
Recognizing the Signs of Low Estrogen You Should Not Ignore
Mar 15, 2026
The first clues that your estrogen levels are dropping are often subtle and easy to dismiss. You might notice hot flashes that seem to come out of nowhere, irregular periods that throw your cycle off, a new kind of irritability, or frustrating nights of tossing and turning. It’s not just you. Think of estrogen as a powerful hormone that helps manage multiple systems in your body. When it starts to decline, those systems can get a little haywire.
What Are the First Signs of Low Estrogen
I often explain it like this: throughout your reproductive years, estrogen acts like a steady conductor, keeping your body's internal orchestra playing in harmony. But as you enter perimenopause and its levels start to fluctuate, the conductor's rhythm gets unsteady. Suddenly, different sections of the orchestra are a little out of sync.
This is why the initial symptoms can feel so random and disconnected. One moment you're hit with a wave of intense heat, and the next you’re feeling uncharacteristically anxious or can't seem to focus. These aren't just isolated issues—they are direct signals that your body is navigating a major hormonal shift.
Categorizing Your Symptoms
To make sense of it all, it helps to see how these signals connect. Grouping them by how they affect your body can turn a confusing list of symptoms into a clear pattern. Recognizing these patterns is the first real step toward managing the changes and feeling like yourself again.
This visual helps show how a single hormonal shift can create distinct ripples across your well-being.
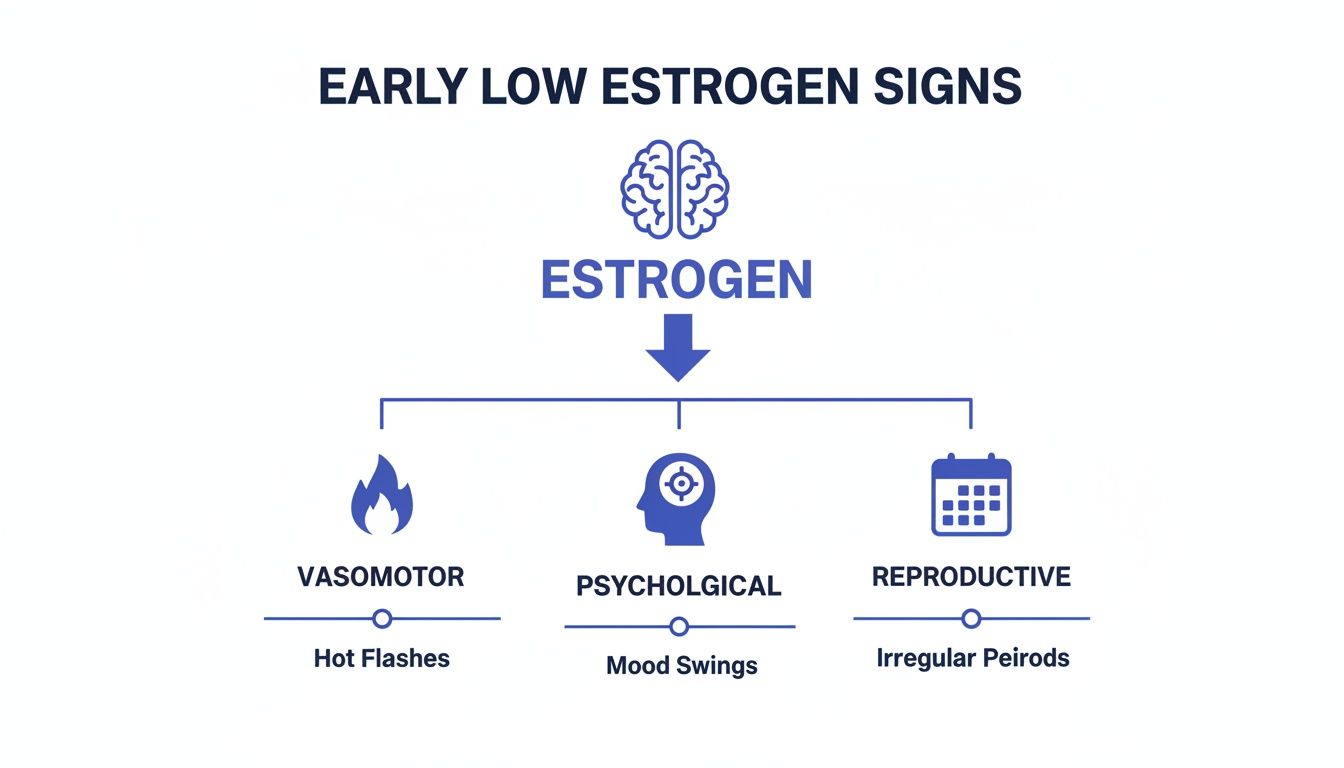
As you can see, what starts as a simple drop in estrogen can trigger interconnected symptoms that affect everything from your body temperature to your mood.
Early Signs of Low Estrogen at a Glance
This table breaks down the initial symptoms to help you quickly identify how declining estrogen may be affecting different aspects of your well-being.
Symptom Category | Common Signs | What It Can Feel Like |
|---|---|---|
Vasomotor | Hot flashes, night sweats | A sudden, intense warmth spreading across your chest, neck, and face. It's often followed by sweating and then a cold chill. |
Reproductive | Irregular or missed periods, vaginal dryness | Your menstrual cycle becomes unpredictable—it might be shorter, longer, heavier, or lighter before it eventually stops. |
Psychological | Mood swings, anxiety, brain fog, irritability | Feeling unusually on edge, tearful, or short-tempered. You might also struggle to concentrate or remember simple things. |
Looking at these symptoms together can help you see the bigger picture. If you're trying to figure out what's going on, you may want to learn more about how to test for menopause and other hormonal changes. Paying attention to these early signals is the best way to start taking control of your health.
The Sudden Heat of Hot Flashes and Night Sweats
Hot flashes and night sweats are probably the most well-known—and often most disruptive—signs of low estrogen. If you've ever experienced one, you know the feeling. One minute, you’re perfectly comfortable. The next, a sudden, intense wave of heat blooms in your chest and rushes upward, engulfing your neck and face. This internal furnace can leave your skin flushed and blotchy as you break out in a sweat, feeling as if you just sprinted up a hill.
This isn't just a feeling; it’s a biological misfire. Your brain's hypothalamus acts as your body’s internal thermostat, working to keep your core temperature just right. Estrogen plays a key role in helping that thermostat stay properly calibrated.
When your estrogen levels start to drop and fluctuate, the hypothalamus gets confused. It can suddenly think you’re overheating, even when you're not. In response, it triggers an all-hands-on-deck cooling response: blood vessels near your skin dilate to release heat, and your sweat glands kick into overdrive. That's a hot flash.
How Hot Flashes Disrupt Daily Life
These episodes are far more than a minor inconvenience. Imagine you're in the middle of a big presentation at work when you feel your face turn beet-red and sweat start trickling down your temples. Or you're trying to have a nice dinner out, only to be hit by a wave of heat so intense you have to start fanning yourself with the menu.
Just as quickly as the heat arrives, it can vanish, leaving you with a sudden cold chill. Many women find themselves shivering in damp clothes, feeling completely drained by the temperature rollercoaster.
The frequency can vary dramatically from person to person. Some women might have a few mild flashes a week, while others might battle dozens of intense episodes every day. This unpredictability can create a lot of anxiety, sometimes making you hesitant to even leave the house. If this sounds familiar, you can get more details by exploring why you may be having hot flashes.
When Hot Flashes Happen at Night
When these episodes strike while you're asleep, they’re called night sweats. You can be jolted awake, completely drenched in sweat, with your pajamas and sheets soaked through. This often forces you to get up, change, and sometimes even remake the bed—completely destroying any chance of a restful night.
This constant sleep disruption creates a domino effect that impacts your entire life:
Daytime Fatigue: Waking up several times a night naturally leads to exhaustion and grogginess the next day.
Mood Swings: A lack of quality sleep can make anyone feel more irritable, anxious, or emotionally fragile.
Brain Fog: Sleep deprivation is a major contributor to the concentration and memory problems often described as "brain fog."
If you’re dealing with this, you are far from alone. A massive global analysis showed that hot flashes affect 54.02% of middle-aged women in developing countries and 50.39% in developed nations. This data confirms that these signs of low estrogen are a shared experience for millions of women worldwide.
Why You Feel So Tired: Unpacking Fatigue and Sleep Problems
If you’re wrestling with a profound, bone-deep weariness that a full night’s sleep can’t seem to fix, you’re not alone. This is one of the most common signs of low estrogen. It’s not the normal tiredness you feel after a long week; it's a heavy, persistent fatigue that can make even the smallest daily tasks feel like climbing a mountain. Many women describe it as feeling like their internal battery is stuck at 20%, no matter how much they try to recharge.
This feeling of being constantly drained isn't just in your head. Estrogen is a key player in how your body produces and manages energy right down to the cellular level. When your levels begin to fall, your body's entire energy-generating system takes a hit, leaving you feeling completely wiped out.
The Sleep-Fatigue Connection
To make matters worse, this exhaustion is often fueled by poor sleep—another classic calling card of low estrogen. We already know that night sweats can jolt you awake, but estrogen's impact on sleep is even more direct. It plays a crucial role in regulating your sleep-wake cycles and helping you achieve the deep, restorative sleep your body and brain crave.
As estrogen declines, you might find it’s harder to fall asleep or, more frustratingly, stay asleep. This kicks off a draining cycle that’s tough to break.
Low estrogen messes with your sleep. It leads to more frequent awakenings and less time spent in the truly restorative stages of sleep.
Poor sleep guarantees daytime fatigue. You wake up feeling like you haven't slept at all, making it a struggle to function during the day.
Exhaustion impacts everything else. This deep fatigue often brings along brain fog, irritability, and a lack of motivation, which in turn can make it even harder to wind down and rest at night.
It’s a vicious cycle, and it explains why you can get a solid eight hours yet still wake up feeling unrefreshed. Breaking free from this pattern is key, and we share practical tips in our guide to finding menopause fatigue relief.
Fatigue Is More Common Than You Think
While hot flashes tend to grab the spotlight, fatigue is often a far more disruptive symptom of hormonal shifts. This isn't just feeling tired; it’s an overwhelming exhaustion that can interfere with your work, your relationships, and your overall quality of life. It’s a very real, physiological symptom—not a personal failing.
Studies on perimenopause reveal a surprising gap between what women expect and what they actually experience. While 71% of women identify hot flashes as a key sign, an even greater number—a staggering 83%—report dealing with significant fatigue, making it one of the most widespread signs of low estrogen.
This physical and mental drain is directly tied to estrogen’s job in managing energy, sleep quality, and even brain chemistry. When levels dip, it’s natural to feel an overpowering tiredness that can derail your daily routine.
Ultimately, the exhaustion you’re feeling is a powerful signal from your body. Recognizing it as a primary sign of low estrogen is the first step toward getting answers and finding strategies that can help you finally recharge.
Navigating Mood Swings, Brain Fog, and Anxiety
Low estrogen doesn’t just mess with your body; some of its most disorienting effects can feel like they’re messing with your mind. If you’ve been feeling on edge, unusually anxious, or like your brain is wrapped in cotton, there's a very real biological reason for it. Estrogen is far more than a reproductive hormone—it’s a key player in your brain, helping to manage mood-regulating chemicals like serotonin and dopamine.
Think of estrogen as a master conductor for your brain’s communication network. It helps ensure the signals that keep you feeling focused, calm, and emotionally balanced are all firing correctly. When estrogen levels drop, that finely-tuned system can get thrown out of whack. The result is often a cascade of confusing and frustrating mental symptoms.
The Brain on Low Estrogen
This hormonal shift can feel like you’re losing a bit of control over your own thoughts and emotions. Many women are caught off guard by sudden changes that are hard to put into words.
Sudden Irritability: You might find yourself snapping over small things that never used to bother you.
Unexplained Anxiety: A wave of panic or a sense of dread can wash over you for no apparent reason, complete with a racing heart.
Weepiness: It's common to feel tearful and emotionally fragile, maybe crying during a commercial or a simple conversation.
Brain Fog: This is that classic feeling of walking into a room and completely forgetting why, or losing your train of thought right in the middle of a sentence.
These experiences aren't a sign that you're "going crazy." They are direct physiological responses to your body’s changing internal chemistry. As your brain adapts to having less estrogen, its entire chemical balance is temporarily disrupted, leading to these jarring mental and emotional shifts.
Low estrogen essentially hits the reset button on your brain's emotional wiring. This can make you feel like a stranger in your own mind, but it’s so important to remember that these are real, treatable symptoms of a hormonal transition.
From Confusion to Clarity
One of the toughest parts of dealing with these signs is the feeling of isolation they can create. You might start to wonder if what you're experiencing is normal or if something is seriously wrong. The cognitive slowdown known as brain fog, for example, can be especially alarming. It's that frustrating sensation that your brain just isn't as sharp as it used to be—words get stuck on the tip of your tongue, and tasks that were once easy now feel overwhelming.
In the same way, new or heightened anxiety can be deeply unsettling. One study found that up to 40% of women struggle with mood changes during this life stage, which just confirms how incredibly common this is. Since low estrogen is a hallmark of perimenopause and menopause, it's helpful to get a clearer picture by understanding menopause and anxiety symptoms and how they can affect daily life.
Simply recognizing that these mental hurdles are tied to your hormones is the first real step toward finding relief. It helps shift the narrative from self-blame to proactive problem-solving. Once you understand the "why" behind your mood swings, anxiety, and brain fog, you can start exploring the right strategies to support your brain and reclaim your mental clarity.
Physical Changes Affecting Your Skin, Bones, and Body
While we often focus on things like mood swings or poor sleep, low estrogen can show up in some very physical ways all over your body. Estrogen is a key player in maintaining your skin, bones, and even your body’s basic structure. Think of it as the project manager for producing collagen, the protein that gives your skin its strength and elasticity.
When estrogen levels dip, so does collagen production. Imagine the scaffolding that keeps your skin looking firm and feeling plump—that's collagen. As that support system starts to weaken, you might notice your skin feels thinner, drier, and less bouncy than it once did. This is often when fine lines and wrinkles seem to appear more pronounced.
And it’s not just your skin. You might also see changes in your hair, like more shedding than usual or a general feeling of thinning. Estrogen helps keep your hair follicles in a healthy growth cycle, and when there's less of it, that cycle can be disrupted, leaving your hair feeling less full.
How Low Estrogen Affects Intimate Health
Now, let's talk about something that's incredibly common but often goes unmentioned: urogenital health. The tissues in the vagina and urinary tract are packed with estrogen receptors, making them very sensitive to hormonal shifts. When estrogen drops, these tissues can become thinner, drier, and less flexible, a condition known as vaginal atrophy or the genitourinary syndrome of menopause (GSM).
This can cause a host of symptoms that can really get in the way of your daily life:
Vaginal Dryness: A persistent feeling of discomfort due to a lack of natural lubrication.
Painful Intercourse: When tissues are dry and thin, sex can become uncomfortable or even painful.
Urinary Urgency: You may feel a sudden, strong need to pee, which can sometimes lead to leaks.
Increased UTIs: Changes to the vaginal pH and urinary tract tissue can leave you more vulnerable to urinary tract infections.
So many women experience these symptoms but feel hesitant to bring them up. It’s vital to remember that these are direct physiological responses to hormonal changes, and they are very treatable. Talking to your doctor is the first step toward feeling comfortable and confident again.
The Connection to Joint Pain and Bone Health
Have you found yourself waking up with more aches and stiffness in your joints? You're not just imagining it. Estrogen has natural anti-inflammatory properties that help keep your joints feeling good. As your estrogen levels fall, you lose some of that protective, lubricating effect, which can lead to an uptick in joint pain and stiffness.
But the impact goes deeper than just aches and pains. Low estrogen poses a silent but serious threat to your bones. Estrogen is crucial for regulating bone remodeling—the natural process where your body clears out old bone and builds new, strong bone. It essentially puts the brakes on the cells that break bone down.
When estrogen declines, that braking system gets weaker. Bone breakdown starts to happen faster than bone formation, causing your bones to lose density and become more porous over time. This process is what leads to a significantly higher long-term risk of osteoporosis, a condition that makes bones brittle and much more likely to fracture. To learn more, this osteoporosis patient information is a great resource.
From dry skin and achy joints to the more serious risk of bone loss, these physical signs paint a clear picture of why paying attention to your estrogen levels is so important for your health today and for years to come.
From Symptom Overwhelm to a Clear Action Plan
When you're dealing with low estrogen, it can feel like you're trying to make sense of a dozen different conversations happening in your body all at once. One moment, a hot flash washes over you. The next, brain fog descends, or a wave of anxiety hits for no apparent reason. It's a confusing and often overwhelming experience when your sleep, mood, energy, and body all seem to be sending different signals.
You end up trying to connect the dots on your own, piecing together clues between what you ate and how you slept, or how your mood tanked after a stressful day. But what if you could stop guessing? What if you could turn all that chaos into a clear, personalized roadmap that actually works for you?
From Guessing to Knowing with Lila
This is exactly where the Lila app can make a world of difference. It was designed to act as your personal guide through the noise, helping you understand your symptoms instead of just enduring them. Using simple daily check-ins, the app helps you track your unique patterns in one convenient place.
With just a few taps, you can log the intensity of your hot flashes, your energy levels, and any shifts in your mood. Think of it like creating a detailed, personal map of your body's hormonal landscape. This approach helps turn that feeling of confusion into real clarity, showing you exactly how different factors are connected to the way you feel each day.
The goal is to put you back in the driver's seat. When you can see your own patterns laid out clearly, you’re no longer guessing what might be wrong—you’re working with real information about what’s happening in your body. That’s the first real step toward regaining control.
Your Personalized Action Plan
Lila doesn’t just show you a chart and leave you to figure it out. Once it starts to understand your specific patterns, it provides a personalized action plan that targets your biggest challenges. Whether your main struggle is poor sleep, mood swings, or constant fatigue, Lila gives you concrete, evidence-based strategies to start feeling better.
This isn’t a generic, one-size-fits-all program. It's targeted support that changes as your needs change. Here’s what makes this approach so helpful:
Centralized Tracking: Finally, one single place to log your symptoms, mood, sleep, energy—even your meals and cycle. You can stop trying to remember how you felt last week or searching through scattered notes.
Data-Driven Insights: Lila connects your daily inputs to uncover trends you might have missed. You might see how a certain food seems to trigger night sweats or how a walk can boost your mood for hours.
24/7 Coaching Support: You don’t have to do this alone. A chat-based coach is always available to offer encouragement, answer your questions, and help you stick with your plan.
With a 4.7-star rating on the App Store and thousands of positive reviews, Lila has already helped over 35,000 women navigate this transition. Many report feeling a noticeable difference within the first week. By turning symptom overwhelm into a clear path forward, you can feel confident and empowered to feel like yourself again.
Frequently Asked Questions About Low Estrogen
It's completely normal to have questions when your body starts changing. Here are straightforward answers to some of the things we hear most often about declining estrogen, designed to give you the clarity you need.
At What Age Do Estrogen Levels Typically Start to Drop?
For most of us, the journey begins with perimenopause, which often kicks off in our 40s. Think of this as the "runway" to menopause. During this time, estrogen levels don't just drop—they can fluctuate unpredictably. However, everyone's timeline is unique; some women notice these shifts in their late 30s, while others won't until their early 50s.
This phase can last for several years. The average age for menopause in the United States is 51, which is the point when your period has been gone for a full year and your estrogen levels settle into a new, consistently lower normal.
Can I Increase My Estrogen Levels Naturally?
That's a common question, but it’s a bit more nuanced than a simple yes or no. While you can't significantly boost your estrogen levels with lifestyle changes alone, you absolutely can support your body's hormonal balance. A great place to start is with phytoestrogens, which are plant-based compounds that gently mimic estrogen's effects in the body.
You can find phytoestrogens in foods like soy, chickpeas, flaxseeds, and sesame seeds. When you pair a diet rich in these foods with regular exercise and solid stress-management habits, you create a powerful foundation to help your body navigate this transition more smoothly.
Keep in mind, though, that these natural approaches may only offer mild relief. If your symptoms are persistent or truly disruptive, it’s best to talk with your healthcare provider about all the options available.
When Should I See a Doctor for Low Estrogen Signs?
The short answer? When your symptoms start getting in the way of your life. If you find your work, relationships, or general sense of well-being are taking a hit, it's time to get professional guidance.
Consider making an appointment if you're experiencing things like:
Hot flashes or night sweats that constantly sabotage your sleep.
Mood swings, anxiety, or brain fog that are affecting your mental clarity.
Vaginal dryness or discomfort that makes intimacy painful or unpleasant.
A level of fatigue that no amount of rest seems to fix.
A doctor can help confirm if low estrogen is the root cause, rule out any other conditions, and work with you to map out a treatment plan that fits your life.
Besides Menopause, What Else Causes Low Estrogen?
While perimenopause and menopause are the headliners, they aren't the only reasons estrogen can decline. A number of other factors can cause levels to drop, including the surgical removal of ovaries (oophorectomy), certain cancer treatments like chemotherapy, or problems with the pituitary gland.
Conditions like premature ovarian insufficiency, where the ovaries stop working properly before age 40, can also trigger an early drop. Even lifestyle factors can play a role—things like over-exercising, eating disorders, or chronic, unrelenting stress can throw your hormones out of whack. If you're under 40 and experiencing symptoms, it's especially important to see a doctor to get an accurate diagnosis.
Ready to move from symptom confusion to a clear action plan? Lila uses AI to help you track your unique patterns and provides a personalized plan to ease your symptoms. Start your journey with Lila today.
You should not have to do it all on your own










