
Conquer menopause joint pain: Practical Tips for Lasting Relief
Mar 14, 2026
If you've started waking up with stiff, achy knees or suddenly find your hands are sore for no apparent reason, you're not imagining things. And you're definitely not alone. This is menopause joint pain, a frustratingly common symptom that’s directly tied to the hormonal shifts happening in your body. But it isn't a life sentence.
Why Your Joints Suddenly Ache During Menopause
Think of estrogen as your body's built-in anti-inflammatory and joint lubricant. It works quietly in the background, keeping cartilage plump and hydrated, tamping down inflammation, and generally making sure your joints move smoothly. As you enter perimenopause and menopause, your estrogen levels drop—sometimes dramatically.
When that happens, your joints lose one of their most important protectors. It's like a key member of your internal maintenance crew suddenly walked off the job.
The result is often a sudden increase in stiffness, aches, and general discomfort that can make you feel years older overnight. Understanding this hormonal link is the first step toward getting a handle on the pain and finding real relief.
The Direct Link Between Estrogen and Joint Health
This isn't just a vague theory; it's a physiological fact. Joint pain is a major symptom for an estimated 70% of women going through menopause. Scientists have found estrogen receptors in all parts of our joints, from the cartilage that cushions them to the bones they connect.
As estrogen levels fall, it can set off a cascade of effects, including increased inflammation, fluid loss in your connective tissues, and even a heightened perception of pain. This is why aches can seem to pop up everywhere, though they often hit weight-bearing joints like the knees, hips, and spine the hardest. You can dive into the research on how menopause affects joint health if you want to explore the science more deeply.
Knowing this connection is powerful. It confirms that the pain is real and stems from concrete biological changes, not just from "getting older."
To see how these changes play out, let’s break it down. Here's a quick look at what's happening inside your joints.
Menopause and Joint Pain at a Glance
Symptom | Underlying Cause (Estrogen Decline) | Commonly Affected Joints |
|---|---|---|
Increased Stiffness | Loss of fluid and elasticity in connective tissues. | Hands, Wrists, Knees, Hips |
Widespread Aches | Heightened inflammation and pain perception. | Shoulders, Neck, Back, Hips |
Reduced Mobility | Cartilage thinning and increased friction in joints. | Knees, Spine, Hips |
Essentially, the loss of estrogen makes your joints more vulnerable to inflammation, stiffness, and the general wear and tear of daily life.
How Hormonal Shifts Impact Your Joint Health
If you've started noticing new aches and stiffness in your joints, you're not imagining things. To really get what’s happening, it helps to see estrogen as your body's natural anti-inflammatory and joint protector. It’s been working behind the scenes for decades, helping to maintain cartilage, regulate the fluid that keeps joints lubricated, and manage inflammation.
During perimenopause and menopause, estrogen levels don't just dip—they can plummet. When this happens, it's like your body's built-in joint maintenance crew goes on an extended vacation. Without enough estrogen to keep things running smoothly, inflammation can flare up, cartilage can lose its cushioning, and your perception of pain can actually increase.
This simple map shows how it all connects.
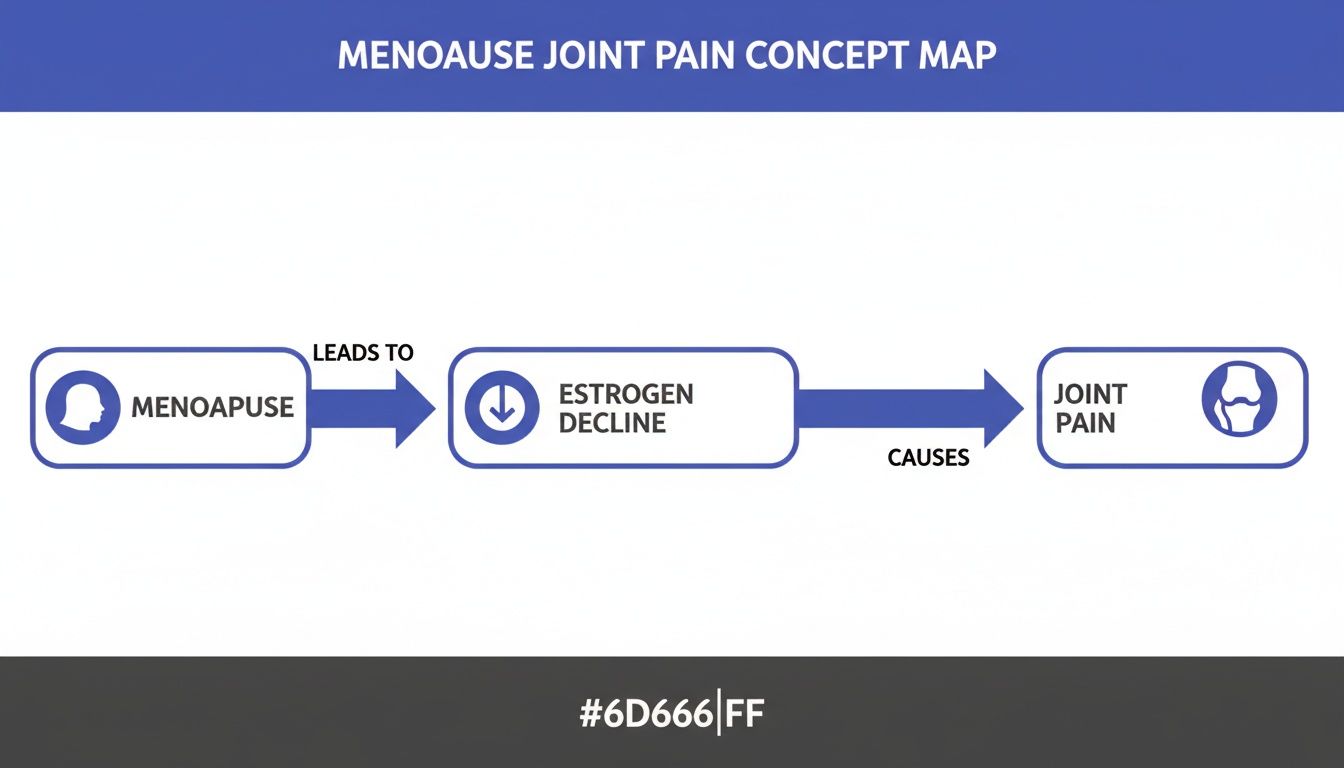
As you can see, the root cause is often the hormonal shift itself, not necessarily a brand-new injury or disease.
The Estrogen Effect on Inflammation and Cartilage
When your estrogen levels are consistent, they do a fantastic job of keeping inflammation under control. As those levels become erratic and decline, your body's inflammatory response can get louder, which is why joints that have never given you trouble might suddenly start to ache.
Think of it like a sound system. Estrogen acts as a volume dial for pain signals. When estrogen is high, the volume is low. As levels drop, the volume gets turned up, making you more sensitive to discomfort.
This drop in estrogen can also unmask or worsen underlying issues. If you have a touch of osteoarthritis that you never even noticed, the hormonal changes can suddenly make the symptoms feel much more intense. Weaker cartilage and less joint lubrication mean that simple, everyday movements can start to feel like a chore.
The Growing Link to Osteoarthritis
This connection is so profound that it’s changing how experts view joint health in women over 40. For many, menopause unfortunately marks the start of a painful relationship with joint problems. In fact, global data from 1990 to 2021 showed a massive 130% increase in postmenopausal osteoarthritis. New cases have surged by 133%, reaching 14.3 million every year.
This isn't just "menopausal arthralgia" (achy joints without damage); it’s often the acceleration of a degenerative joint disease. The loss of estrogen doesn't just cause pain—it contributes to the actual breakdown of the joint structure.
It also affects bone density, which is critical for the integrity of your entire skeletal system. Learning about nourishing your bones is a great next step, as healthy bones provide a strong foundation for your joints. The more you understand what’s happening inside your body, the better equipped you'll be to find relief that works.
Everyday Lifestyle Changes for Soothing Your Joints
Knowing that hormones are behind your new aches and pains is one thing, but figuring out what to do about it is what really matters. The good news is that you have a surprising amount of control over how your joints feel, and it all comes down to your daily habits. Think of these strategies as your personal toolkit for reducing inflammation, boosting flexibility, and building a more resilient body from the inside out.
We’ll focus on four foundational pillars that can make a world of difference: gentle movement, smart weight management, an anti-inflammatory diet, and high-quality sleep.
Embrace Gentle Movement
When your joints are screaming, the last thing you probably want to do is get up and move. But here’s the paradox: the right kind of movement is exactly what they need to feel better. It helps lubricate the joints and strengthens the muscles that hold them steady. It's a lot like working a rusty hinge back and forth with a little oil—that motion is essential to get things working smoothly again.
High-impact exercises like running can feel jarring right now, but low-impact activities are your new best friend.
Swimming and Water Aerobics: The beauty of being in water is that it supports your body weight. This takes all the pressure off your joints while the water itself provides gentle resistance to build muscle.
Yoga and Tai Chi: These ancient practices are phenomenal for improving your flexibility, balance, and overall range of motion. The slow, mindful movements help ease stiffness without putting any undue stress on your body.
Targeted Strength Training: Think of strong muscles as your body's personal shock absorbers. By focusing on strengthening the muscles around your knees, hips, and core, you give your joints a much-needed support system.
Manage Your Weight Mindfully
Your joints, particularly your knees and hips, bear the load of your body with every single step. Research has found that for every one pound of body weight you lose, you take four pounds of pressure off your knees. That adds up fast!
During menopause, hormonal fluctuations can make weight management feel like an uphill battle. But even a modest weight loss of just 5-10% of your body weight can bring a significant improvement in joint pain and function.
This isn't about drastic diets. A combination of gentle, consistent exercise and mindful eating is a far more sustainable and effective way to reach a healthier weight and give your joints a well-deserved break. If you’re struggling with discomfort in your lower body specifically, our guide on managing menopause hip pain has more targeted tips you might find helpful.
Shift to an Anti-Inflammatory Diet
What you put on your plate can either fan the flames of inflammation or help put them out. Since your body is already more prone to inflammation as estrogen declines, an anti-inflammatory diet is a powerful way to calm your system from within and soothe those aches.
The approach is refreshingly simple: eat less of the foods that trigger inflammation and more of the foods that fight it.
Foods to Limit:
Sugar and Refined Carbs: Things like white bread, pastries, and sugary sodas are notorious for causing inflammatory spikes.
Processed Foods: Many packaged snacks and fast foods are loaded with unhealthy fats and additives that your body treats as intruders, triggering an inflammatory response.
Foods to Enjoy:
Fatty Fish: Salmon, mackerel, and sardines are packed with omega-3 fatty acids, which are potent natural anti-inflammatories.
Berries and Leafy Greens: These foods are bursting with antioxidants that help shield your cells from the stress that leads to inflammation.
Turmeric and Ginger: These spices aren’t just for flavor; they contain powerful compounds that have been used for centuries to reduce inflammation.
Prioritize Restorative Sleep
Sleep is your body's dedicated repair shift. When you don't get enough quality rest, it doesn't just leave you feeling tired—it can actually lower your pain threshold, making every ache and pain feel that much worse. Of course, menopause symptoms like night sweats often get in the way, creating a frustrating cycle of pain and exhaustion.
This is where focusing on your sleep hygiene can be a game-changer. Aim for 7-9 hours of quality sleep each night. You can get there by creating a calming bedtime routine, keeping your bedroom cool and dark, and putting away all screens at least an hour before you turn in. Better sleep gives your body the downtime it needs to heal, reduce inflammation, and turn down the volume on pain.
Exploring Medical and Therapeutic Treatments
If you’ve tried adjusting your diet, exercise, and sleep habits but are still waking up stiff and achy, don't lose hope. Sometimes, lifestyle changes aren't enough to tackle menopause-related joint pain on their own. At this point, it’s a good idea to chat with your healthcare provider about medical and therapeutic options that can offer more powerful relief.
Hormone Replacement Therapy (HRT) for Joint Pain
Since falling estrogen levels are at the heart of menopausal joint pain, it makes sense that putting some of that estrogen back can help. That's essentially what Hormone Replacement Therapy (HRT) does. By reintroducing estrogen, HRT can tackle the inflammation and dryness inside your joints, bringing back some much-needed lubrication and easing those widespread aches.
For many women, HRT is a game-changer. By addressing the root hormonal cause, it can alleviate not only joint pain but also other challenging symptoms like hot flashes, night sweats, and mood swings.
Of course, the first step is always a thorough conversation with your doctor. They’ll need to go over your personal and family medical history to make sure HRT is a safe and smart choice for you, walking you through all the benefits and things to consider.
Medications and Supplements for Targeted Relief
Beyond hormones, a whole host of other options can help you get a handle on the pain and inflammation. Think of these as tools in your toolkit—you can use them on their own or combine them with other strategies to build a plan that works for you.
Common Medical and Supplemental Options
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): An over-the-counter staple like ibuprofen can be a lifesaver for managing those occasional, intense flare-ups. It works by blocking the enzymes that trigger pain and swelling.
Turmeric (Curcumin): You probably know this as a bright yellow spice, but its active compound, curcumin, is a well-known anti-inflammatory. Adding it to your meals or taking it as a supplement could help soothe chronic aches.
Glucosamine and Chondroitin: These are natural building blocks of cartilage, the cushion in our joints. While the research is a bit mixed, some women swear by these supplements for reducing pain and improving how their joints feel over time.
Omega-3 Fatty Acids: Found in fatty fish like salmon or in supplement form, omega-3s are powerful anti-inflammatories that are fantastic for overall joint health.
Sometimes, joint pain can manifest in very specific ways, like the intense pain and stiffness of a "frozen shoulder." Learning more about the connection between frozen shoulder and menopause can help you and your doctor find more targeted solutions.
Hands-On Therapeutic Approaches
Don't underestimate the power of physical touch and guided movement. Hands-on therapies can be incredibly effective when you’re feeling stiff and sore. Physical therapy, for instance, is all about strengthening the muscles that support your joints, improving your range of motion, and fixing any postural habits that might be making things worse. A good physical therapist will design a program just for you.
Massage therapy is another fantastic tool. It's wonderful for releasing tight muscles and boosting circulation to stiff, painful areas. Understanding the role of massage in managing joint pain can show you how this kind of direct, soothing relief fits perfectly alongside other treatments.
How Tracking Your Symptoms Unlocks a Personal Relief Plan
Knowing why your joints ache during menopause is a great start, but the real breakthrough comes when you start connecting the dots in your own daily life. Menopause symptoms almost never show up alone; they’re tangled together. A bad night's sleep can easily trigger a morning of intense joint stiffness, which then tanks your mood and energy for the rest of the day.
Think of yourself as a detective investigating your own body. By simply paying attention and noting when your joint pain flares, what you ate, how you slept, or even how you felt emotionally, you start to uncover clues. These clues are the key to creating a relief plan that actually works for you.
From Clues to Concrete Actions
This is where symptom tracking stops feeling like a chore and becomes your most powerful tool. When you monitor these different pieces of your well-being together, you’re not just logging information—you’re drawing a personal map that leads straight to feeling better.
For example, you might discover your knee pain is always worse the day after eating a sugary dessert. Or maybe you'll see a clear pattern between a stressful workday and waking up with an aching back. These aren't just random occurrences; they are your body giving you specific feedback.
This simple process can shift your mindset from a vague frustration like, "My joints always hurt!" to a specific, solvable problem: "My joint pain spikes after I eat sugar and when I don't get enough sleep." That change in perspective is everything when it comes to taking back control.
This is exactly where a tool designed for menopause can make a world of difference. The Lila app was built to help you see these connections without all the guesswork.
It makes it easy to log your daily experiences—from pain levels and sleep quality to mood and energy—all in one place.
This simple daily check-in gathers the "dots" of your health story, making it easy for both you and the app to see the bigger picture emerge.
Building Your Personalized Path Forward
Once you start logging your symptoms, a tool like Lila translates that information into a clear plan. It learns your unique patterns and provides daily, practical guidance to help you manage your specific triggers.
Pinpoint Your Triggers: The app might highlight that your hand stiffness consistently flares up after you eat processed foods, suggesting a simple dietary swap.
Connect Symptoms to Solutions: You might see that a 10% improvement in your sleep quality leads to a 20% reduction in next-day joint pain, giving you a powerful reason to protect your bedtime routine.
Get Daily Guidance: Instead of wondering what to do next, you'll get small, achievable tasks based on what’s proven to help you, like a reminder to do a 15-minute gentle stretch or to drink more water.
This approach takes the guesswork out of managing your joint pain. You can learn more about how a menopause symptom tracker app can help you find your patterns and start feeling better. It’s all about working smarter, not harder, to soothe your joints and feel more like yourself again.
Building Your Personal Joint Pain Action Plan
Alright, we've covered a lot of ground. Now, let's pull all of that knowledge together and turn it into a plan that actually works for you. Getting a handle on menopause-related joint pain isn't about some grand, overwhelming gesture. It’s about creating your own clear path forward, one small, smart step at a time.
Think of this as your personal mission to reclaim comfort and control. The goal is simple: to move from feeling stuck and frustrated by the pain to feeling knowledgeable and empowered to do something about it.
Your Four-Step Roadmap to Relief
This isn't a race. Each of these steps is designed to build on the one before it, helping you create a solid foundation for long-term joint health and real relief from that nagging pain.
Start Tracking Your Symptoms: The first step is always to understand what you're dealing with. Use a tool like the Lila app to start logging when your joints ache, what you ate, how you slept, and how you're feeling. This isn't just busywork—it’s detective work. You’re gathering the clues that will reveal your unique pain patterns and triggers.
Implement One Small Lifestyle Change: Don’t try to overhaul your entire life overnight. That's a recipe for burnout. Once your tracking reveals a potential pattern, pick just one small thing to try. Maybe it's a 15-minute walk every morning, adding salmon to your dinner twice a week, or setting a non-negotiable bedtime. The key is to make it small enough to be sustainable.
Talk to Your Doctor: Armed with your symptom log, you can now have a truly productive conversation with your healthcare provider. Instead of just saying "my joints hurt," you can show them your data. This makes it much easier to discuss medical options like HRT, specific supplements, or other treatments that could be right for your menopause joint pain.
Patience and Consistency Are Key: Lasting relief doesn't happen overnight. It’s the result of showing up for yourself, day after day, with small, consistent habits. Be kind to yourself, notice the small wins, and trust that these steady actions are adding up to big improvements.
Following this simple roadmap puts you back in the driver's seat. You’ll be tackling your symptoms methodically, giving you the clarity and confidence to manage your joint pain for good.
Your Questions About Menopause Joint Pain, Answered
When new aches and pains show up during menopause, it's only natural to have a lot of questions. Let's tackle some of the most common ones I hear from women trying to make sense of what’s happening to their bodies.
Does Menopause Joint Pain Ever Go Away?
This is a big one, and the answer is a hopeful "yes, for many women." This specific kind of joint pain often settles down in the postmenopausal years once your body gets used to its new normal.
However, it's not something you should just wait out. Think of it this way: while the initial hormonal trigger might fade, the inflammation and stiffness it causes can speed up or worsen underlying conditions like osteoarthritis, which doesn't go away.
The good news is that you have a ton of influence here. Being proactive with low-impact exercise, managing your weight, and eating an anti-inflammatory diet can make a world of difference. These habits don't just ease the pain you're feeling now; they help protect your joints for the long haul.
Key Insight: Menopause joint pain doesn't have to be a permanent sentence. The healthy habits you build today are your most powerful tools for feeling better now and preventing future problems.
Can I Take HRT Just for Joint Pain?
Absolutely. If menopause joint pain is significantly impacting your quality of life, it can be a perfectly valid reason to talk to your doctor about Hormone Replacement Therapy (HRT). Since a drop in estrogen is a primary driver of the inflammation and achiness, bringing those levels back up can provide incredible relief.
Of course, HRT is a treatment that affects your whole body, and it comes with both benefits and potential risks. It’s a decision that should always be made with a healthcare provider who understands your full medical history. They can help you figure out if the pros outweigh the cons for your specific situation.
What Is the Difference Between Menopause Joint Pain and Arthritis?
It's so easy to get these two confused, but telling them apart is crucial.
Menopause joint pain, which doctors call arthralgia, feels more like a widespread soreness, achiness, and stiffness. It's that "I feel creaky all over" sensation. Crucially, it doesn't typically cause visible swelling or the kind of joint damage you'd see on an X-ray. It’s a direct response to your fluctuating hormones.
Arthritis, on the other hand, is a disease defined by inflammation inside the joint itself, leading to the physical breakdown of cartilage. That process causes pain, noticeable swelling, and a loss of mobility. While they are different, the hormonal shifts during menopause can sometimes unmask or accelerate an underlying case of osteoarthritis. The only way to know for sure is to get an accurate diagnosis from your doctor.
Ready to stop guessing and start creating a plan that works for you? Lila uses AI to translate your daily symptoms into a personalized action plan, giving you the clarity and support you need to manage joint pain and other menopause symptoms. Start your journey to relief with Lila today.
You should not have to do it all on your own










