
8 Key Exercises to Balance Hormones for Perimenopause
May 2, 2026
One day your workout feels easy and your mind is clear. Two days later, you’re wide awake at 3 a.m., sweating through the sheets, snapping at people you love, and wondering why the same routine suddenly feels draining. That whiplash is common in perimenopause. Hormones don’t decline in a neat line during this stage. They fluctuate, sometimes sharply, and your energy, sleep, appetite, mood, and recovery often fluctuate with them.
That’s why exercise for this phase has to be smarter than “just move more.” The best exercises to balance hormones don’t all work the same way. Some improve insulin sensitivity. Some help buffer stress and calm cortisol-driven symptoms. Some support estrogen-related changes in muscle, bone, and body composition. Some are useful on high-energy days. Others are better when hot flashes, bloating, or poor sleep hit hard.
The good news is that movement can do more than help you cope. Used well, it can become one of your most reliable tools for feeling steadier in your body again. The key is matching the right type of training to the effect you want, then adjusting based on what your symptoms are telling you.
If you’re in your 40s or 50s and trying to figure out what helps, start here. These are the most practical exercises to balance hormones in perimenopause, along with the mechanisms behind them, the trade-offs to watch for, and sample ways to combine them into a week that feels realistic instead of punishing.
1. Resistance Training & Strength Work
If I could pick one foundation for most perimenopausal women, it would be strength training. Not because it fixes everything, but because it affects so many of the problems that show up together in this stage: rising insulin resistance, muscle loss, lower resilience, body composition shifts, and the feeling that your body no longer responds the way it used to.
Resistance training includes dumbbells, barbells, machines, resistance bands, and bodyweight work. Squats, rows, presses, deadlifts, step-ups, lunges, and loaded carries all count. The common thread is tension on muscle, followed by recovery.
Research on women found that traditional resistance training increased estrogen by 72.3 percent, from 65 ± 33 to 112 ± 42 pg/mL, while also reducing testosterone by 49 percent and lowering FSH by 7.7 percent, with only minimal LH change, according to this study on exercise and reproductive hormones in women. That matters in perimenopause because hormonal volatility often shows up as poor sleep, low mood, stubborn fat gain, and reduced recovery.
What it helps most
Strength work is especially useful when you notice:
Blood sugar swings: You get shaky, ravenous, or crash in the afternoon.
Loss of firmness or strength: Daily tasks feel heavier than they used to.
Sleep disruption tied to stress: You’re tired but not settling well at night.
Metabolic slowdown: Your old habits don’t work the same way anymore.
The practical dose is simple. Most women do well with two to three sessions per week, focusing on major muscle groups and leaving recovery days between harder sessions. The weight training routines for women over 50 guide from Lila is a good example of how to structure that without making every workout feel like a max-effort event.
What works and what doesn’t
What works is moderate, repeatable training. Think goblet squats, dumbbell Romanian deadlifts, incline push-ups, seated rows, and split squats for 30 to 45 minutes. Keep a little in reserve instead of grinding every set.
What usually backfires is swinging between extremes. I see women do nothing for months, then jump into punishing bootcamp classes five days a week because they’re frustrated by weight gain. That often spikes fatigue, worsens soreness, and makes the whole plan feel unsustainable.
Practical rule: Lift hard enough to feel challenged, not wrecked. You should finish feeling worked, not flattened.
A good starting week might be full-body strength on Monday and Thursday, with one optional lighter session on Saturday using bands, kettlebells, or bodyweight. If sleep has been poor, reduce volume before you reduce consistency.
2. High-Intensity Interval Training (HIIT)
HIIT is powerful, but it isn’t something to scatter carelessly across the week. In perimenopause, it can be one of the best exercises to balance hormones when used in small doses. It can also be the workout style that pushes a stressed system over the edge if you’re already underslept, underfed, or running hot all day.
HIIT means short bursts of hard effort followed by recovery. That might be cycling sprints on a Peloton, rower intervals on a Concept2, hill repeats outside, or a bodyweight circuit with timed work and rest.
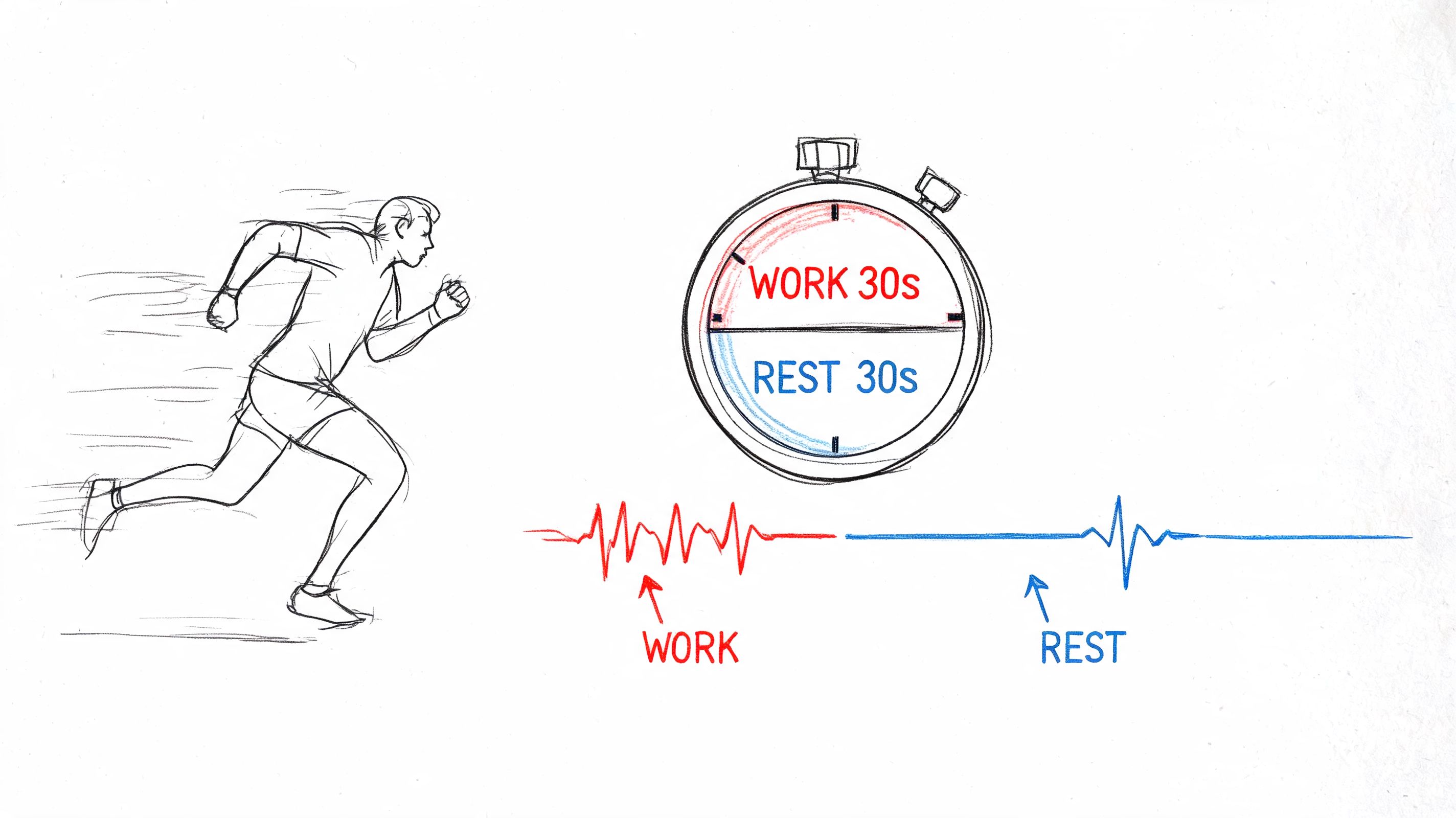
A 12-week HIIT protocol limited to 12 to 20 minutes per session, three times weekly, significantly enhanced insulin sensitivity in women with hormonal imbalances, according to this clinical overview of exercise for hormone imbalance. For women dealing with the insulin resistance pattern that often creeps in during perimenopause, that makes HIIT useful well beyond calorie burn.
The hormonal mechanism
HIIT creates a sharp demand for glucose and pushes the body to become more efficient at managing it. That’s why many women notice better energy stability when they use intervals well. It also tends to be efficient, which matters when you’re busy and already juggling poor sleep.
But the trade-off matters. More isn’t better here. If your nervous system already feels revved up, hard intervals can add to that strain. If evening workouts trigger night sweats or leave you wired, move HIIT earlier in the day or cut the intensity.
Good fit: Short sessions once or twice a week, on days you feel reasonably recovered.
Less ideal: Daily all-out intervals layered on top of strength work and life stress.
Best tools: Bike, rower, incline treadmill, swimming, or brisk hill efforts. These are easier on joints than endless jump-based circuits.
Too much intensity can look productive on paper and still be the reason you’re not recovering.
If symptoms flare after hard sessions, don’t assume exercise is the problem. The dose might be. The Lila guide to exercises to avoid during menopause can help you spot the difference between productive intensity and training that’s adding more stress.
A simple template is 6 to 10 rounds of hard work with easy recovery, capped at a session length you can bounce back from. If the workout leaves you drained for two days, scale it down. In perimenopause, recovery quality is part of the training effect.
3. Walking & Low-Impact Steady-State Cardio
You sleep badly, wake up already warm, and the idea of another hard workout feels like too much. That is often the day walking works best.
For many perimenopausal women, low-impact steady-state cardio is the most repeatable form of exercise in the week. Walking, swimming, easy cycling, hiking, and elliptical work all fit here. The pace stays moderate enough that conversation is still possible, which usually means the session supports recovery instead of adding another stress hit.
The hormonal value is specific. Steady cardio helps muscles use glucose more efficiently, which supports insulin regulation. It can also lower the total stress load compared with frequent high-intensity training, which matters when cortisol is already running high from poor sleep, work pressure, or night sweats. And because it is easier to recover from, it gives you a consistent outlet during weeks when estrogen shifts leave energy and motivation unpredictable.
That consistency matters more than people expect.
In practice, I often use walking as the anchor habit. A woman who cannot tolerate a hard evening class may still do well with a brisk morning walk, a 10 to 15 minute walk after meals, or a longer easy session on the weekend. Those sessions still count. They improve circulation, build aerobic capacity, and often help smooth out the energy crashes that make training feel harder than it should.
Why it works well in perimenopause
Walking is useful partly because the dose is easy to adjust. On a better day, that might mean a longer route or a hillier walk. On a rough week, it may mean two short walks and stopping there. Both approaches can support hormone health if they match your current capacity.
This is also where symptom patterns matter more than rigid plans. If bloating, headaches, irritability, or poor sleep spike, low-impact cardio often keeps you active without pushing you into the hole further. If you are already using symptom tracking, note how your sleep, cravings, mood, and hot flashes respond to different walking times and durations. An app like Lila can help you spot whether post-meal walks improve afternoon energy or whether longer evening walks help sleep, which makes your plan more personal and less guesswork.
How to make it useful
Treat walking as programmed training, not leftover movement.
Use post-meal walks: Even a short walk after lunch or dinner can support blood sugar handling and reduce that heavy, sleepy feeling later.
Build frequency before intensity: Add another day or another 10 minutes before you chase pace.
Use the talk test: If you can speak in full sentences, the effort is usually in the right range for steady-state work.
Match the mode to your joints and symptoms: Swimming or cycling may feel better than walking during flare-ups, pelvic heaviness, or foot pain.
Pair it with strength work: Steady cardio supports insulin and recovery. Strength training is still what best supports muscle and bone.
A practical weekly setup might look like two strength days, one short HIIT session, and three to five walking or other low-impact cardio sessions spread across the week. On high-symptom days, walking can replace a harder session without turning the week into a loss. That trade-off is often smarter than forcing intensity your body is not ready to absorb.
If stress is high and your body responds well to gentler movement, yoga for perimenopause can complement walking days and give you another lower-load option.
The biggest mistake is dismissing low intensity as low impact on hormones. For many women in perimenopause, walking is the modality that keeps cortisol more manageable, supports insulin function, and makes the rest of the plan sustainable enough to work.
4. Yoga & Mindful Movement
You sleep badly, wake up hot at 3 a.m., and your resting heart rate is higher than usual. That is rarely the best day to force intensity. Yoga and mindful movement give you a way to train with what your hormones are doing, not against them.
For many women in perimenopause, the main benefit is not calorie burn. It is better nervous system regulation. That matters because higher stress load can keep cortisol high, disrupt sleep, increase cravings, and make recovery from harder training less predictable. Slower yoga, breath-led mobility, and restorative work can help bring that stress response down enough that the rest of your plan works better.
Hatha, vinyasa, yin, and restorative yoga do different jobs. A stronger flow can improve mobility, coordination, and muscular endurance. Restorative sessions and slower breathwork are often the better call during weeks with more anxiety, poor sleep, hot flashes, or a sense that your body is already overstimulated.
One problem with standard cycle-syncing advice is that it assumes your cycle still behaves predictably. Perimenopause often does not. A discussion of exercise and hormone balance in midlife points in a more useful direction for this stage: symptom-syncing. That means choosing the session based on sleep, mood, joint pain, hot flashes, pelvic symptoms, and energy that day.
Why it helps hormones
Yoga affects hormones more indirectly than lifting or intervals, but that does not make it less useful. Its strongest role is usually cortisol management. When breathing slows, muscle tension drops, and the nervous system shifts out of a constant fight-or-flight pattern, many women notice better sleep, fewer stress spikes, and less of the wired-but-tired feeling that can make perimenopause so frustrating.
There may also be secondary benefits for insulin control. A calmer system often improves appetite regulation and recovery choices, which can make it easier to stay consistent with meals, walks, and strength work. Some women also find that gentler movement reduces symptom volatility across the month, even when cycles are irregular.
Symptom-syncing in practice
If hot flashes are strong, skip the heated class. Choose supported child’s pose, legs-up-the-wall, supine twists, cat-cow, and slow nasal breathing.
If you slept well and feel steady, a stronger flow can fit well on its own or later in the day as mobility support around strength work.
The Lila yoga for perimenopause guide is useful for this reason. It treats yoga as a tool you can match to symptoms, not a fixed identity or all-or-nothing practice.
Where yoga fits in a real week
I usually program yoga in one of three ways for perimenopausal clients: a short reset on high-stress days, a longer recovery session after harder training blocks, or a mobility-focused practice on a non-lifting day. The trade-off is straightforward. Yoga can improve recovery, sleep, and symptom control, but it does not replace the muscle and bone stimulus you get from strength training.
A practical weekly setup might be two strength days, one short HIIT or circuit session if recovery is good, three to five walks, and one or two yoga sessions adjusted to symptoms. If stress is high, yoga may need to replace intensity that week. If symptoms are calm, it can sit alongside heavier training without competing with it.
Tracking that pattern matters. In an app like Lila, log the type of yoga you did, session length, sleep quality, hot flashes, mood, and energy the next day. After a few weeks, the pattern is often clear. Restorative work may help your sleep more than evening cardio, while stronger flows may feel best earlier in the day or away from your hardest lifting sessions.
Here’s a short practice to follow along with when you need something gentle but structured:
On low-sleep days, restorative yoga often does more for hormone balance than forcing a hard workout you’ll need several days to recover from.
5. Strength Training with Metabolic Emphasis (Circuit Training)
Circuit training sits in the middle ground between pure strength work and cardio. You move through several exercises with short rest, which keeps the heart rate up while still loading muscle. For the right person, it’s efficient and motivating. For the wrong person, it becomes disguised HIIT and ends up being too much.
A smart circuit might include a squat, push, row, hinge, and core move. Think kettlebell deadlifts, dumbbell presses, TRX rows, step-ups, and carries. You can do that at home, in a gym, or in a small group class.
Why it helps hormones
This style can be useful when you want both muscle stimulus and metabolic demand in one session. That combination can support insulin sensitivity and help women who feel like long sessions aren’t realistic.
It also has a practical advantage. Many women stick with circuit training because it feels less repetitive than straight sets. Compliance matters. The best plan still has to be something you’ll follow next week.
The trade-offs
Circuit training can drift into sloppy, overheated training fast. That’s the main risk. If rest periods are too short or the loads are too heavy for the pace, form drops and recovery cost climbs.
Use this format when:
You’re short on time: A focused circuit can cover a lot in one session.
You already tolerate strength work well: Circuits work better when basic movement patterns feel familiar.
You want variety: Some women stay more consistent when the session moves.
Skip the “more sweat equals better hormones” mindset. In perimenopause, that logic can backfire. A good circuit should leave you feeling strong and energized, not dizzy and overheated.
A simple example is three rounds of five exercises with controlled transitions. Keep one or two reps in reserve on strength moves and use the clock as a guide, not a weapon. If hot flashes spike during circuits, lower density first. Don’t assume you need to quit the format entirely.
6. Pilates & Core Stabilization Work
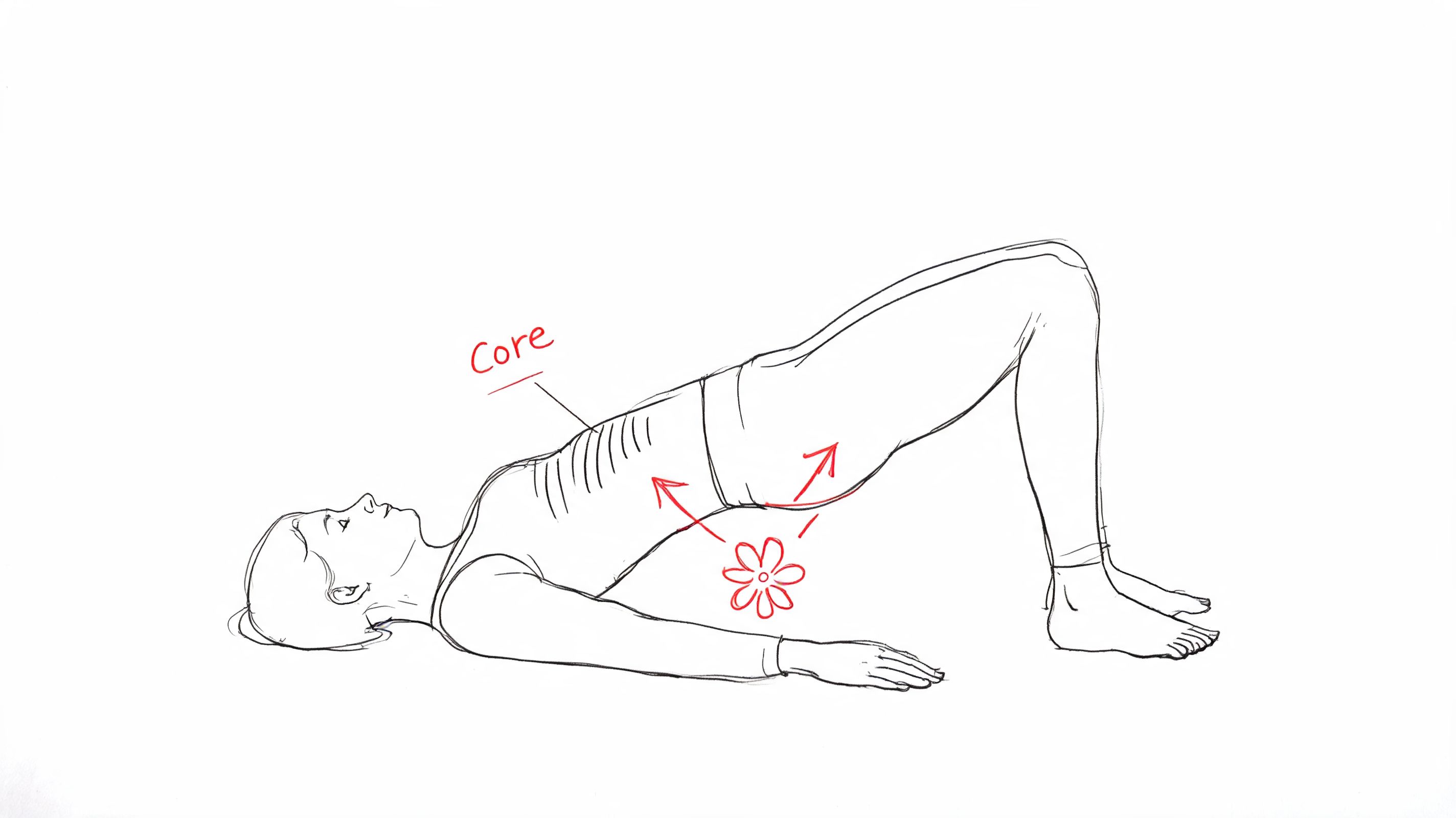
Pilates is often underestimated because it doesn’t always look intense. But in perimenopause, exercises to balance hormones don’t all need to feel hard to be valuable. Pilates can improve body awareness, breathing mechanics, posture, deep core control, and pelvic support, all of which matter more in midlife than many women realize.
That’s especially true if you’re dealing with abdominal pressure, low back tension, leaking with sneezing or jumping, or a general sense that your core doesn’t feel responsive the way it used to.
What Pilates does well
Pilates teaches control. That sounds simple, but it’s powerful. Women in perimenopause often experience a disconnect between effort and outcome. They push harder, but don’t feel better. Pilates often reverses that pattern by improving how you stack your ribcage over your pelvis, how you breathe under effort, and how you recruit the deep trunk muscles without bracing everything.
It’s also a useful bridge. If heavy strength work feels intimidating or you’re coming back from a long break, mat Pilates or reformer sessions can rebuild confidence in movement.
When it’s most useful
Pilates tends to help most when:
You’re rebuilding after inconsistency: It provides structure without a punishing recovery bill.
You have pelvic floor concerns: Breathing and pressure management matter here.
Your back, hips, or neck feel chronically tight: Better alignment can reduce “mystery tension.”
You need a recovery session that still feels productive: Pilates works well between heavier days.
The limitation is that Pilates alone usually isn’t enough for long-term muscle and bone demands in midlife. It’s best as a complement to resistance training, walking, or cycling. Think of it as quality control for how you move, not as the only thing you do.
If you’re using a reformer studio like Club Pilates or a local clinical Pilates class, look for an instructor who can modify for symptoms, pelvic floor issues, or joint pain. Good instruction matters more here than chasing the hardest class on the schedule.
7. Cycling (Indoor & Outdoor) & Lower Body Focus
Cycling is one of the most adaptable cardio options for perimenopause. It’s low impact, easy to scale, and especially useful for women who want a joint-friendlier way to train harder without the pounding of running.
You can ride outdoors, use a spin bike at home, or follow guided classes on platforms like Peloton or Zwift. The format changes, but the basic appeal stays the same: you can control effort very precisely. That matters when symptoms vary from day to day.
The mechanism and the advantage
Because cycling relies heavily on the legs, it recruits large muscle groups and creates a meaningful metabolic demand. That makes it useful for blood sugar regulation and overall conditioning. It also works across intensity zones. One day it’s an easy recovery ride. Another day it’s your interval session.
A practical example is a woman who doesn’t tolerate impact well anymore but still misses vigorous exercise. Indoor cycling often gives her a way back into that feeling of athletic effort without flaring knees, hips, or pelvic symptoms.
How to use it without overdoing it
Cycling works best when you vary the purpose of each ride.
Easy ride: Use this on a poor-sleep day or the day after lifting.
Moderate ride: Good for building aerobic capacity without excessive stress.
Harder ride: Use sparingly and recover from it on purpose.
The downside is that enthusiastic riders often start stacking too much seated cardio without enough upper-body work or mobility. That can leave you tight through the hips, stiff through the thoracic spine, and undertrained elsewhere. Pair cycling with strength training and occasional mobility work.
If you’re considering an electric option for commuting or longer outdoor sessions, this guide to e-bike types, motors, and batteries explained can help you understand the setup choices before you buy.
For women who struggle with heat sensitivity, indoor riding requires airflow. Use a fan. Ventilation isn’t a luxury in perimenopause. It can be the difference between a productive session and one that leaves you feeling awful.
8. Functional Movement & Mobility Work (Including Pelvic Floor Training)
Not every useful exercise looks like a workout. Functional movement work includes squatting, hinging, carrying, reaching, stepping, rotating, getting up and down from the floor, and improving how your joints move through those patterns. In perimenopause, this category becomes more important, not less.
Why? Because hormone shifts often show up as stiffness, aches, reduced recovery, and pelvic floor symptoms that interfere with ordinary life. If carrying groceries hurts, getting off the floor feels awkward, or you leak when you cough, your body is giving you useful information.
This is where quality of life lives
Functional work supports the things you want to keep doing. That includes lifting suitcases, gardening, hiking, playing with grandchildren, climbing stairs without knee irritation, and moving confidently when your balance feels less automatic than it used to.
Pelvic floor training belongs here too. But it’s important not to reduce that to endless Kegels. Some women need better contraction. Some need better relaxation and coordination. That’s why a pelvic floor physical therapist is often the right move when symptoms persist.
A practical approach
Use mobility and function as part of your regular training week, not as punishment after pain appears.
Before workouts: Use dynamic mobility to prepare the joints you’re about to train.
During daily life: Carry groceries evenly, practice controlled sit-to-stands, and use stairs deliberately.
For pelvic floor symptoms: Combine breathing, bridges, squats, and specialist guidance when needed.
For stiffness: Short, frequent mobility work usually beats occasional marathon stretching sessions.
If an exercise plan makes you fitter on paper but less comfortable in daily life, it needs adjusting.
This category won’t usually give you the dramatic “I crushed that class” feeling. What it gives you is more valuable. It helps your training transfer into life, and it helps life stay doable when hormones are anything but predictable.
8-Way Hormone-Balancing Exercise Comparison
Exercise Modality | Implementation Complexity 🔄 | Resource Requirements ⚡ | Expected Outcomes ⭐📊 | Ideal Use Cases 💡 | Key Advantages ⭐ |
|---|---|---|---|---|---|
Resistance Training & Strength Work | 🔄 Medium, requires coaching for safe progressions | ⚡ Moderate, weights/bands/gym or home; 2–3×/week | ⭐⭐⭐⭐, increases lean mass, bone density, insulin sensitivity; reduces hot flashes and improves sleep | 💡 Best for preserving muscle/bone and improving metabolic health during perimenopause | Builds muscle & bone; strong metabolic and symptom benefits |
High-Intensity Interval Training (HIIT) | 🔄 High, intense effort and pacing skills required | ⚡ Low–Moderate, minimal equipment; 20–30 min sessions, needs recovery | ⭐⭐⭐⭐, rapid insulin sensitivity, cardio gains, afterburn; can trigger hot flashes if too intense | 💡 Ideal for time‑pressed individuals seeking fast metabolic/cardio gains | Time‑efficient; strong metabolic and cardiovascular impact |
Walking & Low‑Impact Steady‑State Cardio | 🔄 Low, easy to implement and scale | ⚡ Low, minimal equipment; 30–60 min; can be daily | ⭐⭐⭐, reduces cortisol, improves sleep and mood; gradual fat loss | 💡 Best for sustainable daily activity, stress reduction, and gentle calorie burn | Very low injury risk; highly accessible and sustainable |
Yoga & Mindful Movement (Hatha, Vinyasa, Restorative) | 🔄 Low–Medium, different styles require alignment and breath work | ⚡ Low, mat or class; 20–90 min sessions | ⭐⭐⭐⭐, lowers cortisol, improves sleep, reduces anxiety; modest strength/flexibility gains | 💡 Ideal for anxiety, sleep issues, and parasympathetic activation | Strong mind‑body effects; excellent for stress and sleep regulation |
Strength Training with Metabolic Emphasis (Circuit Training) | 🔄 High, programming and form across exercises needed | ⚡ Moderate, mixed equipment or bodyweight; 30–45 min sessions | ⭐⭐⭐⭐, preserves muscle, boosts metabolism and cardio fitness, high calorie burn | 💡 Best for efficient full‑body conditioning and simultaneous muscle + cardio goals | Hybrid benefits: muscle maintenance plus high metabolic impact |
Pilates & Core Stabilization Work | 🔄 Medium, precision and instruction recommended | ⚡ Low–Moderate, mat or reformer; 2–3×/week | ⭐⭐⭐, improves core, posture, pelvic floor; limited cardio effect alone | 💡 Ideal for pelvic floor rehab, posture correction, and low‑impact core strength | Excellent for pelvic floor and posture; low injury risk |
Cycling (Indoor & Outdoor) & Lower Body Focus | 🔄 Low–Medium, requires bike fit and pacing awareness | ⚡ Moderate, bike or class membership; variable duration/intensity | ⭐⭐⭐, strong cardiovascular benefits and lower‑body strength; scalable intensity | 💡 Good for low‑impact cardio, leg strength, and community classes | Low joint impact; highly scalable and engaging |
Functional Movement & Mobility Work (Including Pelvic Floor) | 🔄 Medium, needs assessment and skillful progressions | ⚡ Low, minimal equipment; may need PT sessions for specifics | ⭐⭐⭐, improves daily function, balance, pelvic health; slower metabolic change | 💡 Best for restoring movement quality, preventing falls, and addressing pelvic dysfunction | Directly improves quality of life, mobility, and injury prevention |
Creating Your Personalized Hormone-Balancing Plan
The biggest mistake I see is trying to use every “good” workout at once. That usually turns into a schedule that looks disciplined for a week and feels impossible by week three. Perimenopause responds better to consistency than to bursts of intensity followed by burnout.
A better approach is to build around a few anchors. For most women, that means two or three strength-focused sessions each week, one or two higher-intensity efforts if recovery supports them, and low-impact movement such as walking on most days. Yoga, Pilates, mobility, and pelvic floor work then become strategic tools you rotate in based on symptoms, schedule, and energy.
A balanced week might look like this:
Monday: Full-body strength training
Tuesday: Walk or easy cycling, plus mobility
Wednesday: HIIT or a metabolic circuit if energy is good
Thursday: Restorative yoga or Pilates
Friday: Full-body strength training
Saturday: Longer walk, hike, or moderate bike ride
Sunday: Mobility, pelvic floor work, or full rest
That’s one template, not a rulebook. Some women do better with three shorter strength sessions. Others recover better with one HIIT session instead of two. If hot flashes spike after evening workouts, move intensity earlier. If poor sleep piles up, reduce total training stress before you decide exercise “isn’t working.”
Tracking profoundly alters your understanding. Symptom patterns in perimenopause are easy to miss when you’re relying on memory. You may feel like nothing helps, when the actual pattern is that your sleep improves after strength days, your bloating calms when you walk after dinner, or your hot flashes worsen after back-to-back hard sessions. Without tracking, those links stay fuzzy.
Using an app like Lila, you can log workouts alongside symptoms, mood, sleep, meals, energy, and cycle changes in one place. That matters because exercise doesn’t work in isolation. The same HIIT workout can feel great one week and awful the next depending on sleep, recovery, stress, and where you are in the perimenopause transition. Logging the full picture helps you see whether the issue is the workout itself or the context around it.
Over time, that gives you something more useful than generic advice. It gives you your own data. You stop asking, “What’s the best exercise for hormone balance?” and start asking, “What’s the best dose for my body right now?” That’s a much more effective question.
The same principle applies to recovery. Training adaptations happen when your body can absorb the work. If you’re always sore, sleeping poorly, or dreading sessions, your plan probably needs less intensity, more fuel, more rest, or better sequencing. This guide on optimizing muscle recovery is a useful reminder that recovery habits shape results just as much as workout choice does.
You do not need a perfect hormonal exercise routine. You need one you can sustain, adjust, and trust. Start with the basics. Build strength. Walk often. Use intensity carefully. Let yoga, Pilates, mobility, and pelvic floor work support the days when your body asks for something different. Then track what happens. In perimenopause, personalization isn’t a luxury. It’s what makes the plan work.
If you want help turning these exercises to balance hormones into a routine that fits your symptoms, Lila can make that process much easier. It combines daily check-ins with personalized action plans, symptom tracking, and an AI coach so you can connect your workouts to changes in sleep, mood, hot flashes, bloating, and energy, then adjust with confidence instead of guessing.
You should not have to do it all on your own










