes things worse.
Move Your Body: You don't have to run a marathon. Regular, gentle movement like walking, swimming, or yoga helps regulate hormones, slash stress, and improve sleep—all of which lead to fewer, less intense hot flashes.
Your Top Questions About Hot Flashes, Answered
Even after getting the facts straight on what causes hot flashes, it's completely normal to have more questions pop up. Let's tackle some of the most common ones head-on, giving you direct, clear answers to help you feel more in control of your health journey.
How Long Do Hot Flashes Typically Last?
This is probably the number one question on everyone's mind. The honest truth? There's no single, predictable timeline. It's incredibly different for every woman.
A single hot flash itself is usually over pretty quickly, lasting anywhere from a fleeting 30 seconds to about five minutes. But the bigger picture—the total time you'll experience them—is a much longer story. On average, most women deal with hot flashes for around 7 to 10 years. They often start during perimenopause and then slowly taper off in frequency and intensity a few years after your last period.
Of course, some women are through this phase much faster, while for a small group, hot flashes can linger for more than a decade. The best way to get a handle on your own experience is to track what's happening. It’s the only way to see your personal patterns and figure out if what you're doing to manage them is actually working.
Can Men Get Hot Flashes, Too?
Believe it or not, yes, men can get hot flashes. It's far less common, though, and it's definitely not a normal part of aging for them. When it does happen, it's almost always because of a sudden, significant drop in testosterone levels.
The most common trigger is androgen deprivation therapy, a treatment for prostate cancer designed to suppress testosterone. The process is surprisingly similar to menopause in women. That abrupt hormonal shift throws the brain's internal thermostat (the hypothalamus) into chaos, triggering the exact same feelings of intense heat, flushed skin, and sweating.
A hot flash in a man is a clear medical signal. Unlike in women, where it's a natural transition, for men it points directly to an underlying hormonal issue, most often related to medical treatment.
If a man starts having hot flashes, it’s a sign he needs to see his doctor to pinpoint the cause, as it isn’t a standard physiological event.
Are Hot Flashes a Sign of Something Serious?
For the vast majority of women in their 40s and 50s, hot flashes are simply a normal, expected part of the menopausal transition. They're your body's response to fluctuating estrogen and aren't a sign of a dangerous disease.
That said, it’s smart to think of them as an important health indicator. Some research suggests that very frequent or severe hot flashes, especially if they begin early in perimenopause, might be linked to a higher risk of cardiovascular problems down the road. This doesn't mean hot flashes cause heart disease, but they can be a valuable clue about your overall vascular health.
You should always talk to your doctor if your hot flashes come with other unusual symptoms.
A Racing or Pounding Heart: While a faster pulse is common during a hot flash, persistent palpitations could point to a thyroid issue.
Unexplained Weight Loss: This is a classic red flag for conditions like an overactive thyroid.
Fever: A true fever, with an elevated body temperature, is not a hot flash. It signals an infection or another illness.
Think of hot flashes as a message from your body that's worth listening to. While they’re usually nothing to worry about, discussing their frequency and intensity with your doctor helps paint a fuller picture of your health.
What Is the Difference Between a Hot Flash and a Night Sweat?
This is a really common point of confusion, but the answer couldn't be simpler. A night sweat is just a hot flash that happens while you're sleeping. That's it.
The physical experience is identical—that sudden wave of heat, the flushed skin, the profuse sweating. The only real difference is the timing and, more importantly, the fallout. Because they strike while you’re asleep, night sweats can be incredibly disruptive.
They frequently lead to:
Serious Sleep Disruption: Waking up drenched in sweat, sometimes several times a night, makes deep, restorative sleep feel impossible.
Daytime Fatigue: Poor sleep inevitably leads to feeling exhausted, foggy, and completely drained the next day.
Increased Brain Fog and Irritability: When you're sleep-deprived, your mood, focus, and ability to think clearly can take a major hit.
Getting a handle on night sweats isn't just about being more comfortable at night. It's about protecting your energy, mood, and overall well-being during the day. Managing them effectively can create a massive positive ripple effect across your entire quality of life.
Navigating perimenopause can feel overwhelming, but you don't have to do it alone. Lila is an AI-powered app that turns confusion into clarity. With quick daily check-ins, Lila creates a personalized action plan to help you manage symptoms like hot flashes, sleep issues, and mood changes. Track your progress, chat with your 24/7 AI coach, and start feeling like yourself again. Join over 35,000 women who are taking control of their health journey at https://getlila.com.
Get Lila, your personal coach for perimenopause.
Built for women in their 40s. 24/7 coaching, in your pocket.


