How to Sleep Better During Perimenopause: A 2026 Guide
Tired of restless nights? Learn how to sleep better during perimenopause with evidence-based steps for managing hot flashes, anxiety, and hormonal changes.

Sleep used to be automatic. Then one night you wake at 3:07 a.m., hot and suddenly wide awake. Your sheets feel wrong. Your mind starts scanning everything at once. Did I forget something? Why am I awake again? Why am I so tired and unable to sleep?
That pattern is so common in perimenopause that I treat it as a health signal, not a personal failure. Many women blame stress, bad habits, or age. Those factors matter, but they are not the whole story.
Sleep disruption in this stage is widespread. Sleep disturbances affect 40 to 60% of women during perimenopause, and perimenopausal women have 1.6 times greater odds of sleep disturbance than premenopausal women, with around 42% meeting clinical criteria for insomnia (Chronobiology in Medicine). If other changes are showing up too, this guide to the 34 symptoms of perimenopause can help connect the dots.
Better sleep usually does not come from one miracle fix. It comes from matching the right intervention to the reason your sleep is breaking down. Temperature swings need a different response than hormone-linked anxiety. A racing mind needs a different plan than early waking.
That is good news, because once you identify your pattern, you can act on it tonight.
Introduction Waking Up to Perimenopause
A common perimenopause night looks like this. You fall asleep tired enough. Then you wake in the dark, either overheated, uneasy, or sharply alert for no obvious reason. You try to force sleep. It gets worse.
This is often the moment women start doubting themselves. Maybe I drank coffee too late. Maybe I am just stressed. Maybe this is how sleep is now.
It is not “just in your head,” and it is not a character issue. Perimenopause changes the body systems that support stable, restorative sleep.
What this disruption feels like
Some women struggle to fall asleep because their body feels keyed up at bedtime. Others fall asleep quickly but wake at 2 or 3 a.m. and cannot settle again. Some are jolted awake by heat. Others are not sweaty at all, but their sleep becomes lighter and more fragile.
Those differences matter. They point to different drivers.
If you keep waking and thinking, “I’m doing everything right, so why is this happening,” the missing piece is often hormonal timing, not effort.
Why hope is realistic
When sleep changes during perimenopause, I encourage women to stop chasing random internet tips and start treating sleep like a pattern to decode. The goal is not perfection. The goal is to identify what is waking you, what is keeping you awake, and what helps your body settle again.
That usually means working on three fronts:
Body: temperature, hormones, meal timing, movement
Mind: anxious thoughts, frustration, conditioned wakefulness
Environment: light, bedding, room setup, screens, sound
Once those pieces line up, sleep tends to become less chaotic and more predictable.
Why Perimenopause Hijacks Your Sleep
The fastest way to feel less helpless is to understand what your hormones are doing at night. Perimenopause sleep problems are not random. They are biological.
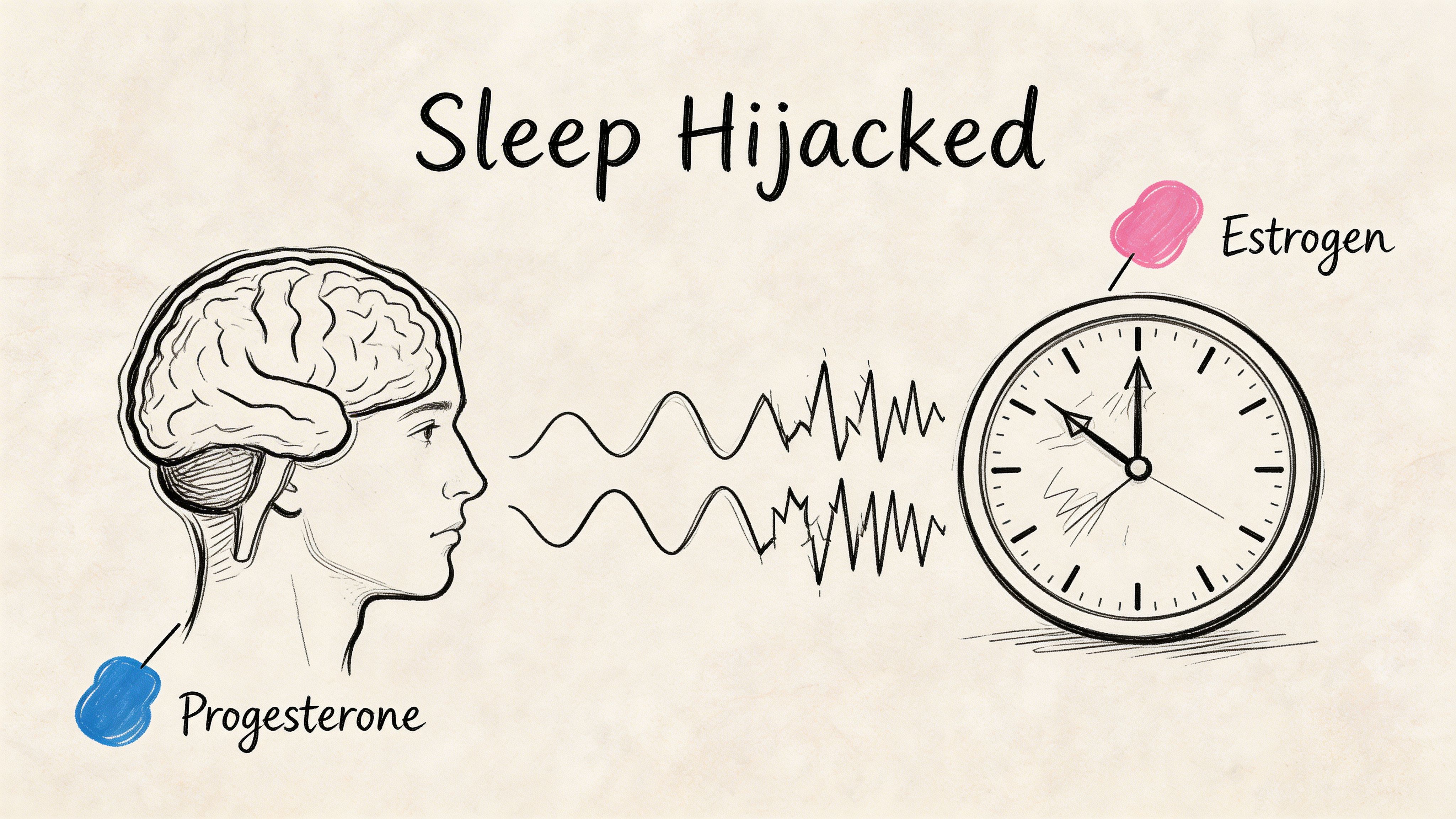
Progesterone loss changes how calm your body feels
Progesterone has a natural sedative effect. As it declines during perimenopause, many women notice it becomes harder to fall asleep and easier to wake up during the night (Stanford Lifestyle Medicine).
This is the part that generic sleep advice often misses. If your old routine used to work and now does not, declining progesterone may be one reason your nervous system no longer drops into sleep so easily.
Lower progesterone often shows up as:
Longer sleep onset: you feel tired but not sleepy
Lighter sleep: small disturbances wake you
More overnight awakenings: especially if your mind turns on fast
More anxiety sensitivity: bedtime becomes mentally loud
If you want context for the hormonal side, normal estradiol levels are worth understanding because estrogen and progesterone shifts tend to affect sleep together.
Estrogen affects temperature and timing
Falling estrogen has a different but equally disruptive effect. It destabilizes thermoregulation, which is why night sweats and hot flashes can shatter sleep. The same Stanford review notes that lower estrogen can also decrease melatonin production, which makes sleep timing less steady and sleep feel less anchored.
That matters because poor sleep in perimenopause is not always about one dramatic symptom. Sometimes it is a chain reaction:
Hormonal change | Common sleep effect |
|---|---|
Declining progesterone | Harder to fall asleep, lighter sleep, more awakenings |
Declining estrogen | Night sweats, hot flashes, fragmented sleep |
Reduced melatonin support | Sleep timing feels less stable |
Why “I’m just getting older” is the wrong conclusion
Age can affect sleep. But perimenopause creates a distinct pattern. Hormone fluctuations alter thermoregulation, circadian rhythm, and sleep architecture. That is why a woman who used to sleep well can suddenly feel like her nights changed without warning.
You are not failing at sleep. Your body needs a more targeted sleep strategy than it did five years ago.
Build Your Unshakable Sleep Routine
You do not need a complicated ritual. You need a routine that lowers friction between “awake” and “asleep.” A good evening routine is boring in the best possible way. It teaches your body what happens next.
Reset the room first
Before you work on supplements, meditations, or mindset, fix the environment. A sleep routine fails quickly if your room is bright, stuffy, noisy, or physically irritating.
Start with the basics:
Make the room dark: blackout curtains or a sleep mask help reduce unnecessary wake-ups.
Reduce heat buildup: breathable sheets and sleepwear matter more in perimenopause than many women realize.
Choose one sound strategy: a fan, white noise, or a quiet room. Constant sound is usually better than unpredictable sound.
Keep the bedroom visually calm: laundry piles, work materials, and bright device lights keep many brains in “task mode.”
If you want a useful primer on bedroom setup and foundational sleep habits, this guide on how to improve sleep quality naturally is a solid companion resource.
Create a power-down hour
Many women do not need a perfect 60-minute bedtime routine. They need a clear off-ramp from stimulation.
A practical power-down hour looks like this:
Stop activating input Turn off work, doom-scrolling, heated texts, and anything that spikes emotion.
Lower physical intensity Switch from bright overhead light to lamps. Change into breathable sleepwear. Let your body register that the active part of the day is ending.
Use one calming anchor Stretching, reading fiction, light journaling, or a short guided practice all work. If movement helps you unwind, gentle yoga for perimenopause can be a useful evening bridge.
Keep bedtime consistent Your nervous system likes rhythm. Going to bed at wildly different times makes a fragile sleep pattern harder to stabilize.
A strong routine does not have to feel elaborate. It only has to feel repeatable.
What usually does not work
Women often put effort into the wrong places. These are common traps:
Saving rest for the weekend: sleeping in late can make the next night harder.
Using wine as a sedative: it may make you drowsy, but it often leads to choppier sleep later.
Staying in bed while frustrated: that can train your brain to associate the bed with wakefulness.
Changing everything at once: if you cannot tell what helps, you cannot build a reliable plan.
A simple nightly checklist
Use this if you want a quick reset tonight.
Evening habit | Keep it simple |
|---|---|
Light | Dim lights before bed |
Screens | Reduce stimulating content |
Bedroom | Cool, dark, breathable |
Mind | One calming practice only |
Timing | Similar bedtime most nights |
Routine is not glamorous. It is effective.
Conquer Night Sweats and Hot Flashes
For many women, temperature management is not a nice extra. It is the center of the sleep plan. If your body keeps overheating at night, no amount of positive thinking will make you stay asleep.
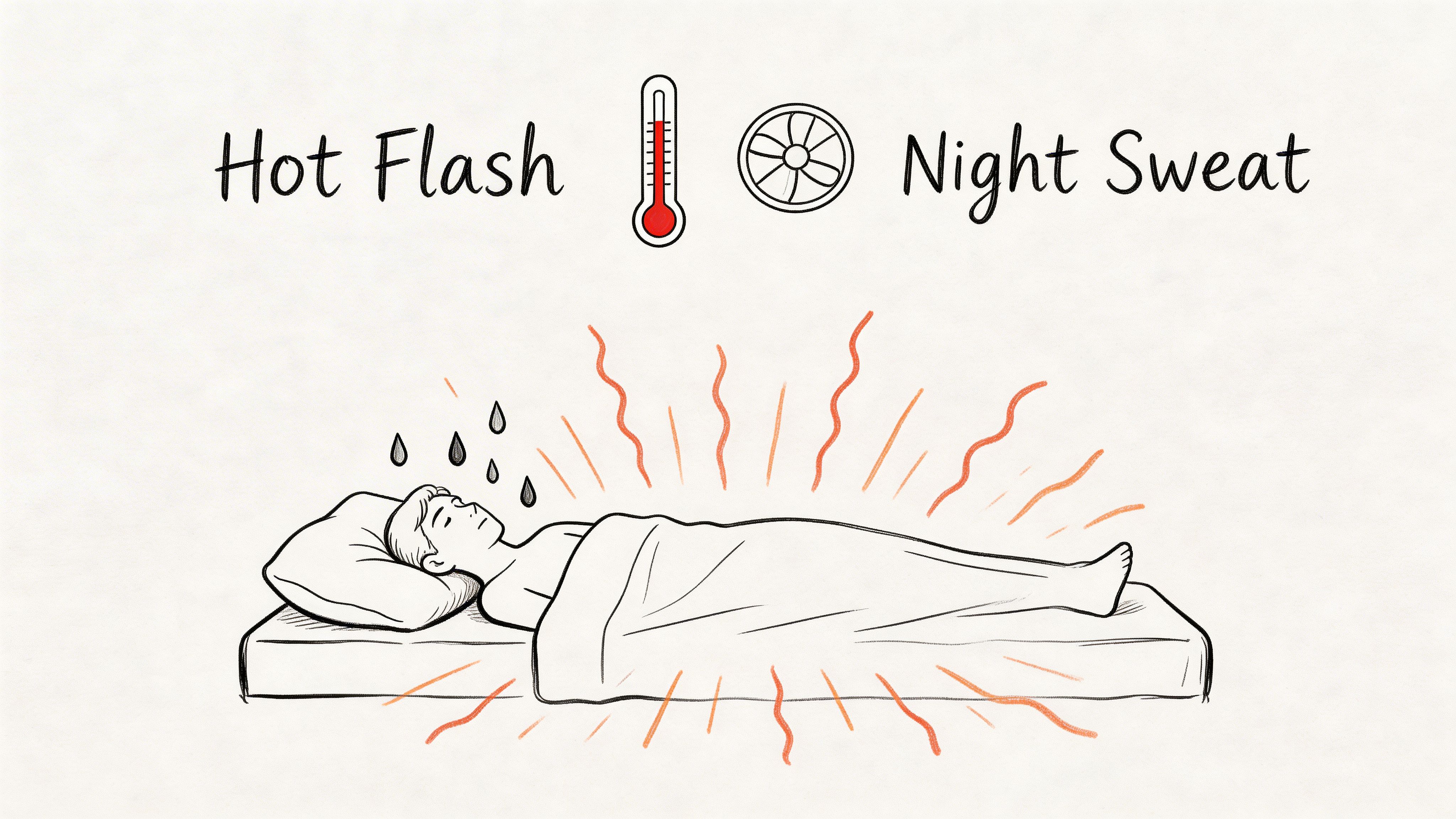
Build a layered cooling system
One cooling trick is rarely enough. Think in layers so one hot flash does not ruin the whole night.
Try this combination:
Breathable sleepwear: cotton, bamboo, linen, or silk tend to feel better than heavy synthetic fabrics.
Breathable bedding: choose sheets and blankets you can peel off quickly without fully waking up.
Air movement: a bedside fan or ceiling fan can help your body cool faster after a heat surge.
Cooling sleep surface: if your mattress traps heat, the problem may be underneath you. This overview of a cooling mattress topper is useful if you are comparing options.
Change what happens before bed
Night sweats often begin before you are asleep. Your evening inputs matter.
A few adjustments help many women:
Take a cool or lukewarm shower
Avoid heavy evening meals if they leave you warm or uncomfortable
Notice alcohol patterns
Watch spicy food if you already run hot at night
None of those are moral rules. They are experiments. If one trigger is obvious for you, that is valuable information.
If heat is the main reason you wake, solve heat first. Do not expect meditation to fix a thermostat problem.
A short visual guide can help if hot flashes are your main issue:
▶ PlayPrepare for the wake-up, not just bedtime
This is a part many overlook. Set up the room so a hot flash is less disruptive when it happens.
Keep a spare top nearby. Use layers instead of one heavy blanket. Place water where you can reach it without fully getting up. The goal is to shorten the time between overheating and settling back down.
The best night-sweat plan is not the one that sounds impressive. It is the one that helps you cool quickly, stay calm, and get back to sleep without turning one wake-up into two hours awake.
Calm a Racing Mind with Cognitive Strategies
When women ask me how to sleep better during perimenopause, this is often the turning point. Not because the sleep problem is “mental,” but because once your brain starts anticipating a bad night, insomnia can continue even after the original trigger changes.
CBT-I is the first-line treatment for perimenopause-related insomnia, and 70 to 80% of users achieve lasting remission. Key steps include using the bed only for sleep and limiting time in bed to actual sleep time, with sleep efficiency targets above 85% reported within weeks (Ubie Health).

Use the bed only for sleep
This is called stimulus control, and it matters more than many expect.
If you lie in bed awake for long stretches, scrolling, worrying, or trying to force sleep, your brain starts linking the bed with alertness. That association is powerful.
A better approach:
Use the bed for sleep and sex only
If you are awake for about 20 minutes, get up
Go somewhere dim and quiet
Do something low-stimulation until you feel sleepy again
That may sound annoying. It is often effective.
Match time in bed to real sleep
Many tired women start going to bed earlier, sleeping in later, or resting in bed more. It feels logical. It often backfires.
Sleep restriction means you temporarily limit time in bed to closer to the amount of sleep you are getting. That creates stronger sleep drive. Then you gradually expand time in bed as sleep becomes more solid.
This works best when done carefully. Keep it simple:
If your pattern is | Try this response |
|---|---|
You spend hours awake in bed | Shorten time in bed |
You fall asleep on the couch, then wake in bed | Move bedtime later and make it intentional |
You nap long and late | Protect nighttime sleep first |
Challenge the story your brain tells at 2 a.m.
Perimenopause can increase anxiety sensitivity. That means a normal middle-of-the-night wake-up can quickly turn into catastrophic thinking.
Common thought: “I’m awake again. Tomorrow is ruined.”
More useful thought: “I’m awake right now. My job is to stay calm, not to force sleep.”
Try a brief worry journal before bed with prompts like:
What is the specific worry?
Can I act on it tonight?
If not, when will I revisit it tomorrow?
What would I say to a friend having this exact thought?
Use one body-based downshift
A racing mind is often a keyed-up body. Give your nervous system a physical cue.
Try 4-7-8 breathing:
Inhale for 4
Hold for 7
Exhale for 8
Do a few rounds without trying to “perform” relaxation. The point is not to knock yourself out. The point is to interrupt the stress loop.
Your goal in the middle of the night is calm, not perfect sleep on demand. Calm often lets sleep return on its own.
Fueling Better Sleep Through Diet and Lifestyle
What you eat, when you move, and how you pace your day all affect nighttime sleep. In this context, small decisions can either support your hormones or make a fragile night more fragile.
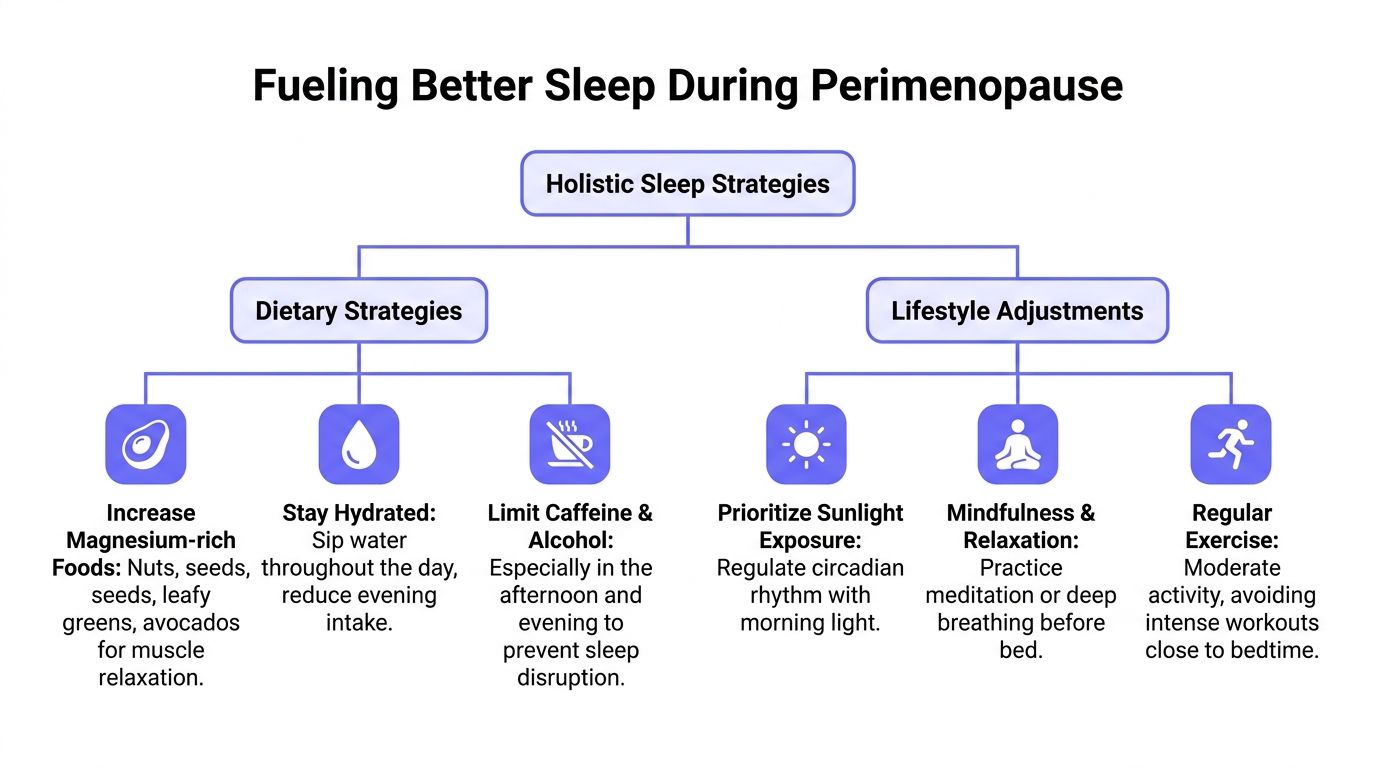
Start with food that supports calm
Declining progesterone can contribute to anxiety and lighter sleep, and one often-overlooked strategy is supporting the body’s calming systems with magnesium-rich foods such as spinach and almonds for muscle relaxation and nervous system regulation (Bristol Menopause Clinic).
This does not mean food is a cure. It means nutrition can either make settling easier or harder.
A practical hierarchy:
Most useful: regular meals, enough protein, magnesium-rich foods, steady hydration through the day
Worth testing: whether late heavy meals, alcohol, or excess caffeine worsen your sleep
Less useful: buying random “sleep foods” without tracking whether they help
Exercise timing matters
Movement supports sleep, but the timing and intensity matter.
For many women:
Morning daylight plus a walk helps anchor circadian rhythm
Moderate daytime exercise supports sleep pressure at night
Hard late-evening workouts can leave the body too activated close to bedtime
If you already know exercise helps your mood but not your sleep, timing may be the issue rather than the activity itself.
Medical options deserve a calm conversation
Lifestyle changes are foundational, but they are not the only path. If sleep disruption is severe, persistent, or clearly tied to broader menopausal symptoms, it is reasonable to discuss medical options with a clinician.
Here is a simple way to think about the tiers:
Tier | What it can help with |
|---|---|
Food and lifestyle | Baseline support, rhythm, nervous system steadiness |
Behavioral treatment | Insomnia patterns, conditioned wakefulness, racing thoughts |
Clinical care | More severe symptoms, medication review, hormone discussions |
Hormone therapy is a medical decision, not a lifestyle hack. Some women want it. Some do not. Some cannot use it. The right decision depends on your symptom pattern, health history, and preferences.
The best approach is honest: use the least complicated tools that help, and escalate care when self-management is not enough.
Create Your Personalized Sleep Action Plan
The biggest mistake I see is trying five changes at once and learning nothing from the results. Perimenopause sleep gets easier when you track patterns with enough detail to spot cause and effect.
Keep your plan narrow for one week
Pick one action from each category:
Environment: cooler bedding, fan, darker room
Mind: worry journal, stimulus control, 4-7-8 breathing
Body: magnesium-rich evening snack, earlier dinner, morning walk
That is enough for a real test.
Track the right things
A useful sleep log is short. You do not need a spreadsheet obsession. You need consistency.
Record:
Bedtime and wake time
How long it took to fall asleep
Night sweats or hot flashes
Racing thoughts or anxiety
Alcohol, caffeine, late meals, or exercise timing
What you tried that night
One option is Lila, which lets users log sleep, meals, mood, energy, and symptoms in one place so they can look for patterns between things like food intake, hot flashes, anxiety, and poor sleep.
Review patterns, not single nights
A bad night proves very little. A repeated pattern tells you what to change.
Look for questions like:
Do I wake more on nights I drink alcohol?
Does a cooler room reduce how long I stay awake after a hot flash?
Is my sleep worse when I skip movement?
Am I dealing more with heat, anxiety, or light sleep?
That is how to sleep better during perimenopause in a way that lasts. You stop guessing and start matching the intervention to your body’s pattern.
If you want a simpler way to track symptoms, sleep, meals, mood, and routines in one place, take a look at Lila. It can help you turn scattered sleep advice into a plan you can test, adjust, and follow consistently.
Get Lila, your personal coach for perimenopause.
Built for women in their 40s. 24/7 coaching, in your pocket.


