
How to Reduce Hot Flashes at Night A Practical Guide
Apr 25, 2026
Waking up hot, damp, irritated, and suddenly wide awake can make the whole night feel lost. You throw off the covers, then get chilled. You flip the pillow. You crack a window. You finally drift off, only to be jolted awake again an hour later. By morning, you’re exhausted and wondering which tip is supposed to work.
Nighttime hot flashes are common, but common doesn’t mean simple. The mistake I see most often is treating them like they have one universal fix. Someone cuts out coffee and feels no change. Someone else buys cooling sheets and still wakes up sweating. Another person notices a big difference just by changing bedtime habits. That doesn’t mean one person is doing it right and another is failing. It means hot flash patterns are often personal.
That’s why the most useful approach isn’t a random list of menopause tips. It’s a personalized relief plan. Common triggers like alcohol, spicy food, stress, and warm rooms matter, but hot flash patterns are highly individualized, and keeping a symptom diary or using a tracking app can help identify when symptoms happen and what combinations set them off, as noted by Summa Health’s guidance on tracking hot flash patterns.
If you want to know how to reduce hot flashes at night, start with two truths. First, your body isn’t being dramatic. There’s a real biological reason this is happening. Second, relief usually comes faster when you stop guessing and start observing patterns. The women who make the most progress are rarely the ones trying the most things at once. They’re the ones who test changes methodically and notice what their own body does in response.
Introduction Finding Your Way Through the Heat
A lot of women come to this problem feeling defeated. They’ve already tried sleeping with one foot out of the blanket, lowering the thermostat a little, or avoiding a few obvious foods. When those quick fixes don’t solve it, it’s easy to assume nothing will.
That’s usually not true. What’s more often true is that the strategy is too general.
A hot flash at night might be tied to room temperature, but it might also be stress from the day, alcohol with dinner, a too-warm mattress, late exercise, or a pattern that only shows up when two or three factors happen together. Some women react strongly to a single trigger. Others only have symptoms when stress combines with a warm bedroom or when poor sleep builds over several nights.
Practical rule: Don’t ask, “What helps hot flashes?” Ask, “What lowers my nighttime episodes most reliably?”
That shift matters. It changes the goal from collecting menopause advice to building a system. Instead of trying six new things in one week, test one or two changes and track what happens. Note your bedtime, room feel, alcohol, caffeine, stress, exercise, and whether you woke flushed, drenched, or anxious. Patterns often become clearer than expected once they’re written down consistently.
A personalized approach also helps you avoid wasting energy on fixes that sound appealing but don’t move the needle for you. Good management is less about perfection and more about pattern recognition. Once you know your triggers, your routine gets simpler. You stop doing everything. You start doing what works.
Understanding Night Sweats and Your Personal Triggers
Hot flashes at night usually feel random, but they’re not coming out of nowhere. Menopause changes the way the body handles temperature regulation. The simplest way to explain it is this: the brain’s internal thermostat becomes more sensitive. A small shift in body temperature that used to pass unnoticed can now trigger sweating, flushing, and a jolt of wakefulness.
The faulty thermostat problem
That thermostat sits in the hypothalamus. When estrogen levels fluctuate or decline, temperature regulation becomes less steady. The body can overreact to normal changes. You may suddenly feel overheated even if the room isn’t objectively hot.
That’s why night sweats can feel so dramatic. Your body acts as if it needs emergency cooling. Blood vessels widen, sweating starts, and then many women feel chilled afterward once the sweat evaporates and the bedding cools.
The frustrating part is that the trigger isn’t always obvious in the moment. What woke you at 2 a.m. may have started with what happened at 6 p.m.
The trigger categories worth watching
Instead of memorizing a giant list, sort triggers into a few buckets. That makes them easier to test.
Food and drink triggers
Alcohol near bedtime: For some women, even a modest evening drink can set up a warmer night. If this seems likely for you, it’s worth reading more about the connection between alcohol and hot flashes.
Caffeine later in the day: Some women tolerate morning coffee well but react to afternoon or evening caffeine.
Spicy meals: These can mimic or intensify the body’s heat response.
Very hot drinks or heavy late meals: If your body is already running warm, these may push it further.
Environmental triggers
Warm bedroom air: A room that feels comfortable at bedtime may feel too warm at 2 a.m.
Heat-trapping bedding: Thick duvets, synthetic sheets, and foam-heavy sleep surfaces can hold warmth.
Tight or non-breathable sleepwear: If fabric can’t release heat and moisture, symptoms often feel worse.
Hot showers or baths close to bed: Some women love them for relaxation but sleep warmer afterward.
Lifestyle and body-state triggers
Stress: Many women notice more nighttime episodes after tense, overloaded days.
Smoking: Tobacco use is linked with increased hot flash risk, so quitting can be part of symptom relief.
Weight-related factors: Extra body heat retention can make nighttime symptoms harder to manage.
Poor sleep itself: Once sleep gets fragmented, the body often becomes more reactive the next night too.
How to identify your pattern without overcomplicating it
You don’t need an elaborate spreadsheet. You need consistency. For the next couple of weeks, track:
What time you went to bed
What you ate and drank in the evening
Whether you felt stressed, wired, or calm
How warm the room and bedding felt
Whether the episode woke you sweating, flushed, anxious, or chilled afterward
Some women don’t react to one trigger alone. They react when stress, warmth, and a late glass of wine stack up on the same night.
That’s where personalized tracking matters most. Generic menopause advice can tell you what might matter. Your notes show what does matter in your life.
Build Your Cool and Calm Sleep Sanctuary
The bedroom should work for you, not against you. If your sleep environment traps heat, every other strategy has to fight uphill. The goal isn’t making the room icy. It’s creating a setup that helps your body release heat quickly and recover fast if a flash hits.
Set the room up for heat release
Experts recommend keeping the bedroom at 60-67°F (15-19°C) to support the body’s natural nighttime cooling pattern, and combining that with breathable bedding made from natural fibers like cotton or linen to reduce sleep disruption from night sweats, according to the National Institute on Aging’s menopause guidance.
That temperature range surprises a lot of women because many bedrooms are warmer than that. If your room tends to hold heat, start by lowering the thermostat a bit more than you normally would and run a fan for airflow. If you don’t control the central air, use window ventilation when weather allows or cool the room before bed.
Don’t ignore the mattress and bedding. A hot room is obvious. Heat trapped under your body is quieter and often just as disruptive.
Choose fabrics that help instead of trapping sweat
The best sleep setup for night sweats is usually simple.
Use cotton or linen sheets: Natural fibers breathe better and tend to feel less swampy during a sweat episode.
Wear loose sleepwear: The goal is air movement, not insulation.
Build layers you can move quickly: A light blanket plus an extra layer works better than one heavy comforter.
Keep a towel or spare top nearby: If you wake up damp, a fast change helps you settle sooner.
If you’re shopping for bedding, look for cooling bedding options that prioritize breathability and moisture control rather than thick plush warmth. Marketing language can be noisy, so focus on practical features you can feel at night.
A layered bed is especially useful because it lets you make small changes without fully waking yourself up. Pull one layer off. Turn the pillow. Shift to the cooler side of the bed. Those small adjustments matter when you’re trying to fall back asleep quickly.
Build a short cooling routine before bed
A good nighttime routine for hot flashes isn’t about doing more. It’s about reducing the heat load you carry into bed.
Try a simple sequence:
Cool the room before you get under the covers.
Drink a little cold water before bed if that feels comfortable for your bladder and sleep.
Take a lukewarm shower instead of a hot one.
Avoid heavy blankets at the start of the night.
Keep a fan, water, and dry sleepwear within reach.
The goal is to reduce friction. When a flash happens, you shouldn’t need to search the house for relief.
If disrupted sleep is part of the bigger picture, this guide on sleeping better during perimenopause can help you think beyond cooling alone and look at the whole bedtime setup.
Here’s a visual walk-through that can help you think through your bedroom setup and airflow choices:
What usually doesn’t work well
Some fixes sound smart but backfire.
Approach | Why it often falls short |
|---|---|
One very cold heavy blanket | You may cool quickly, then overheat again because heat gets trapped |
Synthetic satin-feel sheets | They can feel slick but still hold heat and moisture |
A hot bath right before sleep | Relaxing, yes. Cooling, usually not |
Turning the room cool but wearing thick pajamas | Clothing can cancel out the benefit |
The best bedroom for menopause sleep is adjustable. You want fast, low-effort ways to cool down without fully waking up.
That’s the benchmark I use in practice. Not perfect comfort every minute. Better recovery after each interruption.
Strategic Daily Habits for Fewer Nightly Interruptions
What happens in the bedroom matters. What happens all day matters too. Night sweats often become easier to manage when daily habits lower baseline heat, stress, and symptom sensitivity.
Women often get stuck in all-or-nothing thinking. They assume they need a strict diet, a punishing workout plan, or a shelf full of supplements. Usually, the best results come from steadier, more boring habits.

Food and drink choices that shape the night
Lifestyle changes are a core part of symptom management. The North American Menopause Society highlights that weight loss in overweight women can improve hot flash frequency, studies link smoking cessation to fewer and less severe episodes, and avoiding triggers such as alcohol and spicy foods before bed is widely recommended in the review on nonhormonal management of menopausal symptoms.
That doesn’t mean every woman needs to eliminate every suspected trigger forever. It means evening habits are worth testing carefully.
A useful way to think about dinner and evening intake:
Alcohol may relax you at first, but for some women it sets up a warmer, more fragmented night.
Spicy meals can be fine at lunch and a problem at night.
Caffeine may not trigger a flash directly, but it can raise alertness and worsen the experience of waking.
Large late meals can leave you feeling internally hot when you’re trying to cool down.
Weight, movement, and smoking
Weight management gets discussed in menopause in a way that can feel shaming. It shouldn’t. The more practical point is that metabolic health and symptom control often overlap. If a woman is overweight, even gradual weight loss may help reduce hot flash frequency. Not because she has failed, but because the body often handles temperature and sleep better with less metabolic strain.
Exercise helps too, but timing matters. If intense evening exercise leaves you flushed for hours, it may be a poor fit for now. Moderate movement earlier in the day is often easier to tolerate.
Smoking is a clearer issue. If you smoke, quitting is one of the smartest symptom-management steps you can take, both for hot flashes and for long-term cardiovascular health.
Supplements need a reality check
Many women ask about black cohosh, magnesium, evening primrose oil, soy products, and sleep blends. Some find them helpful. Some notice no difference. The important point is not to treat over-the-counter products as automatically gentle or risk-free.
Use this filter before you buy:
Do I know what symptom I’m trying to target?
Am I starting one new thing at a time?
Have I checked whether it fits my health history and medications?
That last question matters more than people realize. Herbal doesn’t mean harmless. “Natural” doesn’t mean appropriate for every body.
A supplement should earn its place in your routine. If you can’t tell whether it’s helping, don’t keep stacking products and hoping for the best.
Keep the whole day cooler, not just the bedroom
If your home runs warm overall, the evening may begin with your body already overheated. In that case, broader cooling strategies can help. This practical guide on how to cool a room without AC can give you useful ideas for airflow and heat control beyond the bedroom itself.
One tool that can make this process less messy is Lila, which tracks symptoms alongside sleep, meals, mood, energy, and cycles so you can spot whether a rough night followed alcohol, stress, late eating, poor sleep timing, or something less obvious. That kind of centralized tracking is often more useful than memory, especially when symptoms vary from week to week.
A realistic daily rhythm
Here’s the pattern I tend to recommend first:
Part of day | Better bet |
|---|---|
Morning | Caffeine earlier rather than later, and hydrate consistently |
Afternoon | Movement that doesn’t leave you overheated at bedtime |
Evening meal | Lighter, less spicy, less alcohol-heavy if nights are rough |
Late evening | Wind down instead of stacking heat, stress, and stimulation |
You don’t need a perfect routine. You need one that lowers the chance of carrying heat and tension into the night.
Train Your Brain to Manage Hot Flashes
Most women are never told this part: even when you can’t stop every hot flash, you can reduce how much it wrecks the night. That’s not “thinking positive.” It’s learning how to interrupt the spiral of heat, panic, frustration, and full wakefulness.
When a woman starts dreading bedtime because she expects another sweaty wake-up, the nervous system gets involved. The body isn’t just reacting to temperature anymore. It’s reacting to anticipation.

What CBT actually helps with
Cognitive Behavioral Therapy, or CBT, is endorsed by the North American Menopause Society. It doesn’t reduce hot flash frequency, but it can reduce the distress they cause. Mayo Clinic notes that 4-6 sessions can lessen hot flash “bother” and improve sleep and mood in the Mayo Clinic overview of hot flash treatment.
That distinction matters. A lot of women dismiss CBT because they think, “My symptoms are physical.” They are physical. CBT doesn’t deny that. It changes the layer of suffering added by thoughts like:
“I’m never going to sleep again.”
“Tomorrow is ruined.”
“I can’t cope with another one.”
Those thoughts raise alarm. Alarm makes it harder to settle. CBT helps replace that reaction with something steadier and more accurate.
A calmer response in the moment
When a hot flash wakes you, try this sequence:
Name it clearly: “This is a hot flash. It will pass.”
Cool first, don’t catastrophize: Move the blanket, use the fan, sip water.
Keep the mind quiet: Avoid checking the clock if that tends to stress you.
Let the body come down before problem-solving: Night is not the time to analyze your whole menopause plan.
This sounds simple, but it’s powerful. The body settles faster when the brain doesn’t keep shouting danger.
You don’t have to like the hot flash to respond skillfully to it.
Paced breathing and mindfulness
Mind-body techniques aren’t fluff when they’re done consistently. Paced breathing at 5-8 breaths per minute can help quiet the stress response. So can a short daily mindfulness practice. These tools are most useful when practiced before you desperately need them.
Try this before bed:
Inhale gently
Exhale slowly
Keep the breath smooth, not forced
Continue for several minutes
A brief meditation, body scan, or guided relaxation can work the same way. Not because it cools the room, but because it lowers the arousal that often magnifies the disruption.
When outside support helps
Sometimes the distress around symptoms becomes its own problem. If night sweats are feeding anxiety, irritability, relationship strain, or ongoing sleep fear, structured support can help. Some women benefit from menopause-focused CBT resources, while others may want broader professional counselling support to work on stress, sleep anxiety, or coping skills.
That’s not a sign that symptoms are “all in your head.” It’s a practical step when your nervous system has been on alert for too long.
When to Consider Medical and Over-the-Counter Options
If you’ve adjusted your bedroom, cleaned up evening triggers, and built a steadier routine but you’re still waking up drenched and depleted, it may be time to move beyond self-management alone. Medical treatment is not a failure. It’s often the right next step.
A lot of women wait too long because they think they should push through. There’s no prize for suffering through severe night sweats when effective treatment exists.
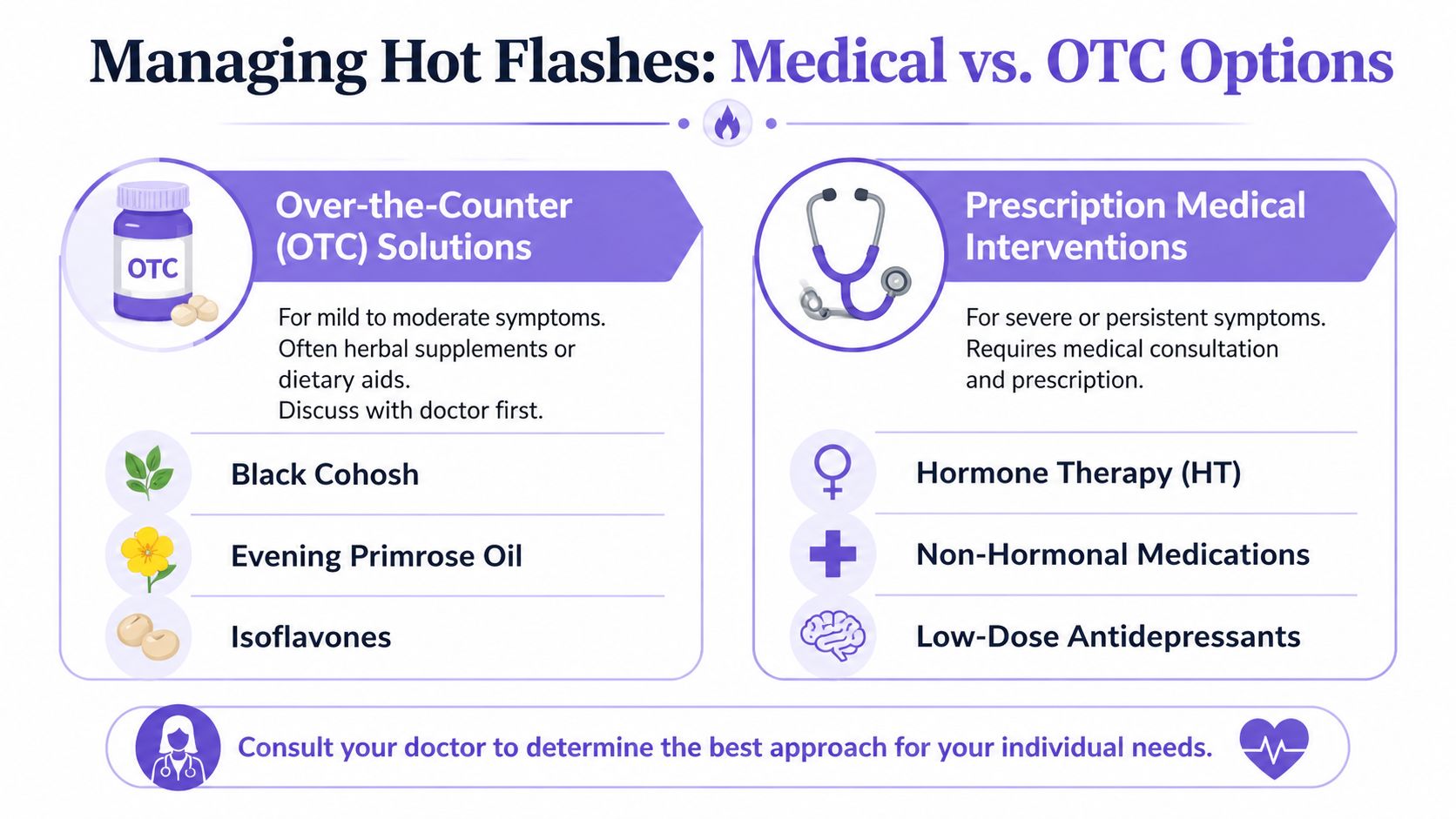
The main options side by side
Menopause Hormone Therapy, or MHT, is the most effective treatment for vasomotor symptoms. It can reduce hot flash frequency by up to 80% and severity by 75% in responsive patients, and non-hormonal prescription options such as SSRIs, SNRIs, and gabapentin can also provide significant relief, as described by UCLA Health’s review of menopause symptom treatment.
Here’s the practical comparison:
Option | Best fit | Main upside | Main trade-off |
|---|---|---|---|
MHT | Women who are appropriate candidates and want the most effective symptom relief | Strongest symptom reduction | Not right for everyone, especially some women with cardiovascular or other risk factors |
SSRIs or SNRIs | Women who can’t or don’t want to use hormones | Helpful non-hormonal option | Side effects and medication fit need review |
Gabapentin | Women whose worst symptoms are at night | Can be especially useful for nocturnal hot flashes | Can cause drowsiness or other side effects |
OTC supplements | Women with mild symptoms who want to try a nonprescription route | Easy to access | Evidence is mixed, quality varies, and interactions matter |
MHT and who should ask about it
For many women, MHT is the treatment that changes the game. If your night sweats are frequent, your sleep is suffering, and you don’t have contraindications, it deserves a real discussion with a clinician. This is especially true when symptoms are affecting your ability to function during the day.
That said, MHT isn’t “for everyone” and it isn’t something to start casually based on a friend’s experience. Your personal history matters. So does timing in relation to menopause onset.
Questions worth bringing to your appointment:
Am I a good candidate for MHT based on my history?
What form would make sense for my symptoms?
What risks matter most in my case?
How will we know whether it’s helping?
Non-hormonal prescriptions for nighttime symptoms
If hormones aren’t a fit or aren’t your preference, there are still strong options. Certain SSRIs and SNRIs can reduce hot flash burden. Gabapentin is often especially relevant when nighttime symptoms are the main complaint.
That distinction matters because not every treatment is equally helpful for every pattern. A woman with all-day symptoms may make a different choice than a woman whose main problem is waking multiple times soaked and unable to get back to sleep.
Over-the-counter products and how to use caution
Many women start with supplements because they’re easy to buy and don’t require an appointment. That’s understandable. But they should still be approached like real interventions, not harmless add-ons.
You’ll see products marketed for menopause support that include herbs, soy-derived compounds, minerals, or mixed formulas. Before trying them, it helps to review a balanced guide to menopause supplements and how to assess them.
Keep these points in mind:
Take one new product at a time
Give it enough time to assess, but not forever if there’s no clear benefit
Check for medication interactions
Bring the actual bottle or ingredient list to your clinician if possible
When to see a clinician sooner
Don’t wait if:
Night sweats are severe enough that sleep loss is affecting work, mood, or safety
You’re unsure whether the sweating is menopause-related
You have a medical history that could affect treatment choice
You’ve tried several lifestyle steps without meaningful relief
You’re considering hormones or combining multiple OTC products
If your nights are repeatedly broken and your days are unraveling, it’s time for a treatment conversation, not more guesswork.
Good care is collaborative. The goal isn’t for a clinician to hand you one generic answer. It’s to match the treatment to your symptom pattern, health history, and preferences.
Conclusion Building Your Personalized Action Plan for Better Nights
The most effective way to approach nighttime hot flashes is to stop treating them like a mystery you’re supposed to endure. They respond best to a clear process. Cool the environment. Reduce obvious evening triggers. Support your nervous system. Consider medical treatment when symptoms are too disruptive to manage with habits alone.
Above all, keep it personal.
A strategy that works beautifully for one woman may do very little for another. That’s why the strongest plan is usually built through testing, tracking, and adjusting. Notice when symptoms happen. Look for combinations rather than single villains. Pay attention to what changes your recovery time after an episode, not just whether the episode happens at all.
If you want to know how to reduce hot flashes at night, think less in terms of “the perfect menopause routine” and more in terms of your own repeatable protocol. Your body will tell you a lot when you give it a structure for feedback.
Better nights often start with small shifts that become obvious only after a little tracking. Once you know your patterns, decisions get easier. Bedtime gets simpler. Sleep becomes less of a fight and more of something you can protect again.
If you want help turning these ideas into a trackable routine, Lila can help you log symptoms, sleep, meals, mood, energy, and cycles in one place so you can spot patterns and build a more personalized plan for better nights.
You should not have to do it all on your own










