
Panic attacks perimenopause: A guide to managing panic attacks perimenopause
Mar 13, 2026
If you've ever been blindsided by a sudden, terrifying wave of fear—your heart hammering against your ribs, your breath catching in your throat—you’re not alone. What you're experiencing is likely a panic attack. For many women in their 40s and 50s, the culprit behind these frightening episodes is perimenopause.
The hormonal upheaval during this life stage is a major reason why your body's internal alarm system can suddenly feel like it's going off for no reason at all.
Why Perimenopause Can Trigger Panic Attacks
Think of your hormones as a complex symphony orchestra that’s played in perfect harmony for decades, with estrogen as the lead conductor. Now, imagine that conductor starts acting erratically during perimenopause. One day she’s there, leading a flawless performance; the next, she’s gone, leaving the musicians in chaos.
This hormonal unpredictability is at the heart of why you might be having panic attacks. Estrogen does more than just run your menstrual cycle—it's a critical player in managing the brain chemicals, like serotonin and cortisol, that regulate your mood and how you respond to stress.
When estrogen levels swing wildly, your brain and body get mixed signals. A sudden drop can unleash a flood of adrenaline—the "fight or flight" hormone—creating the very real physical sensations of a panic attack, even when you're perfectly safe. This isn't a sign of weakness; it's a physiological response to internal chaos.
The Direct Link Between Hormones and Panic
The connection between fluctuating hormones and anxiety is well-established, but it can feel especially intense during perimenopause. In fact, a 2026 study found that 54.2% of women aged 45-70 reported experiencing anxiety, with many noting that the menopausal transition made their symptoms much worse. You can explore the full findings on anxiety prevalence during menopause to learn more.
This isn't just a vague feeling of being on edge. It’s your entire nervous system trying to adapt to a brand-new, unpredictable chemical reality.
Key Insight: A panic attack during perimenopause isn't "all in your head." It's a genuine physical reaction to the turbulent hormonal shifts your body is going through, which can throw your whole stress-response system out of whack.
To see exactly how this works, it helps to break down how these hormonal changes directly fuel panic symptoms.
Here’s a quick look at the main hormonal players and the impact they have on your body’s panic response.
How Perimenopause Triggers Panic Attacks
Hormonal Change | Resulting Impact on Panic |
|---|---|
Erratic Estrogen Levels | Disrupts mood-stabilizing neurotransmitters like serotonin, making you more vulnerable to anxiety and the sudden mood shifts that often precede a panic attack. |
Progesterone Decline | This calming, sleep-promoting hormone dwindles, leading to more restlessness, irritability, and poor sleep—all significant triggers for panic. |
Cortisol Spikes | Fluctuating hormones can signal your body to produce too much cortisol (the stress hormone), leaving you in a constant state of high alert and making it much easier to tip into a full-blown panic response. |
Adrenaline Surges | A sharp drop in estrogen can directly tell your adrenal glands to release a jolt of adrenaline, causing a racing heart, shortness of breath, and sweating—the classic signs of a panic attack. |
Just understanding these biological connections can be a powerful first step toward feeling more in control. Once you know why this is happening, you can start to find the right strategies to manage the physical sensations and calm your system down.
The Science Behind Hormonal Panic Attacks
To get a handle on why panic attacks can suddenly show up during perimenopause, we need to look at what’s going on with your hormones. For most of your adult life, estrogen and progesterone have acted like your brain’s internal balancing act, keeping your mood and stress responses on a relatively even keel.
Estrogen, in particular, has been a key player. It helps support serotonin, the neurotransmitter that acts as your built-in mood brightener. It also helps manage levels of cortisol, your body's main stress hormone. When estrogen is steady, the whole system just works.
But during perimenopause, that steady, reliable system gets thrown for a loop. Estrogen levels don't just gently taper off; they swing wildly up and down, creating the perfect conditions for anxiety and panic to take root.
The Overly Sensitive Car Alarm Analogy
Think of your nervous system as a well-calibrated car alarm. For years, it’s been set just right, only going off when there's a real threat—like someone actually trying to break into the car. This is your body's normal, healthy "fight-or-flight" response in action.
Now, imagine what happens during perimenopause. Those chaotic hormone swings are like a faulty sensor in that alarm system. A sudden dip in estrogen can trigger a flood of adrenaline and cortisol, essentially cranking the alarm's sensitivity dial all the way up.
Suddenly, the alarm is blaring for no reason at all. A gust of wind, a passing car, or just a random thought can set it off. This is precisely what panic attacks in perimenopause feel like. Your body goes into full-blown emergency mode, even if you’re just sitting on the couch or lying in bed.
This concept map breaks down that powerful chain reaction.
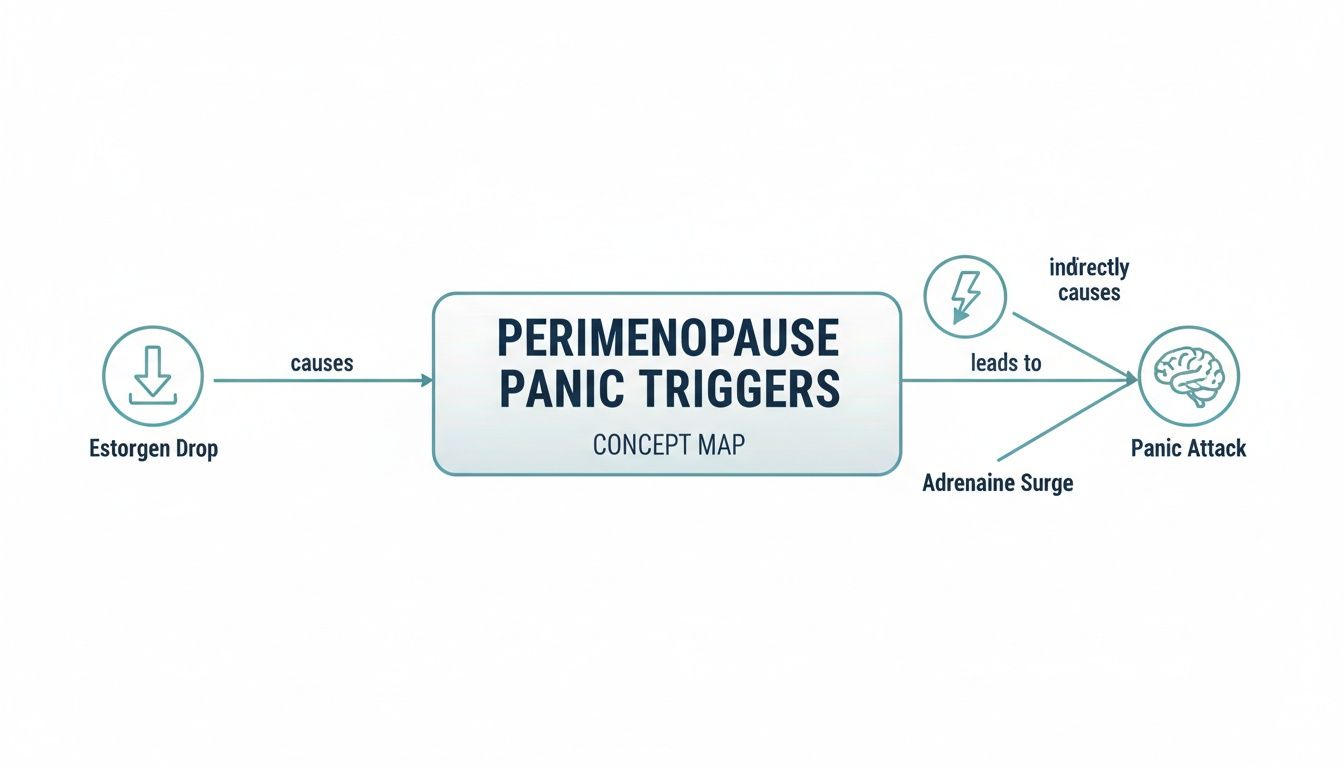
As you can see, it’s a direct biological sequence: the drop in estrogen causes an adrenaline surge, which directly results in a panic attack. It’s not a personal failing; it's physiology.
It's Not Just Estrogen: The Role of Progesterone and Cortisol
While estrogen gets a lot of the spotlight, it isn't working alone. Progesterone, often called the "calming" hormone, also starts its decline. Lower progesterone can make you feel more irritable, restless, and can seriously mess with your sleep—all of which makes you far more vulnerable to anxiety.
When both of these hormones are in flux, your body’s ability to regulate cortisol is seriously compromised. This can leave you feeling perpetually on edge, stuck in a state of high alert where your nervous system is basically primed and ready for a panic response at the slightest nudge.
Your brain and body aren't broken; they are simply reacting to a dramatic internal shift. Understanding this is the first real step toward demystifying the experience and getting back in the driver's seat.
The research backs this up. Panic attacks are known to spike during early perimenopause when the hormonal chaos is at its peak. A 2024 study noted that women in this phase reported the highest levels of stress and were more bothered by anxiety and depression than women who were pre- or postmenopausal. Other studies have found that even after the transition is complete, 17.9% of women continue to experience panic attacks, highlighting the lasting impact. You can read the full research on perimenopausal mental health to dive deeper into these findings.
Once you know the why behind these intense physical and emotional feelings, you can shift from a place of fear to a place of empowerment and start looking for the right solutions.
Recognizing Symptoms And When To Seek Help
When a sudden, crushing wave of fear hits you out of nowhere, your first thought might be, “Am I having a heart attack?” It’s an incredibly common and completely understandable reaction. The physical symptoms of a panic attack during perimenopause can be so intense that they feel terrifyingly similar to a cardiac event. Learning to tell the difference is the first step toward responding with knowledge instead of more fear.
A panic attack isn't just "bad anxiety." It's a full-body, physiological fire drill that ignites without warning and typically peaks within minutes, leaving you feeling exhausted and shaken. It can feel like your body has completely betrayed you.
Common Symptoms Of A Panic Attack
No two people experience panic attacks in exactly the same way, but they often share a cluster of hallmark symptoms. According to the American Psychiatric Association, you don't need to have all of them for it to be a panic attack, but you'll likely recognize a few from this list:
Pounding or racing heart: This is usually the first and most alarming sensation.
Sweating, chills, or hot flashes: Your body’s temperature regulation goes completely haywire.
Trembling or shaking: An uncontrollable physical reaction to the adrenaline coursing through your system.
Shortness of breath: You might gasp for air or feel like you’re being smothered.
A choking sensation: Your throat can feel so tight that it’s hard to swallow.
Chest pain or discomfort: This is the symptom that sends so many women to the ER, convinced it's their heart.
The mental and emotional side is just as powerful. Many women describe a profound feeling of derealization (where the world around you feels strange or unreal) or depersonalization (feeling detached from your own body). This is often accompanied by a deep fear of losing control or a powerful sense of impending doom.
A crucial note: The physical sensations of a panic attack, especially heart palpitations and chest pain, can feel life-threatening. If you are ever in doubt, please seek immediate medical attention. It is always better to rule out a heart condition and be safe.
Advocating For Yourself At The Doctor’s Office
It can feel daunting to walk into a doctor’s office and try to explain these episodes. But getting help is a powerful, proactive step toward getting your life back. A little preparation can make all the difference in having a productive conversation.
Before you go, try to:
Track Your Symptoms: Keep a simple log of when the attacks happen. What time was it? What were you doing? Were other perimenopause symptoms like hot flashes or poor sleep also happening? This context is gold for your doctor.
List Your Questions: In the moment, it’s easy to forget what you wanted to ask. Write down every single question you have, no matter how small it seems.
Be Specific: Instead of just saying, "I feel anxious," try describing the event. For example, "I'm having sudden episodes where my heart races, I get dizzy, and I feel a sense of terror. They last about 10 minutes and leave me exhausted."
Your doctor will likely want to run a few tests, like an EKG or blood work, to make sure nothing else is going on with your heart or thyroid. Many women discover that their heart palpitations are a common and benign part of the perimenopause journey, but it's absolutely vital to have a doctor confirm this. You can learn more in our detailed guide on menopause and heart palpitations.
Once other medical conditions are ruled out, your provider can confidently diagnose a panic disorder and start discussing a plan. Seeing a healthcare professional isn’t a weakness—it’s an act of strength. It's the first step toward managing this very treatable condition and finding your way back to a sense of calm.
Evidence-Based Treatments To Reclaim Your Calm
If you’re dealing with panic attacks during perimenopause, it's easy to feel completely alone and overwhelmed. But I want you to know there are solid, proven ways to get back in control. The key is finding the right blend of support that calms your nervous system while also addressing the hormonal shifts that are often driving the anxiety.
And getting a handle on this isn't just a 'nice-to-have'—it's becoming a critical piece of women's health. The global impact of anxiety disorders on women in perimenopause is growing, and it's a serious concern. One recent analysis projects that disability rates from anxiety in this very group could jump by over 40% by 2035. That’s a staggering number of women who are, or will be, looking for real relief. You can learn more about the projected increase in anxiety rates and what this means for public health.
This makes it more important than ever to know what actually works. When you're in the thick of it, understanding the available panic attack treatment options is your first step toward feeling like yourself again.
Therapeutic Approaches For Lasting Change
Therapy is so much more than just talking about your problems. It’s about building a practical toolkit that helps you rewire your relationship with anxiety for good.
One of the most trusted methods is Cognitive Behavioral Therapy (CBT). Think of it as a way to untangle the knot of panic. CBT works from a simple truth: our thoughts, feelings, and physical reactions are all connected. A scary thought, like "My heart is pounding, I must be having a heart attack," triggers terror, which then makes your heart pound even harder. It’s a vicious cycle.
A CBT therapist helps you spot these catastrophic thought patterns as they happen. You'll learn how to challenge them and swap them for more realistic ones, effectively stopping the panic spiral before it even gets started.
Medical Interventions To Stabilize Your System
Sometimes, your hormones are creating so much internal static that therapy alone feels like an uphill battle. That’s where medical treatments can be a game-changer, providing the stability you need for other strategies to take root.
Some of the most common and effective medical options include:
SSRIs (Selective Serotonin Reuptake Inhibitors): These antidepressants are often a go-to for a reason. They work by making more serotonin—your brain’s "feel-good" chemical—available, which helps regulate your mood and can dramatically reduce how often and how intensely panic attacks hit. They don’t just numb you to anxiety; they help correct the very brain chemistry that's contributing to it.
Hormone Replacement Therapy (HRT): For many women, the most direct path is to get to the root of the problem: hormonal chaos. HRT helps by supplementing your body's dwindling estrogen, which smooths out the wild fluctuations that can trigger adrenaline surges and panic. It’s not for everyone, so you'll need a thorough chat with your doctor about your personal and family health history to see if it's a good fit.
Your doctor might suggest other medications, but SSRIs and HRT are two of the most powerful tools for calming hormonally-driven panic.
Important Takeaway: The best results often come from a combined approach. For instance, using HRT to stabilize your hormones can make it much easier to focus on and benefit from the mental reframing techniques you learn in CBT.
Finding The Right Path For You
There’s no magic bullet here. Choosing a treatment is a team decision you make with your healthcare provider. What works brilliantly for one woman might not be the right fit for another. The best plan for you will always take into account how severe your symptoms are, your overall health, and what you feel most comfortable with.
Here’s a quick breakdown of the main paths you can take:
Treatment Type | How It Helps With Panic Attacks | Best For Women Who... |
|---|---|---|
Cognitive Behavioral Therapy (CBT) | Gives you lifelong skills to spot and change the thought patterns that trigger panic. | Want to build long-term resilience, prefer a non-medical approach, or want to use it alongside medication. |
Antidepressants (SSRIs) | Works on a brain-chemistry level to stabilize your mood, reducing the frequency and intensity of panic attacks. | Are dealing with severe or frequent panic that gets in the way of daily life and need a reliable way to get relief. |
Hormone Replacement Therapy (HRT) | Gets right to the hormonal root cause, leveling out estrogen to reduce triggers like adrenaline surges. | Have panic attacks along with other classic perimenopause symptoms like hot flashes, night sweats, or mood swings. |
Ultimately, reaching out for professional help is the strongest, most proactive step you can take. It’s the starting point for building a plan that will finally quiet the alarm bells and help you feel steady on your own two feet again.
Your Daily Toolkit For Managing Panic And Anxiety
While professional support is a cornerstone of care, the small things you do every day are what truly build your resilience against panic attacks in perimenopause. Think of it as creating a personal toolkit—a set of simple, reliable strategies you can turn to for calming your nervous system and feeling more in control.
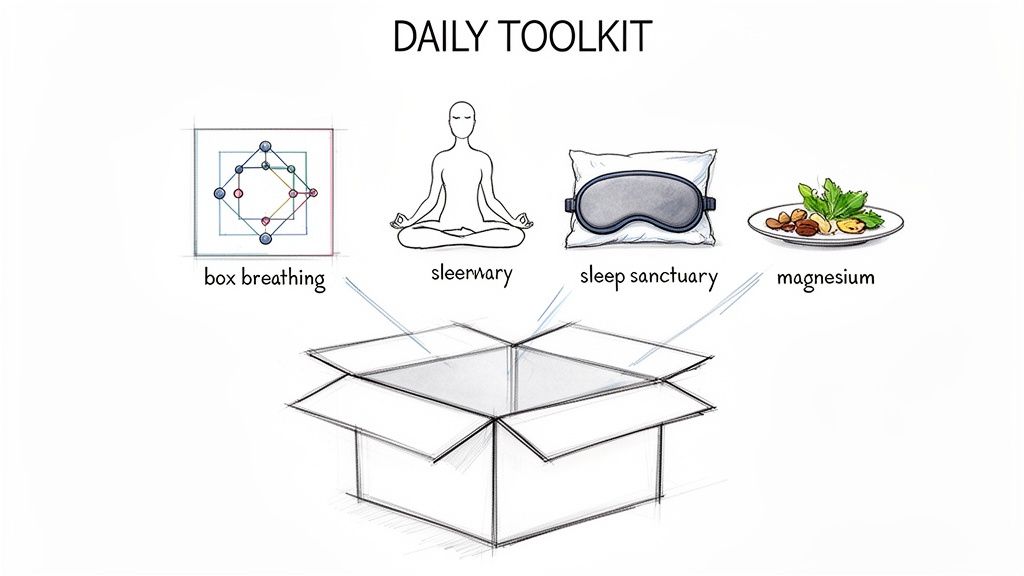
These practices aren't just for stopping a panic attack once it starts; they're about creating a lifestyle that makes your body less vulnerable to them. It’s about building a new foundation of stability, even when your hormones feel anything but stable. For more expert-led strategies, exploring these therapist-backed tips for coping with panic attacks can provide even more support.
In-the-Moment Coping Techniques
When you feel those first tell-tale signs—the racing heart, the tight chest, that sudden wave of dread—having an immediate action plan can make all the difference. These techniques interrupt the panic cycle by grounding you in the present and reminding your brain that you're safe.
Try Box Breathing: This is a surprisingly powerful breathing exercise that can quickly slow your heart rate and switch off your body’s fight-or-flight alarm.
Inhale gently through your nose for 4 seconds.
Hold your breath comfortably for 4 seconds.
Exhale slowly and completely through your mouth for 4 seconds.
Hold again at the end of the exhale for 4 seconds.
Just repeat this cycle for a few minutes. You should start to feel your body unwind.
Use the 5-4-3-2-1 Grounding Method: Panic can make you feel disconnected from reality. This sensory exercise anchors you firmly in the present moment, pulling your focus away from the internal storm.
5: Look around and name five things you can see. (e.g., a picture frame, a crack in the ceiling, a green pen).
4: Notice four things you can feel. (e.g., the texture of your jeans, your feet flat on the floor, a breeze from the window).
3: Acknowledge three things you can hear. (e.g., the hum of the refrigerator, a bird chirping, your own breath).
2: Identify two things you can smell. (e.g., the faint scent of coffee, soap on your hands).
1: Name one thing you can taste. (e.g., the lingering taste of toothpaste, or just the neutral taste in your mouth).
Long-Term Lifestyle Adjustments
While quick-relief techniques are essential, building a wellness-focused foundation is what creates lasting change. These lifestyle shifts provide direct support to your nervous system and help buffer the effects of hormonal fluctuations.
Create a Sleep Sanctuary: Restorative sleep is one of your best allies against anxiety, but hormonal shifts often disrupt it with night sweats and insomnia. It’s time to reclaim your rest.
Turn your bedroom into a cool, dark, and quiet haven.
Cut back on caffeine and alcohol, especially in the hours before bed.
Create a simple, relaxing wind-down routine, like reading a book (not on a screen!) or taking a warm bath.
Move Your Body Mindfully: Regular physical activity is a potent mood stabilizer. You don’t have to run a marathon; gentle, mindful movements can be incredibly effective. Activities like yoga, tai chi, or even a brisk walk combine physical exercise with focused breathing, which has a direct calming effect on the nervous system.
Making small, consistent lifestyle changes can have a profound impact. You might also find it useful to read our guide on managing perimenopause naturally for more ideas on holistic well-being.
Fuel Your Body for Calm: What you eat has a direct line to your brain chemistry and mood. Prioritize a diet of whole, unprocessed foods and focus on nutrients that are known to support a calm and steady nervous system.
Magnesium: Often called nature's relaxant, you can find it in leafy greens, nuts, seeds, and dark chocolate.
Omega-3 Fatty Acids: Critical for brain health, these are abundant in fatty fish like salmon, as well as walnuts and flaxseeds.
Complex Carbohydrates: Foods like oats, brown rice, and quinoa help keep your blood sugar stable, preventing the energy crashes that can often feel like or even trigger anxiety.
By weaving these strategies into your daily life, you aren't just reacting to panic—you are proactively building a more stable, resilient, and calmer version of yourself.
How Tracking Symptoms Can Uncover Your Triggers
Feeling like panic attacks during perimenopause come out of nowhere is one of the most frightening parts of the experience. It can leave you feeling powerless. But what if those episodes aren't as random as they seem?
This is where you get to put on your detective hat. By keeping a simple log of what’s happening in your body and your life each day, you can start to see connections you never noticed before. It’s not about obsessing over every little detail; it’s about spotting the patterns that give you your power back.
So, What Should You Be Looking For?
To truly understand what’s going on, you need to look beyond the panic attack itself. The real clues are often hidden in the hours or even days leading up to it. Getting a complete picture shows you exactly how different parts of your life are playing into your anxiety.
Try to make a quick note of these key areas every day:
Mood & Energy: How are you feeling, really? Jot down whether you felt irritable, on-edge, exhausted, or surprisingly calm and energized.
Sleep Quality: It’s not just about the number of hours. Did you toss and turn? Were you woken up by night sweats? Note how rested you actually feel.
Diet & Hydration: What did you eat and drink? Be honest about caffeine, alcohol, or high-sugar foods—they are very common culprits for ramping up anxiety.
Physical Activity: Did you get your body moving with a walk or some yoga, or was it mostly a sedentary day spent at a desk?
Your Cycle: If you’re still getting a period, make a note of where you are in your cycle. Many women find panic symptoms flare up right before their period starts.
A simple digital tracker can make this feel less like a chore and more like a quick, two-minute check-in with yourself.
Seeing your logs laid out visually makes it incredibly easy to spot trends. You might suddenly realize that your worst anxiety spikes almost always follow a night of broken sleep.
Over time, this data starts to tell a story. You might discover your panic attacks hit after a day with two extra cups of coffee and a stressful work deadline. Or maybe they reliably show up during the week your progesterone levels are dropping.
This information is gold. It helps you anticipate and sidestep your personal triggers, giving you a sense of control that often feels lost during the menopause transition.
Using a dedicated menopause symptom tracker app can make the whole process effortless. When you walk into your doctor's office armed with this personalized data, you can have a much more productive conversation and find solutions that work for your body, not just anybody.
Frequently Asked Questions About Perimenopause Panic Attacks
It’s completely normal to have a lot of questions when your body starts doing things that feel unfamiliar and frightening, like triggering a panic attack out of the blue. Let's walk through some of the most common concerns we hear from women navigating this phase.
Can Perimenopause Cause Panic Attacks At Night?
Yes, absolutely. Waking up in a state of panic is a surprisingly common experience during perimenopause. We often refer to these as nocturnal panic attacks.
So, what's happening? As your hormones fluctuate, the dips that happen overnight can disrupt your natural sleep patterns and trigger a sudden surge of adrenaline—that "fight or flight" chemical. It’s a jolt to the system.
On top of that, other classic symptoms like night sweats can wake you up suddenly with a pounding heart. Before you’re even fully awake, your brain tries to make sense of the sensation and can misinterpret it as a threat, spiraling you into a full-blown panic attack. This is why getting a handle on your sleep routine and winding down properly before bed is one of the best things you can do.
Will My Panic Attacks Go Away After Menopause?
For many women, the answer is a reassuring yes. Once the hormonal rollercoaster of perimenopause ends and your body settles into a new, stable normal in post-menopause, the panic attacks often ease up or stop entirely. Think of estrogen as the conductor of an orchestra; when it stops waving its baton erratically, the internal chaos finally calms down.
The catch, however, is that the experience of having panic attacks can sometimes create a learned fear. Your brain can get stuck in an anxiety loop, even after the original hormonal trigger is gone.
Important Takeaway: This is exactly why it’s so critical to build your mental toolkit during perimenopause. Learning coping skills through things like Cognitive Behavioral Therapy (CBT) doesn't just help you now—it gives you a set of lifelong strategies for managing anxiety, no matter what your hormones are doing.
Is It A Panic Attack Or A Heart Attack?
This is easily the most terrifying question of all, and it's one you should always take seriously. The physical symptoms can feel almost identical, which is why it is absolutely essential to seek immediate medical attention to rule out a heart problem. This is non-negotiable, especially the first time it happens or if you have any risk factors for heart disease.
Once a doctor has given you the all-clear and confirmed your heart is healthy, you can start to feel more confident in identifying these episodes for what they are. One of the key differences to watch for is how the symptoms progress:
A panic attack usually hits a peak of intensity within about 10 minutes before the feelings start to recede.
A heart attack is different; the symptoms tend to persist or even get worse over time.
Getting that initial medical evaluation is crucial. It not only keeps you safe but also gives you the peace of mind you need to use your coping strategies without that extra layer of fear.
Are you ready to stop guessing and start getting real answers? The Lila app combines your daily symptom tracking with a personalized plan to help you manage everything from mood swings to sleep disruption. Take back control of your perimenopause journey by visiting Lila today.
You should not have to do it all on your own










