
Does Low Estrogen Cause Fatigue: does low estrogen cause fatigue
Mar 16, 2026
Yes, low estrogen absolutely causes fatigue. But this isn't the kind of tired you feel after a long day. This is a bone-deep, persistent exhaustion that a good night's sleep just doesn't seem to touch.
Think of estrogen as a master regulator for your body's energy systems. When its levels begin to fall during perimenopause and menopause, several critical functions get thrown off-kilter. The result is a profound sense of fatigue that can make even simple daily tasks feel like climbing a mountain.
The Direct Link Between Low Estrogen And Fatigue
So, how exactly does this hormonal shift drain your vitality? It’s not one single thing but rather a cascade of changes that hit you from different angles. This is why menopause fatigue feels so different and frustrating—it's a complex physiological response, not just a lifestyle issue.
When estrogen was abundant, it worked quietly in the background, keeping your energy, mood, and sleep cycles running smoothly. As it declines, that smooth operation starts to sputter, leading to some very specific problems.
How Estrogen Decline Drains Your Energy
The exhaustion you're feeling isn't "all in your head." It stems from real, physical changes happening inside your body:
Sleep Disruption: Low estrogen is a notorious trigger for night sweats and hot flashes. These sudden temperature spikes can jolt you awake throughout the night, shattering your sleep cycles and preventing you from getting the deep, restorative rest your brain and body need to recharge.
Neurotransmitter Imbalance: Estrogen plays a key role in regulating brain chemicals like serotonin and dopamine, which govern mood and motivation. As estrogen dips, these neurotransmitter levels can become unstable, leading to apathy, low drive, and a mental fog that feels a lot like physical fatigue.
Metabolic Slowdown: This powerful hormone helps influence how your cells use glucose for energy. With less estrogen, your metabolism can become less efficient. Your body might also experience more low-grade inflammation, making you feel sluggish and achy.
Increased Stress Response: Estrogen helps to buffer your body's reaction to stress. Without its calming effect, your adrenal system can go into overdrive, pumping out the stress hormone cortisol. This can leave you feeling "wired but tired" and ultimately leads to burnout.
Getting a handle on these mechanisms is the first step toward reclaiming your energy. For a more comprehensive look at the various causes and solutions for this common symptom, check out our complete guide to menopause fatigue.
To put it all together, here’s a quick summary of how falling estrogen impacts your energy levels.
How Low Estrogen Drains Your Energy
This table breaks down the primary ways declining estrogen contributes to that feeling of persistent exhaustion.
Mechanism | Impact on Your Body | How You Feel |
|---|---|---|
Sleep Disruption | Reduces deep, restorative sleep and increases night sweats, leading to frequent awakenings and poor sleep quality. | Tired even after a full night in bed; often described as 'wired but tired' at night. |
Neurotransmitter Imbalance | Disrupts serotonin and dopamine, which regulate mood, motivation, and the sleep-wake cycle. | Unmotivated, emotionally drained, mentally foggy, and lacking your usual drive. |
Metabolic and Inflammatory Changes | Alters how your cells use energy (glucose metabolism) and can trigger low-grade inflammation. | Physically heavy, sluggish, and dealing with unexplained body aches. |
Increased Stress Response | Changes the rhythm of cortisol (the stress hormone), leading to adrenal strain and anxiety. | Constantly on edge, easily overwhelmed, and quickly exhausted by daily stressors. |
Each of these pathways shows how interconnected your hormonal health is with your daily energy and well-being. By understanding the root causes, you can start to address them more effectively.
The Science Behind Hormonal Fatigue
To understand why you're feeling so utterly exhausted, we have to look at what's happening under the hood. Think of estrogen as a master regulator for your brain's feel-good chemicals. It plays a crucial role in managing neurotransmitters like serotonin (your mood stabilizer) and dopamine (your motivation molecule).
When estrogen levels are steady, so is your mood and drive. But as estrogen starts to fluctuate and decline during perimenopause, it pulls the rug out from under these essential brain chemicals. The result? You can be left feeling flat, unmotivated, and foggy—a feeling that goes far beyond simple tiredness.
The Role of Partner Hormones
But estrogen isn't working in a vacuum. Its partner hormone, progesterone, is also a key player in your energy levels, primarily because of its calming, sleep-promoting qualities. Progesterone is like your body's natural wind-down signal, helping you relax and sink into deep, restorative sleep.
During perimenopause, progesterone levels often drop even before estrogen does. This drop is a major reason so many women experience that frustrating "wired but tired" feeling at night. Your body is screaming for rest, but your mind just won't shut off. This hormonal double-whammy is a huge part of why the fatigue of perimenopause can feel so bone-deep.
This diagram helps visualize how low estrogen's impact on your sleep, mood, and stress response can create a vicious cycle of fatigue.
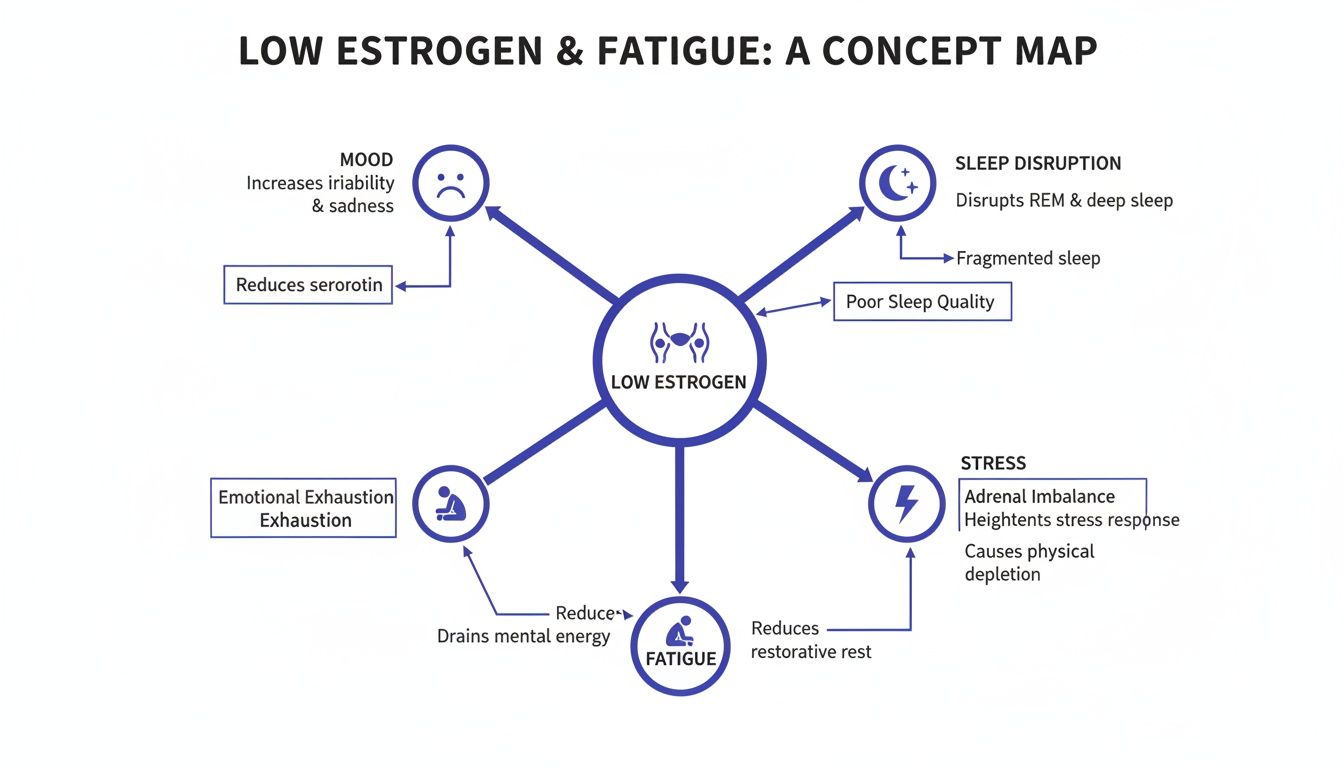
As you can see, these factors don't just add up; they feed into one another, making the overall sense of exhaustion much worse.
This isn't just a minor inconvenience; hormonal fatigue impacts over 75% of perimenopausal women. It’s a direct consequence of estrogen's decline disrupting the delicate balance of neurotransmitters that govern not just mood and motivation, but also our ability to sleep. You can discover more about the wide-reaching effects of low estrogen on AllaraHealth.com.
When you combine disrupted sleep-wake cycles and mood changes with the classic perimenopausal symptom of night sweats, you have a perfect storm for exhaustion. Add in the decline of calming progesterone, and you get those "wired but tired" nights that plague up to 60% of menopausal women.
It's also worth noting that hormones don't operate in isolation from our overall nutrition. Even trace minerals can play a supporting role. For example, looking into the benefits of boron for hormonal balance shows how specific micronutrients can influence estrogen metabolism. Understanding these connections helps you build a more complete picture of how to manage your energy.
Is It Hormonal Fatigue Or Something Else?
When that bone-deep, relentless fatigue hits, it’s only natural to point the finger at your hormones. And while the hormonal rollercoaster of perimenopause is a huge player, the exhaustion you’re feeling is often a bigger, more complicated story. Your body is an intricate system, and sometimes, several different alarms are all blaring at once.
Think of it like the dashboard of your car. That one persistent warning light might be for low estrogen, but what if the lights for low iron, thyroid function, and even stress are flickering, too? To get back on the road, you have to figure out which systems need attention. This is why learning to connect the dots between all your symptoms is one of the most powerful things you can do.
The goal here isn’t to diagnose yourself. It’s to become the lead detective in your own health story, gathering clues so you can have a truly productive conversation with your doctor.
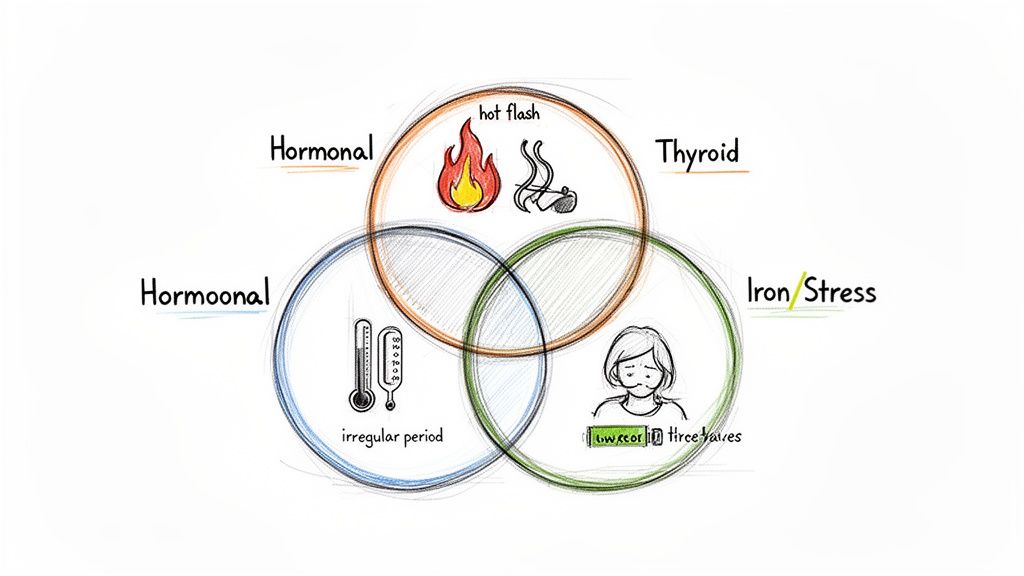
Unpacking Your Symptom Clusters
Looking at your symptoms in groups can give you some valuable hints about what’s going on under the hood. There’s definitely a lot of overlap, but paying attention to the unique combinations can help you and your provider start to narrow things down.
Hormonal Fatigue: If your exhaustion shows up with the classic signs of perimenopause—like hot flashes, night sweats, unpredictable periods, and vaginal dryness—it’s a strong signal that fluctuating estrogen and progesterone are at the heart of the issue.
Thyroid Issues: Is your fatigue paired with feeling cold all the time, unexpected weight gain, constipation, dry skin, or thinning hair? Hypothyroidism can mimic perimenopause symptoms and often develops around the same time in a woman's life, which makes a thyroid check absolutely essential.
Iron Deficiency (Anemia): This kind of fatigue often leaves you feeling winded or breathless after just minor exertion. Other tell-tale signs are pale skin, dizziness, and chilly hands and feet. The heavy, flooding periods common in perimenopause can put you at a much higher risk for iron deficiency.
Chronic Stress & Adrenal Strain: When your fatigue is tangled up with anxiety, a feeling of being constantly "wired," digestive problems, and sleep disruptions (especially waking up between 2-4 AM), your body might be struggling with chronically high levels of the stress hormone cortisol.
Think of tracking your symptoms less like logging data and more like keeping a personal journal. When you use an app like Lila to note your energy, mood, and physical feelings each day, you start to see a story emerge from the noise.
This detailed record is what helps you separate a purely hormonal fatigue pattern from one that’s made worse by other factors. You might notice, for example, that your exhaustion craters right before your period starts or that it skyrockets after a week of high stress. These are the exact insights that empower your doctor to look beyond the obvious and find the real root of your low energy.
How Doctors Diagnose Estrogen-Related Fatigue
Walking into your doctor's office and just saying "I'm exhausted" can feel like a dead end. When you're bone-tired, it's hard to find the words to explain what's happening. The good news is, an experienced clinician knows that fatigue isn't just one thing, and they have a method for figuring out if shifting hormones are to blame.
It all starts with a conversation. Your doctor’s job is to look beyond the word "tired" and understand the texture of your fatigue. Is it a physical heaviness that makes your limbs feel like lead? Or is it a mental fog that makes it impossible to concentrate? This chat is the first, and most critical, step.
Starting with Your Story
Think of your doctor as a detective. Your personal health story—all the details you share—provides the essential clues they need to start solving the mystery of your fatigue. They're looking for a specific pattern that points toward perimenopause.
Be ready to talk about a few key things:
Symptom Timing: Did this exhaustion hit you out of the blue? Does it feel worse right before your period or after a particularly stressful week?
The Usual Suspects: Are you also dealing with other telltale signs like hot flashes, night sweats, brain fog, or unpredictable periods? When fatigue shows up with this crew, it's a huge clue.
Sleep Sabotage: How are you actually sleeping? Waking up multiple times a night or finding yourself drenched in sweat is a recipe for daytime exhaustion.
Your symptom story provides crucial context that a simple blood test can't. Think of it as the map your doctor uses to navigate the diagnostic journey. The more detail you can provide, the clearer the path becomes.
Using Lab Tests for Clues
While your story directs the investigation, your doctor will likely order some bloodwork. This isn't to give you a single "yes" or "no" answer, but to gather more evidence and rule out other culprits that could be masquerading as hormonal fatigue.
Common lab tests include:
Hormone Levels: A blood test can measure your estradiol (the most active form of estrogen) and Follicle-Stimulating Hormone (FSH). A consistently high FSH level is a strong indicator that your ovaries are winding down estrogen production.
Thyroid Panel: An underactive thyroid (hypothyroidism) is a master of disguise, with symptoms that overlap almost perfectly with perimenopause. Checking your thyroid function is non-negotiable.
Complete Blood Count (CBC): This test spots anemia (low iron), a very common cause of deep fatigue, especially for women who experience heavy menstrual bleeding.
Vitamin D and B12: Deficiencies in these key nutrients are notorious for causing profound physical and mental exhaustion.
It's really important to know that your hormone levels can swing wildly from one day to the next during perimenopause. A single "normal" estrogen result doesn't mean your hormones aren't the problem. For this reason, most doctors weigh your overall symptom pattern much more heavily than a single lab number. If you'd like to understand this better, our guide on how to test for menopause explains this in more detail.
By weaving together the threads of your personal health story with targeted lab results, your doctor can get a clear picture, determine if low estrogen is driving your fatigue, and start building a plan to get your energy back.
How to Get Your Energy Back
Knowing why you feel so tired is the first step. Now, let’s talk about what you can actually do about it. Getting your energy back when hormones are the culprit isn’t about finding one quick fix; it's about building a smart, personalized plan that tackles the problem from every angle.
Think of it as creating your own Energy Plan, combining daily habits with the right medical support to get to the root of your exhaustion.
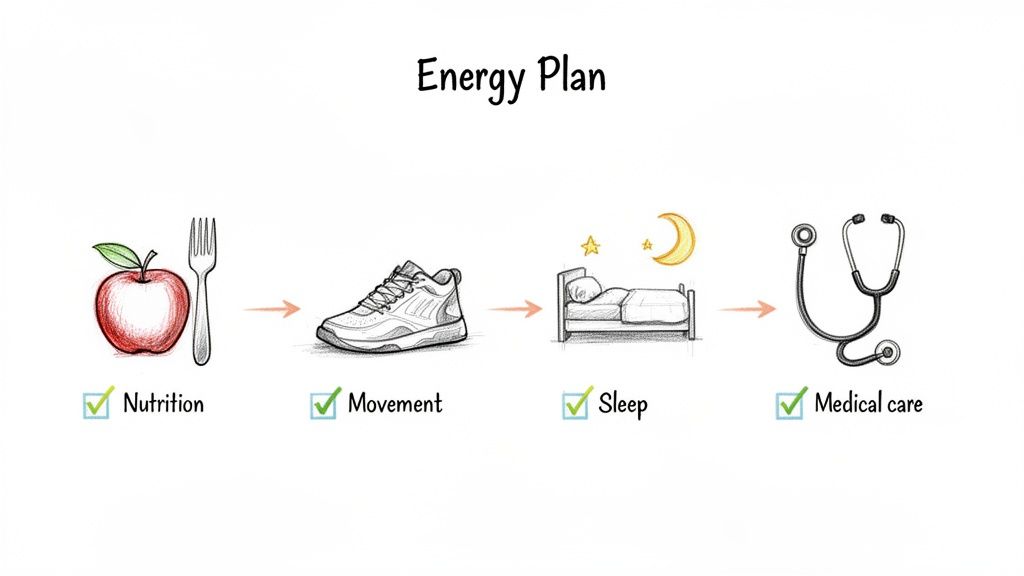
It’s these small, strategic changes working in concert that will truly restore your sense of vitality.
Eat to Beat Fatigue
What’s on your plate directly influences your hormones and energy. As you go through perimenopause, your body's ability to handle blood sugar changes, making you much more susceptible to those awful energy slumps. This makes a balanced diet one of your best defenses.
Here’s where to focus your nutritional efforts:
Make Protein a Priority: Including a good source of protein with every meal helps keep your blood sugar stable and maintains muscle mass, which is a big deal for your metabolism.
Fill Up on Fiber: Think vegetables, fruits, and whole grains. Fiber is your friend because it slows down digestion, helping you avoid the sharp glucose spikes and crashes that feed fatigue.
Factor in Healthy Fats: Foods rich in Omega-3s, like salmon, are fantastic for fighting inflammation—a hidden factor that can make you feel sluggish and drained.
Move to Make Energy, Not Lose It
When you're running on empty, the thought of a workout can seem laughable. But here's the paradox: the right kind of movement actually creates energy. The trick is to avoid pushing yourself so hard that your cortisol levels spike, which will only leave you feeling more depleted.
Instead of grueling, high-intensity sessions, try weaving in these types of movement:
Strength Training: As estrogen drops, holding onto muscle is critical. Simple bodyweight exercises, resistance bands, or light weights are great for improving how your body uses fuel.
Moderate Aerobic Exercise: A brisk walk, a bike ride, or a swim can do wonders for your mood and sleep, boosting your daytime energy without putting extra stress on your body.
Fatigue is a dominant symptom for women, particularly during the perimenopausal years. It’s not just a feeling; it’s a measurable phenomenon that can be tracked and managed.
For many, medical support is a key piece of the puzzle. Treatments like Hormone Replacement Therapy (HRT) can be incredibly effective by directly addressing the low estrogen that causes fatigue and other symptoms, offering significant relief.
Prioritize Sleep to Break the Cycle
Poor sleep and hormonal fatigue are locked in a vicious cycle—one causes the other. To break free, you need to get serious about your sleep hygiene, which just means your environment and routines around bedtime. This includes creating a cool, dark, and quiet bedroom to help with night sweats and establishing a consistent wind-down routine that tells your body it's time to rest. You can find more expert tips in our guide to finding relief from menopause fatigue.
This isn't just in your head. A major national survey found that 57.7% of people struggle with fatigue, but it hits women much harder—64.7% report feeling tired. The gap is even wider for high-frequency fatigue, impacting 20.7% of women compared to just 11% of men. For the 35,000+ women using apps like Lila, tracking energy with daily check-ins helps connect these dots, providing a clear picture of how their cycles and symptoms are linked, as noted in the Midlife in the United States study findings.
Your Questions About Hormonal Fatigue, Answered
When you’re dealing with fatigue during this stage of life, it’s natural to have a lot of specific, personal questions. Let's tackle some of the most common ones I hear from women trying to make sense of their energy levels.
How Quickly Can You Feel Fatigued From Low Estrogen?
Fatigue from declining estrogen isn't usually like flipping a switch. For most women in perimenopause, it’s a slow burn—a gradual, steady decline in energy that builds over months. You might notice a deep exhaustion that a full night's rest just can't seem to fix.
That said, it can also hit more suddenly. This often happens after an event that causes a sharp hormonal drop, like having your ovaries removed. The defining feature, whether it's gradual or sudden, is that the exhaustion just sticks around.
Will My Energy Levels Return To Normal After Menopause?
Many women do find their energy improves once their bodies settle into the new, stable state of lower estrogen after menopause. This is often because the most disruptive symptoms, like night sweats and unpredictable periods, have finally stopped.
However, since estrogen has a long-term effect on things like your metabolism and mood, just waiting for menopause to be "over" isn't a complete strategy. Maintaining that vitality for the long haul really comes down to building proactive, healthy habits.
While the answer to "does low estrogen cause fatigue" is a definite yes, the path back to feeling like yourself is unique. The most powerful thing you can do is build sustainable habits that support your new normal.
Can I Boost Estrogen Naturally To Fight Fatigue?
You can't eat your way back to your pre-menopausal estrogen levels, but you can absolutely support your body's hormonal ecosystem through lifestyle.
Focusing on things you can control makes a huge difference. Adding phytoestrogen-rich foods like flaxseed to your diet, getting a handle on stress to lower cortisol, and maintaining a healthy weight all help soften the impact of low estrogen and can significantly boost your overall energy.
If you're ready to go from just understanding your fatigue to actively managing it, Lila can guide you. Our app uses your daily check-ins to create a personalized plan to help you regain control over your energy, sleep, and mood. Take the first step and get your plan today at getlila.com.
You should not have to do it all on your own










