
Do Hot Flashes Cause High Blood pressure? The Full Story
May 1, 2026
A lot of women ask this question in the middle of a very ordinary moment. You’re answering emails, making dinner, or trying to fall asleep, and suddenly a wave of heat rises through your chest and face. Your skin flushes. Your heart starts pounding. For a few seconds, it can feel unsettling enough to make you wonder, Is this raising my blood pressure?
That concern is reasonable. A hot flash can feel dramatic because your body is doing something dramatic. It isn’t “just in your head,” and it isn’t a trivial symptom you have to dismiss. At the same time, the answer isn’t a simple yes or no. The complete explanation is more useful than that.
Hot flashes can trigger short-term cardiovascular changes in the moment. But the bigger question for long-term health isn’t only whether one hot flash causes a blood pressure spike. It’s how often hot flashes happen, when they happen, and what pattern they follow over time. That pattern can tell you much more about your body than one isolated episode.
That Sudden Wave of Heat and a Pounding Heart
You might know this feeling exactly.
You’re in a meeting, and your neck suddenly feels hot. A minute later, your face is flushed, your shirt feels too warm, and your heart seems louder than the room around you. Or maybe it happens at 2 a.m. You wake up sweating, your chest feels busy, and the first thought that lands is, something is off.

That moment can be confusing because a hot flash often overlaps with other sensations. Heat. Sweating. A pounding heartbeat. Sometimes shakiness. Sometimes anxiety. If you’ve also noticed fluttering or skipped beats, it can help to read more about menopause heart palpitations, causes, symptoms, and relief.
Why this feels alarming
Your body is sending signals fast, and fast signals grab your attention. A hot flash may last only a short time, but it can feel much longer because it activates several systems at once.
Common thoughts women have in that moment include:
“Is this anxiety or menopause?” Sometimes it’s hard to separate them because both can involve sweating and a racing heart.
“Am I having a blood pressure spike?” That can happen temporarily during a hot flash.
“Should I be worried about my heart?” The honest answer is that symptoms deserve attention, especially if they’re frequent or changing.
A symptom can be common and still deserve respect.
The goal isn’t to scare you. It’s to replace vague worry with a clearer picture of what’s happening. Once you understand the mechanics, the experience often feels less mysterious and more manageable.
Your Body's Thermostat on the Fritz
A hot flash is easier to understand as a glitch in your brain’s internal temperature control system.
The key player is the hypothalamus, a small area of the brain that helps keep body temperature in a comfortable range. During the menopause transition, shifting hormone levels can make that system unusually reactive. A small change in body temperature, stress, or even a warm room can set off a response that feels much bigger than the trigger. If you want a fuller explanation of the symptom itself, this guide on why you may be having hot flashes can help.
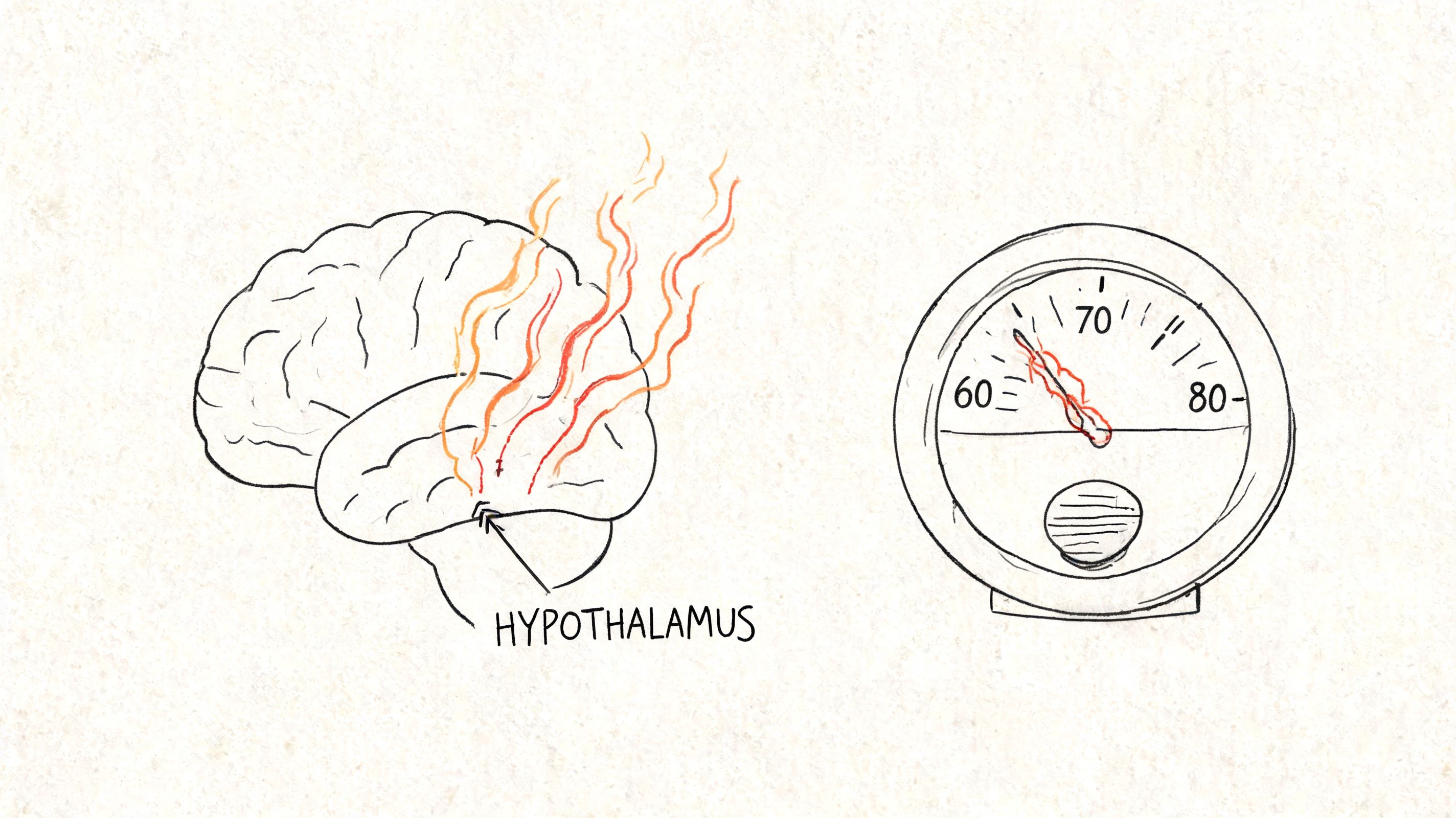
What a hot flash actually is
Your body reacts as if it needs to cool down fast, even when you are not overheating. It opens the escape valves all at once.
That response can include:
Blood vessels widening near the skin, which causes flushing and a sudden rush of heat
Sweating, which helps release heat
A faster or stronger heartbeat, as the nervous system joins the response
A chill afterward, when the cooling response overshoots
That sequence explains why the experience often comes in stages. First the surge of heat. Then sweating. Then a damp, shaky, or chilled feeling once your body has tried to cool itself too aggressively.
Why the symptoms come in a cluster
A hot flash involves several body systems at the same time. The brain sends the alarm. Blood vessels respond. Sweat glands switch on. The nervous system adds that jangly, revved-up feeling.
That is why many women describe a hot flash as a wave. It rises, crests, and passes, instead of feeling like one isolated symptom.
Practical rule: If heat, flushing, sweating, and then cooling tend to show up in the same order, you are probably noticing a vasomotor symptom pattern.
This short explainer may help you visualize the process:
Why this connects to blood pressure
The connection to blood pressure becomes clearer once you understand the thermostat error. A hot flash does not affect temperature alone. It also activates the systems that control blood vessel tone and heart rate.
One episode may cause only a brief shift. The larger question is pattern. If hot flashes happen often, wake you at night, or start clustering at certain times, that repeated strain may matter more than any single event. That is why tracking frequency and timing can be so helpful. It gives you a clearer picture of your own symptom pattern, which is often more useful than a simple yes-or-no answer.
The Momentary Spike The Science Behind Hot Flashes and BP
You feel the rush first. Heat climbs, your heart starts pounding, and you may wonder whether your blood pressure is shooting up too.
For many women, the answer is yes, in the moment.
A hot flash is not only a temperature event. It also briefly activates the cardiovascular system. Heart rate can rise. Blood vessels change tone quickly. Blood pressure may increase for a short period while your body reacts to that sudden internal alarm. The key idea is timing. A temporary surge during an episode is different from having hypertension all day, every day.
One of the clearest studies on this question came from Weill Cornell. Researchers monitored 154 women with portable ambulatory blood pressure devices. 51 women reported hot flashes in the prior two weeks. Among women with hot flashes, mean awake systolic blood pressure was 141 mmHg, compared with 132 mmHg in women without hot flashes. During sleep, mean systolic pressure was 129 mmHg versus 119 mmHg. As reported by Weill Cornell’s summary of the 2007 hot flash and blood pressure study, those differences remained statistically significant even after researchers adjusted for age, body mass index, race or ethnicity, and other standard blood pressure risk factors.
That finding is significant because the connection did not disappear after accounting for the usual explanations. Researchers were not merely observing that one group was older or had more baseline risk. Hot flashes were still associated with higher blood pressure readings.
A useful comparison is a smoke alarm that keeps going off when there is no fire. Each alarm is brief, but it still jolts the whole house. In your body, that jolt can show up as a short-lived rise in heart rate and blood pressure.
So do hot flashes cause high blood pressure
The most accurate answer is more precise than a simple yes or no.
Question | Best answer |
|---|---|
Can a hot flash raise blood pressure in the moment? | Yes. Research supports short-term increases during episodes. |
Does one hot flash mean you have hypertension? | No. A temporary rise is different from a diagnosis of chronic high blood pressure. |
What deserves the closest attention? | Your pattern over time. Frequent or recurring episodes may be more meaningful than one isolated spike. |
This is why home tracking can be so helpful. If you check readings with essential home healthcare blood pressure equipment and log when flashes happen, you start to see whether symptoms cluster at certain hours, disturb sleep, or happen often enough to deserve a closer conversation with your clinician.
One episode is a moment. A repeated pattern is a health signal.
Why Hot Flash Frequency Matters More Than You Think
If a single hot flash is one wave hitting the shore, frequent hot flashes are many small waves hitting the same place over and over. One wave may not change the coastline much. Repeated waves can reshape it.
That’s the more useful way to think about long-term risk.
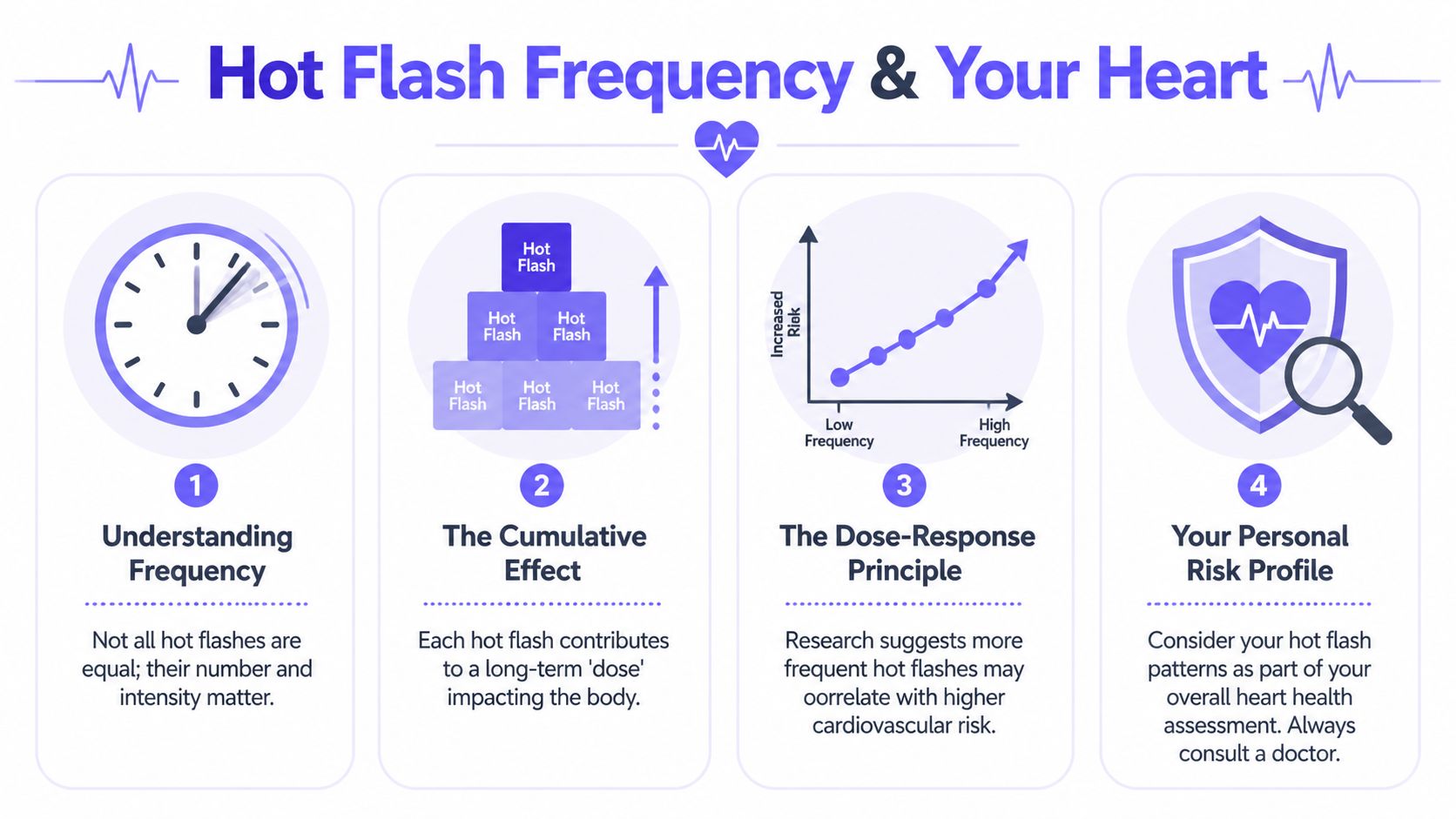
The pattern matters more than the drama of one episode
Many women focus on intensity. Was that flash terrible? Did it wake me up drenched? Did I feel shaky?
Intensity matters for quality of life, but frequency may tell you more about cardiovascular burden. Research from the University of Colorado Anschutz notes that women with hot flashes and night sweats on 6 or more days out of 14 during early menopause had a 62% increased relative risk for major adverse cardiovascular events such as heart attack or stroke. Women with sustained frequent symptoms across multiple annual assessments had a doubling of cardiovascular event risk compared with asymptomatic women, even after adjustment for factors including smoking, physical inactivity, obesity, hypertension, hyperlipidemia, diabetes, socioeconomic status, and education, according to the CU Anschutz article on hot flashes and heart attacks.
Why repeated episodes may strain the body
Hot flashes don’t just create discomfort. They repeatedly activate systems involved in blood vessel tone, heart rate, and stress signaling. Researchers have also linked severe hot flashes with inflammatory changes and markers of subclinical cardiovascular disease in that same summary.
A helpful way to frame it:
One event may create a brief physiologic surge.
Frequent events mean your body repeats that surge often.
Sustained frequent events may signal a bigger cardiovascular pattern that deserves attention.
If your symptoms happen often, the question isn’t only “How bad does each hot flash feel?” It’s also “How often is my body being pushed through this cycle?”
A simple way to think about risk
Here’s a plain-language comparison:
Symptom pattern | What it may suggest |
|---|---|
Occasional hot flashes | A common menopause symptom that may still be uncomfortable, but offers less information on cumulative burden |
Frequent hot flashes over recent weeks | A stronger clue that your cardiovascular system may be under repeated short-term stress |
Frequent symptoms that persist over time | A pattern worth discussing with a clinician, especially if you also have other heart risk factors |
The takeaway isn’t that every woman with frequent hot flashes should panic. It’s that symptom pattern is meaningful data. If you want to understand whether hot flashes affect your heart health, start by asking how often, when, and for how long.
Assessing Your Personal Cardiovascular Risk Profile
Hot flashes don’t exist in a vacuum. They matter most when you view them alongside the rest of your cardiovascular picture.
A woman with frequent vasomotor symptoms and no other major risk factors may need one kind of conversation with her clinician. A woman with the same symptom pattern plus smoking, prediabetes, known hypertension, or a strong family history may need a different level of follow-up.
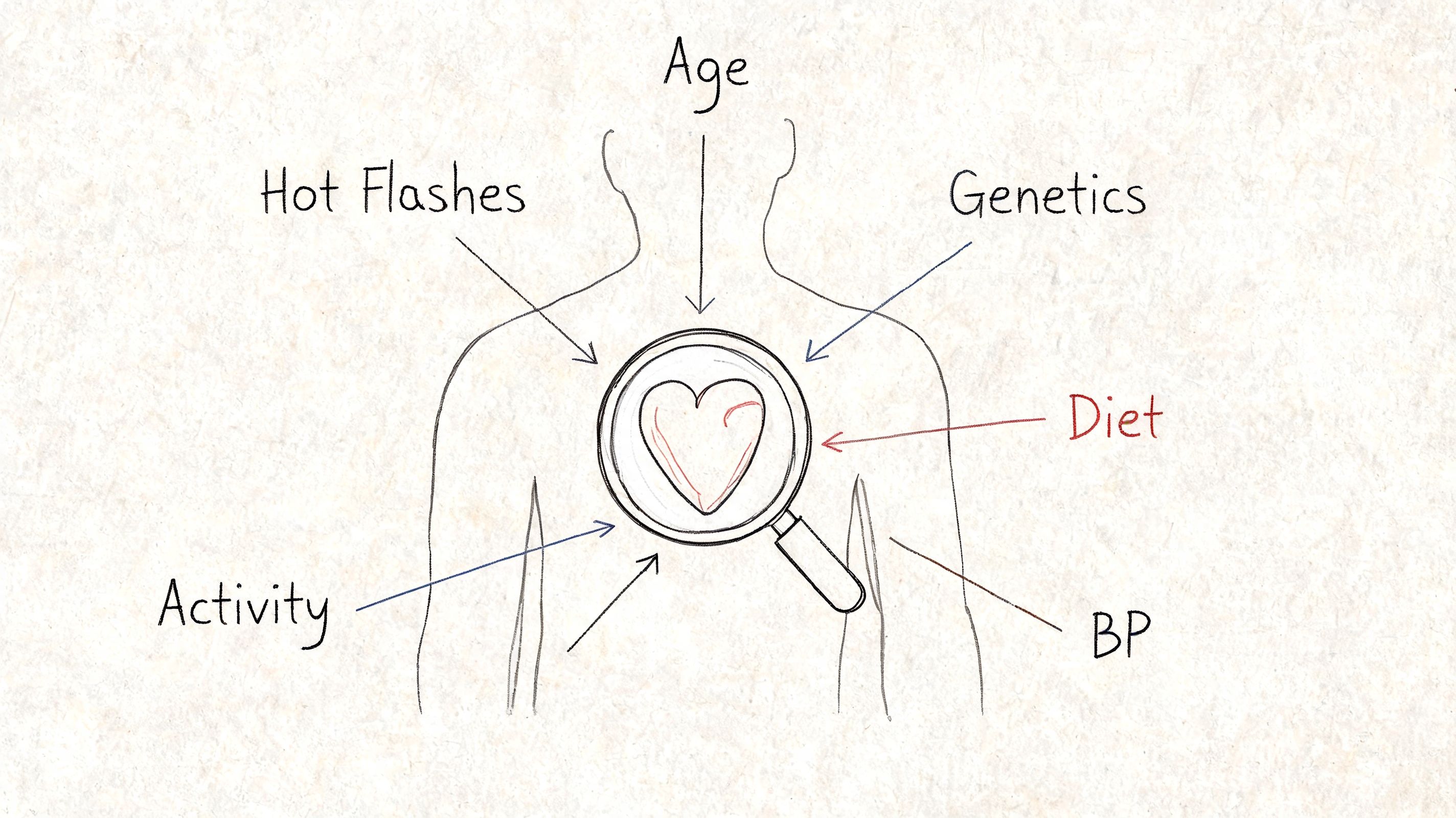
The main categories to think through
Metabolic factors
Weight distribution, insulin resistance, cholesterol issues, and existing high blood pressure all shape your baseline risk. If hot flashes are frequent on top of these factors, they may act more like a warning light than a standalone nuisance.
Lifestyle factors
Smoking, low physical activity, poor sleep, and a diet that makes blood pressure harder to control can all make the overall picture less forgiving. Night sweats matter here too because sleep disruption can ripple into daytime blood pressure, concentration, mood, and appetite.
Non-modifiable factors
You can’t change your age, genetics, or family history. But you can use them to decide how proactive to be. If close relatives had heart disease, stroke, or hypertension, recurring hot flashes become more important to track and discuss.
Questions worth asking yourself
Rather than trying to self-diagnose, use a few grounded questions:
Do my hot flashes cluster at night, during stress, or after poor sleep?
Have I ever had high blood pressure readings outside a hot flash?
Do I already know I have risk factors like high cholesterol, diabetes, or hypertension?
Have my symptoms become more frequent or more disruptive lately?
Recent changes often matter more than distant history.
A practical home-monitoring setup
If you want clearer information before a medical visit, home blood pressure checks can help. Some women like using essential home healthcare blood pressure equipment so they can record readings under usual day-to-day conditions instead of relying on one office measurement.
Keep your notes simple. Write down the reading, time of day, whether a hot flash happened near that reading, and any obvious triggers such as stress, alcohol, poor sleep, or exercise. You’re looking for patterns, not perfection.
A Proactive Plan to Manage Symptoms and Protect Your Heart
The most helpful response to this information is not fear. It’s tracking, adjusting, and speaking up early.
One research review found that the hot flash and blood pressure association was “strongest, almost universally, for analyses pertaining to hot flashes experienced in the last 30 days”, suggesting recent symptom patterns may be more informative than lifetime history, as discussed in this review on vasomotor symptoms and blood pressure patterns. That’s a strong argument for paying attention to what’s happening now, not just what happened years ago.
Start with a short tracking routine
You don’t need a complicated spreadsheet. A simple daily log can reveal a lot.
Track these for a few weeks:
Hot flash timing
Morning, afternoon, evening, overnight.Frequency
Don’t judge it. Just count it.Context
Stressful day, spicy meal, alcohol, poor sleep, exercise, warm room.Blood pressure readings
Take them under calm conditions and note whether a hot flash happened near that time.
This kind of recent, real-world record often gives your clinician a much clearer picture than “I’ve had hot flashes on and off for years.”
Build habits that support both symptoms and blood pressure
Management works best when it pulls double duty. Some changes can support vasomotor symptoms and cardiovascular health at the same time.
Regular aerobic activity can help balance blood pressure and delay hypertension onset. Consistency matters more than heroic workouts.
Sleep protection matters because repeated nighttime symptoms can fragment sleep, and poor sleep can make the next day harder on your body.
Stress-lowering practices like paced breathing may help during high-risk windows, especially if your symptoms cluster around tension or overwhelm.
Heart-supportive eating patterns can make blood pressure easier to manage over time.
If you want a broader overview of understanding and managing blood pressure, that guide can complement the menopause-specific strategies you use.
Small routines beat dramatic resets. The body responds to repetition.
Know when to bring in your clinician
Make an appointment sooner if:
Symptoms are becoming frequent
Night sweats are wrecking your sleep
Home readings are high
You have chest pain, fainting, severe shortness of breath, or new concerning symptoms
A visit can also be a good time to ask whether menopause treatment options are appropriate for you. If you want a plain-English overview before that conversation, this guide on what is hormone therapy for menopause can help you prepare better questions.
Bring your notes. A doctor can do more with “I had hot flashes on most days over the last two weeks, and my BP seemed higher after poor sleep” than with “I’m not sure, but menopause feels rough lately.”
Your Path Forward with Menopause
You are standing in your kitchen, a rush of heat climbs into your chest and face, and your heart starts thumping hard enough to get your attention. A few minutes later, it passes. The question that lingers is the one many women ask in midlife. Was that just a hot flash, or is my blood pressure becoming a problem too?
The clearest answer is a nuanced one. A hot flash can cause a brief rise in blood pressure during the episode, but your longer-term heart picture is shaped more by the pattern of symptoms than by one isolated moment. Frequency matters. Timing matters. Clusters of symptoms matter.
That pattern-based view can feel more manageable once you know what to look for. Your body is giving signals, not random noise. A single hot flash is like one loud knock at the door. Repeated hot flashes, especially if they happen often or disrupt sleep, deserve a closer look because they may line up with broader cardiovascular changes that become more relevant in the menopause transition.
The most useful takeaway
Treat hot flashes as information.
That means paying attention without panicking. Notice how often they happen, whether they show up mostly at night, whether they come with a pounding heart, and whether rough sleep or stress seems to make them more common. Then place those symptoms next to the rest of your cardiovascular risk profile, including blood pressure readings, family history, cholesterol, activity levels, and sleep quality.
What to keep in mind
A hot flash can briefly raise blood pressure
Frequent or clustered hot flashes usually matter more than isolated episodes
Recent symptom patterns are often more helpful than vague memories from months ago
Tracking symptoms over time can reveal trends you would otherwise miss
A clinician can give better guidance when you bring a clear record of what has been happening
Menopause asks you to learn a new version of your body. That can feel unsettling at first, but it can also become a source of clarity. The goal is not to chase every symptom. The goal is to notice patterns early enough to make thoughtful decisions.
If you want a simple way to track hot flashes, sleep, mood, energy, and the patterns that matter most in perimenopause, Lila can help you turn daily symptoms into clearer insights and practical next steps.
You should not have to do it all on your own










