
Does Perimenopause Cause Mood Swings? Yes, Here's Why
May 10, 2026
You snap at someone you love, then feel guilty an hour later. You cry at a commercial that normally wouldn't touch you. By afternoon, you're flat, foggy, and wondering whether you're stressed, depressed, sleep-deprived, or just “not yourself” anymore.
If that sounds familiar, the short answer to does perimenopause cause mood swings is yes. For many women, it does.
What makes this stage especially confusing isn't only the intensity. It's the lack of pattern. PMS at least used to show up on something like a schedule. Perimenopause often doesn't. One week you feel steady. The next, a small inconvenience feels enormous. That unpredictability can make you question your judgment and your mental health.
The good news is that these shifts are real, common, and rooted in biology. They're not a character flaw, and they're not “all in your head” in the dismissive way people sometimes mean it. Once you understand why your mood can feel so changeable, it becomes much easier to spot your own patterns and respond earlier.
It's Not Just You Your Hormones Are On a Roller Coaster
A lot of women reach this point the same way. They don't begin by saying, “I think I'm in perimenopause.” They say, “I'm suddenly so irritable,” or “I don't feel like myself,” or “Why am I crying over things that never used to knock me over?”
That emotional whiplash can be unsettling. You might feel mostly fine in the morning, then angry, tender, or overwhelmed by late afternoon. You may even notice that your reaction doesn't fit the situation. A messy kitchen, a work email, a family request, or a change of plans can land much harder than it used to.
When the swings don't follow a familiar rhythm
This is one reason perimenopause catches people off guard. Many women know what PMS feels like. Perimenopausal mood changes often feel different. They can seem random, disconnected from your period, and hard to predict from one month to the next.
That unpredictability matters. It's not only emotionally draining. It can make you doubt your own experience.
You're not overreacting because you've suddenly become weak. Your body may be sending your brain different chemical signals than it used to.
The core issue is hormonal fluctuation, especially changes in estrogen and progesterone. These hormones don't just affect periods and fertility. They also influence brain chemicals tied to mood, energy, focus, and stress tolerance.
Why validation matters
When mood shifts arrive without warning, many women blame themselves first. They assume they need more discipline, more patience, or a better attitude. Self-blame usually makes things worse.
A better starting point is this:
Name the change: If your emotional responses feel new, stronger, or less predictable, that information matters.
Look for companions: Mood swings often travel with sleep disruption, brain fog, hot flashes, or cycle changes.
Treat it as data: Once you stop judging every shift and start noticing it, you can regain a sense of control.
You don't need to “tough it out” without understanding what's happening. You need a clearer map.
Why Your Brain and Hormones Are Suddenly Out of Sync
Perimenopause isn't a smooth, steady decline. It's closer to a hormonal roller coaster. Your ovaries don't turn the volume down in a straight line. Hormone levels can rise, drop, and swing in ways that make your brain work harder to maintain emotional balance.
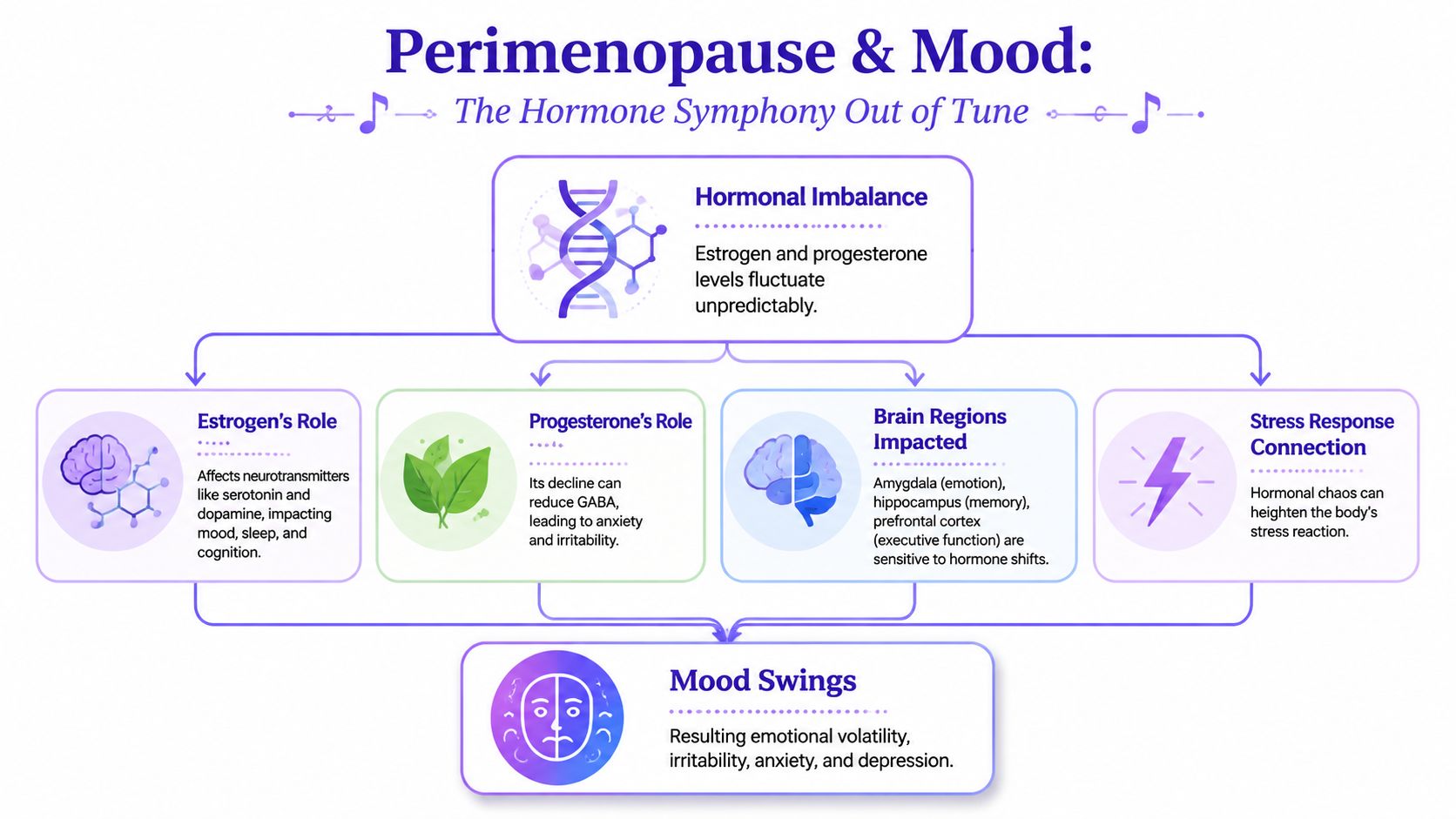
Estrogen is more than a reproductive hormone
Estrogen helps regulate neurotransmitters involved in mood, including serotonin and dopamine. When estrogen becomes erratic in perimenopause, those systems can feel less stable too. That's one reason mood changes can show up as irritability, tearfulness, anxiety, low motivation, or feeling emotionally raw.
One verified summary notes that hormonal volatility in perimenopause can include erratic estrogen surges of up to 200% day to day, along with progesterone drops, and that these shifts can contribute directly to mood swings through serotonin and calming-system disruption, as described by OSU Health's overview of why perimenopause affects mood.
Think of estrogen as part of your brain's mood support crew. When that crew's schedule becomes chaotic, the rest of the system has to scramble. Some days you feel steady. Other days, the same stressor hits much harder.
Progesterone loss can remove some of the calm
Progesterone tends to have a settling effect. As it falls, some women feel more wired, less resilient, and more easily tipped into anxiety or agitation. That doesn't mean every bad day is hormonal. It means the background level of emotional cushioning may be lower than it used to be.
This can be especially confusing if you've always thought of hormone changes as mainly physical. In reality, the brain is highly involved.
Practical rule: If your mood feels more fragile at the same time your sleep, concentration, or stress tolerance worsens, don't look at those symptoms in isolation. They often move together.
Why the unpredictability feels so disruptive
Predictable problems are easier to manage. Unpredictable ones erode confidence.
With classic PMS, you may have learned your pattern over years. Perimenopause often breaks that pattern. A mood dip may come before a skipped period, after a bad night of sleep, around hot flashes, or with no obvious warning at all. That's why tracking matters so much here. It helps you spot a pattern before your mind can.
Some women also notice that changing hormones affect attention, impulse control, and mental overload. If that sounds familiar, this piece on hormonal changes and adult ADHD severity may help connect symptoms that otherwise seem unrelated.
A simple way to picture it
Try this analogy. Your brain likes a stable soundtrack. In perimenopause, the DJ keeps changing the volume without warning. Sometimes the song is calm. Sometimes it's jarring. Your nervous system keeps adjusting, and that constant adjustment can leave you feeling emotionally stretched.
That's why “I don't know who I am this week” is such a common feeling in this stage. The issue isn't a lack of effort. It's that your internal signals have become less predictable.
Identifying the Patterns of Perimenopausal Mood Changes
Mood changes in perimenopause don't all look dramatic. Sometimes they show up as a shorter fuse, less patience, or a low hum of dread that wasn't there before. Sometimes they feel like sudden sadness, unusual sensitivity, or the sense that everyday life has become louder and harder to absorb.
What these mood changes often feel like
A common pattern is not “I'm sad all the time.” It's more like:
Irritability that arrives fast: Small frustrations feel outsized.
Tearfulness without a clear reason: You cry more easily or feel emotionally thin-skinned.
Low energy with a dark edge: You're exhausted, but rest doesn't always fix the emotional heaviness.
Trouble concentrating: Your brain feels scattered, and that can make you more reactive.
Mood shifts that don't match your cycle anymore: The timing feels random.
According to the American College of Obstetricians and Gynecologists, approximately 4 in 10 women, or 40%, experience mood symptoms during perimenopause that mirror PMS, including irritability, low energy, tearfulness, and moodiness, but these symptoms often occur unpredictably outside the usual menstrual pattern. The same source notes that psychological distress reaches 25.6% in late perimenopause in SWAN data, as described in ACOG's discussion of mood changes during perimenopause.
The biggest difference from PMS
The hallmark problem is unpredictability.
With PMS, you may have expected a rough patch before your period. In perimenopause, your mood can feel detached from that old script. You may still have monthly changes, but they're less reliable. If your periods are becoming irregular, the emotional pattern often gets irregular too.
That's why many women spend months wondering what's wrong before they connect the dots. The mood shifts don't announce themselves neatly.
A symptom that feels random is often a symptom you haven't tracked long enough yet.
What to watch for in daily life
Patterns become easier to see when you stop asking, “Why am I like this?” and start asking, “When does this happen, and what tends to come with it?”
A useful starting list includes:
Sleep changes: especially nights when you wake often or struggle to fall asleep
Hot flashes or night sweats: mood dips may cluster around them
Cycle irregularity: skipped periods, shorter cycles, longer gaps
Stress load: caregiving, work pressure, conflict, or travel
Cognitive symptoms: brain fog, forgetfulness, sensory overload
If you want help recognizing the broader picture, this guide to a perimenopause symptoms checklist can help you connect mood changes with other clues you might be brushing off.
Why tracking helps more than guessing
Memory is selective. We tend to remember the worst day and forget the lead-up. Tracking gives you a timeline. You may notice that irritability follows poor sleep, or that anxiety spikes before bleeding starts, or that two symptom clusters often travel together.
That doesn't make every day easy. It does make your experience more legible. And once it becomes legible, it becomes easier to manage.
How to Tell Mood Swings From Depression or Anxiety
Perimenopausal mood swings are real. So are depression and anxiety disorders. Sometimes they overlap. Sometimes one can trigger or worsen the other. The important question isn't whether your symptoms are “serious enough” to deserve attention. The question is what pattern they follow and how much they're affecting your life.
Longitudinal SWAN data found that the adjusted risk of high depressive symptoms increased 20 to 62% during early perimenopause compared with premenopause, with prevalence peaking at 25.6% in late perimenopause, which is why researchers describe this stage as a window of vulnerability for new-onset mood disorders.
A side by side comparison
Symptom Area | Perimenopausal Mood Swings | Clinical Depression (MDD) | Generalized Anxiety Disorder (GAD) |
|---|---|---|---|
Pattern | Often fluctuates. May feel tied to sleep disruption, cycle irregularity, hot flashes, or stress. | More persistent low mood or loss of interest that doesn't lift easily. | Ongoing worry, tension, and feeling keyed up across many situations. |
Predictability | Often unpredictable. Good and bad days may alternate quickly. | Usually more sustained than shifting hour to hour. | Can be constant or frequently present, even without a clear trigger. |
Emotional tone | Irritability, tearfulness, feeling unusually sensitive or reactive. | Hopelessness, emptiness, numbness, or persistent sadness. | Apprehension, dread, racing thoughts, physical tension. |
Energy and focus | Can dip sharply on rough days, then improve. | Often stays low for longer stretches. | Focus may be disrupted by constant worry or mental overactivation. |
Daily functioning | May strain relationships and work, but symptoms can ebb. | Daily life can feel consistently harder to manage. | Worry may interfere with sleep, concentration, and routine decisions. |
When to get help | If symptoms are intense, confusing, or affecting safety, work, or relationships. | Prompt evaluation matters. | Prompt evaluation matters, especially if panic, insomnia, or avoidance grows. |
Signs it may be more than mood swings
Use this as a practical filter.
Symptoms persist: You're not having brief swings. You feel low or anxious most days.
Function drops: Work, relationships, self-care, or basic tasks are getting harder.
Your mind feels stuck: You can't shift out of dread, hopelessness, or constant worry.
Sleep is unraveling: Poor sleep is feeding the emotional spiral instead of being an occasional trigger.
For a deeper look at what depression can look like when it isn't obvious, this guide on identifying unseen depression symptoms is a useful companion.
Panic symptoms deserve a closer look
Some women also notice sudden surges of fear, chest tightness, shakiness, or a sense of losing control during perimenopause. Those episodes can feel terrifying, especially if they're new. This article on panic attacks in perimenopause may help you understand what to bring to a clinician if that's happening.
If you're spending a lot of energy trying to decide whether your symptoms “count,” that alone is a sign to talk with a professional.
You don't need to sort this out perfectly before asking for help. A clinician can help you tell the difference between expected hormonal mood changes and a mood disorder that needs more direct treatment.
Evidence-Based Ways to Regain Emotional Balance
When your moods feel unpredictable, the instinct is often to search for one fix. In practice, most women do better with a toolkit. The key is to build that toolkit around patterns you can observe.

Start with tracking, not guessing
If unpredictability is the hardest part, tracking is the first way back to control.
A simple daily record can include mood, sleep, energy, cycle changes, hot flashes, stress, alcohol, exercise, and major life events. You don't need a perfect spreadsheet. You need enough consistency to notice links.
Try questions like these at the end of each day:
What was my mood range today? Calm, irritable, flat, anxious, tearful, overwhelmed.
How did I sleep? Not just hours, but quality.
What physical symptoms showed up? Hot flashes, headache, breast tenderness, bloating, skipped period.
What was happening around me? Travel, conflict, deadlines, caregiving, social overload.
After a few weeks, many women can see that certain “mood swing” days have recognizable setups. That insight lowers fear. It also helps you prepare.
Stabilize the basics that amplify mood swings
Hormonal shifts may start the fire. Daily habits can either fan it or help contain it.
Protect sleep like it's treatment
Sleep loss can make irritability, anxiety, and tearfulness much sharper. If you're waking at night, try reducing stimulation before bed, keeping a consistent sleep window, and making your room cool and dark. If stress and worry are part of your nighttime pattern, this resource on managing anxiety for improved sleep offers useful strategies.
A few practical habits often help:
Keep mornings anchored: Wake up at a similar time, even after a rough night.
Lower the evening volume: Bright screens, work email, and intense conversations can keep your nervous system revved up.
Notice alcohol: Some women find it worsens sleep fragmentation and next-day mood.
Eat in a way that supports steadier energy
You don't need a “perfect” menopause diet. You do need fewer blood sugar roller coasters. Long gaps without eating, highly processed meals, and too much caffeine can make a fragile nervous system feel even less stable.
Build meals around protein, fiber, and foods that keep you physically satisfied. Steadier energy often means steadier patience.
Move in ways that regulate stress
Exercise doesn't have to be punishing to help mood. Walking, strength work, yoga, and other forms of movement can lower stress and help you feel more grounded in your body. The best option is the one you'll repeat, especially on emotionally uneven weeks.
Small shift: On days when you feel edgy or on the verge of tears, aim for regulation, not performance. A walk and a stretch session may help more than forcing an intense workout.
Use calming tools that work in real life
When emotions spike, broad advice like “reduce stress” can feel useless. More specific tools are easier to use.
Try a short menu:
Box breathing or paced breathing: Helpful when your body feels activated.
Brief journaling: Write what happened, what you felt, and what physical symptoms were present.
Lower sensory load: Turn down noise, postpone nonessential decisions, step outside.
Name the state out loud: “I'm overloaded and hormonally vulnerable today” can reduce shame and stop escalation.
For some women, the fastest win comes from changing the environment before changing the thought.
Know when medical treatment belongs in the plan
Lifestyle support matters, but it isn't the whole story. If symptoms are strong, recurrent, or affecting quality of life, it's worth discussing treatment options with a clinician.
Some women benefit from hormone therapy. Others do better with a non-hormonal approach, including medications used for mood symptoms. Treatment depends on your symptom pattern, medical history, and risk factors. If you're curious about the basics, this explainer on what hormone therapy for menopause is can help you prepare for that conversation.
This short video may also help you think through options and questions for your appointment.
Build your own early warning system
The goal isn't to eliminate every mood shift forever. It's to catch the pattern earlier.
Your early warning signs might include:
More snapping than usual
Sudden hopeless thoughts after a bad night
Crying more easily
Feeling crowded by ordinary demands
Wanting to isolate
Once you know your signs, you can respond sooner. That may mean protecting sleep that night, lightening your schedule, skipping alcohol, taking a walk, or messaging your doctor if the pattern is getting stronger.
That's how tracking becomes more than record-keeping. It becomes a tool for self-trust.
Creating Your Support Team for Perimenopause
Some symptoms can be managed with self-awareness and good support. Some need medical care. Knowing the difference is a strength, not an overreaction.
Perimenopause can worsen existing mental health conditions. In one verified review, 68% of women with bipolar disorder experienced at least one major depressive episode during this phase, and one in three women overall encounter psychological changes such as anxiety or depression through perimenopause into early post-menopause, as described in this review of perimenopause and mood disorders. That's one reason professional guidance matters if your symptoms feel bigger than simple moodiness.
When to reach out sooner
Please contact a clinician promptly if:
Your mood changes are persistent: You're not bouncing back between rough patches.
Daily life is suffering: Work, relationships, parenting, or self-care feel much harder.
You have a mental health history: Especially depression, anxiety, bipolar disorder, or severe PMS.
You feel unsafe: Thoughts of self-harm, hopelessness, or not wanting to be here need immediate support.
How to prepare for the appointment
You don't need to walk in with a perfect theory. Bring observations.
A helpful note on your phone can include:
What you feel: irritability, sadness, anxiety, rage, tearfulness, numbness
When it happens: around sleep disruption, cycle changes, hot flashes, or stress
How long it lasts: brief swings, full days, or longer stretches
What else is changing: concentration, appetite, energy, periods, night waking
Bring examples, not just labels. “I cried in a meeting and then couldn't focus for hours” gives a doctor more to work with than “my mood is off.”
You deserve support that takes both hormones and mental health seriously.
If you want a simple way to spot patterns before they spiral, Lila can help you track mood, sleep, symptoms, energy, meals, and cycles in one place, then turn that information into a personalized plan. When perimenopause feels unpredictable, having a daily check-in and clear next steps can make you feel more in control and more like yourself again.
You should not have to do it all on your own









